Abstract
Objectives
To examine associations between red blood cell distribution width (RDW) and organ involvement and disease activity in patients with Behçet’s disease.
Methods
Haematological and inflammatory parameters including RDW, high-sensitivity C-reactive protein (hsCRP) and erythrocyte sedimentation rate (ESR) were examined in patients with Behçet’s disease and in healthy controls. Patients were divided into those with active or inactive disease.
Results
Data from 236 patients with Behçet’s disease (77 with active and 159 with inactive disease) and 72 controls were analysed. RDW, ESR and hsCRP were significantly higher in patients with Behçet’s disease than in controls, and in those with active disease compared with inactive disease or controls. In addition, ESR and hsCRP were significantly higher in those with inactive disease than controls. No correlations were found between hsCRP, ESR and RDW. No differences were observed in RDW, ESR or hsCRP between patients with or without ocular or vascular involvement. Multivariate logistic regression analysis revealed that RDW was significantly higher in active disease compared with inactive disease.
Conclusions
RDW was increased in active disease compared with inactive disease. No relationships were found between organ involvement and RDW. RDW may be a cost-effective, novel potential parameter to evaluate disease activity in Behçet’s disease.
Keywords
Introduction
Haematology autoanalysers not only count and size circulating cells but also determine cell volume and variation in cell size. 1 The red blood cell distribution width (RDW; also known as the red blood cell distribution width-coefficient of variation) is an indicator of erythrocyte heterogeneity or anisocytosis. It is calculated by dividing the standard deviation of the mean cell size by the mean cell volume of red blood cells and multiplying by 100 to convert to a percentage. 2 An elevated RDW can be seen in diseases such as anaemia, renal dysfunction, thyroid disease, hepatic dysfunction, nutritional deficiencies (iron, vitamin B12 and folic acid), bone marrow dysfunction, cancer, diabetes mellitus and inflammatory disease. 3 Studies report that RDW was associated with inflammatory indices such as C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR).4–7
Behçet’s disease is a chronic, recurrent, multisystemic inflammatory disorder. It is characterized by involvement of the mucocutaneous, urogenital, ocular, vascular, locomotor, neurological, gastrointestinal and respiratory systems, and inflammatory attacks. 8 Both ESR and CRP have been used to assess activity in Behçet’s disease. 9 Although other investigational markers have been identified, they are not routinely used in clinical practice since they are not easily measured and clinical values have not been established.10,11
The aim of the present study was to investigate whether RDW may have potential as a diagnostic marker in Behçet’s disease by examining associations between RDW, organ involvement and disease activity.
Patients and methods
Patients
Patients with Behçet’s disease were identified retrospectively from the database of the Rheumatology Department, Faculty of Medicine, Gaziantep University, Gaziantep, Turkey. The study was conducted between January 2007 and August 2013. Patients were diagnosed according to the International Study Group criteria for Behçet’s disease. 12 Exclusion criteria included autoimmune disease (such as Sjögren’s syndrome, rheumatoid arthritis and inflammatory bowel disease), malignant disease, thyroid disease, bone marrow dysfunction, diabetes mellitus, end-stage renal disease and liver disease. Demographic parameters such as age, sex, clinical features and organ involvement were obtained from patient records. Controls consisted of healthy volunteers who were recruited prospectively from members of hospital staff or patients’ relatives. Patients and controls were age- and sex-matched.
Written consent had been obtained from all patients as standard practice on admission to hospital, covering the use of their data for research purposes. All controls gave written informed consent when recruited. The study protocol was approved by the Clinical Research Ethics Committee of Gaziantep University (no. 40/2013) and conducted according to the Declaration of Helsinki.
Patients with Behçet’s disease were divided into those with active disease and those with inactive disease, using the Turkish version of the simplified Behçet’s Disease Current Activity Form (BDCAF).13,14 Active disease was defined as a BDCAF value ≥2. Those with active disease were being treated with standard regimens, involving immunosuppressive and anti-inflammatory drugs.
Laboratory measurements
Complete blood count, high-sensitivity CRP (hsCRP) level and ESR were measured. Blood samples were obtained following an overnight fast and were drawn from the antecubital vein for immediate analysis. Blood assayed for hsCRP was collected in standard serum gel biochemistry tubes. hsCRP levels were measured using an immunonephelometry assay on a Dade Behring Nephelometer BN II device (Siemens Healthcare GmbH, Erlangen, Germany). Blood for ESR measurement was collected in citrated glass tubes; ESR was measured using a traditional Westergren method. Blood collected in tubes containing ethylenediaminetetra-acetic acid was analysed to give a complete blood count, including RDW, haemoglobin, mean corpuscular volume (MCV), white blood cell count (WBC), red blood cell count (RBC), lymphocytes, neutrophils, haematocrit, mean corpuscular haemoglobin (MCH) and mean corpuscular haemoglobin concentration (MCHC), using a Coulter LH 780 device (Beckman Coulter, Miami, FL, USA).
Statistical analyses
Based on the reference values of RDW for healthy subjects, the minimum sample size required was determined as 54 in each group to demonstrate a significant difference of 1 ± 2 units between patients with Behçet’s disease and controls (α = 0.05, 1−β = 0.80).
Results were given as n patients or mean ± SD. The distribution of continuous variables was evaluated using the Kolmogorov–Smirnov test. Two normally distributed variables were compared using Student’s t-test, with Mann–Whitney U-test being used for non-normally distributed variables. Analysis of variance and least significant difference multicomparison tests were used to compare more than two normally distributed variables, while Kruskal–Wallis and pairwise multicomparison methods were used for non-normally distributed variables. The χ2-test was used for the analysis of associations between categorical variables. Pearson’s correlation coefficient test was used for correlation analysis of hsCRP, ESR, RBC, haemoglobin, MCV and MCHC against RDW. Multivariate logistic regression was used to adjust for the effect of other possible factors. Receiver operating characteristic (ROC) analysis was performed to assess the ability of RDW to differentiate patients with Behçet’s disease from healthy controls and active from inactive disease. A P-value < 0.05 was considered to be statistically significant. All statistical analyses were performed using IBM SPSS® software, version 22 (IBM, Somers, NY, USA).
Results
A total of 236 patients with Behçet’s disease (131 male; 105 female) and 72 controls (38 male; 34 female) were included in the study. Of the patients with Behçet’s disease, 77 had active disease and 159 had inactive disease.
Demographic and haematological parameters in patients with active or inactive Behçet’s disease and controls.
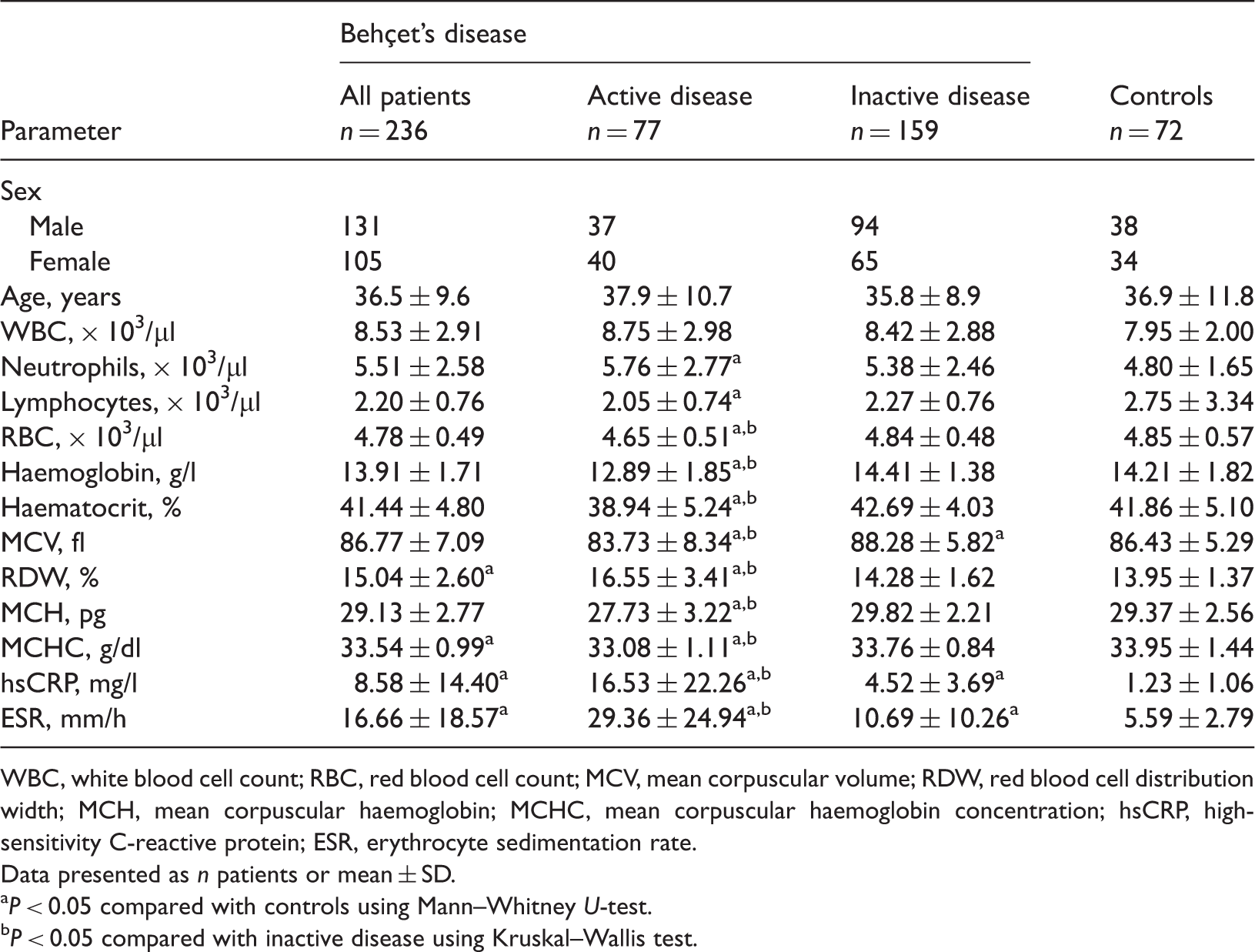
WBC, white blood cell count; RBC, red blood cell count; MCV, mean corpuscular volume; RDW, red blood cell distribution width; MCH, mean corpuscular haemoglobin; MCHC, mean corpuscular haemoglobin concentration; hsCRP, high-sensitivity C-reactive protein; ESR, erythrocyte sedimentation rate.
Data presented as n patients or mean ± SD.
P < 0.05 compared with controls using Mann–Whitney U-test.
P < 0.05 compared with inactive disease using Kruskal–Wallis test.
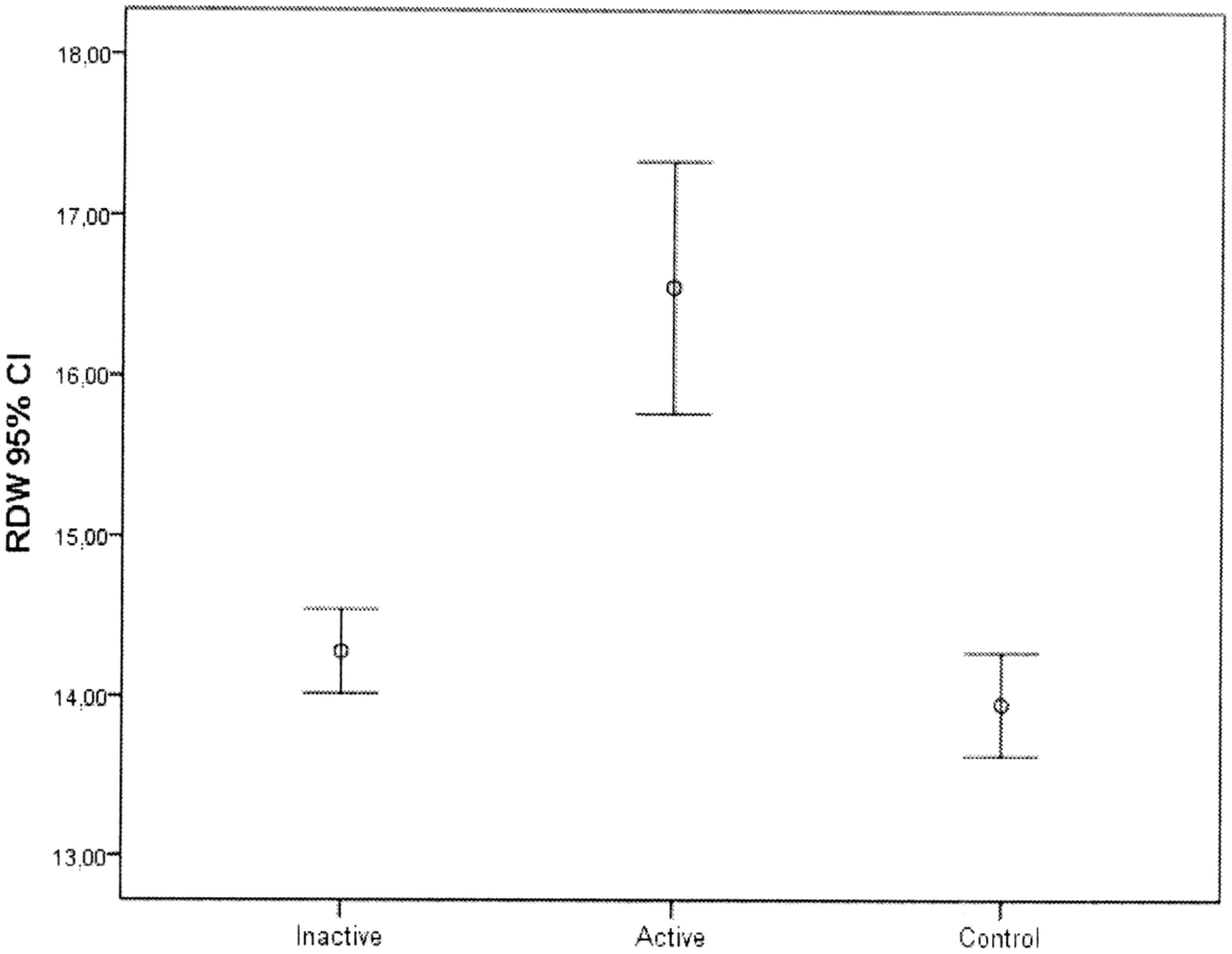
Red blood cell distribution width (RDW) in patients with active or inactive Behçet’s disease and controls; data shown are mean ± 95% confidence intervals (CI).
Haematological parameters in patients with Behçet’s disease with or without ocular or vascular involvement.

WBC, white blood cell count; RBC, red blood cell count; MCV, mean corpuscular volume; RDW, red blood cell distribution width; MCH, mean corpuscular haemoglobin; MCHC, mean corpuscular haemoglobin concentration; ESR, erythrocyte sedimentation rate; hsCRP, high-sensitivity C-reactive protein; NS, not statistically significant (P ≥ 0.05) using Mann–Whitney U-test.
Data presented as mean ± SD.
There were moderate negative correlations between RDW and haemoglobin (r = −0.452, P < 0.001), haematocrit (r = −0.479, P < 0.001) and MCV (r = −0.356, P < 0.001) in patients with active Behçet’s disease. No correlations were found between RDW and ESR or hsCRP in either active or inactive disease. There was a moderate negative correlation between RDW and MCHC in patients with inactive Behçet’s disease (r = −0.363, P < 0.001).
Differentiation of patients with Behçet’s disease from controls, and of active disease from inactive disease using RDW, was investigated with ROC analysis. Comparing patients with Behçet’s disease and controls, the area under the ROC curve for RDW was 0.665 ± 0.0362 for a cut-off level of > 4% (sensitivity 56.5%; specificity 66.7%; P < 0.0001). Comparing patients with active Behçet’s disease and those with inactive disease, the area under the ROC curve for RDW was 0.784 ± 0.0336 for the cut-off level of > 14.9% (sensitivity 72%; specificity 78.2%; P < 0.0001). Thus, RDW was more significant when differentiating active disease from inactive disease than in differentiating patients with Behçet’s disease from controls.
Multivariate logistic regression analysis of patients with Behçet’s disease versus controls, and patients with active versus inactive Behçet’s disease.

RDW, red blood cell distribution width; hsCRP, high-sensitivity C-reactive protein; MCV, mean corpuscular volume; ESR, erythrocyte sedimentation rate; MCHC, mean corpuscular haemoglobin concentration; NS, not statistically significant (P ≥ 0.05).
Discussion
The present study demonstrated that RDW, ESR and hsCRP were increased in patients with Behçet’s disease compared with healthy controls. In addition, significant increases in RDW, ESR and hsCRP were observed in those with active disease compared with those with inactive disease. Those with inactive disease also had significantly higher ESR and hsCRP levels than controls.
There are very few studies evaluating the relationships between these parameters in the literature. In a study by Aktürk et al., 15 ESR, CRP and RDW were significantly higher in patients with active Behçet’s disease than those with inactive Behçet’s disease or controls. Moreover, they found that ESR, CRP and RDW were significantly higher in patients with inactive Behçet’s disease compared with controls. In addition, Vayá et al. 16 reported that RDW and CRP were significantly higher in patients with Behçet’s disease than in controls. The findings of both these studies are consistent with the results of the present study.
Increased RDW values have been reported to be associated with disease activity in a number of inflammatory and autoimmune diseases such as inflammatory bowel disease, rheumatoid arthritis and systemic lupus erythematosus.4–7 In addition, RDW has been shown to be positively correlated with inflammatory indices such as CRP and ESR.17,18
In the present study ESR and hsCRP were significantly higher in those with active disease than in those with inactive disease or controls. However, no correlations were found between RDW, ESR and hsCRP within each group. Vayá et al. 16 also reported no correlation between RDW and several inflammatory parameters in patients with inactive Behçet’s disease, whereas Aktürk et al. 15 found modest positive correlations between ESR, CRP and RDW.
In the present study, increased RDW levels were associated with Behçet’s disease activity, but the mechanism is unclear. Elevated RDW may arise from several mechanisms such as chronic inflammation, iron, vitamin B12 or folate deficiencies and oxidative stress, which may result in ineffective erythropoiesis. Among these mechanisms, oxidative stress and inflammation have been shown to be significant determinants of elevated RDW.7,19,20 It has been suggested that raised levels of the cytokines interleukin 1, interleukin 6 and tumour necrosis factor-α in inflammatory diseases can shorten the lifespan of red blood cells, leading to an increased RDW.21,22An increase in RDW may also be caused by oxidative damage. Several studies have demonstrated an oxidative response in patients with Behçet’s disease; as a result of exposure to oxidative stress, the lifespan of erythrocytes decreases, production of reticulocytes increases and the RDW increases in peripheral blood.23,24
In the present study, significantly higher RDW values were seen in patients with active Behçet’s disease compared with those with inactive disease after multivariate logistic regression analysis for age, sex, CRP, MCV, ESR and MCHC. This difference in RDW was seen even though all the patients with active disease were receiving immunosuppressive and anti-inflammatory drugs, which are known to suppress erythrocyte stem cells. 25 Therefore the main factor affecting the increase in RDW in those with active Behçet’s disease is likely to be severe inflammation and oxidative stress resulting from disease activity.
Haemoglobin, RBC, haematocrit, MCHC, MCH and MCV levels were lower in those with active disease compared to those with inactive disease. Reductions in these parameters may also be associated with anaemia of chronic disease. 26 Anaemia as a chronic disorder has been shown to reflect disease activity in systemic autoimmune diseases, with several inflammatory cytokines being implicated in its pathogenesis. 27
The present study is the first to examine the relationship between RDW and organ involvement in Behçet’s disease. There were no significant differences in RDW, ESR and hsCRP between patients with or without vascular or ocular involvement. In a study on patients with scleroderma, a significantly higher RDW was found in patients with vascular involvement compared with those without major vascular symptoms. 28 In the present study, WBC, neutrophils, RBC, haemoglobin, haematocrit and MCV values were significantly higher in patients with vascular involvement compared with patients without. However, all the patients with vascular involvement were male, which may have influenced these results. A more even sex distribution would allow a more robust analysis of these parameters and vascular involvement.
A limitation of the present study was the inclusion of patients with anaemia. No information was provided relating to levels of serum folic acid, iron or vitamin B12. Deficiency of these vitamins and minerals may result in anaemia, thus affecting RDW levels.
In conclusion, the findings of the present study suggest that RDW may be a novel potential marker in determining the active period of Behçet’s disease. The cause of increased RDW values in Behçet’s disease is unclear. Further studies are required to understand the importance of an increased RDW in Behçet’s disease and to clarify the mechanisms involved.
Footnotes
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not for profit sectors.
