Abstract
Objective
We conducted a systematic literature search and meta-analysis to identify randomized controlled trials (RCTs) comparing the efficacy and safety of ramosetron versus ondansetron for the prevention of postoperative nausea and vomiting (PONV; PON and POV, respectively) in patients undergoing laparoscopic surgery.
Methods
The electronic databases PubMed, EMBASE, Web of Science, and Cochrane Library were searched up to March 2019 to identify relevant studies.
Results
The final pooled analysis included 6 RCTs and revealed that postoperative treatment with ramosetron at 24 to 48 hours after surgery significantly reduced the incidence of PON and POV relative to treatment with ondansetron. In a subgroup analysis, ramosetron 0.3 mg tended to reduce PON (0–2 hours) and POV (24–48 hours) more effectively than ondansetron 4 mg. However, no statistical difference was observed between ramosetron 0.3 mg and ondansetron 8 mg in terms of the reduction of PON or POV during any time interval within the first 48 hours after surgery.
Conclusions
Our results indicate that ramosetron 0.3 mg is superior to ondansetron 4 mg and comparable to ondansetron 8 mg for PONV prophylaxis after laparoscopic surgery.
Keywords
Introduction
Although both physicians and patients consider the avoidance of postoperative nausea and vomiting (PONV) to be an important clinical issue, this distressing complication remains common after surgical procedures.1,2 Patients who undergo laparoscopic surgery are highly susceptible to PONV because abdominal gas insufflation may stretch mechanoreceptors in the intestine, leading to serotonin release and the subsequent activation of serotonin subtype 3 (5-HT3) receptors. 3 The reported incidences of PONV in patients undergoing laparoscopic surgery range from 46% to 72%.4,5 In addition to causing psychological and physical discomfort, PONV increases the risk of postoperative morbidities such as pulmonary aspiration, dehydration, wound dehiscence, and electrolyte imbalance. These morbidities can disrupt the surgical wound and place an increased burden on the hospital system.6,7 Therefore, the prevention and/or treatment of PONV may accelerate early postoperative recovery, alleviate undesirable side effects, and increase patient satisfaction.7,8
The use of various types of antiemetics such as phenothiazines 9 and benzamide 10 to prevent and treat PONV in patients scheduled to undergo laparoscopic surgery is of increasing research interest, although the effects of these agents on PONV remain largely unclear. Of the presently available antiemetics, 5-HT3 receptor (5HT3R) antagonists (e.g., ondansetron, ramosetron) are widely used to prevent PONV.11,12 Members of this superfamily of Cys-loop, ligand-gated ion channels act as highly potent antagonists of serotonin binding to 5HT3Rs on the terminals of afferent branches of the vagus nerve and in certain areas of the brain. 13 Accordingly, these drugs can be used to treat PONV in patients recovering from surgery. Ondansetron, the first commercially available 5HT3R antagonist, has a relatively short half-life of 3 to 5 hours and has been shown to be more potent than conventional antiemetics (e.g., metoclopramide and droperidol) for the prevention of PONV.14–16 Ramosetron, a newly developed 5HT3R antagonist, has a relatively long duration of action (up to 48 hours) and a markedly slow rate of dissociation from its bound receptor. Accordingly, the receptor antagonist effect of ramosetron is more persistent than that of ondansetron.17,18 The first report describing 5HT3R antagonist therapy for the prevention of PONV in patients undergoing laparoscopic surgery was published in 2010. 19 Although several randomized controlled trials (RCTs) have since been conducted to compare the efficacy and safety of ondansetron and ramosetron for the prevention of PONV after laparoscopic surgery,19–21 the conclusions have been somewhat inconsistent. Accordingly, it remains unclear whether ramosetron is more effective than ondansetron for the prevention of PONV in patients after laparoscopic surgery.
Therefore, the present analysis aimed to identify published RCTs that compared the efficacy and safety of ramosetron versus ondansetron for the prevention of PONV in patients undergoing laparoscopic surgery under general anesthesia. We anticipate that the results of our analysis will add to the existing knowledge on this topic and facilitate surgeons, anesthesiologists, patients, and policymakers in making relevant decisions regarding the future care of this patient population.
Materials and methods
Search strategy
Independent systematic searches of the PubMed, EMBASE, and Web of Science databases up to March 2019 were conducted by two of the study authors (Yiping Li and Ruiming Deng) to identify all relevant available studies. The search was restricted to articles published in English, and the following keywords were applied: “ramosetron,” “ondansetron,” “postoperative nausea and vomiting,” “PONV,” “PON,” “POV,” “nausea,” “vomiting,” “laparoscopic surgery,” “laparoscopic,” “randomized controlled trial,” and “RCT.” We also searched the reference lists of the retrieved articles to identify additional relevant studies.
Inclusion and exclusion criteria
Studies were selected according to the following inclusion criteria: (i) RCT design; (ii) intervention of ramosetron versus ondansetron for the prevention of PONV; (iii) patients inclusion of undergoing laparoscopic surgery; (iv) data available for analysis; and (v) at least one of the following outcomes: incidence of nausea or retching/vomiting (primary outcome) and side effects following the administration of ramosetron or ondansetron, such as dizziness, headache, and drowsiness (secondary outcomes). Studies written in a language other than English were excluded.
Data extraction and quality assessment
The two authors independently extracted the following outcome-related data from all potentially eligible studies: first author, publication year, country, interventions, participant age, sample size, and primary results. Two additional authors (Juan Zhou and Yuan Chen) independently conducted a quality evaluation of all selected studies using the Cochrane Collaboration tool. 22 The following six specific domains were evaluated: sequence generation, allocation concealment, blinding, incomplete outcome data, selective outcome reporting, and other issues. Any discrepancies were resolved by discussion with a third author (Aiping Ouyang) when necessary.
Statistical analysis
All statistical calculations were performed using Revman 5.2 (Cochrane Collaboration). Data were expressed as relative risk (RR) with 95% confidence intervals (CIs). Statistical heterogeneity was evaluated using I2 statistics, with values >50% indicating significant heterogeneity. An I2 value <50% indicated no statistical heterogeneity, and in such cases a fixed-effect model was applied to the analysis. Otherwise, a random-effect model was applied. A funnel plot was used to assess publication bias.
Results
A total of 115 studies were retrieved during the initial searches of the electronic databases. Ninety-eight articles were excluded after screening the titles and abstracts according to the inclusion/exclusion criteria. Of the 17 remaining studies considered eligible for the detailed evaluation, 11 articles were excluded as irrelevant after reviewing the full manuscript. Finally, the data from six studies19–21,23–25 involving 361 patients in the ondansetron group and 326 patients in the ramosetron group were included in the meta-analysis. A detailed flow diagram of the study selection process is presented in Figure 1. The basic characteristics of each included study are listed in Table 1. The six domains evaluated for bias across all studies are shown in Table 2.

Search strategy and selection of randomized controlled trials included in the meta-analysis.
Characteristics of studies included in the meta-analysis.

Quality assessment of included studies.

PON
As shown in Figure 2, five studies19–21,23,25 that included 629 patients treated with ondansetron or ramosetron at different time intervals after laparoscopic surgery reported the incidence of PON events. No heterogeneity in the outcome of PON was observed between patients treated with ramosetron and those treated with ondansetron during different time periods. The RR for the periods 0 to 2, 2 to 24, and 0 to 24 hours was 0.83 (95% CI, 0.68–1.01), 0.88 (95% CI, 0.69–1.11), and 0.87 (95% CI, 0.74–1.02), respectively. A pooled analysis based on a fixed-effects model revealed that, at 24 to 48 hours after surgery, treatment with ramosetron was more effective at reducing the incidence of PON compared with treatment with ondansetron (RR, 0.63; 95% CI, 0.40–0.99; P = 0.05).

Forest plot of relative risk from a comparison of postoperative nausea between the ramosetron and ondansetron groups: (a) 0 to 2 hours; (b) 2 to 24 hours; (c) 0 to 24 hours; (d) 24 to 48 hours.
Next, a subgroup analysis was performed to determine whether the dose of ondansetron (4 or 8 mg) might affect the incidence of PON when compared with ramosetron 0.3 mg. Compared with ondansetron 4 mg, ramosetron treatment was more effective at preventing the incidence of PON at 0 to 2 hours after surgery (RR, 0.81; 95% CI, 0.67–0.99; P = 0.04). There was no statistically significant difference in the incidence of PON observed between the ramosetron and ondansetron 4 or 8 mg groups during other time periods.
POV
As shown in Figure 3, five studies19,20,23–25 in 614 patients examined the incidence of POV (ondansetron, n = 326; ramosetron, n = 288). A meta-analysis of the results of these studies showed that there was no statistically significant difference in the incidence of POV between the two treatment groups at different time intervals within the 24-hour period after laparoscopic surgery. The RRs for 0 to 2, 2 to 24, and 0 to 24 hours were 0.99 (95% CI, 0.61–1.62), 1.12 (95% CI, 0.58–2.18), and 1.02 (95% CI, 0.64–1.62), respectively. At 24 to 48 hours after laparoscopic surgery, ramosetron 0.3 mg was significantly more effective than ondansetron 4 mg in reducing POV (RR, 0.26; 95% CI, 0.13–0.49; P<0.0001).

Forest plot of relative risk from a comparison of postoperative vomiting between the ramosetron and ondansetron groups: (a) 0 to 2 hours; (b) 2 to 24 hours; (c) 0 to 24 hours; (d) 24 to 48 hours.
Additionally, a subgroup analysis was conducted to determine whether ondansetron dose (4 or 8 mg) might affect the incidence of POV when compared with ramosetron 0.3 mg. A fixed-effects model analysis of the pooled data revealed no statistically significant difference in the incidence of POV between the ramosetron group and the ondansetron 4 and 8 mg groups at 0 to 2 hours after laparoscopic surgery.
Side effects
Four of the included studies20,21,23,25 reported the side effects (headache, dizziness, drowsiness) experienced by patients treated with ramosetron or ondansetron during the 48-hour period after laparoscopic surgery. A pooled analysis based on a fixed-effects model did not reveal significant differences between the ondansetron and ramosetron groups for incidence of headache (RR, 0.57; 95% CI, 0.28–1.17), dizziness (RR, 0.98; 95% CI, 0.55–1.74), or drowsiness (RR, 0.98; 95% CI, 0.55–1.75) (Figure 4).

Forest plot of the relative risk from a comparison of the side effects experienced by patients receiving ramosetron and ondansetron treatment: (a) dizziness; (b) headache; (c) drowsiness.
Publication bias
A funnel plot was used to qualitatively assess the potential publication bias among the studies. The partially symmetrical funnel plot presented in Figure 5 indicates that there was no potential publication bias in the included studies.
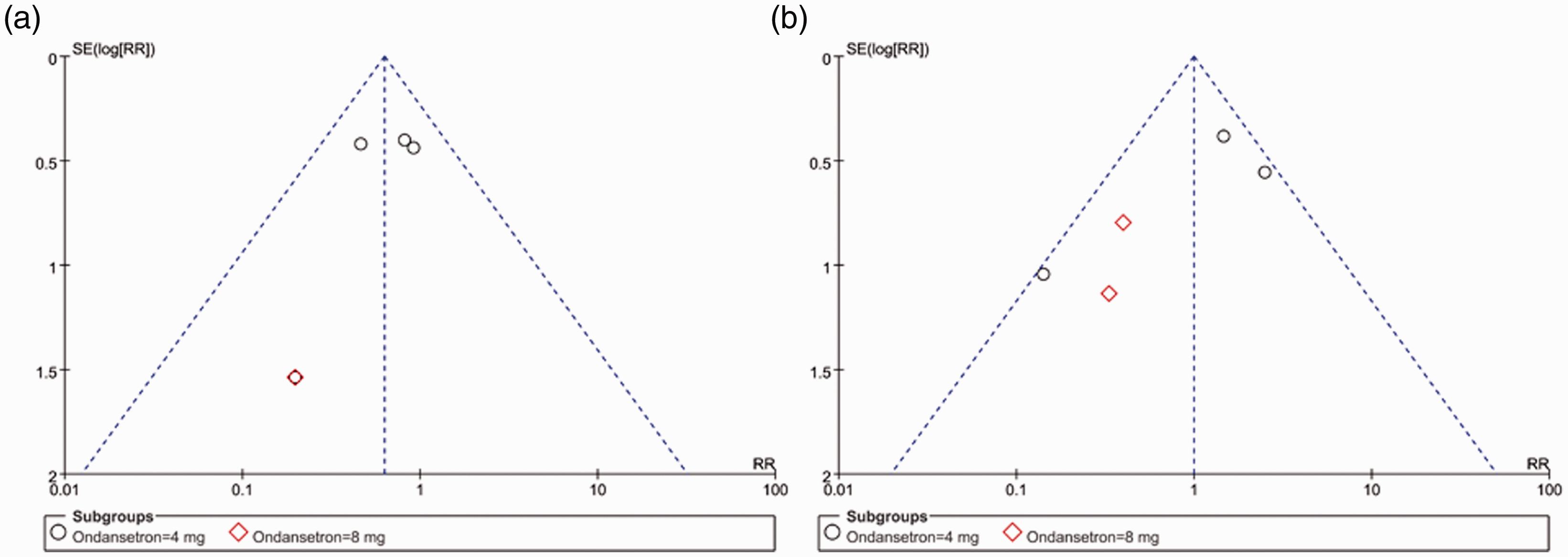
Funnel plot of studies included in the meta-analysis: (a) postoperative nausea (PON) at 24 to 48 hours after laparoscopic surgery; (b) postoperative vomiting (POV) at 0 to 2 hours after laparoscopic surgery.
Discussion
PONV remains an important issue in clinical procedures involving anesthesia, and particularly in laparoscopic surgery. 26 In addition to its strong association with patient dissatisfaction, PONV may have adverse consequences such as unexpected hospital admission, delayed recovery, and delayed return to work. 3 Therefore, the prevention of PONV after laparoscopic surgery is typically prioritized to the same extent as is relief of postoperative pain. 27
Previous meta-analyses compared ramosetron and ondansetron as prophylactic treatment for PONV.28,29 However, the clinical value of these previous meta-analyses remains uncertain because of the inclusion of different types of surgery, which was associated with an increased risk of bias. In the present meta-analysis, we specifically evaluated the effects of ramosetron and ondansetron for the prevention of PONV after laparoscopic surgery. Our findings are highly relevant as they represent the first separate comparison of the effects of 0.3 mg ramosetron versus different doses of ondansetron (4 or 8 mg) for the prevention of PONV after laparoscopic surgery. Our results indicate that in comparison with ondansetron, ramosetron yielded a statistically significant reduction in the incidence of PON and POV during the first 24 to 48 hours after laparoscopic surgery. Our findings were in part consistent with those of previous meta-analyses.28,29 Our subgroup analysis indicated that ramosetron 0.3 mg significantly reduced the incidence of PON within first the 2 hours after laparoscopic surgery when compared with ondansetron 4 mg. Additionally, during the first 24 to 48 hours after laparoscopic surgery, ramosetron showed a tendency towards more effective reduction of POV compared with ondansetron. In contrast, no statistical difference was observed between ramosetron 0.3 mg and ondansetron 8 mg for the prevention of PON or POV during any time interval within the first 48 hours after surgery. Furthermore, no inter-group differences were observed in the incidence of adverse events such as headache, dizziness, and drowsiness. Paventi et al. 30 reported that single-dose ondansetron 8 mg was more effective than ondansetron 4 mg for prevention of PONV after laparoscopic cholecystectomy, while Ryu et al. 19 showed that the effects of ondansetron 8 mg were comparable to those of ramosetron 0.3 mg. Taken together with these earlier reports, our results strongly indicate that the antiemetic effect of ramosetron 0.3 mg is superior to that of ondansetron 4 mg and not inferior to that of ondansetron 8 mg.
Many researchers consider nausea to be induced via a wide range of irritating events in the cerebral cortex, nucleus solitaries, nerve endings in the stomach or duodenum, and chemoreceptor trigger zone (CTZ), thus stimulating vomiting centers in the brain that control nausea and vomiting. 31 However, the exact mechanism by which pneumoperitoneum induces PONV remains unclear. Previous evidence suggests that carbon dioxide plays a central role in the development of PONV after laparoscopic surgery, as do the activation of neurogenic pathways via splanchnic pressure and traction reflexes, rapid peritoneal expansion, and increased blood pressure in the peritoneal cavity after gas insufflation.32–34 These mechanisms activate 5HT3Rs by inducing the release of emetogenic substances such as serotonin or other neurotransmitters. 3 Histamine and acetylcholine are vital neurotransmitters detected in the vomiting center, while 5-hydroxytryptamine and dopamine are vital neurotransmitters in the CTZ. Ramosetron has a higher affinity for 5HTRs than ondansetron does, and this high affinity may partly explain why ramosetron 0.3 mg yielded significant reductions in POV relative to ondansetron 4 mg in the present analysis.
This study had several notable strengths. First, our meta-analysis was based on rigorous methodology, as all identified studies were RCTs. Second, the studies included in the analysis were assessed to be of a relatively high level of quality and fulfilled our predefined inclusion criteria. Third, the baseline characteristics of the patients included in the RCT were largely comparable, suggesting that the overall patient population was generally representative.
Despite the evidence favoring ramosetron provided by the data included in this meta-analysis, several potential limitations should be mentioned. First, the literature search was limited to studies published in the English language, which might have contributed to language bias. Second, only six RCTs were included, which limited our ability to perform additional subgroup analyses of some outcomes. Therefore, we could not determine the source of heterogeneity. Third, some of the included studies had relatively small sample sizes, which might have affected the reliability of the conclusions. Finally, genetic variations among individuals might contribute to differences in response to the same form of antiemetic therapy. However, our meta-analysis only included RCTs from a single region (Asia), which may have contributed to selection and reporting biases.
Conclusion
The results of our meta-analysis indicate that ramosetron 0.3 mg was superior to ondansetron 4 mg and not inferior to ondansetron 8 mg for the prevention of PONV in patients after laparoscopic surgery. However, further well-designed, large, multi-center RCTs are needed to confirm these findings.
Footnotes
Authors' contributions
Yiping Li contributed to the study design and writing of the manuscript. Ruiming Deng and Juan Zhou performed the data collection and data analysis. Yuan Chen and Aiping Ouyang edited the manuscript. All authors read and approved the final version of the manuscript.
Consent for publication
Not applicable.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
