Abstract
Objective
To compare surgical complications and functional outcomes of the ring plate versus the non-ring plate approach to the surgical repair of scapular body fractures (SBFs; AO/OTA classification: 14-A2.2).
Methods
This retrospective study reviewed data from adults with SBFs who underwent a modified Judet approach combined with non-ring or ring plates between November 2006 and June 2013. The primary outcomes were the Constant and Murley score and the Disabilities of the Arm, Shoulder and Hand (DASH) score. The secondary outcomes were radiographic findings.
Results
A total of 318 patients had a non-ring or ring plate internal fixation, of which 147 patients (ring-treated, n = 72; non-ring-treated, n = 75) were evaluated with a mean follow-up period of 60 months. At the 3-month follow-up, the complication rate was 2.8% and 13.3% for the ring-treated and non-ring-treated groups, respectively. The difference persisted over time, with significantly different rates of 8.3% and 20.0% at the final follow-up for the ring and non-ring groups, respectively. The ring-treated group had significantly higher postoperative Constant and Murley scores and lower DASH scores compared with the non-ring-treated group.
Conclusion
Application of a modified Judet approach combined with ring plate internal fixation for the treatment of SBFs may be the preferred treatment option.
Introduction
Management of scapular body fractures (SBFs; AO/OTA classification: 14-A2.2) has most often been defined as ‘benign neglect’.1–4 Despite the assessment of the impact of ‘benign neglect’ by multiple studies,1,3,5–7 there is a lack of consistency regarding its effectiveness in preventing or avoiding complications, or its impact on longer-term outcomes. This controversy remains due to small sample sizes and low rates of complications induced by SBFs, which limits the power of these studies.2,3,8 Despite generally good results, not all SBFs heal uneventfully, and there has been a resurgence of interest in determining which patients would benefit from surgical management because SBFs are inclined to occur as a consequence of high-energy injuries that cause various complications, including poor tissue healing, trauma-induced chronic pain, vascular nerve injury or entrapment, increased risk of infection, heterotopic ossification, and diminished range-of-motion.4,9–11
A systematic review of the surgical management of SBFs (AO/OTA classification: 14-A2.2) found that good to excellent functional outcomes were detected in almost 85% of patients. 12 Despite the lack of sufficient evidence to formulate definite criteria for the surgical management of SBFs (AO/OTA classification: 14-A2.2), the review highlighted that most SBFs can be treated effectively, but the criteria for deciding which fractures have a tendency to result in poor outcomes are still evolving. 12 Additionally, despite being rarely treated surgically, some SBFs benefit from surgical stabilization to rebuild the function of the shoulder joint, which is an active treatment decision and not ‘benign neglect’. The ultimate goal of treatment is to maintain the function of the shoulder joint to avoid related complications. Furthermore, the decision to use surgical management must consider the surgeon’s skill level and whether the SBF is highly displaced. Regrettably, surgical management, while beneficial, is limited by the concept of conservative treatment. The decision of whether to perform surgical treatment in SBFs (AO/OTA classification: 14-A2.2) remains controversial,2,6 and there are limited data in the literature for guiding orthopaedic surgeons on deciding on the most appropriate treatment to achieve the best possible clinical outcome for the patient. Current knowledge on the outcomes of surgically treated SBFs has been derived from small and indirect comparisons.
The purpose of this retrospective study was to compare the long-term functional outcomes and complications of non-ring or ring plate internal fixation for the treatment of SBFs (AO/OTA classification: 14-A2.2) using the Constant and Murley scores and Disabilities of the Arm, Shoulder and Hand (DASH) scores as the primary endpoints. The secondary outcomes were radiographic findings.
Patients and methods
Study population
This retrospective study enrolled consecutive patients with SBFs (AO/OTA classification: 14-A2.2) who were initially treated using non-ring or ring plate internal fixation between November 2006 and June 2013 that were identified in the databases of two centres: The Jinshan Hospital, Fudan University, Shanghai, China and The First Affiliated Hospital of Sun Yat-sen University, Guangzhou, China. The inclusion criteria were as follows: (i) age ranging from 20 to 70 years; (ii) confirmed closed SBFs (AO/OTA classification: 14-A2.2); (iii) X-rays taken directly after the accident; (iv) no sign of shoulder osteoarthritis; (v) all patients undergoing treatment with a reconstruction locking plate composed of J-type pure titanium and screws (2.0 and/or 2.7 mm; Smith & Nephew, Memphis, TN, USA). The main exclusion criteria included poly-trauma, multiple fractures, pathological fractures, planned surgery, dyspraxia, chemotherapy or endocrine therapy for other diseases, active metabolic bone diseases, primary tumours or advanced malignancy, life expectancy < 2 years, a bone mineral density T score ≤–2.5 SD at the femoral neck or lumbar spine, mental illness, severe infectious diseases, and an American Society of Anesthesiologists score of IV or V.
The Institutional Review Boards of The First Affiliated Hospital of Sun Yat-sen University and Jinshan Hospital of Fudan University provided approval for the study, which included an exemption from informed consent because of the retrospective design of the study. All clinical investigations were conducted according to the principles expressed in the Declaration of Helsinki.
Definitions of the descriptive variables
If the fracture fragments failed to be clearly defined on plain films, a computed tomography (CT) scan was performed. Radiological union was assessed using standard views, including an antero-posterior view, angled view, and trans-scapular view. The trans-scapular view was defined by the following radiographic parameters: restoration of cortical continuity, loss of a clear fracture line, presence of callus. Nonunion was defined as the state in which disturbed consolidation of a fracture that needs further surgical intervention or a prolonged healing time of more than 12 months or more. Malunion was defined as any nonanatomic fracture alignment or angulation measured intraoperatively or postoperatively with radiographs. Heterotopic ossification was graded according to the Brooker classification. 13 The Constant and Murley scores and DASH scores were graded by an experienced orthopaedic surgeon during the postoperative visits and were documented in this study as the constant score outcome at each follow-up.
Study design
The study cohort involved a consecutive series of patients with SBFs (AO/OTA classification: 14 14-A2.2) who were retrospectively reviewed between November 2006 and June 2013. Eligible patients were divided into two groups. All SBFs were treated in a lateral position on a radiolucent table. The ring-treated group included patients who sustained SBFs and underwent a modified Judet approach combined with ring plate internal fixation; and the non-ring-treated group included patients with SBFs who were treated using a modified Judet approach combined with non-ring plate internal fixation. Examples of the two surgical approaches are shown in Figures 1 and 2. Follow-up was at 1, 3, 6, and 12 months postoperatively and yearly thereafter. The Constant and Murley and DASH scores were used for functional evaluation during examination.

A representative example of a left scapular body fracture undergoing a modified Judet approach combined with non-ring plates (reconstruction locking plate of J-type pure titanium) in a 43-year-old male patient. (A) Preoperative anteroposterior (AP) X-ray. (B) Horizontal spiral computed tomography (CT) scan of the scapula. (C) Three-dimensional reconstruction of the CT of the scapula. (D) Immediate postoperative AP X-ray.
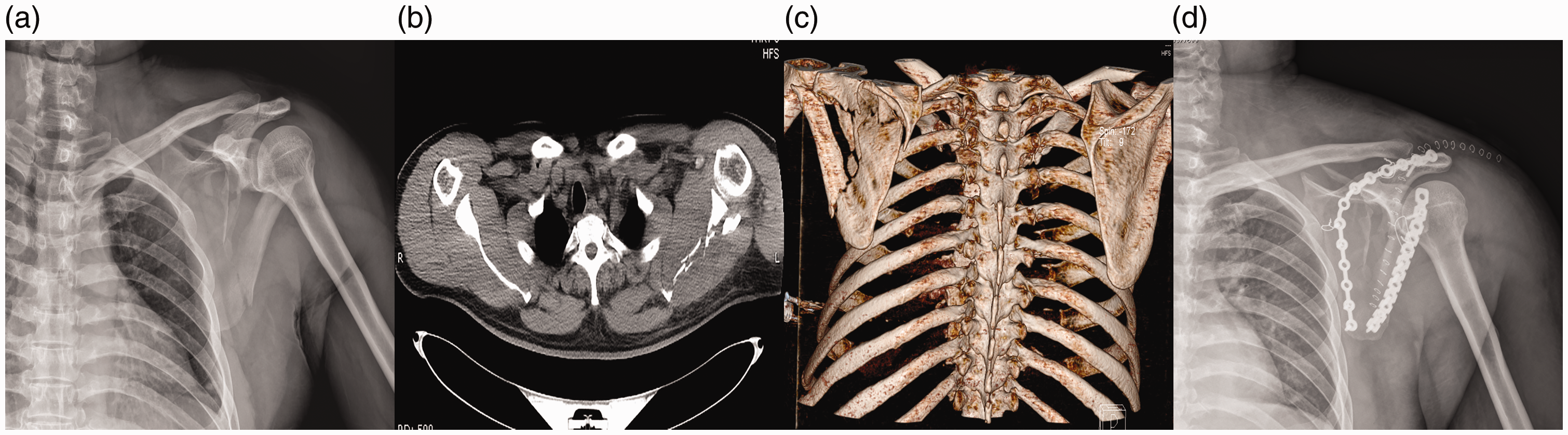
A representative example of a left scapular body fracture undergoing a modified Judet approach combined with ring plates (reconstruction locking plate of J-type pure titanium) in a 41-year-old male patient. (A) Preoperative anteroposterior (AP) X-ray. (B) Horizontal spiral computed tomography (CT) scan of the scapula. (C) Three-dimensional reconstruction of the CT of the scapula. (D) Immediate postoperative AP X-ray.
Surgical techniques
The modified Judet approach described previously was applied in all patients. 15 In addition, based on the modified Judet approach, the ring fixation technique was merged, as shown in Figure 3. The main variation in the surgical technique for patients with SBFs who received the modified Judet approach combined with non-ring or ring plate internal fixation was minimization of tissue damage until the operative procedure was completed, thus maximizing functional recovery after surgery. For the procedure, a three-point and two-line principle was applied. Reduction was achieved by vertical or horizontal compression of the three points. If this was not sufficient or there was a noticeable vertical or horizontal displacement, a distal fragment traction or poking reduction technique was utilized by a pin or Kirschner wire. Then, plates and screws (2.0 and/or 2.7 mm; Smith & Nephew) were inserted along the predetermined locations under the guidance of a mobile C-arm (Cios Spin; Siemens Healthcare GmbH, Erlangen, Germany) (Figures 1D and 2D).

The ‘three-point and two-line’ principle of internal fixation. The ring-treated approach with identified bony columns (two dotted lines) and three anatomical landmarks (three black points). A reconstruction locking plate of J-type pure titanium was placed along the dotted lines. Three points: scapular neck, intersection of the scapular spine and medial border, and subscapular angle. Two lines: acromion-scapular spine-subscapular angle line and the scapular neck-subscapular angle line.
Postoperative management
Pain management was achieved with an intravenous drip of 40 mg parecoxib sodium (Dynastat™; Pfizer, Walton Oaks, UK) combined with a 0.9% sodium chloride solution every 24 h for 3 days. A single dose of 6–7 mg/kg teicoplanin (Aventis Pharma, West Malling, UK) was administered to all patients twice a day for 3 subsequent days. The quality of surgery was evaluated by immediate postoperative radiographs to check for fracture reductions and implant positions. A postoperative rehabilitation protocol performed on the first postoperative day was essentially equivalent in both groups. Standard rehabilitation instructions were given by a physiotherapist. Sling or shoulder immobilization was applied for support initially and weaned off as tolerated. Pendulum exercises as well as active assisted flexion and abduction exercises below the horizon were started 1 day postoperatively. Isometric muscle strength training was performed only within 1 week postoperatively. Shrug training began on the second postoperative week. Shoulder passive motion was performed for the initial 3–4 weeks postoperatively, and shoulder active motion began at 5–6 weeks. After 6 weeks, patients were able to use their shoulders without pain. Patients were not allowed to engage in active shoulder external rotation for the first 7–8 weeks. Strengthening exercises were only allowed once radiological fracture union was confirmed.
Postoperative evaluation
Follow-up occurred 1, 3, 6, and 12 months postoperatively and every year thereafter. The primary endpoint measured was the Constant and Murley and DASH scores. The secondary endpoint was patient-related radiographic outcomes that were reviewed by two physicians (G.Z.L. and W.G.Y.). Major changes of the implant were noted. A literature review was then conducted to identify similar studies and to compare the functional and radiographic outcomes of surgical programmes.
Statistical analyses
All statistical analyses were performed using the SPSS® statistical package, version 23.0 (IBM Corp, Armonk, NY, USA) for Windows®. The descriptive and outcome variables were assessed by calculating the frequencies and means. The continuous variables were compared between groups using Pearson’s χ2-test, Fisher's exact test, independent samples t-test or the Mann–Whitney U-test. Comparisons between groups were performed for binary variables. Analyses were performed based on the data up to the primary analysis cut-off. All reported tests were two-tailed. A P-value < 0.05 was considered statistically significant.
Results
Of the 318 patients with SBFs (AO/OTA classification: 14-A2.2) who underwent the modified Judet approach combined with non-ring or ring plate internal fixation, 115 patients (36.2%) were excluded based on the inclusion and exclusion criteria, leaving 203 patients available for analysis (Figure 4). During follow-up, 56 patients were not able to continue participating in the study: three patients died of car accidents; eight patients sustained cerebrovascular accidents; six patients developed cardiovascular diseases; nine patients developed diabetic complications; and 30 patients died of uraemia, malignant tumours or severe infections. Consequently, 147 patients (86 male and 61 female) with a mean age of 37.5 years (range, 20–70 years) were available for final analysis (two groups: ring-treated group [n = 72] and non-ring-treated group [n = 75]). Eighty-seven patients (59.2%) had injuries on the dominant side. The mechanism of injury was thought to be a high-energy injury in all but seven patients (4.8%), who sustained a SBF caused by a low-energy injury. The mean surgical injury interval was 2 days (range, 6 h–7 days). Of the 147 patients included in the final analysis, 106 (72.1%) were followed for a mean of 60 months (range, 24–90 months) after surgery (Table 1).
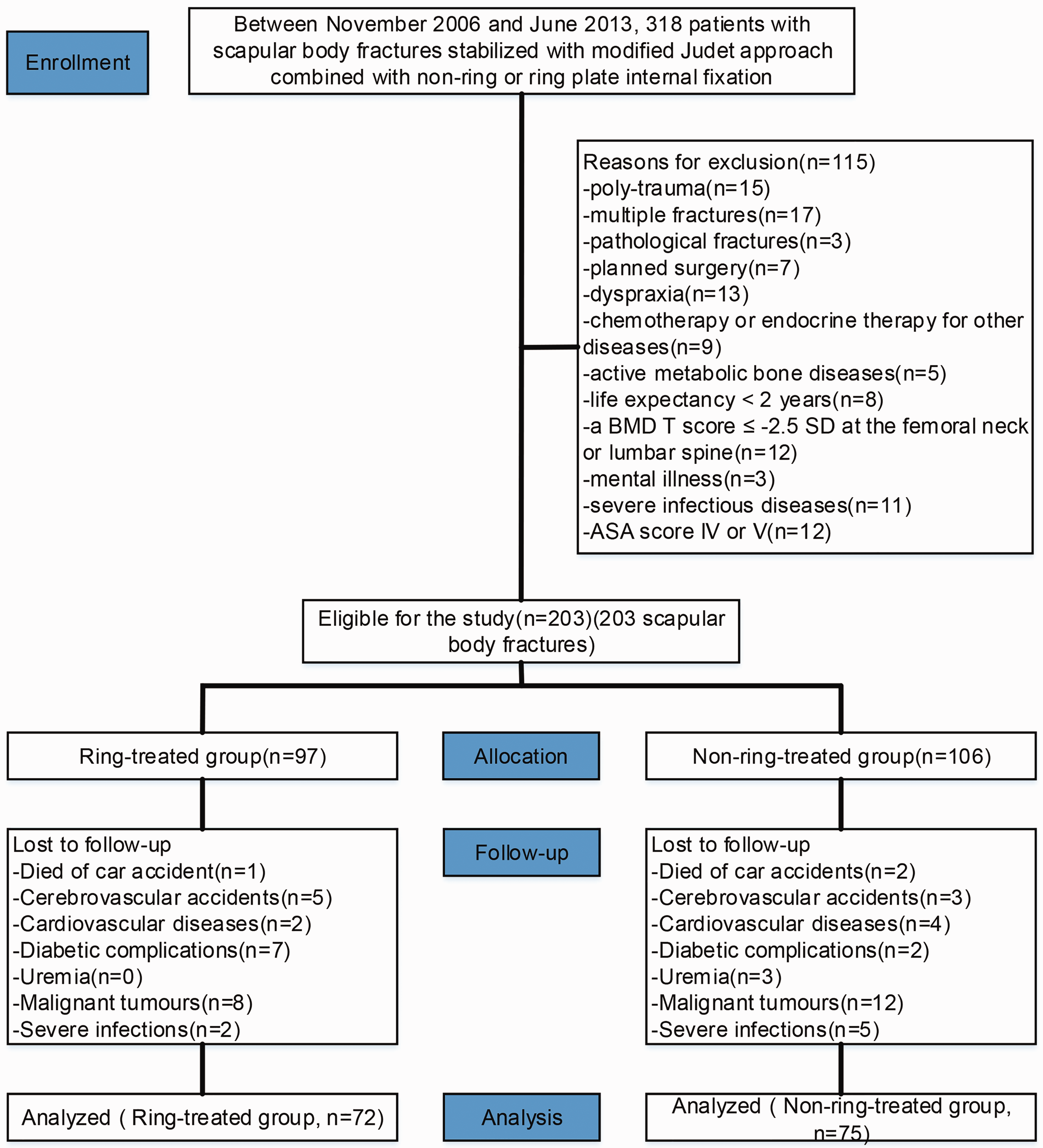
Flow diagram demonstrating the identification of patients in this retrospective study to compare the long-term functional outcomes and complications following a modified Judet approach combined with non-ring or ring plate internal fixation for the treatment of scapular body fractures (AO/OTA classification: 14-A2.2) using the Constant and Murley scores and Disabilities of the Arm, Shoulder and Hand (DASH) scores as the primary endpoints. BMD, bone mineral density; SD, standard deviation; ASA, American Society of Anesthesiologists.
Demographic and clinical characteristics of the patients (n = 147) who were enrolled in this study to compare the outcomes following ring-treated on non-ring-treated surgery for scapular body fractures.

Data presented as mean ± SD or n of patients.
No significant between-group differences (P ≥ 0.05).
ASA, American Society of Anesthesiologists.
Shoulder function, which was assessed as the mean ± SD of all of the Constant and Murley scores up to the final follow-up, was 85.33 ± 4.62 points in the ring-treated group and 81.49 ± 7.12 points in the non-ring-treated group. Significant differences between the two groups were detected at each follow-up, as shown in Table 2.
Long-term follow-up of functional outcomes of the shoulder based on the Constant and Murley score for patients (n = 147) who were enrolled in this study to compare the outcomes following ring-treated or non-ring-treated surgery for scapular body fractures.

Data presented as mean ± SD.
aBetween group comparisons were analysed using independent samples t-test.
The mean and median DASH scores at the final follow-up were 11.1 points and 5 points (range, 0–46 points), respectively, in the ring-treated group; compared with 16.4 points and 8 points (range, 0–67 points), respectively, in the non-ring-treated group. The ring-treated group had significantly lower postoperative DASH scores compared with the non-ring-treated group (P = 0.027).
An increased incidence of clinical complications was observed at the 3-month follow-up with rates of 2.8% (2/72 patients) and 13.3% (10/75 patients) for the ring-treated and non-ring treated groups, respectively (P = 0.033). The difference persisted over time, with significantly more patients in the non-ring-treated group (20.0%; 15/75 patients) experiencing complications compared with the ring-treated group (8.3%; 6/72 patients) (P = 0.043) at the final follow-up (Table 3). Twelve clinical complications in six patients were observed in the ring-treated cohort; 18 clinical complications were noted in 15 patients in the non-ring-treated cohort. There were no statistically significant differences between the two groups in terms of the incidence of refracture, vascular nerve injury, traumatic arthritis, impingement pain, scapular spine fracture, unexplained pain, infection, stiff shoulder secondary to SBF, haematoma, nonunion, and heterotopic ossification at final follow-up. There were statistically significant differences in aseptic loosening (i.e. instability) and malunion between the two groups (P < 0.05 for both comparisons).
Comparison of the complications for patients (n = 147) who were enrolled in this study to compare the outcomes following ring-treated on non-ring-treated surgery for scapular body fractures at final follow-up.
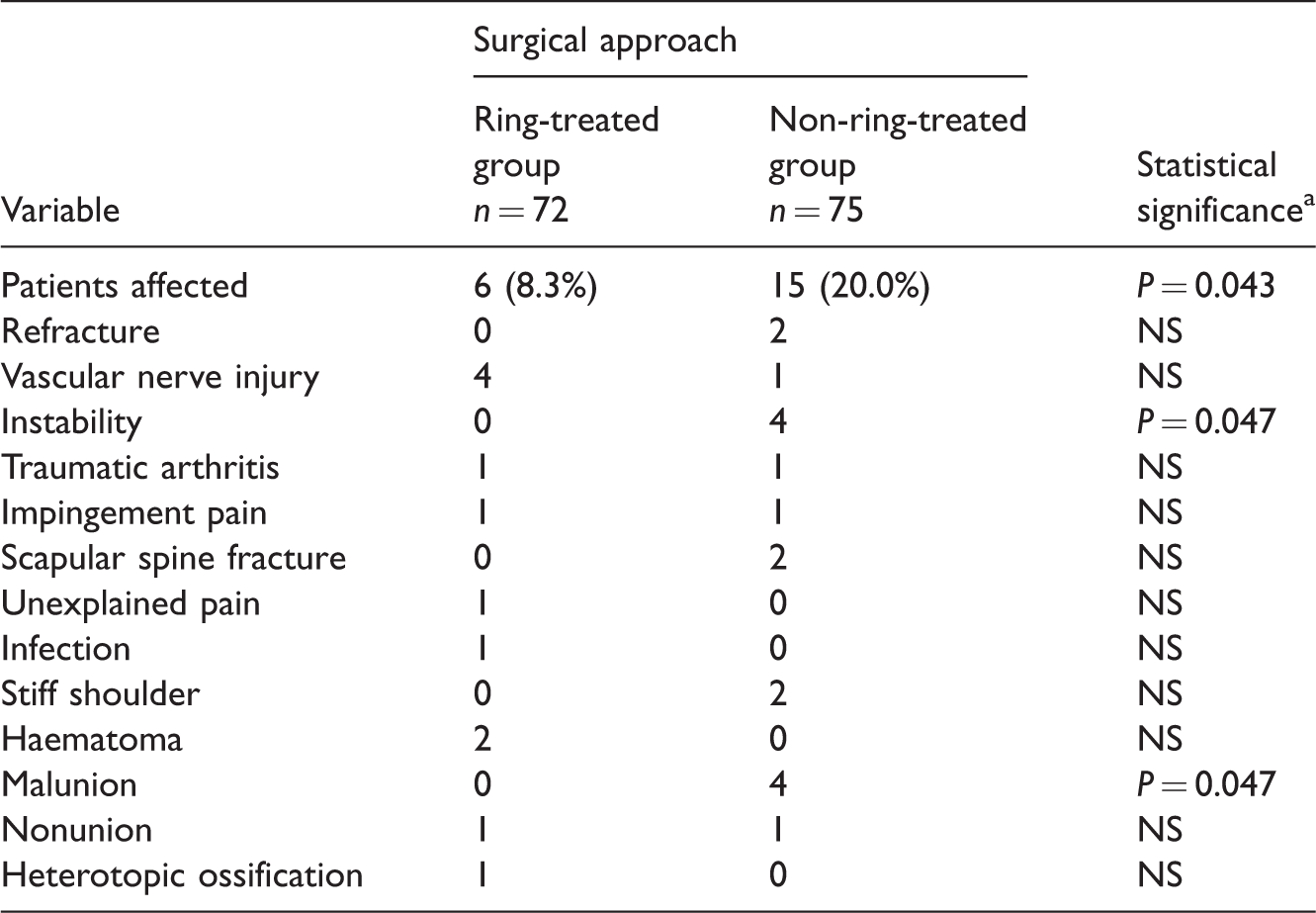
Data presented as n of patients.
aBetween group comparisons were analysed using Pearson’s χ2-test.
NS, no significant between-group difference (P ≥ 0.05).
Discussion
Long-term results following non-ring or ring plate internal fixation procedures for SBFs (AO/OTA classification: 14-A2.2) using Constant and Murley and DASH scores as the primary endpoints have been reported infrequently.5,16,17 The mean duration of follow-up in previous studies was less than 36 months.18,19 In the current study, patients were followed for a mean of 60 months. The most important finding of the current study was that patients undergoing ring plate internal fixation had significantly higher postoperative Constant and Murley scores and lower DASH scores compared with those patients receiving non-ring plate internal fixation.
These current findings are consistent with the mean Constant and Murley score of 78.80 ± 4.45 points reported previously. 2 In this current study, ring plate internal fixation was reliable because the incidence of clinical complications in the ring-treated patients was 8.3%. Furthermore, other studies that compared long-term functional outcomes and clinical complications following the modified Judet approach combined with non-ring or ring plate internal fixation had similar results.1,20,21 A study reported previously demonstrated good functional outcome scores and a low rate of clinical complications (instability and malunion) with 9% compared with 6% at a mean follow-up of 23 months. 15 The present findings demonstrated that there were significant differences between the two groups for two complications, instability and malunion, which was inconsistent with several previous studies that demonstrated an absence of significant differences in these two complications.21–23 For example, a prospective study that included 112 patients with SBFs treated with non-ring or ring plate internal fixation showed no significant differences in these two complications. 21 However, the same prospective study failed to describe the fracture characteristics, such as displacement and the number of fracture fragments, which makes it difficult to evaluate their findings and is a key obstacle in recommending surgical treatment for SBFs. 21
Although several studies have reported that ring plate fixation achieves better results than non-ring plate fixation for the treatment of SBFs, there has been an increasing tendency to perform non-ring plate fixations for SBFs.16,18,19 Generally, a higher clinical complication rate has been detected after non-ring plate fixation than after ring plate fixation.1,19 In the present study, the percentages of instability and malunion were 0.0% and 0.0%, respectively, for the ring-treated group; and 5.3% and 5.3%, respectively, for the non-ring-treated group during the final follow-up, which were in agreement with previous findings.1,14,19 Some researchers have highlighted that the rates of instability and malunion were higher after utilizing non-ring fixation than ring fixation.5,19,21,24 Furthermore, the current study demonstrated higher rates than those published in some previous reports,25,26 but the rates were lower than those published in the more recent reports.5,18 Despite the variable rates of instability and malunion, a consistent difference in the two surgical groups was observed.
Comparison between these current results and those obtained by previous studies revealed some similarities,1,2,19,21 such as the findings for nonunion, stiff shoulder, refracture, traumatic arthritis, or heterotopic ossification between the ring-treated and non-ring-treated groups, but underlined that there were differences regarding the rates of instability and malunion, which appeared to be distinguished by and proportional to the duration of follow-up. In the current study, there were significant differences in the rates of instability and malunion associated with mechanical loosening, which occurred after the 4-year follow-up. Systematic reviews, with or without meta-analysis, reported no significant differences in the rates of instability and malunion after an approximately 3-year follow-up.11,12 A meta-analysis involving 3427 patients in 53 studies demonstrated a fairly low malunion rate (2.2%) when non-ring fixation was utilized. 7 Another report also described a low rate (3.3%) of malunion after a 2-year follow-up period. 9 The current findings were inconsistent with those reported previously, which did not show any significant differences in malunion after a 2-year follow-up period. 26
Previous studies reported that functional outcomes were associated with clinical complications (instability and malunion).11,16,19 These current long-term follow-up results showed that the ring-treated group had significantly higher postoperative Constant and Murley scores and lower DASH scores compared with the non-ring-treated group. These results are inconsistent with the findings of previous studies,1,18,19 which demonstrated that the modified Judet approach combined with non-ring plate internal fixation performed for the treatment of SBFs (AO/OTA classification: 14-A2.2) provided poor functional outcomes due to high rates of clinical complications. There could be a situation in which a previous trauma permanently results in poor outcomes due to fracture sequelae.
Poor Constant and Murley scores were reported previously in a 2-year follow-up study; 17 and a 3-year follow-up study described the deterioration of functional outcomes. 18 Given that the monthly Constant and Murley scores were not available in the present study, it is impossible to ascertain the pattern of the decrease. Nevertheless, as reported previously, 1 weak fixation strength, implant looseness or fracture fragments provide no meaningful benefit on functional outcomes. Furthermore, if the influence of these negative factors continues, the shoulder function will further deteriorate, as reflected in the Constant and Murley score, with grave consequences for the health of patients.
This current study had several limitations. First, it was limited by its retrospective nature, and the retrieval of some information was difficult despite all attempts to obtain the required data, so there were incomplete data for some patients. Secondly, this study was not randomized, and consequently, selection bias was hard to avoid. Thirdly, patient- and surgeon-related confounding factors may have existed. The multi-institutional nature of the database, including the involvement of multiple orthopaedic surgeons, potentially yields a difference in the results across varying surgical techniques and experiences.
In conclusion, this retrospective analysis showed that a modified Judet approach combined with ring plate internal fixation was safe and may provide a better functional outcome and lower rate of clinical complications compared with a modified Judet approach combined with non-ring plate internal fixation. These findings will help inform ongoing discussions about implementation of decision-making surgery in patients with SBFs. However, these current conclusions may be compromised by unmeasured confounders as well as the absence of relevant data or data heterogeneity. In the future, a large prospective study should be performed to determine the impact of these factors.
Footnotes
Declaration of conflicting interests
The authors declare that there are no conflicts of interest.
Funding
Funding for this research was received from the Shanghai Municipal Health and Family Planning Commission (no. 2014-403 and no. 201640057).
