Abstract
Primary thyroid lymphoma (PTL) is a very rare type of thyroid malignant tumor. PTL coexisting with papillary thyroid carcinoma (PTC) is even scarcer and can be easily overlooked. We present our experience of the diagnosis and treatment of a 37-year-old woman with primary thyroid diffuse large B cell lymphoma complicated with PTC. We also considered this case in the context of previous reports. The results indicated that the incidence of concurrent Hashimoto’s disease varied among patients with different lymphoma subtypes, with the highest incidence in patients with mucosa-associated lymphoid tissue lymphoma. Furthermore, thyroid cancer and thus the combination of PTL and PTC were more common in women.
Keywords
Introduction
Primary thyroid lymphoma (PTL) is an uncommon type of thyroid lymphoma accounting for only about 1% to 5% of thyroid malignant tumors and 1% to 2% of extranodal lymphomas.1,2 Its clinical manifestations are variable, but it is usually characterized by a rapidly enlarging, painless thyroid mass accompanied by compressive symptoms, shortness of breath, stridor, dysphagia, and hoarseness.
In contrast, papillary thyroid carcinoma (PTC) is one of the most frequent thyroid cancers and accounts for nearly 70% of all thyroid malignant tumors. However, the simultaneous occurrence of PTL and PTC is very rare, and few cases have therefore been reported.
In this study, we report a rare case of concomitant primary thyroid diffuse large B cell lymphoma (DLBL) and PTC. In addition, we systematically reviewed the pertinent literature and identified reports of a further 16 patients. We further explored and summarized the characteristics of these diseases based on the current and previous cases.
Case report
A 37-year-old woman with dyspnea and swallowing difficulties caused by a rapidly expanding mass in her neck over the previous 4 weeks was referred to the First Affiliated Hospital of Xi’an Jiao Tong University. The patient had no familial history of thyroid disease, immunodeficiency, or prior malignancy. Physical examination revealed no abnormalities in the superficial lymph nodes, liver, or spleen, but a palpable, tough mass was identified in the right neck.
A computed tomography (CT) scan revealed a 3.0 × 3.0 cm thyroid with a density similar to that of muscle, in a moderately narrowed airway. A thoraco-abdominal CT scan detected no irregularities in other locations, and bone marrow aspirate and cerebrospinal fluid analyses also showed no pathological symptoms.
Ultrasound-guided fine needle aspiration (FNA) of the thyroid was conducted. Ultrasound evaluation revealed diffuse homogeneous enlargement of the right thyroid lobe to 3.2 cm in diameter. Ultrasound-guided FNA with rapid on-site evaluation was implemented as described previously, 3 and lobectomy of the right thyroid gland was performed.
Hematoxylin and eosin staining of the lobectomy sample showed large, atypical lymphocytes intermingled among the main cell population. The large immature lymphoid cells were roundish and smaller compared with the normal mature lymphoid cells. Moreover, chromatin accumulation was seen in the nucleus of the large immature lymphoid cells, the nuclear membranes were irregular, and mitoses were increased (Figure 1a). Immunohistochemical staining suggested that the lymphoma was positive for CD20, Ki-67 (90%), and Bcl-6, and negative for CD3, CD10, Mum-1, and molecular-oriented germinal center phenotype. Hematoxylin and eosin staining demonstrated the presence of a PTC in the thyroid gland, with the PTC cell nuclei being enlarged and oval, and showing nuclear features including powdery chromatin, nuclear grooves, and small nucleoli (Figure 1b and 1c).
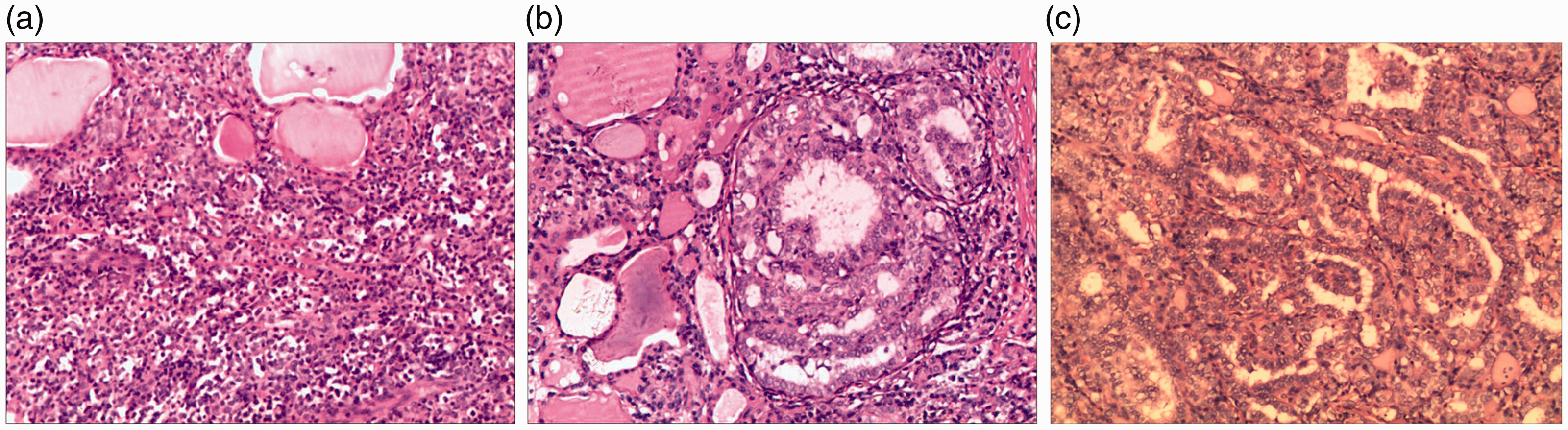
(a) Immature lymphoid cells were roundish and smaller, with chromatin accumulation in the nucleus. Arrow indicates lymphoma cells in thyroid tissue (100× magnification). (b, c) Papillary thyroid cancer cell nuclei were enlarged and oval (100× magnification). (Hematoxylin and eosin staining).
The patient received six cycles of chemotherapy including cyclophosphamide, doxorubicin, vincristine, and prednisone (CHOP). The subsequent 1-year regular follow-up revealed no pathological characteristics and no signs of recurrence.
This case report was approved by the First Affiliated Hospital of Xi’an Jiao Tong University (Xi’an, China) and written informed consent was provided by the patient.
Discussion
A retrospective survey of 1,104,269 tumor patients found an the incidence of multiple primary cancers of 0.73% to 11.7%, with a higher prevalence in the elderly. 4 The diagnosis of multiple primary cancers is based on the international standards developed by Warren and Gates in 1932. 5 Although the coexistence of PTL and PTC is rare, there have been a few previous reports.6,7 The current patient had two independent malignant tumors each with unique characteristics, as confirmed by histological and pathological examinations and consistent with the diagnostic standards of primary cancers. We compared the clinical characteristics of the current and previously reported cases (Table 1).
Comparisons among different lymphoma subtypes.

Values given as number (%). Differences between lymphoma subtypes were analyzed by Fisher’s exact tests. MALT, mucosa-associated lymphoid tissue; DLBL, diffuse large B cell lymphoma; SLL, small lymphocytic lymphoma.
Most primary lymphomas in previously reported patients with coexisting PTL and PTC were non-Hodgkin B-cell lymphomas (NHLs), of which approximately two-thirds were associated with Hashimoto’s thyroiditis. 8 Hashimoto’s thyroiditis was present in 13/16 patients (81.25%), including in all patients with mucosa-associated lymphoid tissue (MALT) lymphoma. The incidence of Hashimoto’s thyroiditis differed significantly among the four lymphoma groups: MALT, DLBL, MALT + DLBL, and small lymphocytic lymphoma (P = 0.014, Fisher’s exact test). Among all the patients, 14 (87.5%) had normal thyroid function, with no native lymphoid tissue. The pathogenesis of PTL is currently poorly understood and it has been suggested to be correlated with virus infection and immune deficiency. Hashimoto’s thyroiditis, as a chronic autoimmune thyroiditis, might also have an important connection with PTL. According to a unitarian theory of pathogenesis, chronic, antigenic stimulation of lymphocytes could gradually induce monoclonality of H-chains and their progression toward DLBL, while inflammation could induce the synthesis of tumorigenic compounds, such as cyclooxygenase-2, which has been detected in both thyroid epithelial neoplasms and Hashimoto’s thyroiditis. Both of the above factors may result in lymphomas in patients with autoimmune disorders. 9 In addition, Trovato et al. 10 recommended the importance of regular follow-ups to ensure an early diagnosis, considering the increased risk of neoplasms in patients with long-standing Hashimoto’s thyroiditis and nodular lesions.
The most common NHLs involving the thyroid include DLBL and extranodal marginal zone B-cell lymphoma, while primary Burkitt’s lymphoma and T-cell lymphoma of the thyroid are extremely rare, with only a few isolated case reports.11,12 However, we found that MALT lymphoma (62.5%) was more likely than DLBL (25%) to coexist with PTC. The reasons for this apparent discrepancy are unclear. Considering that DLBL could develop from MALT lymphoma, and that these two lymphoma subtypes were detected in the same gland in a previous study, 13 their coexistence could contribute to an earlier diagnosis.
The incidence of thyroid cancer has been consistently higher among women than men for several decades. 14 Among the current and previous cases studied here, 11 (68.75%) patients with thyroid cancer were female, confirming that women are more likely to be affected by PTC and DLBL than men.
The main treatment for PTC is surgery, but a comprehensive treatment strategy is needed for coexisting PTL and PTC. Some authors have suggested that surgical resection, radiotherapy, and combined chemotherapy may be important factors in improving the prognosis of these patients. 15
All patients in this study and review had prolonged survival times, except for one patient with triple primary cancers (primary thyroid MALT lymphoma, DLBL, and PTC). The shortest survival times were observed in patients with larger nodules and in older patients. The current patient was relatively young and had a relatively small lesion, and accordingly had a good prognosis with no recurrence within the following year after treatment.
In conclusion, despite the rarity of coexisting primary thyroid DLBL and PTC, patients with this combination should be thoroughly evaluated. The current and previous cases highlight the differences in the incidence of Hashimoto’s thyroiditis among patients with different lymphoma subtypes, with the highest incidence associated with MALT lymphoma. Notably, our review also showed that women are more vulnerable to thyroid carcinoma than men.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
