Abstract
Agenesis of the dorsal pancreas is a rare congenital pancreatic malformation. We herein describe a 67-year-old woman with a 5-day history of lower back pain who was eventually diagnosed with agenesis of the dorsal pancreas. Abdominal computed tomography showed an enlarged pancreatic head, but the pancreatic body and tail were invisible. The magnetic resonance imaging findings were similar to the computed tomography findings. Magnetic resonance cholangiopancreatography showed that the major pancreatic duct was mildly dilated but otherwise normal. Endoscopic ultrasound revealed absence of the pancreatic body and tail, an enlarged head of the pancreas, and mild pancreatic duct dilation. The final diagnosis was dorsal pancreatic agenesis.
Keywords
Introduction
Agenesis of the dorsal pancreas is a rare congenital pancreatic malformation that may be associated with other congenital abnormalities. It was first described in 1911 in an autopsy study. 1 Patients with agenesis of the dorsal pancreas can be asymptomatic or present with abdominal pain, weight loss, pancreatitis, diabetes mellitus, bile duct obstruction, or duodenal obstruction; rarely, they may also develop pancreatic exocrine insufficiency or pancreatic adenocarcinoma.2–4 Agenesis of the dorsal pancreas can be detected with computed tomography (CT), ultrasound, magnetic resonance imaging, magnetic resonance cholangiopancreatography (MRCP), and the gold-standard technique endoscopic retrograde cholangiopancreatography (ERCP).5,6 Compared with surface ultrasound, endoscopic ultrasound (EUS) is closer to the pancreas and shows the lesions more clearly. Additionally, EUS-guided fine needle aspiration (EUS-FNA) can reduce the damage induced by biopsy. EUS has high value in the diagnosis of pancreatic diseases. 7 Therefore, EUS may be useful in the diagnosis of agenesis of the dorsal pancreas.4,6
Case report
This case report describes a 67-year-old woman who presented to the hospital with a 5-day history of lower back pain. The pain was persistent, but she had no abdominal pain, nausea, or fever. She had no medical or surgical history, had no allergies, did not consume alcohol, and was not a smoker. Physical examination revealed no abnormalities.
Abdominal CT showed an enlarged head of the pancreas and atrophy of the body and tail of the pancreas (Figure 1). This caught the attention of the physicians, and the patient was admitted to the hospital. Magnetic resonance imaging showed the same abnormalities: the pancreatic head was increased in size and the pancreatic body and tail were invisible (Figure 2). The pancreatic duct system was more clearly visible by MRCP; the distal portion of the pancreatic duct was invisible, and the proximal portion was mildly dilated (Figure 3). In the subsequent EUS examination, the body and tail of the pancreas were absent, the head of the pancreas was increased in size, and the pancreatic duct was mildly dilated (3.5 mm) (Figure 4(a), (b)).
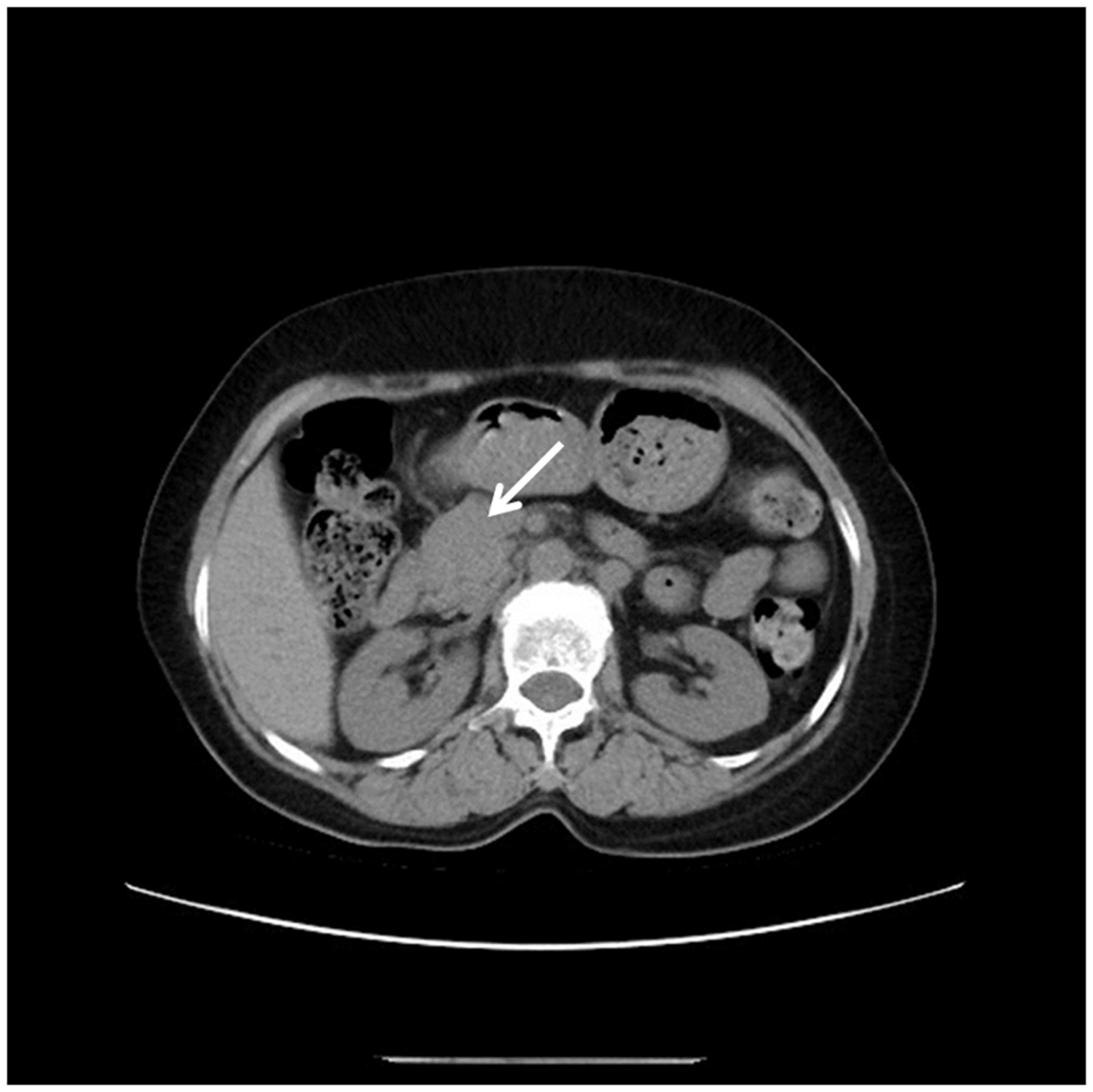
Abdominal computed tomography showing an enlarged pancreatic head (white arrow). The body and tail of the pancreas are missing

Abdominal magnetic resonance imaging showing an enlarged pancreatic head (white arrow). The body and tail of the pancreas are missing

Magnetic resonance cholangiopancreatography showing mild dilation (3.5 mm) of the proximal pancreatic duct (white arrow). The distal portion of the pancreatic duct is invisible

Endoscopic ultrasound (a) The head of the pancreas was enlarged, and the pancreatic duct was mildly dilated (3.5 mm). CBD, common bile duct; PD, pancreatic duct. (b) The body and tail of the pancreas were absent
A glucose tolerance test (fasting blood glucose, 4.93 mmol/L; blood glucose 120 minutes after sugar ingestion, 8.09 mmol/L) indicated that the patient had impaired glucose tolerance. The blood and urine amylase levels were within the reference range. The carcinoembryonic antigen level was 1.43 ng/mL (reference range, 0–7 ng/mL), and the CA19-9 level was 4.62 U/mL (0–34 U/mL).
Considering the EUS and other imaging findings as well as the laboratory examination results, we finally diagnosed the patient with agenesis of the dorsal pancreas.
The patient’s lower back pain gradually improved during treatment with alprostadil injection, pantoprazole sodium injection, and compound digestive enzyme capsules. However, the cause of the pain remained unclear because we found no evidence supporting pancreatitis, intestinal obstruction, malignancy, or diabetic neuropathy, all of which are common causes of pain in patients with agenesis of the dorsal pancreas. At the 2-year follow-up, the patient was asymptomatic with no treatment. Unfortunately, a radiologic re-examination was not performed.
Discussion
The pancreas arises from the dorsal and ventral anlagen. The normal structure of the pancreas includes the head, uncinate process, neck, body, and tail. The ventral pancreatic anlage forms the posterior part of the head and uncinate process, while the dorsal pancreatic anlage contributes mainly to the upper head, neck, body, and tail of the organ.6,8 Each anlage possesses a duct system. At the sixth to seventh week of gestation, the ventral pancreas fuses with the dorsal pancreas. During the fusion, the ventral and dorsal ducts form the main pancreatic duct. The accessory pancreatic duct is formed from the portion of the dorsal anlage that gives rise to the upper pancreatic head. A disorder during the embryological development of the pancreas can lead to congenital abnormalities, 6 such as agenesis of the dorsal pancreas.
With the development of medical imaging technology, many ways to diagnose agenesis of the dorsal pancreas have been established, such as CT, magnetic resonance imaging, ultrasound, and EUS. Kabnurkar et al. 9 recently reported that features of agenesis of the dorsal pancreas features as shown by positron emission tomography/CT, ERCP, or MRCP are necessary to reveal the major and accessory duct systems. 10 Differential diagnoses of agenesis of the dorsal pancreas include pancreas divisum and pseudo-agenesis. Failure of the ventral and dorsal pancreatic ducts to fuse is called pancreas divisum. Atrophy of the body and tail of the pancreas secondary to chronic pancreatitis with sparing of the pancreatic head is termed pseudo-agenesis. 11 Some reports have described the application of EUS in pancreas divisum and chronic pancreatitis, confirming that EUS can reliably find the pancreatic duct. 12 Although few reports in the literature mention the use of EUS in the diagnosis of agenesis of the dorsal pancreas, EUS is an important diagnostic tool for this condition. Because agenesis of the dorsal pancreas is sometimes complicated by pancreatic tumors, such as ampullary carcinoma, 13 pancreatic neuroendocrine tumor, 14 pancreatic ductal adenocarcinoma, 15 and mucinous adenocarcinoma, 2 EUS-FNA-guided biopsy may be helpful. Malak et al. 16 implied that EUS-FNA was more sensitive than ERCP cytology in diagnosing malignant pancreatic neoplasms. Each examination has its advantages; thus, a full understanding of the characteristics of each examination will be beneficial for correct diagnosis of the disease.
Conclusion
Agenesis of the dorsal pancreas, an extremely rare congenital pancreatic malformation, must be kept in mind when the body and tail of the pancreas are not seen during routine examinations. EUS may have a role in the diagnosis of pancreatic dysplasia through its ability to clearly show the pancreatic duct and parenchyma. Additionally, as a minimally invasive technique that can be combined with EUS-FNA, it may be superior to ERCP.
Supplemental Material
IMR884148 Supplemetal Material - Supplemental material for Performance of endoscopic ultrasound for diagnosis of agenesis of the dorsal pancreas: a case report
Supplemental material, IMR884148 Supplemetal Material for Performance of endoscopic ultrasound for diagnosis of agenesis of the dorsal pancreas: a case report by Jin Wei Zhong, Ling Min Yu, Qing Ji Ying, Wen Wen Peng, Chang Zhao Xu, Zhen Zhai Cai, Zhan Xiong Xue and Yu Hui Zhou in Journal of International Medical Research
Footnotes
Acknowledgment
I deeply thank the contribution of each co-author.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Ethics and consent statements
This was a retrospective study involving only one patient. The study was conducted in accordance with the declaration of Helsinki, and all examinations described in this article were performed for medical purposes. The patient’s information was kept strictly confidential during the study. Verbal consent was obtained from the patient.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
