Abstract
Objective
To investigate the effect of combined prophylactic ramosetron and total intravenous anaesthesia (TIVA) on postoperative nausea and vomiting (PONV), compared with sevoflurane anaesthesia without prophylactic antiemetics, in female patients undergoing thyroidectomy.
Methods
Female patients were randomized between the sevoflurane group (anaesthesia maintained with sevoflurane) or TIVA + ramosetron group (TIVAR; 0.3 mg ramosetron just before anaesthesia induction, remifentanil and propofol anaesthesia). Incidence and severity of PONV and use of rescue antiemetics were recorded during the first 24 h after surgery.
Results
In the early postoperative period (0–6 h), the incidence of PONV, severe emesis and rescue antiemetic use were significantly lower in the TIVAR group (n = 36) than in the sevoflurane group (n = 36). In the late postoperative period (6–24 h), the incidence of severe emesis was significantly lower in the TIVAR group than in the sevoflurane group.
Conclusions
A combination of TIVA and prophylactic ramosetron decreases early PONV and late postoperative severe emesis compared with sevoflurane anaesthesia.
Introduction
Postoperative nausea and vomiting (PONV) is a common adverse outcome of surgery and anaesthesia 1 that causes more distress than postoperative pain. 2 Several factors are known to increase the risk of PONV, including patient characteristics (sex; smoking status; history of motion sickness or PONV), anaesthetic technique, and type of surgery.1,3 The incidence of PONV after thyroidectomy is 64–71% following the use of inhalational anaesthesia without prophylactic antiemetics.4–7
Total intravenous anaesthesia (TIVA) with propofol reduces the incidence of PONV compared with inhalational anaesthesia,4–10 especially in women.5–7 This antiemetic effect is limited to the early postoperative period, however,7–10 and 35–40% of patients will still experience PONV.5–7,10 A multimodal PONV management strategy requires long-acting antiemetics. 11
Antagonists to 5-hydroxytryptamine receptor 3 (5-HT3) are commonly used to prevent PONV.12–15 Ramosetron has more avid 5-HT3 receptor affinity and longer duration of action than ondansetron and granisetron,16,17 and has a superior antiemetic effect to palonosetron. 18 The efficacy of TIVA with propofol and remifentanil or ramosteron on PONV has been demonstrated in several studies,7,8,13–15 but this combined effect is not well studied in patients undergoing thyroidectomy without opioid-based patient-controlled analgesia.
The present study was designed to investigate the combined effects of prophylactic intravenous ramosetron and TIVA with propofol and remifentanil on PONV in female patients undergoing thyroidectomy, compared with sevoflurane inhalational anaesthesia without use of prophylactic antiemetics.
Patients and methods
Study population
The study prospectively recruited female euthyroid patients scheduled for thyroidectomy under general anaesthesia at Ajou University Hospital, Suwon, Republic of Korea between March 2013 and March 2014. Patients were required to be American Society of Anesthesiology physical status I or II and aged 20–60 years. Exclusion criteria were: >30% over ideal body weight; renal disease; hepatic disease; history of adverse reaction to 5-HT3 antagonists; antiemetic use within 24 h prior to surgery.
Written informed consent was obtained from all patients and the study protocol was approved by the Ajou University Hospital Institutional Review Board. Patients were randomly allocated between two groups (sevoflurane group [control] or TIVA + ramosetron group [TIVAR]) using computer-generated random numbers. A medical history including smoking, motion sickness and PONV was taken and demographic data were recorded.
Anaesthesia
In the sevoflurane group, anaesthesia was induced with 4–5 mg/kg thiopental sodium administered via intravenous (i.v.) injection and maintained with sevoflurane in 50% oxygen. In the TIVAR group, 0.3 mg ramosetron was administered i.v. just before anaesthesia induction. Anaesthesia was induced and maintained with i.v. remifentanil (target blood concentration 3.5–4.5 ng/ml) and propofol (target blood concentration 3.0–4.5 µg/ml). Blood concentrations of propofol and remifentanil were controlled using Orchestra™ (Fresenius Kabi, Bad Homburg, Germany).
Anaesthesia continued in all patients according to institutional standards: patients were given 0.6 mg/kg i.v. rocuronium to facilitate tracheal intubation, anaesthesia depth was monitored with Bispectral Index™ Monitor (Aspect Medical Systems, Norwood, MA, USA) and ventilation was mechanically controlled with oxygen/air mixture (fractional inspired oxygen 0.5), adjusted to maintain end tidal carbon dioxide 35–40 mmHg throughout surgery.
After surgery, muscle relaxation was antagonized with 0.002 mg/kg i.v. glycopyrrolate and 0.03 mg/kg i.v. pyridostigmine. Ketorolac tromethamine (Keromin®, Hana Pharm Co., Seoul, Republic of Korea) was used for postoperative analgesia (30 mg i.v. as required).
Study assessments
Postoperative assessments were made at 1 h in the postanaesthesia care unit and at 6 h and 24 h in the general ward by interview and medical record reviews (by H.B.J. and S.Y.L.). Nausea was defined as a subjective, unpleasant sensation associated with awareness of the urge to vomit. Nausea severity was evaluated using a numerical scale ranging between 0 and 10 (0, no nausea; 10, most severe nausea). Retching was defined as the laboured, spastic, rhythmic contraction of respiratory muscles without expulsion of gastric contents and was regarded as vomiting. Vomiting was defined as the forceful expulsion of gastric contents from the mouth. Severe emesis was defined as the presence of nausea (≥7) or retching/vomiting. The rescue antiemetic, i.v. metoclopramide (10 mg) was administered when nausea of ≥5 persisted, or at the patient’s request. Pain scores were measured using an 11-point rating scale (0, no pain; 10, most severe pain). Any other adverse events were also recorded.
Statistical analyses
Sample size was determined using a power analysis based on the following assumptions: incidence of PONV (nausea, retching or vomiting) after thyroidectomy would be 63%, and a decrease from 63% to 25% would be considered clinically significant. The analysis showed that 31 patients per each group would be sufficient to detect a between-group difference with an α-error of 0.05 and a power (1 -β) of 0.8. The study therefore aimed to include 36 patients per group to account for possible drop-outs.
Data were presented as mean ± SD or n (%). Between-group differences were analysed with Student’s t-test for parametric data (age, weight, height, anaesthesia time, operation time) and χ2-test for discrete variables (history of motion sickness/PONV/smoking, presence of PONV, adverse events and severe emesis). Statistical analyses were performed using SPSS® version 17.0 (SPSS Inc., Chicago, IL, USA) for Windows®. P-values < 0.05 were considered statistically significant.
Results
The study included 72 women (mean age, 42.9 ± 8.6 years; mean weight, 58.5 ± 8.5 kg; Figure 1), randomised to either the sevoflurane group (n = 36) or the TIVAR group (n = 36). There were no significant between-group differences in demographic or surgical characteristics (Tables 1 and 2).
Chart indicating the flow of patients through the study investigating postoperative nausea and vomiting in female patients undergoing thyroidectomy. Demographic characteristics of female patients included in a study to evaluate the combined effects of prophylactic intravenous ramosetron and total intravenous anaesthesia with propofol and remifentanil (TIVAR) on postoperative nausea and vomiting (PONV) following thyroidectomy, compared with sevoflurane inhalational anaesthesia without use of prophylactic antiemetics. Data presented as mean ± SD or n (%). No statistically significant between-group differences (P ≥ 0.05; Student’s t-test or χ2-test). Surgical and anaesthetic data of female patients undergoing thyroidectomy with total intravenous anaesthesia with propofol and remifentanil (TIVAR) and prophylactic intravenous ramosetron, or sevoflurane inhalational anaesthesia without use of prophylactic antiemetics. Data presented as n (%) or mean +/− SD. No statistically significant between-group differences (P ≥ 0.05; χ2-test).


Incidence of postoperative nausea and vomiting (PONV) and adverse events in female patients following thyroidectomy with total intravenous anaesthesia with propofol and remifentanil (TIVAR) and prophylactic intravenous ramosetron, or sevoflurane inhalational anaesthesia without use of prophylactic antiemetics.
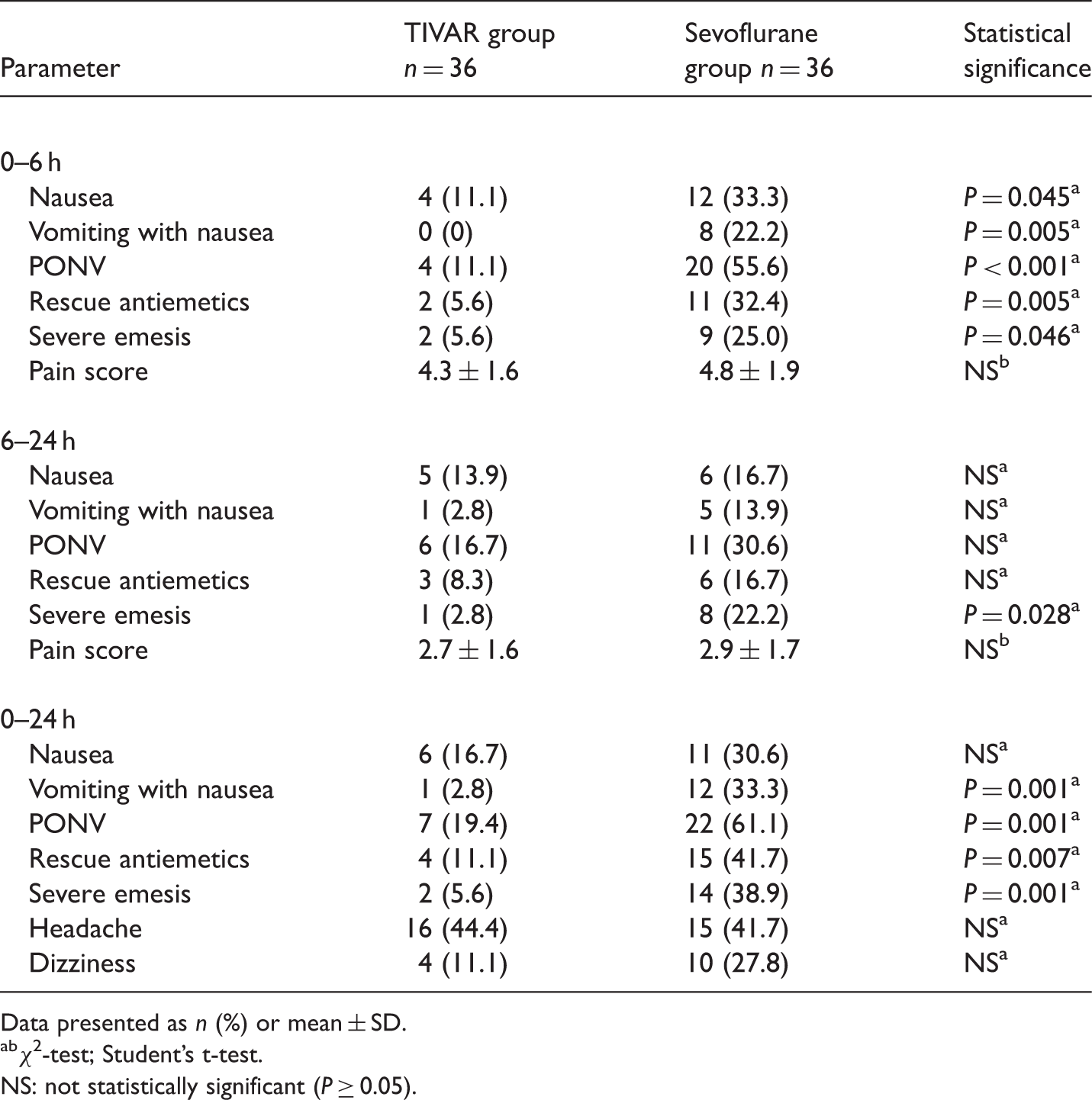
Data presented as n (%) or mean ± SD.
abχ2-test; Student’s t-test.
NS: not statistically significant (P ≥ 0.05).
Overall, in the 0–24 h postoperative period, the incidence of vomiting (P = 0.001), PONV (P = 0.001), severe emesis (P = 0.001) and rescue antiemetic use (P = 0.007) were each significantly lower in the TIVAR group than in the sevoflurane group. There were no significant between-group differences in pain score or incidence of adverse events at any time (Table 3).
Discussion
The present study found that the combined use of TIVA (propofol–remifentanil) with ramosetron decreased the incidence of PONV (during the first postoperative 24 h) to 19.4% from 61.1% with sevoflurane inhalational anaesthesia. The aetiology of PONV after thyroidectomy is unknown, but factors including sex, age and intense vagal stimulation (through surgical handling of the neck structure) are known to be involved. 4 Other risk factors include obesity, history of motion sickness, previous PONV, smoking history and anaesthetic technique.1,3 There were no between-group differences in patient demographics and surgical details in the present study, therefore the difference in PONV incidence can be attributed to anaesthetic technique and antiemetic (ramosetron) administration.
Inhalational anaesthesia is a principal cause of PONV, especially during the early postoperative period.19,20 The incidence of PONV following sevoflurane anaesthesia was 61.1% in the present study, a finding compatible with the results of others.4–7
The use of TIVA with propofol and remifentanil is known to reduce the incidence of PONV.7,8,21 Propofol has antiemetic properties, acting on area postrema neurons via the γ-aminobutyric acid (GABA)A receptor to reduce activity and serotonin levels in the area postrema and cerebrospinal fluid.22,23 Remifentanil is a nonaccumulative ultrashort-acting opioid with known antiemetic effects. Interestingly, the combination of remifentanil and sevoflurane does not increase the incidence of PONV compared with sevoflurane alone. 24
Although propofol based TIVA is associated with a lower incidence of PONV, its effect is limited to the early postoperative period. The choice of anaesthetic technique (volatile vs. TIVA) may be the main risk factor for early (0–2 h) but not late PONV (2–24 h). 19 In several types of surgery, the antiemetic effect of propofol-based TIVA was limited to within 6 h postoperatively.7–9 We have previously demonstrated that TIVA with propofol/remifentanil significantly reduced the incidence of PONV compared with sevoflurane anaesthesia at 0–6 h postoperatively (30.5% vs 55.9%) but not 6–24 h postoperatively (16.9% vs 22.0%). 7 Others have reported that 30–40% of patients experience PONV after propofol-based TIVA,7,8,14 therefore the use of other antiemetics as well as TIVA is required to prevent PONV. It is generally recognised that a multimodal approach is more effective in preventing PONV compared with other strategies. 25
Ramosetron is a 5-HT3 receptor antagonist that is used as an effective antiemetic in various types of surgery. 13 It has higher 5-HT3 receptor affinity and longer duration of action than other 5-HT3 receptor antagonists, with longer elimination half-life (9.3 h) than ondansetron (3.5 h), granisetron (4.9 h) and alosetron (3.0 h).16,17 In the present study, the use of TIVA with ramosetron (TIVAR) resulted in a lower incidence of nausea, vomiting, PONV, severe emesis and use of rescue antiemetics in the early postoperative period (0–6 h) compared with the sevoflurane group. The use of TIVA without prophylactic antiemetics decreased the incidence of PONV by 45% (without reducing the incidences of nausea and rescue antiemetic use) compared with sevoflurane anaesthesia. 7 Taken together, these data suggest that the addition of ramosetron to TIVA may decrease the incidence and severity of PONV compared with inhalational anaesthesia.
During the late postoperative period (6–24 h) in the present study, only the incidence of severe emesis was significantly decreased in the TIVAR group compared with the sevoflurane group. Despite the long half life of ramosetron, it did not produce a sufficient antiemetic effect in the late postoperative period. Although the combined effects of changing anaesthetic technique (inhalational anaesthesia to TIVA) and prophylactic ramosetron administration are mainly limited to the early postoperative period, the effect on severe emesis was extended to later in the postoperative period. This result is consistent with a study that showed a decrease in early PONV and late postoperative vomiting, but not late postoperative nausea, with the use of ramosetron. 19
A major limitation of our study was the lack of a TIVA control group in which patients did not receive prophylactic ramosetron. This is partly offset by the findings of our previous study that evaluated PONV following TIVA or sevoflurane anaesthesia. 7
In conclusion, a combination of TIVA and prophylactic ramosetron administration appears to decrease early PONV and late severe emesis, compared with sevoflurane anaesthesia.
Footnotes
Declaration of Conflicting Interest
The authors declare that there are no conflicts of interest.
Funding
This study was funded by Astellas Pharma Korea Inc. (AKR-NA-2012-01)
