Abstract
Objective
This study was performed to evaluate the potential predictors of poor outcomes associated with diabetes-specific microvascular pathologies and to analyze their influence on clinical outcomes by adjusting for other well-known prognostic factors in patients with acute ischemic stroke.
Methods
We analyzed 1389 consecutive adult patients with acute ischemic stroke and explored the relationship among clinical characteristics, laboratory measurements, imaging findings, and 6-month functional outcomes.
Results
The final study population comprised 216 patients with both acute ischemic stroke and diabetes mellitus who were followed up for 6 months. A multiple logistic regression analysis of poor outcomes revealed the following independent predictors: leukoaraiosis severity [odds ratio (OR), 7.38; 95% confidence interval (CI), 1.40–38.86, per 1-point increase), diabetic nephropathy (OR, 10.66; 95% CI, 1.10–103.43), and the admission National Institutes of Health stroke scale score (OR, 2.58; 95% CI, 1.36–4.92 per 1-point increase). In this model, admission hyperglycemia and intracerebral hemorrhagic transformation were not independent prognostic predictors.
Conclusion
Microvascular complications (such as nephropathy) caused by diabetes mellitus predict an unfavorable clinical outcome after acute ischemic stroke. Diabetic nephropathy may partly affect post-stroke prognosis by means of exacerbating leukoaraiosis.
Keywords
Introduction
The prognosis after stroke is poor in patients with diabetes. A higher incidence of death or dependency and of recurrent stroke after stroke onset is observed in patients with than without diabetes.1,2 Various predictors associated with long-term functional deficits and mortality after stroke in patients with diabetes have been reported. Hyperglycemia at admission and in the early phase after acute ischemic stroke is associated with a worse functional outcome in patients both with and without diabetes.3–5 The pre-stroke glycemic control status as defined by the glycated hemoglobin (HbA1c) concentration on admission is another predictor of poor outcomes. 6 In a previous study, however, maintenance of the serum glucose concentration within a specific range in the first hours of acute ischemic stroke was not beneficial in terms of the functional outcome, death, or improvement in final neurological deficits and significantly increased the number of hypoglycemic episodes. 7 Previous evidence supports a link between microvascular complications and an increased risk of cardiovascular events in patients with type 2 diabetes. 8 Additionally, chronic nephropathy and proteinuria worsen post-stroke functional outcomes.9,10
This study was performed to explore the relationship between diabetic microvascular complications and a poor prognosis of acute ischemic stroke. We formulated the following hypotheses: (1) Not only hyperglycemia but also chronic microvascular complications of diabetes (diabetic retinopathy, diabetic nephropathy, and diabetic neuropathy) predict an unfavorable post-stroke outcome. (2) These microvascular complications worsen the prognosis by exacerbating cerebral small vessel disease. In the present study, we investigated the relationship between the clinical characteristics and 6-month functional outcomes after acute ischemic stroke in patients with diabetes.
Patients and methods
Patient selection and baseline characteristics
Consecutive patients who were admitted to The 2nd Affiliated Hospital of Chongqing Medical University within 24 hours of acute ischemic stroke onset were enrolled in our single-hospital observational cohort study. Patients with a history of clinically diagnosed stroke were excluded. Our study was performed in accordance with the ethical standards formulated in the Helsinki Declaration. Written informed consent was obtained from all patients before initiation of the study. Ethical approval was obtained from the ethics committee of The 2nd Affiliated Hospital of Chongqing Medical University. The following clinical information was assessed: age, sex, cigarette smoking, alcohol consumption, hospitalization, history of transient ischemic attack, hypertension, diabetes mellitus and its microvascular complications, atrial fibrillation, peripheral artery disease, valvular heart disease, coronary heart disease and prior acute myocardial infarction, congestive heart failure, previous treatment (antiplatelet, anticoagulant, antihypertensive, statins, antidiabetic, and others), baseline body temperature, and systolic and diastolic blood pressure at admission. The stroke etiology was prospectively classified according to the Trial of Org 10172 in Acute Stroke Treatment (TOAST) criteria 11 : large artery atherosclerosis, cardioembolism, small vessel occlusion, and others (either other determined etiology or undetermined etiology). The severity of neurologic impairment was evaluated using the National Institutes of Health stroke scale (NIHSS) and Glasgow Coma Scale at admission and discharge. The therapies after admission were administered according to the published guidelines. 12
Laboratory measurements at admission
The white blood cell count, hematocrit, platelet count, blood urea nitrogen level, serum creatinine level, and international normalized ratio were obtained at admission. The concentrations of total cholesterol, low-density lipoprotein cholesterol, high-density lipoprotein cholesterol, triglycerides, and HbA1c were measured the following day after fasting. The urine protein and ketone levels were evaluated semiquantitatively. The estimated glomerular filtration rate (eGFR) at admission was calculated according to the Modified Diet in Renal Disease equation recommended by the National Kidney Foundation: eGFR (ml/min/1.73 m2) = 186 × [serum creatinine (mg/dl)−1.154 × age (years)−0.203 × (0.742 if female)]. 13
Diagnostic criteria for diabetes mellitus and its chronic complications
The plasm glucose level at admission was measured before administration of intravenous solutions or glucose-lowering therapies. The diagnosis of diabetes mellitus included both known pre-existing diabetes and newly diagnosed diabetes. Known pre-existing diabetes was diagnosed before stroke. The HbA1c level at admission was not an exclusion criterion for known pre-existing diabetes. Patients were newly diagnosed with diabetes according to the following criteria: fasting plasma glucose level of >7.0 mmol/l (126 mg/dl), symptoms of hyperglycemia and a casual plasma glucose level of >11.1 mmol/l (200 mg/dl), and a 2-hour plasma glucose level of >11.1 mmol/l (200 mg/dl) during a 75-g oral glucose tolerance test. 14 Patients with an HbA1c level of <6.5% at admission were excluded to rule out stress hyperglycemia after stroke. 15 Diabetic retinopathy, nephropathy, and neuropathy were recorded at admission. Retinopathy was diagnosed by funduscopic examination or retinal photography according to an established international classification.16,17 This international classification describes the clinical levels of diabetic retinopathy and diabetic macular edema as follows: no apparent retinopathy, mild nonproliferative diabetic retinopathy, moderate nonproliferative diabetic retinopathy, severe nonproliferative diabetic retinopathy, proliferative diabetic retinopathy, macular edema apparently absent, and macular edema apparently present. Nephropathy was diagnosed by the presence of proteinuria or an abnormal eGFR. Specific urinary albumin excretion measurements were not available in this study; therefore, semiquantitative dipstick measurements of albuminuria were used as recommended by the American Diabetes Association guidelines. 18 Neuropathy was diagnosed as a generalized symmetric polyneuropathy or a focal or multifocal neuropathy according to the clinical features and neuroelectrophysiological examination findings as recommended by the American Diabetes Association guidelines. 19 Glucose-lowering therapies and feeding were administered in accordance with published guidelines. 12
Image analysis
Radiographic examinations were used to exclude transient ischemic attack, determine the clinical subtypes of stroke, measure the severity of leukoaraiosis (LA), localize infarcts, and diagnose intracerebral hemorrhagic transformation (HT). Upon admission, all patients underwent brain computed tomography performed with a 64-row detector scanner (GE LightSpeed VCT XTe; GE Medical Systems, Milwaukee, WI, USA). Brain magnetic resonance imaging (MRI) was performed with a 1.5-tesla magnetic resonance system (GE Signa; GE Medical Systems) within 7 days of hospitalization. A standardized stroke protocol was used in all patients and included T2-weighted, T1-weighted, and diffusion-weighted echo-planar images; axial fluid-attenuated inversion recovery images; and magnetic resonance angiography. The modified Fazekas scale was used to rate the severity of LA at baseline on MRI. The patients were accordingly subdivided into three severity groups: grade 0 (no changes); grade 1 (mild changes): single lesions of <10 mm and/or areas of “grouped” lesions of <20 mm in any diameter; grade 2 (moderate changes): single hyperintense lesions of 10–20 mm and hyperintense areas linked by no more than “connecting bridges” of >20 mm in any diameter; and grade 3 (severe changes): both single and confluent hyperintense areas of ≥20 mm in any diameter. 20 Severe LA was defined as a modified Fazekas scale score of ≥3. Intracerebral HT was diagnosed by computed tomography within 1 week after ischemic stroke onset and classified by the method used in the European Cooperative Acute Stroke Study I. 21 The internal carotid artery intima–media thickness (IMT) was measured from the media–adventitia interface to the intima lumen interface by B-mode color Doppler carotid echography. An increased IMT was defined as a thickness of >1.5 mm. All neuroimaging measurements were performed by neuroradiologists or trained sonologists blinded to the clinical data.
Study outcomes
Follow-up was from April 2010 to May 2012. Surviving patients were tracked by regular outpatient consultations or a structured telephone interview of the patients and their families. All patient records available from hospitals and primary care facilities underwent a detailed evaluation. The 6-month outcome was measured by clinicians blinded to the patients’ baseline clinical and imaging data using a 7-point modified Rankin scale (mRS) (0: no symptoms; 1: no significant disability, able to carry out all usual activities despite some symptoms; 2: slight disability, able to look after own affairs without assistance but unable to carry out all previous activities; 3: moderate disability, requires some help but able to walk unassisted; 4: moderately severe disability, unable to attend to own bodily needs without assistance and unable to walk unassisted; 5: severe disability, requires constant nursing care and attention, bedridden, incontinent; 6: dead). An unfavorable outcome was defined as an mRS score of ≥3.
Statistical analyses
Categorical data were compared using the chi-square test. Continuous variables were analyzed using an unpaired t test or the nonparametric Mann–Whitney U test. Scoring variables were analyzed by the Wilcoxon rank sum test. All parameters presented in Tables 1 to 3 were analyzed in univariate and multivariate models to identify significant associations with favorable outcome at 6 months. Adjustments in that analysis were based on univariate significance. Another multivariate logistic regression based on risk factors for cerebral small vessel disease identified by the univariate analysis was performed to identify independent predictors of severe LA. The multivariable model was built by a stepwise selection procedure involving optimization of the Akaike information criterion. The level of significance was set at 95% (P = 0.05). All analyses were performed using SPSS16.0 (SPSS Inc., Chicago, IL, USA).
Baseline and demographic characteristics of all patients
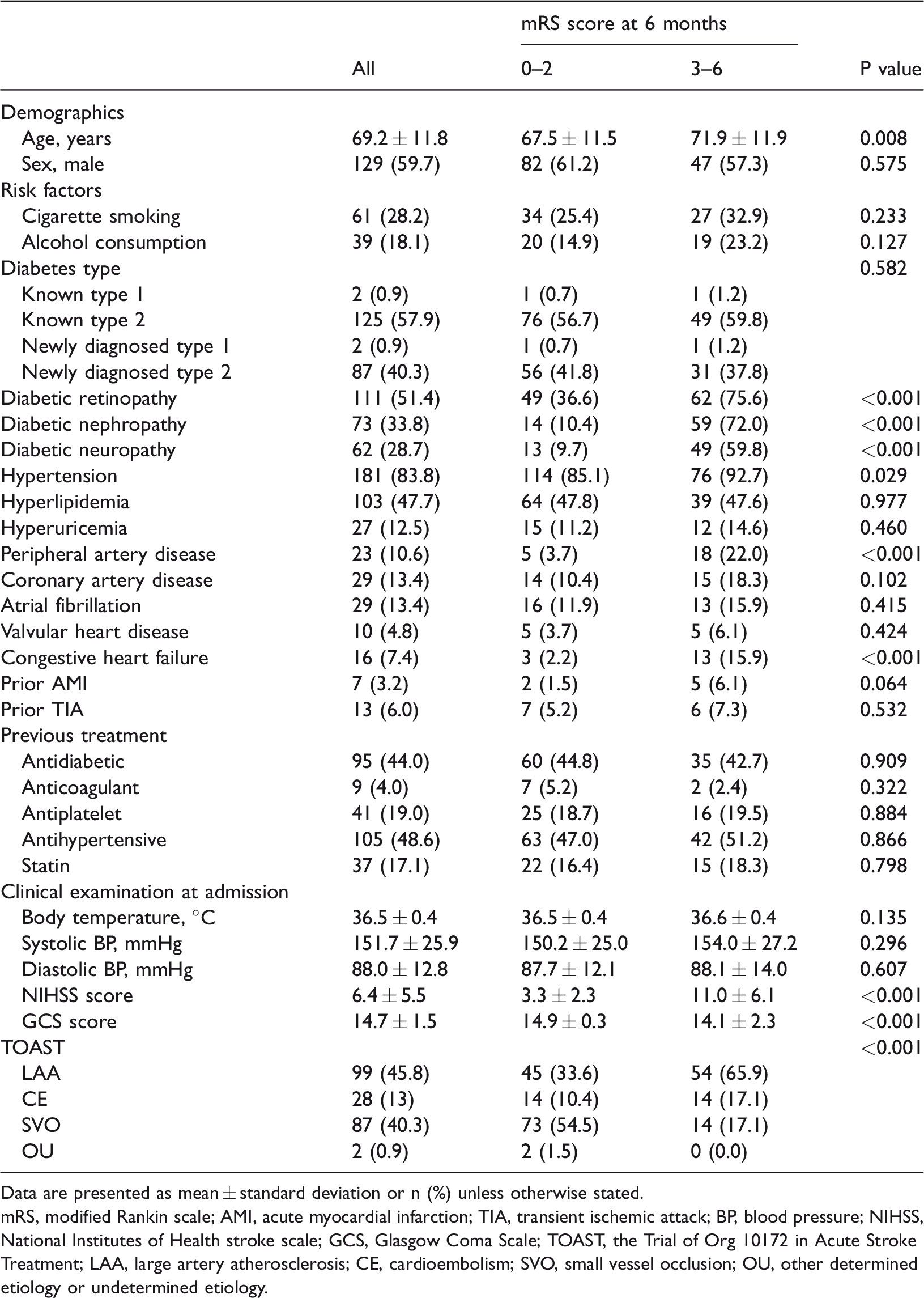
Data are presented as mean ± standard deviation or n (%) unless otherwise stated.
mRS, modified Rankin scale; AMI, acute myocardial infarction; TIA, transient ischemic attack; BP, blood pressure; NIHSS, National Institutes of Health stroke scale; GCS, Glasgow Coma Scale; TOAST, the Trial of Org 10172 in Acute Stroke Treatment; LAA, large artery atherosclerosis; CE, cardioembolism; SVO, small vessel occlusion; OU, other determined etiology or undetermined etiology.
Results
In total, 1389 consecutive adult patients who presented within 24 hours of stroke onset were enrolled from October 2009 to September 2011. Of these patients, 393 (28.3%) were diagnosed with diabetes mellitus. For economic reasons, 102 patients with diabetes refused to undergo cranial MRI or examinations for diabetic complications. Because of changes in the patients’ telephone numbers or family addresses, 75 patients were unable to be followed up. The final study population comprised 216 patients (mean age, 69.2 ± 11.8 years; 59.7% men) who were followed up for 6 months. The mean NIHSS score on admission was 6.4 (interquartile range, 1–28). In total, 89 patients were newly diagnosed during hospitalization, and 127 had known pre-existing diabetes. They were treated with intravenous thrombolysis (n = 3, 1.4%), anticoagulants (n = 26, 12.0%), and antiplatelets (n = 187, 83.0%). A total of 134 patients had a good outcome (mRS score of ≤2) and 82 had a poor outcome (mRS score of ≥3).
The baseline characteristics and demographic characteristics of all patients are shown in Table 1. In the bivariate analysis, a poor 6-month outcome was significantly associated with older age (P = 0.008), a higher prevalence of hypertension (P = 0.029), peripheral artery disease (P < 0.001), congestive heart failure (P < 0.001), diabetic microvascular complications (P < 0.001), and higher admission NIHSS and Glasgow Coma Scale scores (P < 0.001). Furthermore, large artery atherosclerosis was more common in patients with an unfavorable outcome (P < 0.001). Table 2 shows the laboratory measurements at admission and imaging findings. Patients with higher plasma glucose levels at admission had more severe functional deficits 6 months after stroke (P < 0.001). Proteinuria and urine ketones were more frequent in patients with a poor outcome (P < 0.001). The HbA1c level, eGFR, and other laboratory measurements were not statistically significant. Compared with the patients with good outcomes, a higher IMT (P < 0.001), more severe LA (P < 0.001), and more frequent presence of HT (P < 0.001) were observed in the patients with poor outcomes.
Laboratory measurements at admission and imaging findings

Data are presented as mean ± standard deviation or n (%) unless otherwise stated.
mRS, modified Rankin scale; HbA1c, glycated hemoglobin; BUN, blood urea nitrogen; sCr, serum creatinine; eGFR, estimated glomerular filtration rate; IMT, internal carotid artery intima–media thickness; HT, hemorrhagic transformation.
Post-stroke complications of all patients

Data are presented as n (%).
mRS, modified Rankin scale.
Table 3 shows the post-stroke complications. Post-stroke swallowing dysfunction (P < 0.001), infection (P < 0.001), and seizure (P < 0.001) were more frequent in patients with poor outcomes.
After adjusting for potential confounders, age [odds ratio (OR), 1.06; 95% confidence interval (CI), 1.03–1.10; P = 0.001 per 1-year increase], prevalence of hypertension (OR, 1.36; 95% CI, 0.88–2.10), diabetic nephropathy (OR, 3.56; 95% CI, 1.45–8.76; P = 0.006), diabetic neuropathy (OR, 3.33; 95% CI, 1.08–10.25; P = 0.036), and increased IMT (OR, 7.16; 95% CI, 3.03–16.93; P < 0.001 per 1-mm increase) predicted severe LA (Table 4). Initially, a multiple logistic regression analysis of unfavorable clinical outcomes revealed the following independent predictors: the modified Fazekas scale score (OR, 7.38; 95% CI, 1.40–38.86; P = 0.018 per 1-point increase), diabetic nephropathy (OR, 10.66; 95% CI, 1.10–103.43; P = 0.041), and NIHSS score on admission (OR, 2.58; 95% CI, 1.36–4.92; P = 0.004 per 1-point increase). In this model, hyperglycemia at admission was not an independent prognostic predictor, and there was no significant association between the presence of HT and a poor outcome (Table 5).
Independent variables associated with severe leukoaraiosis
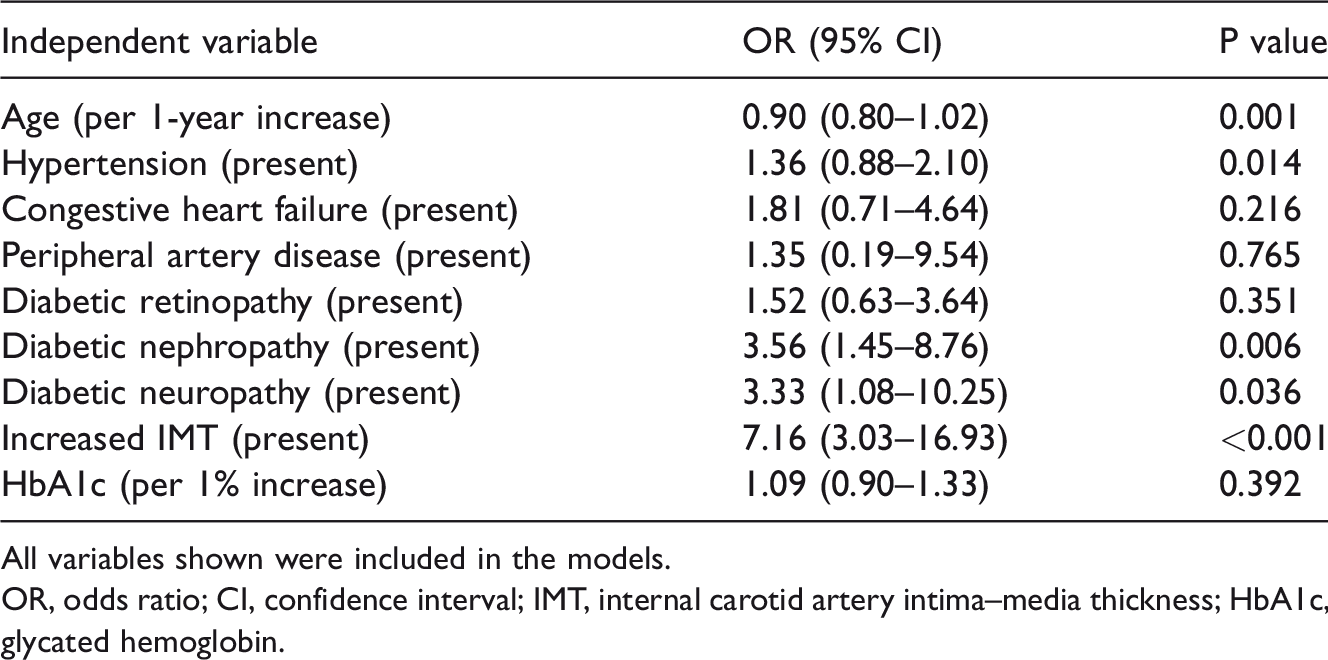
All variables shown were included in the models.
OR, odds ratio; CI, confidence interval; IMT, internal carotid artery intima–media thickness; HbA1c, glycated hemoglobin.
Independent variables associated with poor outcomes

All variables shown were included in the models.
OR, odds ratio; CI, confidence interval; LAA, large artery atherosclerosis; NIHSS, National Institutes of Health stroke scale; GCS, Glasgow Coma Scale; HT, hemorrhagic transformation; IMT, internal carotid artery intima–media thickness.
Discussion
The present study has shown that LA and diabetic nephropathy independently worsen the long-term functional status after acute ischemic stroke in patients with diabetes. LA is a feature of small cerebrovascular pathologies (arteriolosclerosis, cerebral amyloid angiopathy, inherited and genetic small vessel diseases, inflammatory and immunologically mediated small vessel diseases, and others). In patients with diabetes, cerebral small vessel diseases and diabetic nephropathy may have a common pathogenesis such as age (or diabetes duration), hyperglycemia, hypertension, or hypercholesterolemia. 22 Thus, LA may be regarded as a diabetic microvascular complication involving the brain. In regions affected by LA, reduced vascular density and chronically impaired tissue perfusion result in infarct extension. 23 Henninger et al. 24 provided new insight by showing a significant inverse correlation between LA severity and robustness of leptomeningeal collaterals, indicating a collective role in the reduction of autoregulatory mechanisms with subsequently aggravated tissue damage. Furthermore, another previous study demonstrated that severe LA was associated with cognitive impairment, stroke recurrence, impaired functional recovery, and increased mortality. 25
Increasing numbers of researchers 26 believe that LA should be regarded as an intermediate surrogate of stroke more than a risk factor. We demonstrated that diabetic nephropathy and neuropathy were associated with a >3-fold higher risk for severe LA. Cooper 27 stated that diabetic nephropathy is clinically characterized as a triad of renal impairment, proteinuria, and hypertension. However, in the present multivariate analysis, proteinuria and renal impairment were not independent predictors of LA severity or the post-stroke functional outcome when diabetic nephropathy was accounted for. The evidence instead suggests that the deleterious effects of proteinuria and renal dysfunction on cerebral tissue damage may be equivalent to the deleterious effects of diabetic microvascular complications.
Impaired renal function was associated with unfavorable clinical outcomes after stroke in the present study. In other studies, an eGFR of <60 ml/min/1.73 m2 was associated with severe white matter lesions and poor survival in patients with acute stroke. When adjusted for age, sex, risk factors, stroke severity, and subtype, both a low and high eGFR was associated with long-term mortality after ischemic stroke in young patient cohorts.28,29 A potential mechanism underlying poor post-stroke survival with an abnormal eGFR is cerebral small vessel disease. Patients with a lower eGFR have been shown to have a lower deep white matter volume and more white matter lesions. 30 The same association between mild and moderate to severe chronic kidney disease (as identified by the eGFR) and white matter hyperintensity volume using quantitative measures was demonstrated in the Northern Manhattan study. 31 Proteinuria is an early manifestation of chronic kidney disease and is associated with cerebral small vessel disease. 32 It is also associated with a higher risk of progression in patients with lacunar stroke, 33 is associated with severe neurological deficits after stroke, and predicts stroke recurrence and long-term post-stroke mortality.34–36 Some observational studies have demonstrated that microalbuminuria damages endothelial function by increasing serum levels of thrombomodulin 32 and decreasing circulating vascular endothelial growth factor. 37 Large artery stiffening may be another link between albuminuria and cerebral lacunar infarction. 38 From an evolutionary point of view, the “strain vessel hypothesis” states that cerebral hemorrhage and infarction occur most frequently in the area of small perforating arteries that are exposed to high pressure and that must maintain strong vascular tone to provide large pressure gradients from the parent vessels to the capillaries. The glomerular afferent arterioles of the juxtamedullary nephrons are analogous to the perforating arteries. Hypertensive vascular damage occurs first and more severely in the juxtamedullary glomeruli. Therefore, albuminuria may be an early sign of vascular damage to “strain vessels” such as perforating arteries and juxtamedullary afferent arterioles. Albuminuria would indicate an impairment of renal medullary circulation downstream from the juxtamedullary glomeruli and therefore impaired pressure natriuresis, which would lead to salt sensitivity of blood pressure. 39 A previous study showed that diastolic and systolic blood pressure levels were significantly associated with subcortical and periventricular white matter lesions 40 ; in the present study, however, hypertension was not an independent risk factor for LA in patients with diabetes. The hemodynamic explanation for the brain damage caused by chronic nephropathy offered by the “strain vessel hypothesis” has come under question in patients with diabetes.
The major strengths of this study are the large sample of hospitalized patients with a confirmed diagnosis of diabetes and its microvascular complications. A systematic overview 3 indicated that hyperglycemia (including stress-induced hyperglycemia and diabetes mellitus) developed in 30% to 40% of people with acute ischemic stroke. Unlike stress-induced hyperglycemia, diabetes mellitus is a metabolic disease characterized by hyperglycemia resulting from defects in insulin secretion, insulin resistance, or both. The metabolic abnormalities in patients with diabetes are associated with chronic microvascular complications. Therefore, it is very important to distinguish among known diabetes, newly diagnosed diabetes, and stress-induced hyperglycemia. In addition to the well-documented early phase of post-stroke hyperglycemia, continuous glucose monitoring system profiling has demonstrated a late hyperglycemic phase that exists in patients with stroke both with and without diabetes. 41 Post-stroke stress-induced hyperglycemia is easily mistaken for diabetes in clinical practice despite the fact that the plasma glucose level is continuously monitored. An HbA1c level of ≥6.5% at admission indicates pre-existing diabetes.3,15 This criterion was used to reject stress-induced hyperglycemia in the present study. Furthermore, although assessment of urine albumin excretion is an important way to diagnose diabetic nephropathy, 14 some patients with either type 1 or type 2 diabetes have a decreased GFR in the presence of normal urinary albumin excretion. 18 The GFR is another important parameter of overall kidney function. Diagnosis of diabetic nephropathy using two parameters (eGFR and proteinuria) improved the detection rate of renal microvascular damage in this study.
Our study has some limitations. First, for multiple reasons, some patients with diabetes who developed ischemic stroke were registered in this study but subsequently excluded. The findings of this study require verification in a multicenter study with a much larger sample size. Second, the relationship between albuminuria and cerebrovascular damage is considered to be dose-dependent. Microalbuminuria and macroalbuminuria are different risk factors for cerebrovascular disease. A systematic review and meta-analysis 42 identified 7 studies comprising 46,638 participants with 1,479 stroke events. The incident stroke risk was significantly greater for macroalbuminuria than microalbuminuria. Because the levels of albuminuria were measured semiquantitatively in the present study, microalbuminuria and macroalbuminuria could not be accurately distinguished. Although proteinuria was more frequent in patients with poor outcomes, no association was found between proteinuria and the 6-month prognosis in the logistic regression analysis. In our future work, we plan to evaluate the urinary albumin excretion levels after ischemic stroke in patients with diabetes.
In conclusion, the present study has shown that microvascular complications caused by diabetes mellitus predict unfavorable clinical outcomes after acute ischemic stroke. Diabetic nephropathy may affect the post-stroke prognosis by means of exacerbating LA or other conditions.
Footnotes
Acknowledgements
The authors sincerely thank all of the patients for their participation in the study and all of the staff members in the Department of Neurology, 2nd Affiliated Hospital of Chongqing Medical University for their assistance in every step of this study.
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Funding
This work was supported by the Natural Science Foundation of China (Grant No. 81271306).
