Abstract
Objectives
The goal of this study was to analyze skeletal, dental, and soft tissue changes of patients treated with customized lingual systems and to evaluate the clinical effectiveness of miniscrew anchorage.
Methods
Nine upper first premolar extraction patients who were treated with customized lingual appliances were included in this study. Miniscrews were used for reinforcement of molar anchorage. Cephalometric films and study models were obtained before treatment (T1), after alignment (T2), and after treatment (T3). Treatment effects were analyzed by cephalometric radiographs and study models.
Results
The upper anterior teeth were retracted significantly at T2 and T3 (4.41 ± 4.14 mm and 5.51 ± 2.48 mm, respectively). During space closure, the upper first molars showed slight mesial movement (1.50 ± 1.97 mm). The intercanine width of the upper arch increased at T2 (1.59 ± 1.81 mm), but decreased at T3 (0.11 ± 1.00 mm). The sella-nasion-A, A-nasion-B, and mandibular plane angles were not significantly changed at T3. The upper lip showed continuous retraction at both T2 and T3 (1.40 ± 1.46 mm and 2.32 ± 2.48 mm, respectively).
Conclusions
By using miniscrew anchorage for lingual orthodontics, patients’ dental and soft tissue changes considerably improved and molar anchorage was reinforced.
Keywords
Introduction
To resolve tooth crowding and protrusion or other aesthetic difficulties, patients choose orthodontic treatment. However, in some cases, buccal orthodontics are not aesthetically acceptable for reasons related to social interactions, workplace expectations, or simple personal preferences. For these reasons, patients seek aesthetic orthodontic treatment. Lingual orthodontics and Invisalign are currently the main invisible and aesthetic orthodontic appliances. Because it provides good control of the teeth, lingual orthodontics has an advantage over Invisalign treatment, especially for patients seeking to relieve severe dental malocclusion.1,2 Customized lingual appliances, which were introduced by Wiechmann in 2001, are much more convenient for orthodontists; therefore, customized lingual appliances are widely used in the clinic.3,4 Previous studies have confirmed that a convex profile is more common among Asian people than in those in Western countries. With the increasing migration to Western countries from Asian countries (e.g., China, Indonesia, Vietnam, and Korea), there has been a corresponding increase in the need for orthodontic treatment, especially for improving patients’ convex profiles.5–8 Miniscrew anchorage is a type of “absolute anchorage,” which plays an important role in space and anchorage control. With the application of miniscrew anchorage, the range of orthodontics has been greatly expanded. 9 Because the brackets are placed closer to the center of resistance within the teeth, the biomechanical mechanism of lingual orthodontics differs from that of buccal orthodontics, especially at the stage of space closure. During the space closure stage in lingual orthodontics, combined buccal and lingual forces can be applied to prevent the “bowing effect.” Palatal miniscrew anchorage in lingual orthodontics has shown a dramatic treatment effect in some orthodontic case reports.10,11
In this study, we describe the use of miniscrews in customized lingual orthodontics and the associated dentoskeletal and soft tissue changes in patients, as determined by linear and angular measurements of cephalometric radiographs; in addition, we study models to evaluate the clinical effectiveness of miniscrew anchorage in lingual orthodontics.
Methods
This study was approved by the Institutional Review Board of Peking University, Hospital of Stomatology (IRB #2011019). Patients who were seeking aesthetic orthodontic treatment and had accepted lingual orthodontic treatment were recruited at the Department of Orthodontics, Peking University School and Hospital of Stomatology, from February 2011 to February 2012. All included patients provided informed consent before this study.
Inclusion criteria
Permanent and complete dentition with fully erupted secondary molars. Class I classification with bimaxillary protrusion or Class II classification. A convex profile and premolarextraction.
Exclusion criteria
Severe skeletal disharmony requiring surgical treatment. A history of orthodontic treatment, poor oral habits, or general diseases.
Treatment design
All patients were treated with a customized lingual appliance (slot size of the brackets, 0.018 × 0.025-inch; Incognito, Bad Essen, Germany) by using indirect bonding. At the initial alignment stage, 0.016-inch and 0.016
Before space closure, miniscrews (diameter, 1.5 mm; length, 9 mm; Zhongbang Medical Treatment Appliance, Xi’an, China) were placed palatally between the upper first molar and second premolar; an elastic power chain was loaded between the miniscrews and upper canines, 2 weeks after miniscrew placement.
Combined palatal-buccal forces and sliding mechanics were used in all cases at the space closure stage (Figure 1). A 0.016

Palatal miniscrew anchorage scheme.
Data collection
Cephalometric radiographs and study models were obtained before treatment (T1), after alignment (T2), and after treatment (T3). Linear and angular measurements of the cephalometric radiographs were performed by using CIS software (CIS was developed by the Craniofacial Growth and Development Center, School of Stomatology, Peking University and School of Computer Science, Peking University) (Figure 2). We used an electronic vernier caliper (accuracy of 0.01 mm) to perform model measurements. All 23 linear and angular measurements were performed twice and were analyzed by an examiner at an interval of 1 week (Figures 2 and 3); we used the average values of these measurements as the final results (Table 1). Differences between T2 and T1 and between T3 and T2 were then calculated (Tables 2 and 3).

Linear and angular measurements.

Model analysis.
Descriptive statistics of patients before treatment (T1), after alignment (T2), and after treatment (T3) † .
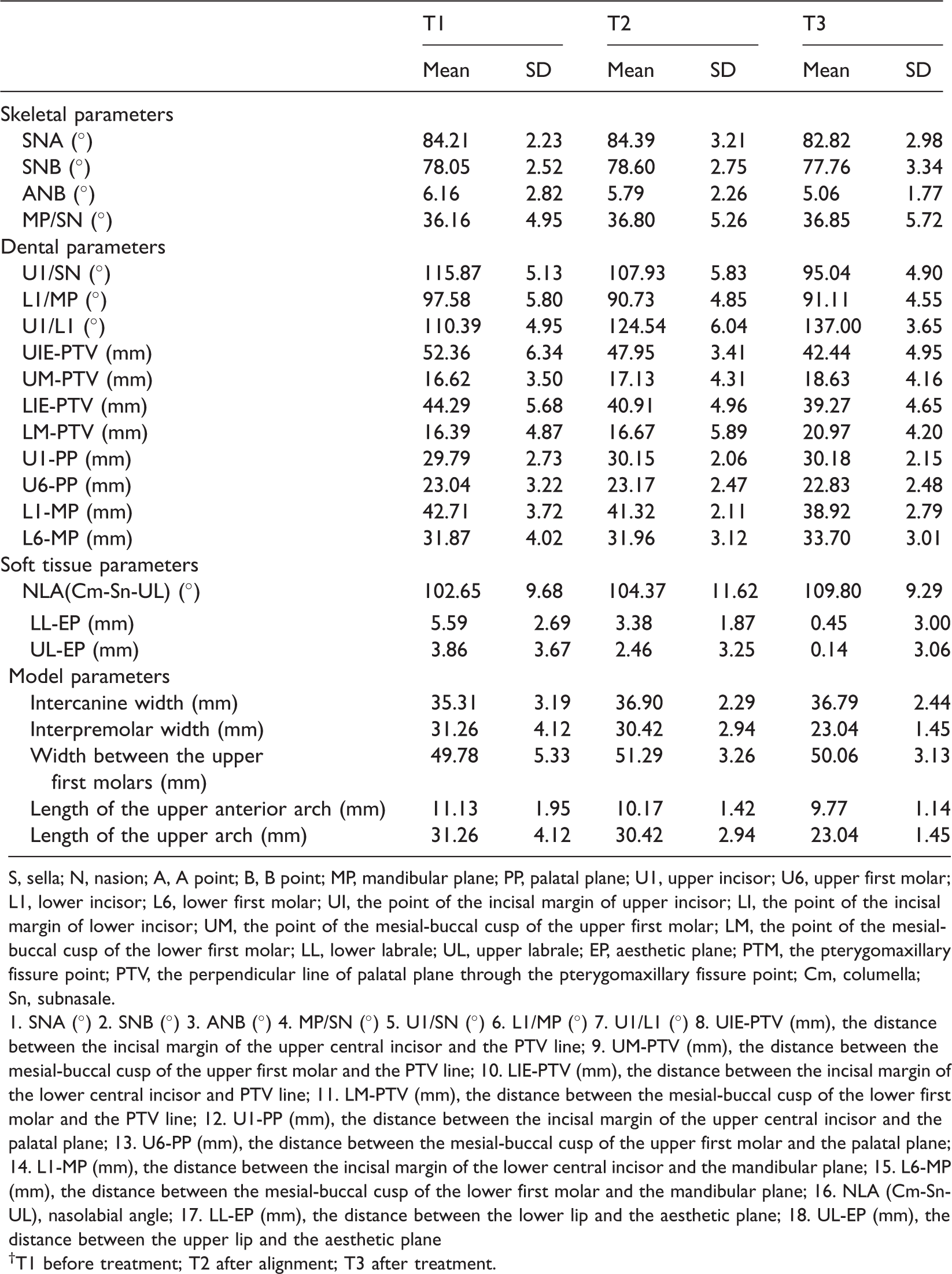
S, sella; N, nasion; A, A point; B, B point; MP, mandibular plane; PP, palatal plane; U1, upper incisor; U6, upper first molar; L1, lower incisor; L6, lower first molar; UI, the point of the incisal margin of upper incisor; LI, the point of the incisal margin of lower incisor; UM, the point of the mesial-buccal cusp of the upper first molar; LM, the point of the mesial-buccal cusp of the lower first molar; LL, lower labrale; UL, upper labrale; EP, aesthetic plane; PTM, the pterygomaxillary fissure point; PTV, the perpendicular line of palatal plane through the pterygomaxillary fissure point; Cm, columella; Sn, subnasale.
1. SNA (°) 2. SNB (°) 3. ANB (°) 4. MP/SN (°) 5. U1/SN (°) 6. L1/MP (°) 7. U1/L1 (°) 8. UIE-PTV (mm), the distance between the incisal margin of the upper central incisor and the PTV line; 9. UM-PTV (mm), the distance between the mesial-buccal cusp of the upper first molar and the PTV line; 10. LIE-PTV (mm), the distance between the incisal margin of the lower central incisor and PTV line; 11. LM-PTV (mm), the distance between the mesial-buccal cusp of the lower first molar and the PTV line; 12. U1-PP (mm), the distance between the incisal margin of the upper central incisor and the palatal plane; 13. U6-PP (mm), the distance between the mesial-buccal cusp of the upper first molar and the palatal plane; 14. L1-MP (mm), the distance between the incisal margin of the lower central incisor and the mandibular plane; 15. L6-MP (mm), the distance between the mesial-buccal cusp of the lower first molar and the mandibular plane; 16. NLA (Cm-Sn-UL), nasolabial angle; 17. LL-EP (mm), the distance between the lower lip and the aesthetic plane; 18. UL-EP (mm), the distance between the upper lip and the aesthetic plane
†T1 before treatment; T2 after alignment; T3 after treatment.
Descriptive statistics of changes in patients after alignment (T2–T1) † .

†T1 before treatment; T2 after alignment.
‡indicates significance. NS, not significant; *p<0.05; **p<0.01, ***p<0.001.
§Data that did not follow a normal distribution are described by Z values from the Wilcoxon rank-sum test.
S, sella; N, nasion; A, A point; B, B point; MP, mandibular plane; PP, palatal plane; U1, upper incisor; U6, upper first molar; L1, lower incisor; L6, lower first molar; UI, the point of the incisal margin of upper incisor; LI, the point of the incisal margin of lower incisor; UM, the point of the mesial-buccal cusp of the upper first molar; LM, the point of the mesial-buccal cusp of the lower first molar; LL, lower labrale; UL, upper labrale; EP, aesthetic plane; PTM, the pterygomaxillary fissure point; PTV, the perpendicular line of palatal plane through the pterygomaxillary fissure point; Cm, columella; Sn, subnasale.
1. SNA (°) 2. SNB (°) 3. ANB (°) 4. MP/SN (°) 5. U1/SN (°) 6. L1/MP (°) 7. U1/L1 (°) 8. UIE-PTV (mm), the distance between the incisal margin of the upper central incisor and the PTV line; 9. UM-PTV (mm), the distance between the mesial-buccal cusp of the upper first molar and the PTV line; 10. LIE-PTV (mm), the distance between the incisal margin of the lower central incisor and PTV line; 11. LM-PTV (mm), the distance between the mesial-buccal cusp of the lower first molar and the PTV line; 12. U1-PP (mm), the distance between the incisal margin of the upper central incisor and the palatal plane; 13. U6-PP (mm), the distance between the mesial-buccal cusp of the upper first molar and the palatal plane; 14. L1-MP (mm), the distance between the incisal margin of the lower central incisor and the mandibular plane; 15. L6-MP (mm), the distance between the mesial-buccal cusp of the lower first molar and the mandibular plane; 16. NLA (Cm-Sn-UL), nasolabial angle; 17. LL-EP (mm), the distance between the lower lip and the aesthetic plane; 18. UL-EP (mm), the distance between the upper lip and the aesthetic plane.
Descriptive statistics of changes in patients after treatment (T3–T2) † .

†T1 before treatment; T2 after alignment; T3 after treatment.
‡indicates significance. NS, not significant; *p<0.05; **p<0.01, ***p<0.001.
§Data that did not follow a normal distribution are described by Z values from the Wilcoxon rank-sum test.
S, sella; N, nasion; A, A point; B, B point; MP, mandibular plane; PP, palatal plane; U1, upper incisor; U6, upper first molar; L1, lower incisor; L6, lower first molar; UI, the point of the incisal margin of upper incisor; LI, the point of the incisal margin of lower incisor; UM, the point of the mesial-buccal cusp of the upper first molar; LM, the point of the mesial-buccal cusp of the lower first molar; LL, lower labrale; UL, upper labrale; EP, aesthetic plane; PTM, the pterygomaxillary fissure point; PTV, the perpendicular line of palatal plane through the pterygomaxillary fissure point; Cm, columella; Sn, subnasale.
1. SNA (°) 2. SNB (°) 3. ANB (°) 4. MP/SN (°) 5. U1/SN (°) 6. L1/MP (°) 7. U1/L1 (°) 8. UIE-PTV (mm), the distance between the incisal margin of the upper central incisor and the PTV line; 9. UM-PTV (mm), the distance between the mesial-buccal cusp of the upper first molar and the PTV line; 10. LIE-PTV (mm), the distance between the incisal margin of the lower central incisor and PTV line; 11. LM-PTV (mm), the distance between the mesial-buccal cusp of the lower first molar and the PTV line; 12. U1-PP (mm), the distance between the incisal margin of the upper central incisor and the palatal plane; 13. U6-PP (mm), the distance between the mesial-buccal cusp of the upper first molar and the palatal plane; 14. L1-MP (mm), the distance between the incisal margin of the lower central incisor and the mandibular plane; 15. L6-MP (mm), the distance between the mesial-buccal cusp of the lower first molar and the mandibular plane; 16. NLA (Cm-Sn-UL), nasolabial angle; 17. LL-EP (mm), the distance between the lower lip and the aesthetic plane; 18. UL-EP (mm), the distance between the upper lip and the aesthetic plane.
Data interpretation
Landmarks and cephalometric planes are described in Figure 2. Sagittal changes in landmarks were analyzed by measuring the distances between the landmarks and the PTV line (the perpendicular line of palatal plane through the pterygomaxillary fissure point); vertical changes in landmarks were analyzed by measuring the distances between the landmarks and the palatal or mandibular planes. The accuracies of linear and angular measurements were 0.05 mm and 0.05°, respectively.
Study models were analyzed to determine changes in the upper dental arch. Intercanine width represented anterior arch width; the width between the upper first molars represented posterior arch width. The vertical distance between the mesial contact point of the incisors and the line of the cusps of the canines represented the length of the upper anterior arch. The vertical distance between the mesial contact point of the incisors and the line of the mesial-buccal cusps of the first molars represented the full length of the upper arch.
Statistical analysis
Statistical analysis was performed by using IBM SPSS Statistics for Windows, version 19.0 (IBM Corp., Armonk, NY, USA). Student’s t-test was used to analyze dentoskeletal and soft tissue changes in patients between T2 and T1 and between T3 and T2, when the parameters followed a normal distribution. When the parameters did not follow a normal distribution, we applied the Wilcoxon rank-sum test. Statistical significance was set at 0.05.
Results
Nine patients (age range: 11 to 26 years) with Class I malocclusion (two subjects) or Class II division 1 malocclusion (seven subjects), who needed upper first premolar extraction along with lower first or second premolar extraction, and who required maximum anchorage were included in this study. The duration of treatment was 24 ± 6 months. All miniscrews were stable during treatment. The descriptive parameters of the patients at T1, T2, and T3 were recorded (Table 1). These statistics were the means and standard deviations of skeletal, dental, soft tissue, and model parameters.
During alignment, the upper and lower anterior teeth showed some retraction. The upper incisor showed 7.95° lingual tipping and 4.41 mm of distalization (p < 0.05), but the extrusion of the incisors was not significant. Significant anchorage loss was not observed in the upper arch, and the upper molars did not significantly shift mesially. Intercanine width increased (p < 0.05), but interpremolar width decreased (p < 0.05). The length of the upper anterior arch decreased (p < 0.05). For soft tissue changes, upper and lower lip protrusion decreased significantly (p < 0.05 for both, Table 2). No significant changes in the skeletal A point or mandibular plane angle were observed at T2. Regarding the changes between T3 and T2 (Table 3), the upper molars showed some mesial movement and intrusion, but this change was not significant. Thus, miniscrews prevented the loss of upper anchorage and achieved significant retraction of the upper incisors, which showed 12.89° lingual tipping and 5.51 mm of distalization.
During space closure, the interpremolar width and the length of the upper arch decreased significantly (p < 0.001 for both). However, the intercanine width and intermolar width did not change significantly (Table 3). Soft tissue changed substantially after space closure; upper and lower lip protrusion decreased, while the facial profile was improved. The NLA became more obtuse (p < 0.05). After space closure, the SNA decreased 1.57°. Some retraction of the A point was observed, although the change was not significant.
Discussion
Dentoskeletal effects
Adult patients choose lingual orthodontics for aesthetic reasons; however, many of them have severe dentoskeletal problems, such that a good orthodontic treatment result is therefore difficult to achieve. Because many people may reject surgery, the use of an appliance combined with miniscrew anchorage can be an effective means of treatment. Miniscrew anchorage is effective for reinforcement of anchorage and can also control sagittal and vertical tooth movement; Ruan 12 found that miniscrews could provide maximum anchorage for both adolescents and adults. Several reports10,11 on the use of miniscrew anchorage in lingual orthodontics have shown that this technique achieves effective tooth retraction and anchorage control.
In our study, the upper molar shifted 0.51 mm mesially at T2, although this was not significant. No obvious anchorage loss in the upper arch was observed at the alignment stage, suggesting that additional anchorage control devices may not be necessary during alignment in lingual orthodontics. After space closure, the upper first molar shifted 1.50 mm mesially, which was not significant; this change demonstrated that miniscrew anchorage provided effective anchorage control. In addition, the upper first molar intruded by 0.34 mm due to the vertical component of the retraction force.
Kelley 13 speculated that a lingual bite splint could cause an intrusion of the upper incisors; however, Fulmer and Kuftinec 14 did not report similar findings. Gorman 15 found that, although 0.5 mm intrusion of the upper incisors occurred, no significant difference was observed, compared with buccal orthodontics; extra force was suspected for the intrusion of upper incisors in some cases. With labial appliances, the upper incisors can be intruded and retracted significantly by miniscrews; 12 however, with lingual orthodontics, the effects may differ. In our study, the upper incisors of the patients were extruded by 0.35 mm at T2, which was not significant. During space closure, the U1/SN angle decreased by 12.89° and the UIE-PTV decreased by 5.51 mm; in this case, the upper incisors showed significant retraction. The upper incisors were extruded by 0.03 mm, which was not significant. If significant intrusion of the upper incisors is required, additional methods may be necessary, with lingual orthodontics (e.g., upper anterior miniscrews) for intrusion. After treatment, lower incisors showed significant retraction. Because of the unique mechanism of lingual orthodontics, lower incisor retraction is much more easily achieved than in labial orthodontics, especially in cases that require lower extraction.
Recently, some researchers16–19 have revealed that, regardless of tooth extraction, intercanine width would increase significantly with buccal orthodontics. Most studies have reported16–18 that the interpremolar and intermolar width decreased significantly in the extraction group and increased in the non-extraction group.
We found that, at T2, upper intercanine width increased significantly, whereas upper interpremolar width decreased significantly. The upper intermolar width increased, but this change was not significant. After space closure, the widths between the upper canines, premolars, and first molars decreased, similar to the results of the study by Upadhyay. 9
Sharma 20 reported that, in bimaxillary protrusion cases in which anterior teeth were retracted, reductions occurred in skeletal SNA and SNB, as well as in soft tissue. In our study, the SNA angle decreased slightly, but this change was not significant.
With lingual orthodontics, many scholars have speculated that mandibular clockwise rotation and an increase in lower facial height may occur after treatment, possibly due to molar extrusion. Fulmer and Kuftinec 14 found that the mandibular plane angle increased by 0.6° after lingual orthodontic treatment. In our study, the mandibular plane angle did not change significantly during the treatment period, demonstrating that a lingual appliance supported by miniscrews can be used to achieve better vertical control.
Soft tissue effects
After space closure, the upper and lower incisors, as well as the upper and lower lips, were retracted; the NLA became more obtuse; and the profile of the patients improved significantly. At T2, the UIE-PTV decreased by 4.41 mm and the UL-EP decreased by 1.40 mm. After space closure, the UIE-PTV decreased by 5.51 mm and the UL-EP decreased by 2.32 mm. Retraction of the upper anterior teeth was proportional to that of the upper lip.
There is an obvious relationship between retraction of the upper incisors and lip position, although it is not linear. 21 Scott and Jernigan 22 reported that, in upper first premolar extraction cases, the retraction ratio of the upper incisors and upper lip was 2.68:1. Ramos 23 reported that the ratio of retraction of the upper incisors and upper lip was 1:0.75 to 1:0.70. These studies confirmed that retraction of upper anterior teeth was proportional to that of the upper lip, although the ratios of change differed. Brock 24 confirmed that the ratio of retraction of the upper incisors and upper lip differed significantly between white and black subjects, with greater retraction of the upper lip observed in white subjects.
Clinically, there is not a large proportion of patients with severe dentoskeletal malocclusion requiring maximum anchorage, especially for lingual orthodontic treatment. A large sample size study would provide additional information regarding miniscrew anchorage control. However, with this limited sample, we revealed that the tendencies of the dentoskeletal and soft tissue changes were quite similar; maximum anchorage was achieved by miniscrews in our study. These results can provide a preliminary reference for the clinicians. It will be instructive to increase the sample size in future studies, in order to more thoroughly explore the efficiency of miniscrews in lingual orthodontics and reduce individual variations.
Conclusion
Customized lingual appliances supported by miniscrew anchorage can achieve a beneficial treatment effect. Miniscrews provided maximum anchorage control and maximum retraction of the upper incisors; moreover, they effectively maintained the mandibular plane angle during lingual orthodontic treatment.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This work was supported by International Science & Technology Cooperation Program of China [Grant No. 2015DFB30040]; the National Science Foundation of China [81300897, 81571815, 81300850, and 81470717]; the Beijing Municipal Natural Science Foundation [7152156]; the Young Scientists Fund of PKUSS [20110203 and 20170109]; and the New Clinical Technology Fund of PKUSS [PKUSSNCT-11A07].
