Abstract
Background
Pain management for multiple bone metastases is complex and often requires multidisciplinary treatment. We herein describe patient-centered multidisciplinary pain management for metastatic cancer.
Case presentation: A 61-year-old woman with multiple bone metastases of uterine cervical cancer developed intractable low back pain. After external beam radiotherapy failed, we performed lumbar spinal intralesional curettage, pedicle screw fixation, and nerve decompression. However, the neuralgia persisted. We then percutaneously injected epirubicin into the intervertebral foramina under computed tomography guidance for L5 dorsal root ganglion destruction. Osteoplasty was performed under C-arm X-ray guidance; however, the sacrum was mistaken for the ilium, and treatment was ineffective. We administered zoledronic acid and strontium-89. The last resort was outpatient implantation of an epidural bupivacaine-morphine infusion system. A visual analog scale (VAS) was used for pain evaluation. Lumbar spinal intralesional curettage and fixation, epirubicin-induced ganglion destruction, and administration of zoledronic acid and strontium-89 decreased her VAS pain score from 7–8 to 3–4. Radiotherapy and nerve decompression and release were ineffective, as was osteoplasty because of the location error. The epidural infusion system decreased the VAS score from 7–8 to 2–3 and was highly efficient.
Conclusions
Multidisciplinary integrated treatment for metastatic cancer can be effective.
Keywords
Background
Nearly all patients with cancer will experience pain during the course of their illness, especially patients with multiple bone metastases of various primary cancers. Such pain is usually complex and has a mixed underlying mechanism; hence, the three-step analgesic ladder established by the World Health Organization provides inadequate pain control with only oral or transdermal options. 1 Pain management for multiple bone metastases often requires multidisciplinary treatment and an integrated approach, including surgery, systemic chemotherapy, radiotherapy, interventional therapy, and/or other adjuvant approaches. Surgical resection and nerve decompression are indicated for intractable neuralgia resulting from tumor compression or invasion. If the neuralgia recurs or is not alleviated after surgery, sensory nerve blockade or destruction with neurotoxins such as alcohol, phenol, or adriamycin may be necessary. Strontium-89 and bisphosphonates can also effectively alleviate bone pain. 2 Pain resulting from bone-destructive erosion, periosteal expansion under tension, or structural/mechanical instability may be managed with percutaneous cementoplasty techniques such as vertebroplasty, kyphoplasty, or osteoplasty. An epidural and intrathecal drug infusion system may also be deployed. All of these interventional techniques should be part of a multidisciplinary management program that constitutes the fourth consecutive step of the pain treatment ladder established by the World Health Organization. 3
We herein report a case involving a patient with multiple bone metastases of uterine cervical cancer in which patient-centered multidisciplinary pain management provided integrated palliative care and ultimately formed a nearly painless end-of-life experience until the patient died at home. During the treatment period, some unsatisfactory curative effects and even errors occurred. Consideration of these events will provide physicians with valuable information to avoid such problems in clinical practice. To our knowledge, very few published reports have described such an integrated approach to pain management.
Case presentation
This study was approved by the Shanxi Provincial People’s Hospital ethics committee. The patient’s family provided written informed consent for publication of this report.
A 61-year-old woman presented with a 3-month history of progressive pain affecting her left low back and left lower extremity. Her medical history included hysterectomy for treatment of uterine cervical cancer 4 years previously. She had undergone systemic chemotherapy and radiotherapy after the operation and recovered well. Three months before presentation to our hospital, she developed the above-mentioned pain and underwent computed tomography (CT), magnetic resonance imaging (MRI), and a technetium-99m nuclide bone scan. She was diagnosed with multiple bone metastases of uterine cervical cancer and underwent external beam radiotherapy for the lumbar lesion (30 Gy in 10 fractions); however, the pain became aggravated. Upon admission, her general state of health was moderate, and she was confined to a wheelchair. Physical examination revealed marked left paraspinal tenderness and movement limitation of the lumbar spine with neurological deficits at the level of left L5. A left straight leg raise test was positive, and her L5 neuralgia was severe. Her visual analog scale (VAS) pain score was 8 points (range, 0–10 points), and opioids were administered twice per day. CT and MRI showed ill-defined, erosive lesions in the L5 vertebra and left pedicle as well as tumor infiltration of the L5 exiting nerve root (Figures 1, 2). We performed palliative intralesional curettage, left L5 nerve decompression and release, and unilateral pedicle screw fixation. During the operation, the left half of the L5 vertebra, left pedicle and inferior articular process of L5, and left partial articular process of S1 were resected. The left L5 nerve root was swollen and surrounded by tumor tissue approximately 3 cm from the dura origin. Radical decompression was carried out along left L5 nerve pathway until the outer aspect of the L5/S1 intervertebral foramina was reached. L4 and S1 were fixed with screws through their left pedicles (Figures 3, 4). No bone grafting was performed considering the patient’s short life expectancy. After the operation, her low back pain was alleviated and the L5 neuralgia promptly vanished. However, the L5 neuralgia reappeared on postoperative day 5. Despite administration of mannitol, pregabalin, and Neurotropin® (Nippon Zoki Pharmaceutical Company, Osaka, Japan), the patient’s neuralgia persisted. After fully informing the patient of the curative nature of the procedure and obtaining written consent, we performed percutaneous injection of epirubicin into the intervertebral foramina under CT guidance for left L5 dorsal root ganglion destruction on postoperative day 10. After precise localization under CT guidance, 1 mL of iohexol was injected to verify accurate placement of the needle (18 G), and 1 mL of 0.5% lidocaine was then injected. The patient reported unprecedented comfort after 3 minutes, and 2 mL (10 mg/3 mL) of epirubicin sodium chloride solution was then injected (Figure 5). The L5 neuralgia subsequently became transiently aggravated for about 2 hours and then was markedly alleviated; the patient’s VAS score decreased to 3–4 points, and her extremity movement was normal. She was discharged from the hospital. After 4 weeks, she developed left buttock pain and required retreatment with opioids. CT showed osteolytic destruction on the posterior superior iliac spine, which coincided with her symptom (Figure 6). After readmission, we performed percutaneous osteoplasty under C-arm X-ray guidance. During the operation, the lesion site was difficult to locate by X-ray because of the overlapping bone structures. The patient was still painful postoperatively, and plain radiography and CT showed an incorrect location of the osteoplasty; that is, the sacrum had been mistaken for the ilium despite the fact that the sacrum was also infiltrated with carcinoma (Figures 7, 8). We informed the patient of this occurrence and suggested re-osteoplasty for the iliac lesion under CT guidance. She declined this treatment and requested conservative therapy. We administered 4 mg of zoledronic acid (Zometa; Novartis Pharmaceuticals Corporation, Basel, Switzerland) and 4 mCi of strontium-89 chloride (Metastron; GE Healthcare, Chicago, IL, USA) to relieve the bone metastatic pain and then discharged the patient. Good efficacy was maintained for about 4 months, after which she presented with intolerable squeezing pain in the left buttock and left proximal femur. Her general state was poor and feeble. Surgical implantation of an epidural infusion system containing 20 mL of 0.5% bupivacaine and 2 mg of morphine (one infusion twice a day) was performed on an outpatient basis. She was satisfied with the pain relief, and her VAS score decreased to 2–3 points. She died at home peacefully 3 months later. In summary, lumbar intralesional curettage and fixation, epirubicin-induced ganglion destruction, and administration of zoledronic acid and strontium-89 alleviated her pain from a VAS score of 7–8 to 3–4. Radiotherapy and nerve decompression and release were ineffective, as was osteoplasty because of the location error. The epidural infusion system alleviated her pain from a VAS score of 7–8 to 2–3 and was the most efficient treatment. These results are summarized in Table 1.
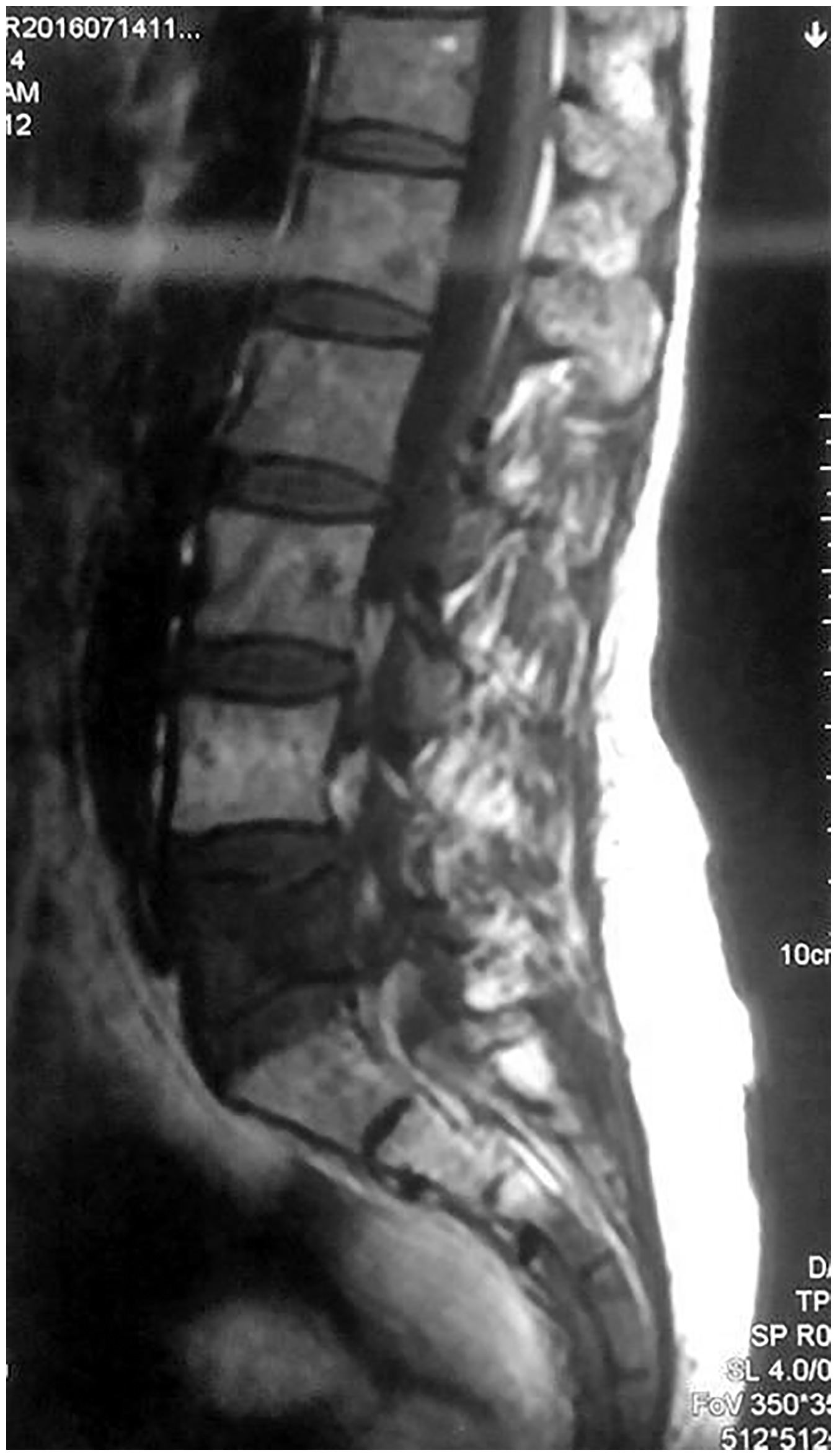
A T1-weighted magnetic resonance image showed ill-defined, hypointense lesions in the L5 vertebra and sacrum.

A T2-weighted magnetic resonance image showed tumor infiltration of the left L5 exiting nerve root in the nerve root canal.
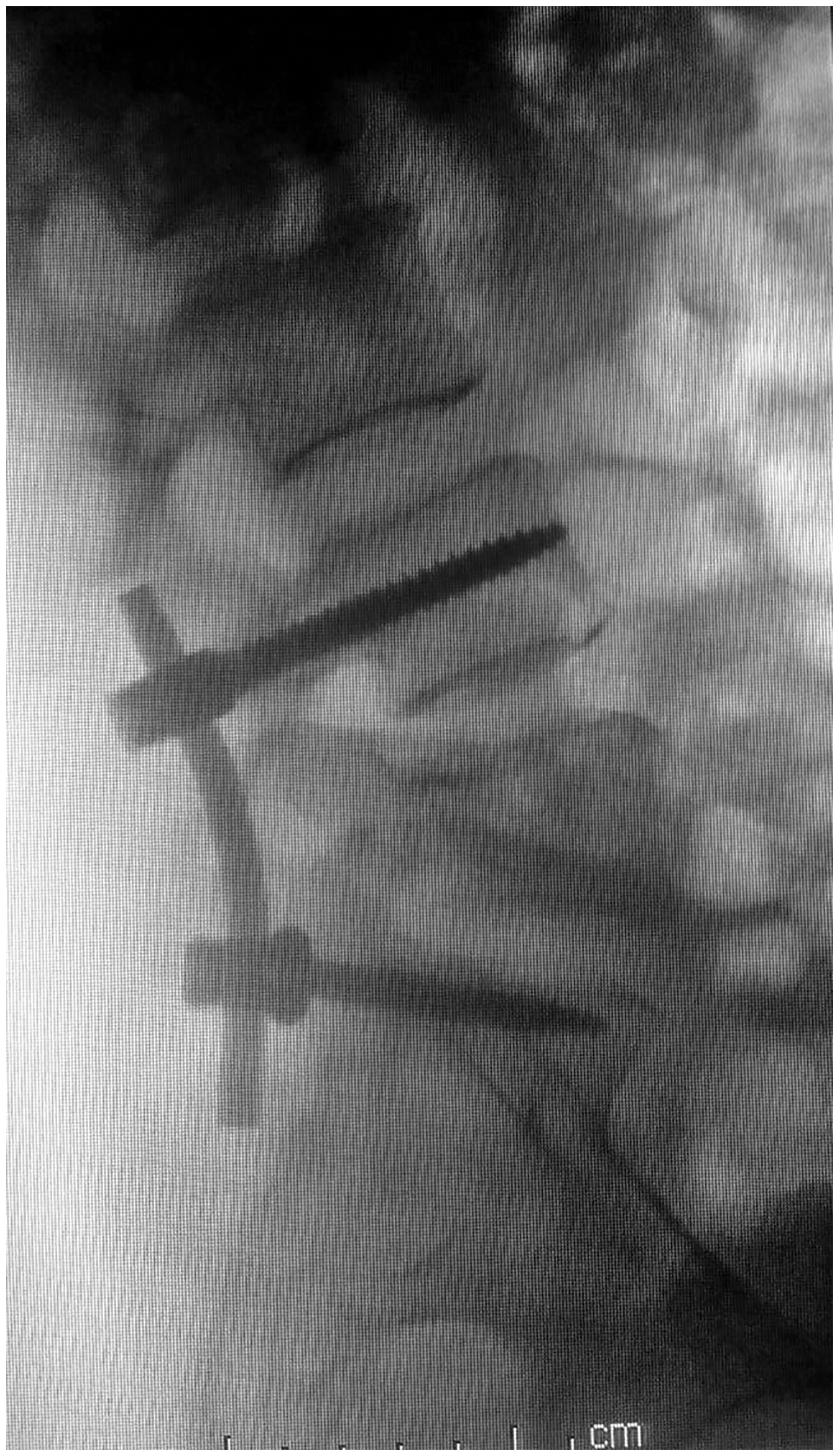
A postoperative lateral radiograph showed the unilateral pedicle screw fixation system for L4 and S1.

Postoperative computed tomography showed the extent of decompression of the L5 left nerve root canal.

Percutaneous injection of epirubicin into the intervertebral foramina under computed tomography guidance for L5 dorsal root ganglion destruction. Iohexol was injected to verify accurate placement of the needle.

Computed tomography showed osteolytic destruction of the posterior superior iliac spine.

A plain radiograph showed the incorrect location of the osteoplasty; i.e., the sacrum was mistaken for the ilium.
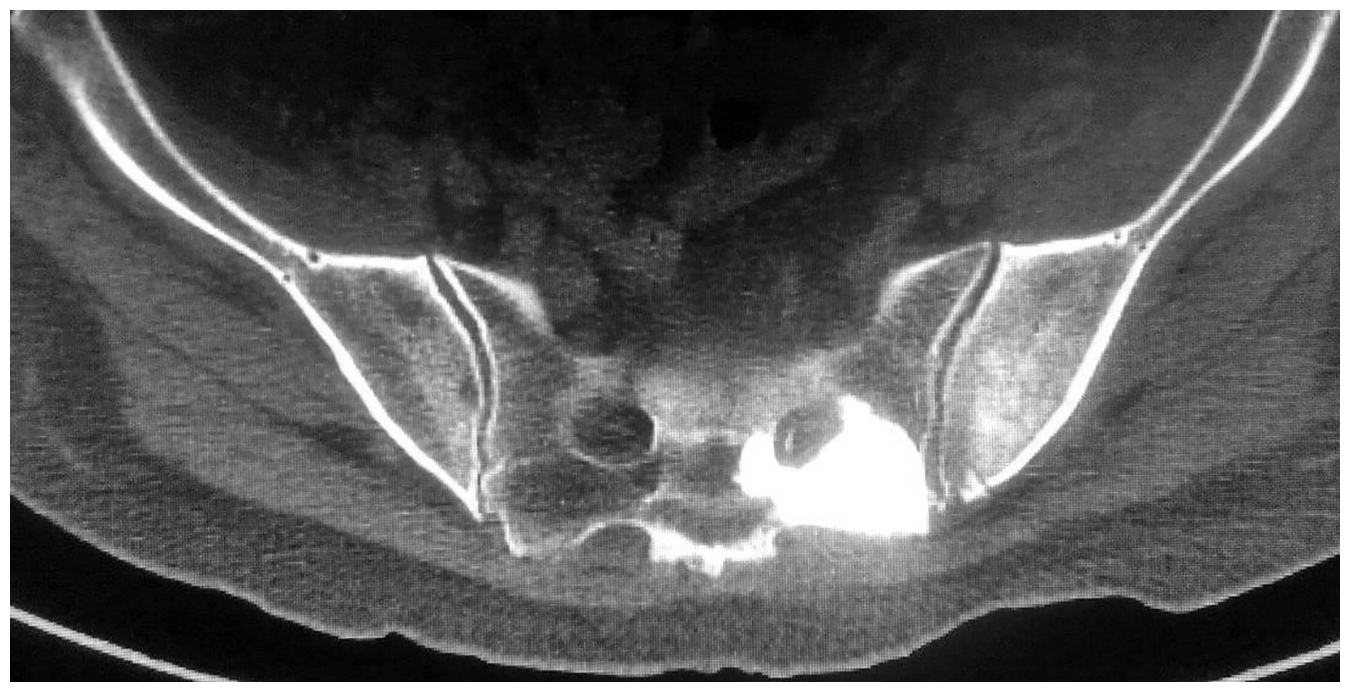
Computed tomography showed the incorrect location of the osteoplasty.
Treatment options and efficacy

mo: months before death; pre: pretreatment; post: post-treatment; VAS: visual analog scale
Discussion
Cancer-induced bone pain develops by multiple mechanisms rather than a single neuropathic, visceral, or inflammatory mechanism. Several possible mechanisms have been reported. 4 However, the exact mechanism remains unclear. Therefore, some patients may be refractory to pharmacological treatment according to the three-step analgesic ladder established by the World Health Organization. Fortunately, many specific interventional pain management techniques can serve as effective alternatives for these patients. Moreover, earlier application of these techniques is recommended before considering the use of strong opioids. 5 Before choosing and utilizing these interventional techniques, the cause of pain should be identified if possible. Additionally, multidisciplinary treatment and cooperation among clinicians from several disciplines are imperative for an integrated program. 6
In the present case, we utilized various palliative methods to alleviate the patient’s metastatic bone pain and eventually gained favorable efficacy. Palliative surgical curettage and stability reconstruction can help the patient leave his or her bed and live actively. Palliative surgery is valuable and beneficial according to evidence-based criteria for selecting patients with advanced cancer.7,8 Although we performed radical decompression and release of the L5 nerve root, the neuralgia quickly recurred postoperatively. We speculate that this was neuropathic pain resulting from tumor infiltration, which causes central sensitization even if the tumor has been eradicated. 9 After medical therapy failed, we resorted to epirubicin injection under CT guidance for L5 dorsal root ganglion destruction. Epirubicin is a cytotoxic agent widely used for systemic, regional, and local chemotherapy. It is the isomer of adriamycin (doxorubicin) and has less cardiac toxicity and a stronger effect than adriamycin. Epirubicin can be swiftly transported to sensory neurons by way of retrograde axoplasmic flow when injected below the epineurium and can induce selective and permanent destruction of the target sensory ganglion cells. This technique is highly selective without any systemic side effects and has been applied for both neuropathic pain and intractable pain such as that caused by malignant tumors. Kato et al. 10 first reported satisfactory clinical effects of this method for the treatment of intractable neuropathic pain. He et al. 11 reported the feasibility and safety of this percutaneous CT-guided combinatorial ablative procedure with and epirubicin mixture. We also obtained a good effect in the present case. After epirubicin injection, the neuralgia was transiently aggravated due to nerve stimulation by the medication. Therefore, we now inject 1 mL of dexamethasone before the epirubicin injection and have noticed that this transient nerve stimulus disappears.
We employed osteoplasty for treatment of the metastatic osteolysis. This technique is a safe and effective treatment for pain caused by metastatic bone tumors in the pelvis and femur. Yamada et al. 12 examined the pain-relieving effects of percutaneous osteoplasty for pain caused by metastatic bone tumors and confirmed that it was technically feasible and could provide durable relief of symptoms. However, we mistook the sacrum for the ilium because of the overlapping bone structures and the consequent inability to attain precise localization by X-ray. This is a valuable clinical lesson. Compared with a fluoroscopy-assisted technique, CT-guided cement injection can decrease the risk of incorrect localization, cement extravasation, nerve injury, and other complications. CT guidance is essential for localization in areas such as the pelvis despite the possibility of greater radiation exposure. We administered zoledronic acid and strontium-89 to take advantage of the two different mechanisms of action of these drugs in reaching and remaining within the bone metastasis. Many studies have confirmed the clinical effectiveness and cost-effectiveness of combining zoledronic acid and strontium-89; both have palliative benefits and are used to control bone symptoms and prolong survival in patients with bone metastasis.13–15 In the present case, the treatment efficacy was maintained for about 4 months, after which the patient developed intolerable squeezing pain at additional sites. Our last resort for pain relief was outpatient-based surgical implantation of an epidural bupivacaine-morphine infusion system. For end-of-life patients with refractory pain, this system may provide profound analgesia with minimal side effects and allow patient care on an outpatient basis. Lin et al. 16 confirmed that a totally implantable programmable drug delivery system was an attractive option for managing refractory cancer pain and could provide reliable long-term analgesia without permanent nerve or plexus destruction. Compared with other methods, we regard this epidural bupivacaine-morphine infusion system as the most efficient for pain relief.
Conclusion
We have herein described a patient with complex and refractory pain requiring comprehensive treatment. Such treatment should be carried out in multiple steps, and each step must be adapted to the stage of the disease. This requires multidisciplinary treatment and an integrated approach. Such a treatment model of palliative care can provide an acceptable quality of life.
Footnotes
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Funding
This research was supported by a grant from the Provincial Natural Science Foundation of Shanxi, China (2010021035-4).
