Abstract
Rosai-Dorfman disease (RDD) or sinus histiocytosis with massive lymphadenopathy is a rare benign disorder usually characterized by massive painless cervical lymphadenopathy and systemic manifestations. Extranodal involvement, especially spinal involvement, is extremely rare. We report a 41-year-old man who presented with only intermittent dorsodynia. His condition was diagnosed as non-specific inflammatory disease on the basis of preoperative puncture biopsy results. We performed total surgical resection. Histopathological findings showed distinctive emperipolesis and immunohistochemistry results were positive for cluster of differentiation CD68 and S100 and negative for CD1a. A good prognosis was confirmed at the 3-month follow-up visit. This is the first case of RDD of the subdural spine with such a long segment lesion. There is still no consensus regarding appropriate therapy for this type of RDD and the preoperative diagnosis remains challenging. The unusual presentation of our case serves as a reference when diagnosing and treating RDD.
Introduction
Rosai-Dorfman disease (RDD) is a rare histioproliferative disorder that was first described as sinus histiocytosis with massive lymphadenopathy in 1969; and it was subsequently defined as a benign lymphohistiocytic proliferative condition involving the lymph nodes.1,2 It is commonly characterized by massive, painless bilateral lymph node enlargement in the neck and it is frequently associated with a fever. 2 Extranodal involvement, including the central nervous system (CNS), oculi, upper respiratory tract, skin, head, and neck, is very rare. Isolated intramedullary spinal RDD is especially rare, as less than 50 cases of CNS involvement have been reported, and isolated intramedullary involvement has only been reported in three cases.3–6
Case report
A 41-year-old man presented to the Department of Orthopaedics, Union Hospital, Tongji Medical College, Huazhong University of Science and Technology, Wuhan, Hubei Province, China in December 2015 with a 1-year history of intermittent dorsodynia that radiated to the chest. There was no fever, palpable lymph nodes, or skin lesions. The patient was started on steroids and he showed immediate neurological improvement. However, his symptoms quickly reappeared. A thoracic magnetic resonance imaging scan showed oval epidural, long flake, space-occupying lesions located at the C7–T7 level of the spinal cord that were isointense on T1-weighted imaging and hypointense on T2-weighted imaging. A dura tail sign, which is usually indicative of intraspinal meningioma, was observed. The paravertebral regions were also involved at the level of T5 vertebrae (Figure 1). The strength of both limbs was a 5/5 grade, muscular tension was normal, and pathological reflex was negative. Whole-body bone scanning and a bone marrow smear were undertaken to help diagnosis. The whole-body bone scan showed heterogeneously increased tracer at the T2 and T3 vertebrae (Figure 2). The bone marrow smear showed actively proliferating cells (Figure 3A). To establish a tissue diagnosis, the patient underwent a computed tomography-guided biopsy of the paravertebral mass and chronic inflammation was observed (Figure 3B).
Thoracic magnetic resonance imaging scans of a 41-year-old man with a 1-year history of intermittent dorsodynia: (A) sagittal T2-weighted images showed oval epidural, long flake, space-occupying lesions located at the C7–T7 level of the spinal cord that were hypointense; (B) sagittal T1-weighted images with contrast demonstrated homogeneous enhancement of the lesion and the dura tail sign was also observed (arrowhead); (C) the paravertebral regions were involved in T5 vertebrae (axial of T5). A whole-body bone scan of a 41-year-old man with a 1-year history of intermittent dorsodynia demonstrated heterogeneously increased tracer at the T2 and T3 vertebrae. Representative photomicrograph of a bone marrow smear taken from a 41-year-old man with a 1-year history of intermittent dorsodynia showed that the cells of the marrow were actively proliferating (May-Giemsa stain). Scale bar 50 µm (A). A preoperative computed tomography-guided puncture biopsy specimen of the paravertebral mass showed numerous plasma cells and a small number of lymphocytes, which were considered to be indicative of chronic inflammation (haematoxylin and eosin). Scale bar 125 µm (B). The colour version of this figure is available at: http://imr.sagepub.com.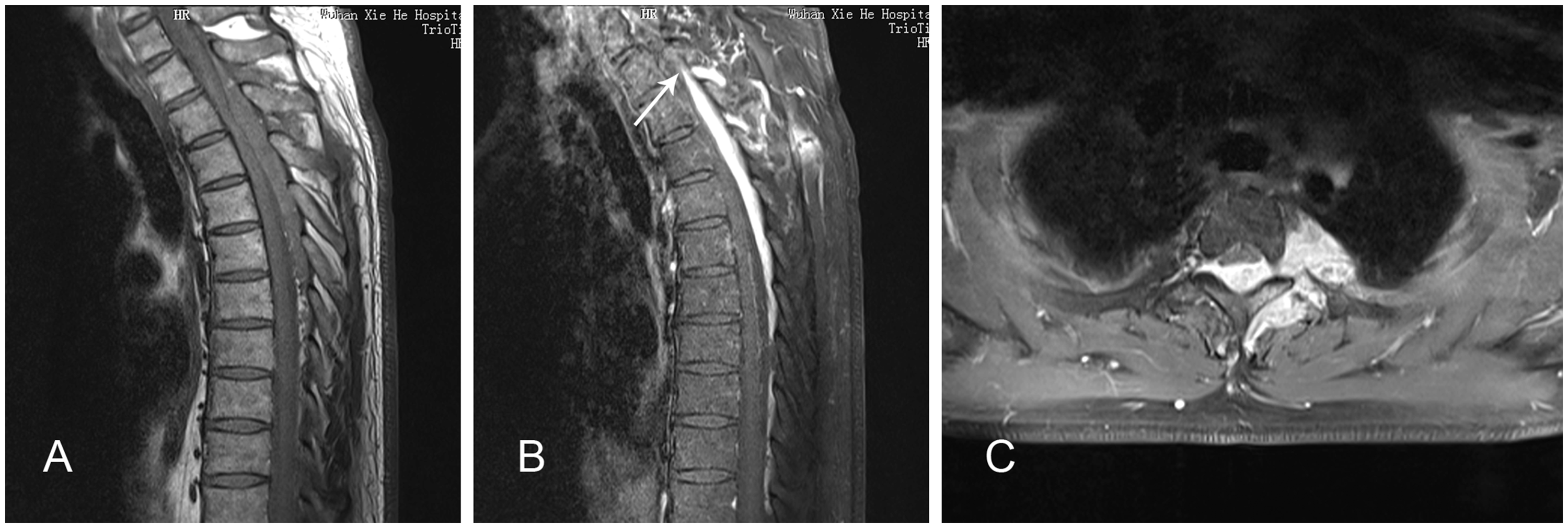


Surgery was undertaken to debulk the lesion completely and release the pressure on the nerve root. Pedicle screw fixation was used to restore spinal stability (Figure 4).
Postoperative thoracic radiographic scans showing pedicle screw fixation that was used to restore spinal stability.
Postoperative immunohistochemical staining of the specimen showed that the histiocytes were positive for CD68 (Figure 5A), CD163 (Figure 5B) and S100 (Figure 5C), but they were negative for CD1a and CD34 (images not shown). The ratio of the κ and λ expression was normal, which helped to exclude multiple myeloma. Postoperative histopathological examination showed that the specimen had an ample amount of fibrous connective tissue and there was a massive amount of diffuse or nodular tissue cell, lymphocyte, and plasma cell infiltration. Typical emperipolesis, a characteristic feature of RDD, was found in haematoxylin-eosin sections (Figure 5D). The lymphocytes and plasma cells were engulfed in histiocytic cytoplasm. All of these findings were suggestive of RDD.
Representative photomicrographs showing positive immunohistochemical staining of neoplastic cells for cluster of differentiation CD68 (A), CD163 (B) and S100 (C). Haematoxylin-eosin stained sections showed emperipolesis, a characteristic feature of Rosai-Dorfman disease. The lymphocytes and plasma cells were engulfed in histiocytic cytoplasm (D). Scale bar 50 µm. The colour version of this figure is available at: http://imr.sagepub.com.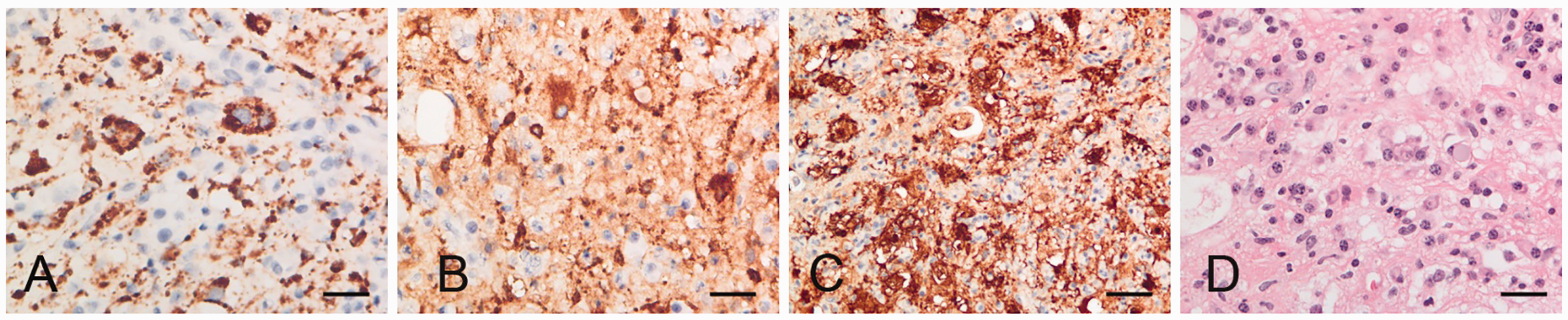
Postoperatively, the patient reported that the symptoms of dorsodynia improved significantly. However, his sensation and strength were similar to that preoperatively. As the lesion was completely resected, postoperative chemotherapy and radiotherapy were not recommended. A good prognosis was confirmed at the 3-month follow-up visit.
Discussion
Histology
Usually histiocytes derived from the CD34+ stem cell and CD34+ progenitor cell develop along two major pathways, and they differentiate into either Langerhans cells (CD1a+, Langerin+, CD68–, and S100+) or non-Langerhans cells (CD1a–, CD68++, and S100+/–).7,8 Two previous reports proposed that most cases of non-Langerhans cell histiocytosis (non-LCH) are derived from the same precursor cell, and that they also have an identical immunophenotype (factor XIIIa+; CD68+, CD163+, CD14+; S100–, CD1a–); they referred to these disorders as the juvenile xanthogranuloma (JXG) family.9,10 However, RDD is a systemic non-LCH derived from another cell line. Pathologically, it is called the non-JXG family. RDD is usually self-limiting because of the accumulation of S100+, CD1a–, CD68++, fascin++, and CD163++. 11 Emperipolesis is a characteristic feature in which erythrocytes, lymphocytes, or plasma cells are engulfed in histiocytic cytoplasm (Figure 5D).12,13 Although emperipolesis is not unique to RDD, it is usually considered diagnostically significant when combined with positive S100 protein expression. The S100 protein is considered a constitutive protein of RDD.1,13
Aetiology
The aetiology of RDD remains unknown; however, many studies have demonstrated that the main pathogenic factors are immune or autoimmune dysfunction.8–10 Moreover, some infectious factors such as the human papillomavirus-6, Epstein-Barr virus,
Disease presentation and diagnosis
The mean age of onset is 20.6 years, but there is a wide age distribution. 15 The most common presentation is painless cervical adenopathy, and it usually presents with some systemic symptoms such as a fever, night sweats, malaise, and weight loss in the short term.12,15,16
Extranodal involvement accounts for about 40% of cases, and usually the orbits, skin, upper respiratory system,12,16 and CNS involvement accounts for less than 5% of cases.17–19 Laboratory findings usually show an increased erythrocyte sedimentation rate (88.5%) and hypergammaglobulinaemia (75%). 20 A case report described a patient in whom the dural tail sign was observed on imaging (i.e. the lesion was attached to the dura mater), and this sign usually suggests spinal meningioma; the authors proposed that RDD should be differentiated from a common intraspinal dural-based lesion. 21 RDD has a variety of imaging manifestations, 22 so the diagnosis of RDD usually requires histological confirmation.
Treatment
The therapeutic methods for treating the CNS manifestations of RDD are controversial, but they include the use of surgical resection, radiotherapy, immunomodulatory agents and corticosteroids. However, the main treatment method for spinal RDD is usually to undertake a total resection or subtotal resection if the mass. Importantly, RDD with CNS involvement is usually sensitive to corticosteroids, which supports the hypothesis that RDD is essentially an exaggerated immunological dysfunction.23,24 Complete surgical resection has been proven to result in a good outcome.2,17 A report described recurrences in a case in which the lesions were not completely resected. 25 The authors used low-dose radiotherapy to treat this patient. 25 Corticosteroids are also proven to be effective in these patients.6,26,27
Conclusions
Rosai-Dorfman disease with a long segment subdural spine lesion is an extremely rare disease and the diagnosis of spinal RDD is challenging. Surgical resection as a kind of diagnostic method and treatment has been proven effective; however, more research is expected to improve the preoperative diagnostic rate and determine more treatment options. Long-term outcomes and the postoperative prognosis also remain unclear.
Footnotes
Declaration of conflicting interests
The authors declare that there are no conflicts of interest.
Funding
This study was funded by grants from the National Natural Science Foundation of China (Grant numbers: 81072187 and 81541056).
