Abstract
Objectives:
To evaluate markers of infection and identify risk factors for the development of pneumonia following acute ischaemic stroke in patients with diabetes mellitus.
Methods:
Patients with diabetes mellitus (
Results:
Raised levels of IL-6 and CRP, older age, more severe stroke, longer duration of hospitalization and dysphagia were significantly associated with the development of pneumonia. Patients with pneumonia had significantly worse outcomes compared with nonpneumonia patients after 1 month. Raised WBC count and mean body temperature were not significant predictors of pneumonia.
Conclusions:
Markers of infection, more severe ischaemic stroke, dysphagia and older age may help in predicting the occurrence of pneumonia at stroke onset.
Introduction
Pneumonia is a common cause of death in stroke patients.1–5 The risk of infection may be attributed to stroke-induced immuno -depression syndrome, which is characterized by the loss of lymphocytes, cytokine production, decreased monocyte count and function, and interferon-γ deficiency. These effects on the immune system are associated with pneumonia after stroke.6,7
Various infection biomarkers may facilitate the early diagnosis of pneumonia following acute ischaemic stroke; however, the relationship between these and pneumonia in patients with diabetes mellitus following acute ischaemic stroke is not clear. The aim of the present study was to identify the early predictors of pneumonia and to determine the influence of pneumonia on functional outcome after acute ischaemic stroke, in patients with diabetes mellitus.
Patients and methods
Study Population
This prospective study collected records from consecutive hospitalized patients with ischaemic stroke and diabetes mellitus who were treated at Gansu Province People's Hospital and the Second Hospital of Lanzhou University, Gansu, China, between February 2008 and September 2011. Those patients with symptoms and signs of acute ischaemic stroke, who were treated within 24 h of symptom onset, had diabetes and gave informed consent were eligible for inclusion in the study. Patients were excluded if they had an upper respiratory tract infection, a urinary system infection or were immunocompromised by chemotherapy. At admission, diabetes was diagnosed according to the Expert Committee on the Diagnosis and Classification of Diabetes Mellitus, and pneumonia was confirmed using the Mann criteria.
9
Metabolic syndrome was diagnosed according to the 2006 definition of the International Diabetes Federation.
10
Hypertension was diagnosed according to the Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure.
11
Coronary artery disease was diagnosed according to Libby
The study was approved by the Ethics Committees of the two participating hospitals (Gansu Province People's Hospital and the Second Hospital of Lanzhou University), and patients provided verbal informed consent to participate in the study.
Study Assessments
At admission, patients underwent a computed tomography scan to exclude a diagnosis of haemorrhagic stroke. Body temperature was measured with the patient in a supine position and the mean of the morning, afternoon and evening temperatures was calculated. On the day of admission, blood samples (6 ml) were collected after an 8-h fast. Part of each blood sample was treated with ethylene diamine -tetra-acetic acid to prevent coagulation; the other part was left at for 30 min at room temperature prior to centrifugation at 1400
Stroke severity was assessed by a neurologist using the National Institutes of Health Stroke Scale (NIHSS), 13 which is a 15-item scale for evaluation of the effect of acute stroke on the level of consciousness, language, neglect, visual-field loss, extraocular movement, motor strength, ataxia, dysarthria and sensory loss. Functional outcome was assessed 30 days after the onset of stroke, using the modified Rankin Scale (mRS), 14 which is a 0 – 6 scale ranging from 0 (no symptoms) to 6 (death).
Statistical Analyses
Differences in patient characteristics and clinical variables in pneumonia and nonpneumonia patients were analysed using the χ2-test and two-tailed
Results
In total, 106 patients with diabetes mellitus and acute ischaemic stroke were included in the study. Of these, 32 patients (30.2%) had pneumonia and 74 (69.8%) did not have pneumonia at admission. Their clinical characteristics are shown in Table 1. Patients with pneumonia were significantly older than those without pneumonia (
Baseline characteristics of the patients entered into the present study who had diabetes mellitus, were hospitalized after acute ischaemic stroke and did or did not have poststroke pneumonia on admission

Data presented as mean ± SD or
Analysed by the χ2-test or two-tailed
National Institutes of Health Stroke Scale. 13
Serum levels of IL-6 and CRP, and the WBC count and mean body temperature were significantly higher in patients with pneumonia compared with patients without pneumonia (
Comparison of serum levels of interleukin (IL)-6 and C-reactive protein (CRP), white blood cell (WBC) count and mean body temperature in patients with diabetes who were hospitalized after acute ischaemic stroke and did or did not have poststroke pneumonia on admission

Data presented as mean ± SD.
Analysed by the two-tailed
Pneumonia patients had a significantly worse functional outcome than non -pneumonia patients 1 month after admission, with a greater proportion of pneumonia patients having severe disability (mRS 3 – 6) compared with those with little or no disability (mRS 0 – 2) (
Logistic multiple regression analysis showed that age, stroke severity (higher NIHSS), the levels of IL-6 and CRP, and dysphagia were significantly associated with pneumonia (
Functional outcome assessed using the modified Rankin Scale 14 30 days after the onset of acute ischaemic stroke in patients with diabetes who were hospitalized after acute ischaemic stroke and did or did not have poststroke pneumonia on admission

Data presented as
Analysed by the χ2-test.
Logistic multiple regression analysis of the risk factors for developing pneumonia in patients with diabetes who were hospitalized after acute ischaemic stroke
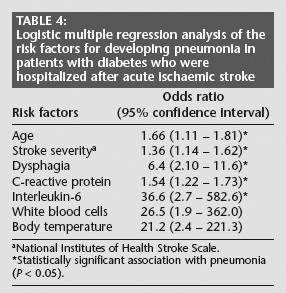
National Institutes of Health Stroke Scale.
Statistically significant association with pneumonia (
Discussion
The prevalence of pneumonia in the present study was 30.2%, which is higher than in previous reports.15–18 Patients with diabetes mellitus, however, are more prone to infection compared with nondiabetic patients, 19 so the inclusion of ischaemic stroke patients with diabetes mellitus in the present study may have contributed to this higher rate of pneumonia. In addition, the patient sample size may have been too small to identify a reliable rate of pneumonia.
The present study demonstrated that the risk of developing pneumonia was significantly higher in older patients with diabetes mellitus following severe ischaemic stroke. In addition, patients with pneumonia at admission had a significantly longer duration of hospitalization and, at 30 days after the onset of stroke, had significantly greater disability according to the mRS. 14 Serum levels of IL-6 and CRP were also significantly associated with pneumonia.
Previous studies have examined various risk factors for infection,4,20–24 including greater stroke severity on admission, total anterior circulation infarction, Barthel Index < 5, Glasgow Coma Scale score < 9, infarction in the region of the middle cerebral artery, older age, current atrial fibrillation, tube feeding and history of congestive heart failure. Amelioration of neurological impairment and prevention of complications are already major goals of stroke treatment. Conservative measures provide limited protection against poststroke pneumonia, raising the possibility that stroke-induced alteration of the systemic immune response might be important.
The present study showed that risk factors for pneumonia include older age, stroke severity, dysphagia and raised serum levels of IL-6 and CRP. The raised IL-6 and CRP levels could be attributed to stroke-induced immunodepression syndrome, in which case modulating these cytokines and the immune system may be potential new treatment strategies for acute ischaemic stroke with pneumonia. 25
The relationship between an increased risk of infection and more severe ischaemic cerebral infarctions, based on a raised NIHSS on admission, has previously been established.26–29 Several randomized trials have demonstrated a reduction in the infection rate in stroke patients treated prophylactically with antibiotics.30–33 Thus, the early initiation of antibiotics in older patients with severe ischaemic stroke should be considered in order to improve clinical outcome.
In conclusion, older patients with more severe ischaemic stroke are more susceptible to developing pneumonia during hospitalization, which contributes to poor functional outcome. Increased levels of IL-6 and CRP, older age, a higher NIHSS and dysphagia may predict the occurrence of pneumonia on the day of stroke symptom onset. Early identification and treatment of these patients may improve clinical outcomes.
Footnotes
The authors had no conflicts of interest to declare in relation to this article.
