Abstract
Objective
To investigate the relationship between health insurance status and outcomes of septic acute kidney injury (AKI) related hospitalizations in an intensive care unit (ICU) in Ningbo, China.
Methods
For this retrospective study, information was extracted from patients notes and billing records for patients >18 years of age with a diagnosis of AKI admitted to the ICU department, Ningbo First Hospital from April 2013 to March 2018.
Results
Of the 368 patients with sepsis admitted to ICU, 167 (45%) developed AKI; 95 patients were insured and 72 were uninsured. Compared with insured patients, uninsured patients were younger, had higher Acute Physiology and Chronic Health Evaluation II (APACHE II) and Sequential Organ Failure Assessment (SOFA) scores, but had less catheter interventions and received less renal replacement therapy (RRT). Results from a multivariate analysis showed that independent predictors of ICU mortality were age, APACHE II scores, MODS scores, use of RRT and lack of insurance.
Conclusions
Uninsured patients with septic AKI were younger, stayed a shorter time in ICU, had higher illness severity scores and a higher ICU mortality than insured patients. Importantly a major risk factor for ICU mortality in this group was lack of insurance.
Introduction
In recent years, China’s economy has grown rapidly. However, China’s health care system is struggling to keep pace with the country’s economic growth.1,2 Accessibility and affordability of healthcare is a major problem. 3 The huge gap between the development of health care systems and economic growth prompted the Chinese government to implement a system-wide healthcare reform plan and provide universal health insurance for 1.3 billion people.4,5 However, the universal insurance coverage faces many challenges including unequal utilization and allocation of health services, increased medical expenditures and large disparities between urban and rural areas. 6
Acute kidney injury (AKI) is a common disease in critically ill patients. The prevalence of AKI in the intensive care unit (ICU) is between 35–60% with an associated mortality rate of 30– 70%. 7 In China in 2013, the costs of hospitalisations associated with AKI were estimated to be US$13 billion. 8 More than half of all AKI cases are sepsis-related and sepsis is a contributing factor in more 20% of ICU patients with AKI.9,10 Although the increase in private healthcare insurance in China may lead to the provision of more organized interventions for patients with septic AKI, such as renal replacement therapy (RRT), 11 access to healthcare and utilization of health insurance for migrant workers faces barriers. 12 A study from Shenzhen, China, showed that 55% of migrant workers did not have health insurance and 62% did not visit a doctor when they were ill. 13
The aim of this current study was to investigate the relationship between health insurance status and outcomes of septic AKI related hospitalizations in an ICU unit in Ningbo, China. We hypothesized that uninsured patients with septic AKI would be more severely ill and have a higher ICU mortality rate than insured patients with septic AKI.
Patients and methods
This retrospective study included patients over 18 years of age with a diagnosis of AKI admitted to a mixed adult ICU department, Ningbo First Hospital, Ningbo, China from April 2013 to March 2018. Patients who had chronic kidney disease and/or had received regular dialysis irrespective of the cause were exclude from the study. AKI was defined according to RIFLE criteria (i.e., Risk, Injury, Failure, Loss, End stage kidney disease). 14 Chronic kidney disease was defined according to National Kidney Foundation guidelines and was present if the patient had a glomerular filtration rate <60 ml/min/1.73 m2 or kidney injury for more than three months. 15 Sepsis and septic shock were defined according to consensus guidelines. 16
Patient data were extracted from the patients’ medical records and a database containing billing information by one of the investigators [G.C.]. Demographic and admission data were recorded on data collection tables. Interventions, RRT requirements, ICU length of stay (LOS), hospital-LOS, development of septic shock, multiorgan dysfunction syndrome (MODS) 17 and ICU mortality were recorded. In addition, changes in renal function (e.g., serum creatinine, urinary output) were documented. Illness severity within 24 h of entering the ICU was evaluated retrospectively by another investigator [H.F.] using the Acute Physiology and Chronic Evaluation II (APACHE II) scoring system 18 and the Sequential Organ Failure Assessment (SOFA) score. 19 The study was approved by the ethics committee of Ningbo First Hospital and, because it was retrospective in design, a signed waiver of informed consent was obtained.
Statistical analyses
The collected information was analysed by two investigators [H.F. and Y.Z.] using the Statistical Package for Social Sciences (SPSS) for Windows release 16.0 (SPSS Inc., Chicago, IL, USA). Normally distributed continuous variables were reported as means with standard deviation (SD) and Student t-test was used to compare data. Non-normally distributed continuous variables were reported as medians with interquartile range (IQR) and Friedman’s test or Mann-Whitney U test were used to compare data where appropriate. Categorical values such as proportions were compared using Fisher’s exact test or χ2 test. A multivariate logistic regression analysis was used to examine the impact of various factors on the ICU mortality. A P-value <0.05 was considered to indicate statistical significance.
Results
During the five-year study period (April 2013 to March 2018), 3654 were admitted to the ICU centre, of whom 368 (10%) had sepsis. Of these patients, 167 (45%) developed septic AKI; 95 were insured and 72 were uninsured. Uninsured patients were younger, had statistically significantly higher APACHE II and SOFA scores on admission, had shorter ICU-LOS and higher ICU mortality rates than insured patients (Table 1). However, there were no differences between uninsured and insured patients in terms of medical histories and source of sepsis (Table 2). The most common source of infection in both groups was pulmonary infection (61%) followed by abdominal infection (27%).
Characteristics and outcomes of insured and uninsured patients with septic acute kidney injury (AKI).

Data are presented as mean ±SD, n (%) or median (interquartile range).
Medical history and sources of sepsis for the insured and uninsured patients with septic acute kidney injury (AKI).
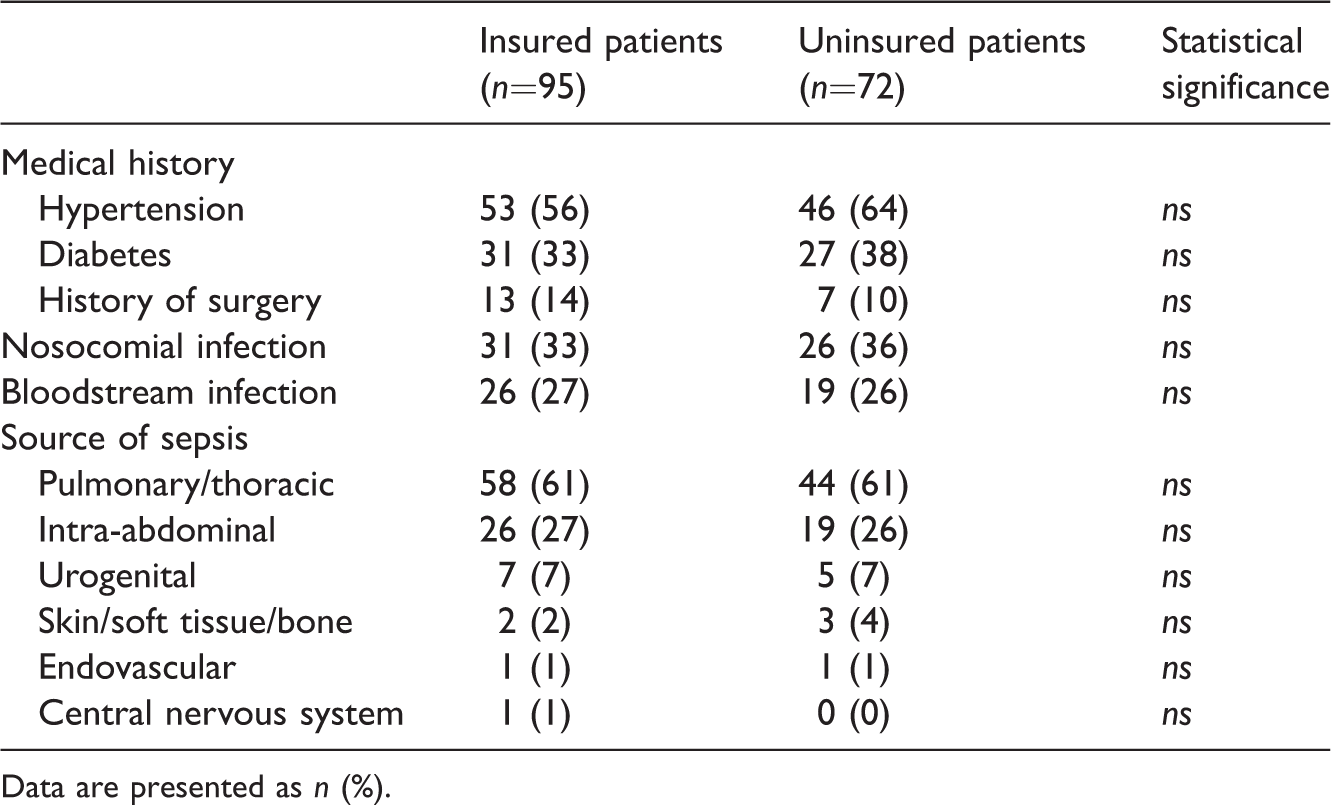
Data are presented as n (%).
On admission, there were no significant differences between uninsured and insured patients in urine output, RIFLE category, serum urea, and creatinine (Table 3). The numbers of patients who used diuretics and nephrotoxins were also similar between the two groups. While, uninsured patients had significantly less interventions in terms of central venous catheters, pulmonary arterial catheters and RRT compared with insured patients, they had significantly more occurrences of septic shock and MODS.
Details of kidney function and interventions in patients with septic acute kidney injury (AKI).

Data are presented as mean ±SD, n (%) or median (interquartile range).
aNephrotoxin exposure included: radiocontrast media; aminoglycosides; cardiopulmonary bypass; rhabdomyolysis (i.e., serum creatinine kinase >1500 U/L); amphotericin.
RIFLE, Risk, Injury, Failure, Loss, End stage kidney disease criteria; 13 RRT, renal replacement therapy; MODS, multiple organ dysfunction syndrome.
The uninsured patients with septic AKI had a higher ICU mortality than insured patients (60% vs. 37%, P=0.004). Multivariate analysis showed that low age, lack of insurance, presence of septic shock, high APACHE II score, high SOFA score, MODS and underuse of RRT were statistically significant risk factors for ICU mortality (Tables 1,3 and 4).
Multivariate analysis of variables associated with ICU mortality among patients with septic acute kidney injury (AKI).
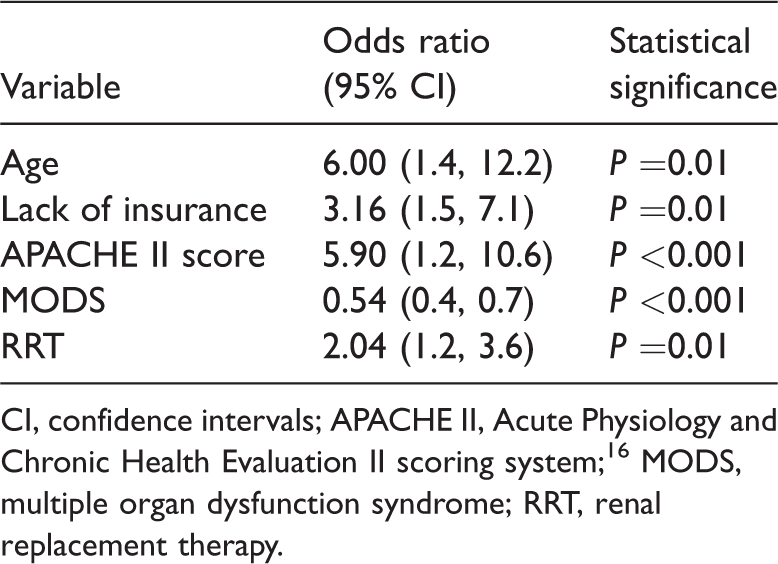
CI, confidence intervals; APACHE II, Acute Physiology and Chronic Health Evaluation II scoring system; 16 MODS, multiple organ dysfunction syndrome; RRT, renal replacement therapy.
Discussion
Although Chinese public medical insurance coverage has increased in recent years, there are still large disparities in availability and affordability between urban and rural communities. 20 For example, the insurance coverage of urban migrants is low and is thought to be affected by their gender, age, education, income level and settlement. 21 In addition, compared with settled groups, migrants are at increased risk of chronic conditions, such as hypertension, diabetes and cancer. 12 However, their migration status prevents them from enjoying the same social benefits as urban residents. 11 Without medical insurance from a locality, Chinese migrants' access to health services in that area, particularly costly medical procedures, is limited. 22
Data from this retrospective study showed that uninsured patients with septic AKI were younger and had higher APACHE II and SOFA scores at admission compared with insured patients. Following admission to ICU, uninsured patients with septic AKI had a higher incidence of septic shock and MODS compared with insured patients, but had used less interventions. Not surprisingly, risk factors associated with ICU mortality in this group of patients included age, APACHE II score, MODS and use of RRT. Whether lack of health insurance had affected the overall health status of the patients or their medical treatment is unknown, but this study showed that health insurance was an independent risk factor for ICU mortality in patients with septic AKI. To our knowledge, this is the first study to report this finding.
Limited social benefits render migrants dependent on personal or family resources to provide medical services. 23 However, families often refuse the option of costly treatments such as RRT or catheter interventions because of the lack of funds. A study conducted among migrants in Gansu, China, showed that economic difficulties were one of the major obstacles in preventing migrants from obtaining health services. 24 Another study showed that uninsured migrant workers tended to seek care less frequently when sick than insured migrant workers. 13 These factors may have contributed to the findings of this present study which showed that, compared with insured patients, uninsured patients were more seriously ill when they are admitted to hospital, had less interventions and a poorer prognosis. Therefore, increasing health insurance coverage for migrants and the proportion of medical reimbursements available may be effective measures in reducing high mortality rates in patients with septic AKI in China. 25
The study had several limitations. Firstly, this was a retrospective study and therefore liable to record bias. Secondly, some of the data were extracted from a database that used billing codes and lacked independent validation. For example, it was unclear from the billing database if sepsis was the main reason for hospital admission or an in-hospital complication. In addition, the timing of AKI could not be established from this database. Finally, several potentially important variables, such as patient's rural or urban status, household registration location, proportion of reimbursement from resident location were not assessed.
In summary, data from this retrospective study conducted in Ningbo, China found that uninsured patients with septic AKI were younger, stayed in the ICU less time, had less interventions, higher illness severity scores and higher ICU mortality than insured patients with septic AKI. Importantly a major risk factor for ICU mortality in this group was lack of insurance. A prospective population-based study is urgently needed to study the relationship between health insurance status and the outcomes of AKI in patients with sepsis.
Footnotes
Author contributions
H.F., Y. Z. and G. C. contributed equally to this work and are considered as co-first authors.
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This study was supported by Ningbo Natural Science Fund (2017A610188), Zhejiang Natural Science Fund (LQ18H150001), Zhejiang Provincial Medical and Health Science Fund (2017KY134, 2018KY667, 2018KY669, 2018KY685).
