Abstract
Objective
To reveal the correlation between APACHE III score and sleep quality in patients in the intensive care unit (ICU).
Methods
This prospective, observational study included patients aged ≥18 years, who had been admitted to an integrated ICU for ≥48 h. Age, sex, Pittsburgh Sleep Quality Index (PSQI) prior to ICU, Numeric Rating Scales (NRS), noise, illumination, number of nursing interventions, Richards Campbell Sleep Questionnaire (RCSQ), and APACHE III score during sleep were evaluated.
Results
A total of 124 ICU patients were included, all with APACHE III scores < 60. APACHE III scores were not significantly associated with RCSQ scores. There were significant inverse associations between sleep quality in the ICU and PSQI score prior to ICU (odds ratio [OR] 0.587, 95% confidence interval [CI] 0.365, 0.945) and noise (OR 0.628, 95% CI 0.522, 0.756).
Conclusion
In ICU patients with APACHE III scores below 60 points, APACHE III score was not associated with sleep quality. PSQI score prior to ICU and noise were significantly inversely associated with sleep quality in this ICU patient population.
Introduction
Sleep is a basic physiological requirement of human beings and an essential condition for the recovery of individual intelligence and energy. As a special group, patients in the intensive care unit (ICU) have the characteristics of severe and complex disease, and sleep problems should not be ignored. The prevalence of sleep disturbance in critically ill patients is reported to be more than 50%, 1 and in ICU patients, sleep disorders are closely related to mortality, infection rate and complications. 2 The causes of sleep disorders in ICU patients are not fully understood, but many extrinsic and intrinsic factors have been proposed, such as type and severity of disease, noise, light, pain, drugs used in treatment, mechanical ventilation and frequent nursing interventions.2–4 While the exact relationship between sleep and severity of illness in ICU patients remains uncertain, it is likely important. 5 However, only a limited number of studies have specifically investigated the correlation between severity of illness and sleep quality in ICU patients.
Due to the specific ICU environment and the fact that patients are unconscious, a duty of the therapeutic team is to assess a patient’s sleep. Polysomnography remains the gold standard procedure for qualitative and quantitative sleep assessment in the ICU setting, 6 and using this method, unequivocal sleep disruption has been demonstrated in critically ill patients, characterized by extreme sleep fragmentation, an over-representation of Stage 1 and Stage 2 non-REM sleep, reduced or absent slow-wave sleep and REM sleep, and circadian rhythm abnormalities.7,8 However, polysomnography itself has limitations, for example, electrodes and a registering device may introduce potential disturbances into the examination environment. 9 The Richards-Campbell Sleep Questionnaire (RCSQ) 10 scale is the most widely used among the existing subjective sleep assessment methods, as it is easy to score, concise, and less time consuming, making it an extremely attractive choice for assessing sleep quality in ICU patients. Any inaccuracies linked to subjective evaluation of sleep quality in ICU patients may be related to the effect of sedatives on cognitive function, which may interfere with patient memories of sleep quality. 11 As such, the present study included patients who had not used an analgesic and/or sedative within 24 h of the study.
The Acute Physiologic and Chronic Health Evaluation (APACHE) III scoring system is a predictive scoring system most frequently used to measure the severity of disease and prognosis of patients in the ICU. 12 Based on previous studies, 13 the aim of the present study was to divide patients into three categories according to APACHE III score and mortality rate, as follows: APACHE III score ≤30 points, APACHE III score 31–59 points, APACHE III score ≥60 points. Previous studies have been mostly retrospective and have not excluded the effects of common factors affecting sleep quality.14–17 From the clinical point of view, it is highly problematic to limit or discontinue therapy due to the potential risk of quantitative and qualitative sleep disorders. 14 Thus, the aim of the present study was to explore the correlation between APACHE III score and sleep quality in ICU patients, using a prospective observational design that excluded the effects of common factors affecting sleep quality, such as noise, light, pain, mechanical ventilation and frequent nursing interventions.
Patients and methods
Study population
This prospective observational study was conducted in an integrated ICU of Renmin Hospital of Wuhan University, China, between March 2018 and May 2018. Patients were sequentially enrolled if they met the following inclusion criteria: age ≥18 years; Glasgow coma score ≥14 points, and duration of ICU hospitalization > 48 h. Exclusion criteria were as follows: history or evidence of sleep disorder (e.g. obstructive sleep apnoea); current hearing and speech impairment; craniocerebral injury; mental illness; alcohol consumption ≥50 units per week; Pittsburgh Sleep Quality Index (PSQI) 18 >5 points prior to ICU admission; undergoing mechanical ventilation within 24 h of study assessment; use of analgesic and/or sedative within 24 h of study assessment; delirium (Intensive Care Delirium Screening Checklist [ICDSC] 19 score ≥4 points); and haemodynamic instability (systolic blood pressure < 90 mm Hg after treatment).
The study was approved by the Human Research Ethics Committees for Renmin Hospital of Wuhan University, and written informed consent was obtained from the patients or their legal proxies.
Data collection
The ICU patients were screened daily from Monday to Friday for enrolment into the study. All eligible patients underwent a sleep evaluation for 12 h (from 20:00 h on the first evaluation day to 08:00 h on the second day) at 24 h following admission into the ICU. Clinical data were collected for all included patients to establish a database comprising: age; sex; PSQI score prior to ICU admission; ICDSC score on ICU admission; ICU admission diagnosis; pain level (Numeric Rating Scale [NRS]); 20 noise; illumination; number of nursing interventions (including turning and blood sugar measurements) during the sleep evaluation; RCSQ; and ICDSC and APACHE III score during sleep.
The PSQI score prior to ICU admission was obtained by the investigators (CYW, LZF) once the patient was admitted to the ICU and conscious, and thus, relied on the patients’ recall of sleep status nearly 1 month before admission to the ICU. The ICDSC 19 is the most commonly used instrument for detection of delirium in the intensive care setting. The ICU admission ICDSC scores were obtained by investigators (CYW, LZF) once the patient was admitted to the ICU. Pain scores were obtained using the NRS, which was completed by patients indicating the severity of their pain on a scale with markings from 0 to 10 mm. 20 Noise and light levels next to the patient’s ear and pillow were measured at three time-points (at 20:00 h on the first day, at 00:00 h and at 04:00 h on the second day) using a UT353 digital sound level meter and UT383 mini digital illumination meter (Uni-Trend Technology Co., Dongguan, China), respectively, and a mean value was calculated for each patient. Quality of sleep was measured using the Chinese version of RCSQ. This instrument includes five items, and evaluates perceived sleep depth, sleep latency (time to fall asleep), number of awakenings, efficiency (percentage of time awake) and sleep quality. Each item was scored on a paper-based 100-mm visual analogue scale (VAS). The mean of the five RCSQ items was used as the total score, with higher scores representing an overall perception of better sleep. Patients were requested to appraise their sleep by responding to questions that were read aloud one by one. After each question, patients set a mark on the VAS, or if they could not set the mark themselves, they pointed at the chosen spot with the tip of their finger, and the investigator (CYW, LZF) marked the scale accordingly. The NRS score, noise, illumination, number of nursing interventions, RCSQ, ICDCS and APACHE III score during sleep were completed by the researchers before 12:00 h on the second day of sleep evaluation. Patients with an ICDCS score ≥4 points on ICU admission or during sleep were excluded from the final analyses. APACHE III scores obtained during the sleep evaluation were used to divide the patients into three groups: APACHE III score ≤30 points, APACHE III score 31–59 points, APACHE III score ≥60 points. A patient’s survival status was obtained via phone interview by an investigator (MS) on day 28 following the ICU sleep assessment.
Statistical analyses
Data with normal distribution are presented as mean ± SD, data with non-normal distribution are presented as median (interquartile range), and categorical data are presented as proportion or frequency (percentage). One-way analysis of variance (ANOVA) and Student’s t-test were performed to compare means of normally distributed variables. Mann–Whitney U-test was used to evaluate non-normally distributed variables, and χ2-test was used to analyse categorical variables. When results were statistically significant, the odds ratio (OR) and 95% confidence intervals (CI) were calculated. The relationship between APACHE III score and RCSQ score was determined by correlation analyses, using Pearson's correlation coefficient for normally distributed variables, and Spearman’s rank correlation coefficient for non-normally distributed data. The influencing factors of sleep quality in ICU patients were analysed by univariate logistic regression. All statistical analyses were performed using SPSS statistical software, version 19.0 (IBM, Armonk, NY, USA) and a P value <0.05 was considered statistically significant.
Results
A total of 198 patients were initially enrolled into the study, and following exclusions, 124 patients were included in the final analyses (Figure 1).
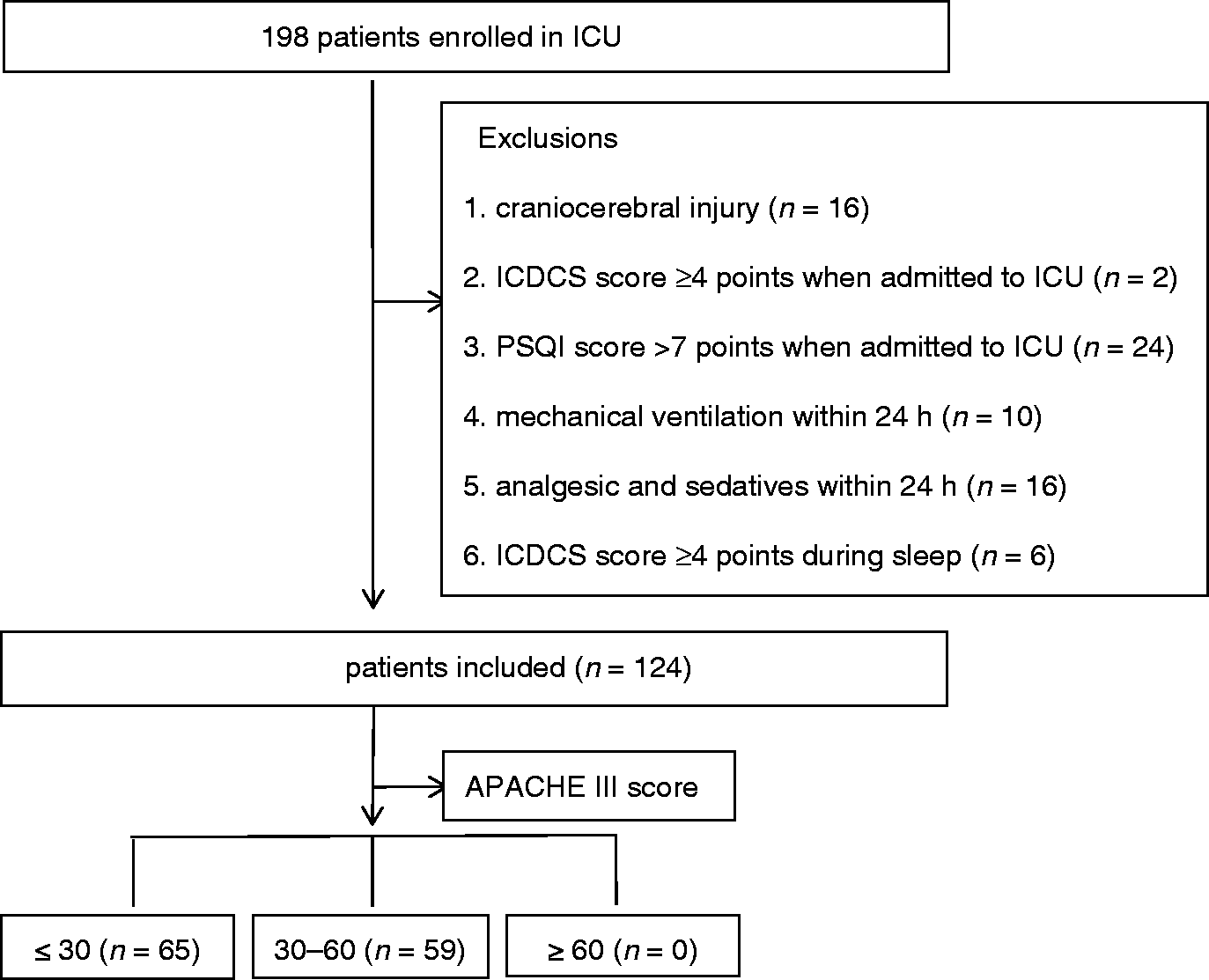
Flow diagram showing case screening, exclusions and inclusions in the final analyses. ICU, intensive care unit; ICDSC, Intensive Care Delirium Screening Checklist; PSQI, Pittsburgh Sleep Quality Index; APACHE, Acute Physiologic and Chronic Health Evaluation.
In the present study population, APACHE III scores during the sleep evaluation were all below 60 points, so the patients were divided into two groups only: APACHE III score ≤30 points (n = 65) and APACHE III score 31–59 points (n = 59; Table 1). All continuous variables showed non-normal distribution; thus, between-group differences were analysed using Mann–Whitney U-test. There were no statistically significant between-group differences in sex, PSQI score, NRS score, levels of noise or illuminance, number of nursing interventions, or ICU admission diagnoses (P > 0.05; Table 1). Patients with APACHE III scores of 31–59 points were significantly older than those with APACHE III scores ≤30 points (P < 0.001). The RCSQ scores were significantly higher in patients with APACHE III scores of 31–59 points compared with patients whose APACHE III scores were ≤30 points (P = 0.030). The mortality rate was also significantly higher in patients with APACHE III scores of 31–59 points verses those with APACHE III scores ≤30 points (P = 0.049). Sepsis was the leading cause for ICU admission (21 patients, 16.9%), followed by cardiovascular serious disease (19 patients, 15.3%), respiratory critical disease (17 patients, 13.7%) and gastrointestinal critical disease (17 patients, 13.7%; Table 1).
Demographic and clinical characteristics of patients in the intensive care unit, grouped according to APACHE III score during sleep.

Data presented as median (interquartile range), or n (%) prevalence.
APACHE, Acute Physiologic and Chronic Health Evaluation; PSQI, Pittsburgh Sleep Quality Index; NRS, Numeric Rating Scales; RCSQ, Richards-Campbell Sleep Questionnaire scale; ICU, intensive care unit.
NS, no statistically significant between-group difference (P > 0.05; Mann–Whitney U-test or χ2-test).
The age characteristics were incomparable between the two groups, therefore, the between-group difference in RCSQ score was suspected to be influenced by age factors. Spearman’s correlation coefficient analysis revealed that there was no statistically significant correlation between APACHE III scores and RCSQ scores (P = 0.073). Subsequent partial correlation analysis was performed to exclude the effects of age, PSQI score, pain, noise, illuminance and nursing intervention on sleep. APACHE III score showed no statistically significant correlation with RCSQ score (P = 0.986) when controlling for age, PSQI score, NRS score, noise, illumination and number of nursing interventions. The distribution of APACHE III and RCSQ scores in ICU patients is shown in Figure 2.
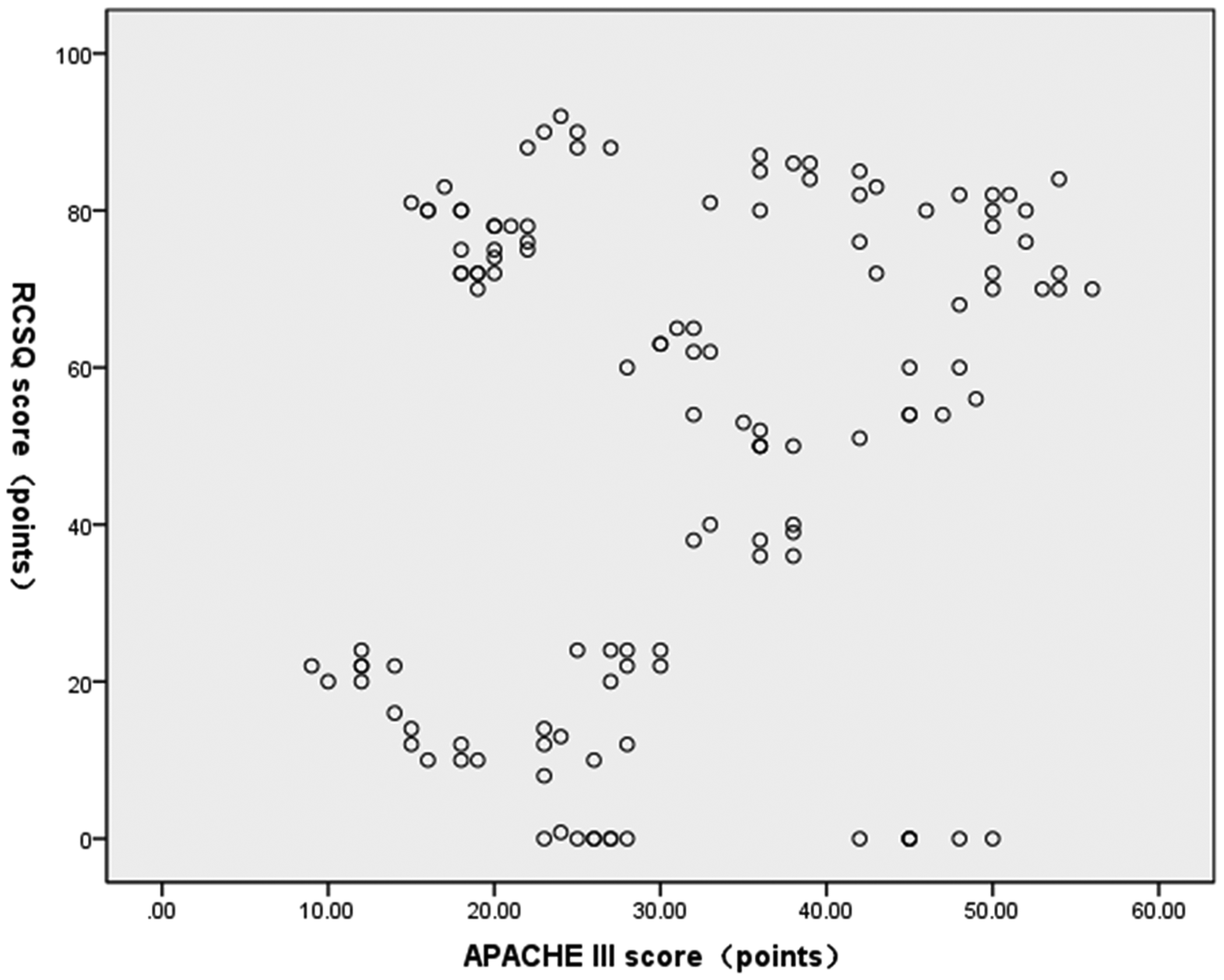
Scatter plot showing the distribution of APACHE III and RCSQ scores of 124 patients in the intensive care unit. APACHE, Acute Physiologic and Chronic Health Evaluation; RCSQ, Richards-Campbell Sleep Questionnaire scale.
Patients were further divided into groups according to RCSQ score obtained during the sleep evaluation: good sleep (RCSQ score ≥76 points) and worse sleep (RCSQ score < 76 points). The proportion of ICU patients with good sleep quality was found to be only 29.8% (37 patients). To further explore potential factors influencing sleep quality, univariate logistic regression was performed on the whole ICU study population (n = 124; Table 2). No statistically significant associations were found between RCSQ score and APACHE III score (P = 0.450), however, there were significant inverse associations between RCSQ score and PSQI score prior to ICU (OR 0.587, 95% CI 0.365, 0.945) and between RCSQ score and noise (OR 0.628, 95% CI 0.522, 0.756).
Univariate logistic regression analyses of factors influencing sleep quality of patients in the intensive care unit (n = 124).

OR, odds ratio; CI, confidence interval; PSQI, Pittsburgh Sleep Quality Index; NRS, Numeric Rating Scales; APACHE, Acute Physiologic and Chronic Health Evaluation.
NS, no statistically significant correlation (P > 0.05).
Patients were also divided into two groups according to noise intensity during the night, as previously described: 21 high noise group (noise score, ≥59 dB; 45 patients) and low noise group (noise score < 59 dB; 79 patients). The proportion of patients with good sleep quality in the high noise group (0%) was significantly lower than in the low noise group (39 patients [49.4%]; P <0.01). Sound levels above 59 dB at night were associated with a higher incidence of poor sleep quality (OR 1.975, 95% CI 1.589, 2.455).
Discussion
The present study found that there was no statistically significant correlation between APACHE III score and sleep quality in ICU patients whose APACHE III scores were below 60 points. PSQI score prior to ICU and noise were significantly inversely associated with sleep quality in ICU patients whose APACHE III scores were below 60 points.
The present study showed no significant correlation between APACHE III score and sleep quality in ICU patients, which was not as expected for this study population. Gabor et al., 15 showed that slow-wave sleep was significantly lower in a mechanically-ventilated ICU patient group compared with healthy participants exposed to the ICU environment, suggesting that critical disease may be a factor affecting sleep quality. It should be noted that mechanical ventilation is known to impede sleep in ICU patients, 22 thus, the present authors speculate that the lower sleep quality in ICU patients may be related to mechanical ventilation, and not necessarily to the severity of disease. A randomized, controlled pilot study in a neurologic ICU showed that patients with unscorable sleep recordings had significantly higher APACHE-II scores. 16 Unscorable ‘sleep’ should be regarded not as sleep per se, but as an electrophysiological sleep-like state, as it may not fulfil the physiologic roles of typical sleep. The authors appeared to infer that higher APACHE II scores were associated with worse sleep quality, 16 but the study was small in size and did not compare common factors affecting sleep quality in patients with different severity of illness. In addition, the study did not describe whether sleep was monitored during the daytime or at night. 16 A cross-sectional study in three respiratory care centres 23 showed that APACHE-II scores were inversely related to the Verran and Snyder-Halpern (VSH) Sleep Scale, 24 in patients who were all mechanically ventilated. 23 Ventilatory modes and settings can both affect sleep quality,22,25 however, the ventilatory modes and settings were not described in detail in the study.
The present research findings are consistent with some published studies. For example, a cross-sectional study in the ICU found that APACHE II and APACHE III scores were not associated with sleep quality (assessed according to a modified Freedman questionnaire) 26 in ICU patients, 14 and a patient survey of sleep quality found no significant correlations between perceived sleep quality (according to the authors’ own questionnaire) and APACHE II score. 17 In both of these studies, sleep quality questionnaires were completed at or after hospital discharge. However, in the present study, sleep quality questionnaires were completed on day 2 of the sleep evaluation. The present study also excluded the effects of common factors affecting sleep quality, such as age, sex, pain, noise, illumination and number of nursing interventions. The age characteristics of the two groups divided by APACHE III score in the present study were incomparable, therefore, partial correlation and logistic regression analyses were employed, and revealed that there were no significant associations between sleep quality in ICU patients and APACHE III score. In this sense, the present findings seem more convincing, however, it should be noted that all patients in the present study had APACHE III scores below 60 points. A multicentre study including 20 988 ICU patients found that APACHE III scores differed between survivors and non-survivors (48 ± 22 and 85 ± 29, respectively). 27 Based on these findings, the present authors infer that the disease severity in the present study population was relatively mild, and this may have been due to the fact that patients undergoing mechanical ventilation within 24 hours, and those with haemodynamic instability, were excluded. Thus, the correlation between APACHE III score and sleep quality in more seriously ill patients requires further exploration. The present research findings may be due to the variety and complexity of diseases associated with patients in the ICU, whose severity may have different effects on sleep quality. As such, the effects on sleep quality of various diseases observed in ICU patients also requires further study.
The present results are relevant to improving sleep strategies, and imply that more attention should be paid to factors other than illness severity, that may affect sleep quality. Critically ill patients in the ICU are exposed to a wide range of disturbances including noise, light, diagnostic and therapeutic procedures, mechanical ventilation, medication, and the critical illness itself. All of these factors may disturb normal sleep, but it remains unknown which of these plays the most important role in sleep disruption in critically ill patients. 28 Therefore, the present research analysed common factors affecting sleep quality using univariate logistic regression, and showed that PSQI score prior to ICU admission and noise were significantly inversely associated with sleep quality in ICU patients whose APACHE III score was below 60 points. These results are similar to those of Stewart et al., 29 who found that sleep quality prior to ICU admission was inversely associated with ICU sleep quality. 29 The role of noise in disturbing sleep in critically ill patients has been discussed previously. 30 For example, Freedman et al. 8 found that environmental noise was responsible for <20% of awakenings, while sound levels above 77 dB have been associated with awakenings for 60% of the time during the night. 21 The present study showed that the incidence of poor sleep quality increased with sound levels above 59 dB at night, which implies that sound level intensity severely affects sleep quality in ICU patients. Taken together, the results indicate that PSQI scores should be assessed and noise monitoring should be strengthened once the patients enter ICU. More attention should be paid to those with higher scores, and efforts should be made to improve the sleep quality of patients within the ICU.
The results of the present study may be limited by several factors. First, subjective indices were used to evaluate sleep quality, which may have memory bias that affects the evaluation of sleep quality. Study objectivity could be enhanced by the use of multiple evaluation methods with higher reliability, such as sleep monitors, to analyse the patients’ quality of sleep. Secondly, the sample size was relatively small. Although a significant relationship was not found between APACHE III and RCSQ scores in patients with APACHE III scores of 31–59 points, there were higher median (interquartile range) values that were heading towards statistical significance. The authors speculate that with a larger sample size, the statistical results may be different, thus, a prospective study with a larger sample size is required to elucidate the present results. In addition, not all of the factors that disturb sleep (such as depression) were collected. Finally, the APACHE III scores were less than 60 in patients included in the present study, and the severity of disease was relatively mild, which does not reflect the overall perspective of illness severity in ICU patients.
In conclusion, there was no significant correlation between APACHE III score and sleep quality in ICU patients whose APACHE III score was less than 60 points. The correlation between APACHE III score and sleep quality in more seriously ill patients requires needs further exploration. PSQI score prior to ICU and noise were significantly inversely associated with sleep quality in ICU patients whose APACHE III score was less than 60 points. Therefore, PSQI scores should be assessed and noise monitoring should be strengthened once the patients enter ICU. More attention should be paid to those with higher scores, and efforts should be made to improve the sleep quality of patients within the ICU.
Footnotes
Acknowledgements
The authors would like to thank Qiao Huang, who participated in the design of the study and performed the statistical analysis, and Zheng-le Zhang, who helped to draft the manuscript.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
The present study was supported by National Natural Science Foundation of China grant (no. 81770089).
