Abstract
Objective
To investigate retinal maturation in premature infants (gestation age <37 weeks). using computer-assisted indirect ophthalmoscope imaging.
Methods
Premature infants at postmenstrual age 33–46 weeks, who underwent fundus examinations using computer-aided indirect ophthalmoscopy, were stratified into seven postmenstrual-age groups. Images of macular morphology, peripheral retinal vascularization and fundus pigmentation were compared.
Results
The study included 268 infants in the following postmenstrual-age groups: 33–34 weeks (n = 19), 35–36 weeks (n = 37), 37–38 weeks (n = 49), 39–40 weeks (n = 55), 41–42 weeks (n = 49), 43–44 weeks (n = 34), and 45–46 weeks (n = 25). The macula matured with increasing postmenstrual age. A mature macula was observed in 92% of infants at 45–46 weeks. Complete vascularization was achieved at 41–42 weeks in the nasal retina and at 43–44 weeks in the temporal retina. The number of retinas with normal pigmentation increased with postmenstrual age (rising to 84% of infants at postmenstrual age 45–46 weeks).
Conclusions
Following premature birth, macular morphology, retinal vascularization and retinal pigmentation continue to develop. This study provides reference images of normal retinal development in premature infants.
Keywords
Introduction
Retinopathy of prematurity (ROP), the abnormal growth of blood vessels on the retina in premature infants, is a major cause of blindness and accounts for 6–18% of blindness in children. 1 Timely screening of premature infants who are at risk of ROP is crucial for disease management, because early treatment can improve visual outcomes.2–4 Screening and treatment of ROP remains challenging, however, as knowledge relating to normal morphological development of the retina in premature infants is scarce, making diagnosis and differential diagnosis of early stage ROP in premature infants difficult. Indirect ophthalmoscopy is the standard screening method for ROP,5–7 however, there are no published studies describing features of normal morphological development of the retina in Chinese premature infants observed through indirect ophthalmoscopy, except for a few observational studies using the RetCam® system (Clarity Medical Systems, Pleasanton, CA, USA).8,9 The RetCam wide-field digital retinal imaging machine, which is used for ROP screening or paediatric fundus examinations, is rarely available in hospitals in developing countries, due to its high cost compared with conventional indirect opthalmoscopes. Thus, it would be advantageous for ophthalmologists in developing countries (such as China) to understand the features of retinal development in Chinese premature infants, as observed using an indirect ophthalmoscope; information on such features could be used for indirect ophthalmoscope training in ROP screening.
The purpose of the present research was to study features of retinal development in Chinese premature infants using computer-assisted indirect ophthalmoscope imaging to record the fundus during examinations. Images taken during ROP screening were retrospectively reviewed, to investigate the retinal features of premature infants, focusing on changes of the macula, peripheral retinal vascularization, and fundus pigmentation at different postmenstrual ages (the time lapsed between the first day of the last menstrual period and birth [gestational age] plus the time lapsed following birth [chronological age]).
Patients and methods
Study population
This retrospective observational study included consecutive premature infants (gestational age <37 weeks), examined at paediatric ophthalmology clinics or during neonatal consultation at the Guangzhou Women and Children’s Medical Centre, Guangzhou, China, between September 2006 and July 2007. Patients with ROP and patients with retinal tumour(s) were excluded from the study.
An experienced neonatologist determined the postmenstrual ages, based on the mother’s menstrual history, obstetric data, and physical examination of the neonate. Infants were grouped according to postmenstrual age as follows: 33–34 weeks; 35–36 weeks; 37–38 weeks; 39–40 weeks; 41–42 weeks; 43–44 weeks; 45–46 weeks.
The study was approved by the Ethics Committee of Guangzhou Women and Children’s Medical Centre. Written informed consent is a prerequisite for ROP screening at Guangzhou Women and Children’s Medical Centre, and as such, all parents had provided written informed consent for screening prior to the study.
Ophthalmologic examinations
Infants’ pupils were dilated with mydriatic eye drops (0.5% cyclopentolate and 0.5% phenylephrine) applied 1 h prior to retinal examinations. Local anaesthetic eye drops (0.4% oxybuprocaine) were applied 5 min prior to examinations. The same ophthalmologist (T.L.) performed all fundus examinations using a HEINE SIGMA® 150 computer-assisted indirect ophthalmoscope (The GLOBAL VISION Company, Guangzhou, China); examinations were video recorded for analysis. ROP was diagnosed in accordance with criteria defined by the Committee for the Classification of Retinopathy of Prematurity. 10 Fundus examinations were first performed at postmenstrual age ≥32 weeks and examinations were performed every 2–3 weeks until postmenstrual age 46 weeks. The examination result from the first time each infant attended the paediatric ophthalmology clinic or neonatal consultation at the Guangzhou Women and Children’s Medical Centre, was included in analyses: this may have been the infant’s first examination or first follow-up examination.
Assessment of retinal features
The main retinal features observed were the macular halo, macular central fovea, peripheral vascularization of the retina and fundus pigmentation. Incidence of macular morphology (macular halo and central fovea) at different stages of maturation were recorded and calculated as a percentage of the total studied in each group. Incidence of mature macular morphology and macular central fovea (clear macular halo and dark-red spot with a concave pit in the central fovea) were compared between the different postmenstrual age groups.
For peripheral retinal vascularization, the presence of peripheral vessel stripes close to the ora seratta was regarded as complete vascularization in the nasal or temporal retinas. Incidences of vascularization in the nasal or temporal retina were evaluated based on the number of infants with complete retinal vascularization in each group as a percentage of the total studied in each group. Fundus pigmentation was evaluated, based on the number and distribution of retinal and choroidal pigment granules, and results were categorized into one of three types based on fundus colour: retinal type (normal pigmentation, retinas appear taupe-coloured with intensively and uniformly distributed retinal and choroidal pigment granules in the periphery, so that the vessels of choroid below cannot be seen); choroidal type (hypopigmentation, appears similar to Albinism fundus and retinas appear orange-red with fewer retinal and choroidal pigment granulates, compared with the retinal type); scleral type (hyperpigmentation, retinas appear dark brown characterized by more retinal and choroidal pigment granulates compared with the retinal type). 11 Results were only categorized if they clearly met the criteria for one of the three groups; other findings were uncategorized.
Statistical analyses
Data were presented as mean ± SE or percentage incidence. Analyses were performed using SPSS® software, version 13.0 (SPSS Inc., Chicago, IL, USA) for Windows®. Differences between sets of data were compared using χ2-test. Probability values (P) < 0.05 were considered statistically significant.
Results
Of 295 consecutively enrolled premature Chinese infants initially included, 27 were subsequently excluded from analyses: 14 infants with ROP who received surgical treatment; 10 infants with ROP and subsided lesions; two infants with ROP and congenital retinoschisis; one infant with a retinal tumour. A total of 268 premature Chinese infants (178 male, 90 female) were analysed, with a mean birth weight of 1.86 ± 0.43 kg (range, 0.90–3.00 kg), and mean gestational age of 31.99 ± 2.19 weeks (range, 29–36 weeks). Not all of the 268 infants were available for follow-up at every scheduled examination, therefore only one examination result was included per infant, as described in the methods. The number of infants analysed in the postmenstrual age groups were as follows: 33–34 weeks (n = 19); 35–36 weeks (n = 37); 37–38 weeks (n = 49); 39–40 weeks (n = 55); 41–42 weeks (n = 49); 43–44 weeks (n = 34); 45–46 weeks (n = 25). There were no statistically significant between-group differences in terms of gestational age and birth weight.
Retinal morphology observations
Morphological features of retinal development in premature infants at various postmenstrual ages, observed by computer-assisted indirect ophthalmoscope imaging, are shown in Figure 1. Compared with infants of a younger postmenstrual age (with ambiguous macular halo and macular hypopigmentation), a macular halo and the macular central fovea could be observed in 95% (99/104) of infants at postmenstrual age 37–40 weeks (Figure 1A and B). In 92% (23/25) of infants at postmenstrual age 45 weeks, the central fovea was dark red with a concave pit (Figure 1C). In the nasal retina, the primary branches of nasal arteriovenous vessels were obvious in 41% (43/105) infants at postmenstrual age 33–38 weeks, and the peripheral retina exhibited a typical light grey appearance (Figure 1D). In 87.3% (48/55) of infants at postmenstrual age 39–40 weeks, the secondary branches of retinal vessel stripes were clearly observed and peripheral vessels reached the ora seratta (Figure 1E), exhibiting a typical red appearance, which indicated complete nasal retinal vascularization. At postmenstrual age 39–40 weeks, the branches of temporal retinal arteriovenous vessels were observed in the temporal retina, vessel stripes were also clearly seen, and the typical light-red appearance reached its temporal retina II region. In 83.7% (41/49) of infants at postmenstrual age 41–42 weeks, the temporal retinal vessels reached the ora seratta, and the typical light-red appearance reached the III region (Figure 1F).
Representative morphological features of retinal development in premature Chinese infants observed by computer-assisted indirect ophthalmoscope imaging. (A) Temporal retina of premature infant, postmenstrual age 35 weeks: macular halo was ambiguous (black arrows) with macular hypopigmentation and visible choroid blood vessel stripes (red arrow). (B) Left temporal retina of premature infant, postmenstrual age 39 weeks showing macular halo (black arrows). (C) Right temporal retina of premature infant, postmenstrual age 45 weeks showing macular halo (black arrows) and dark-red central fovea (red arrow): central fovea exhibited a concave pit without macular foveal reflex. (D) Left nasal retina of premature infant, postmenstrual age 37 weeks: secondary branches of retinal vessels were not observed, and the peripheral retina exhibited a light-grey appearance (black arrows). (E) Right nasal retina of premature infant, postmenstrual age 39 weeks: nasal retina vessel stripes were observed and peripheral vessels were close to ora serrata. (F) Right temporal retina of premature infant, postmenstrual age 42 weeks. (G) Retina of premature infant, postmenstrual age 33 weeks: retina was orange-red with visible underlying choroidal vessels (black arrows). (H) Posterior pole of the retina of premature infant, postmenstrual age 37 weeks: the amount of peripheral retinal pigment granules was less in the posterior pole of the retina than in peripheral retina; underlying choroidal vessels were visible in the posterior pole. (I) Posterior pole of the retina of a premature infant, postmenstrual age 40 weeks: the whole retina was dark brown, and the macula was not visible (white arrows). The colour version of this figure is available at: http://imr.sagepub.com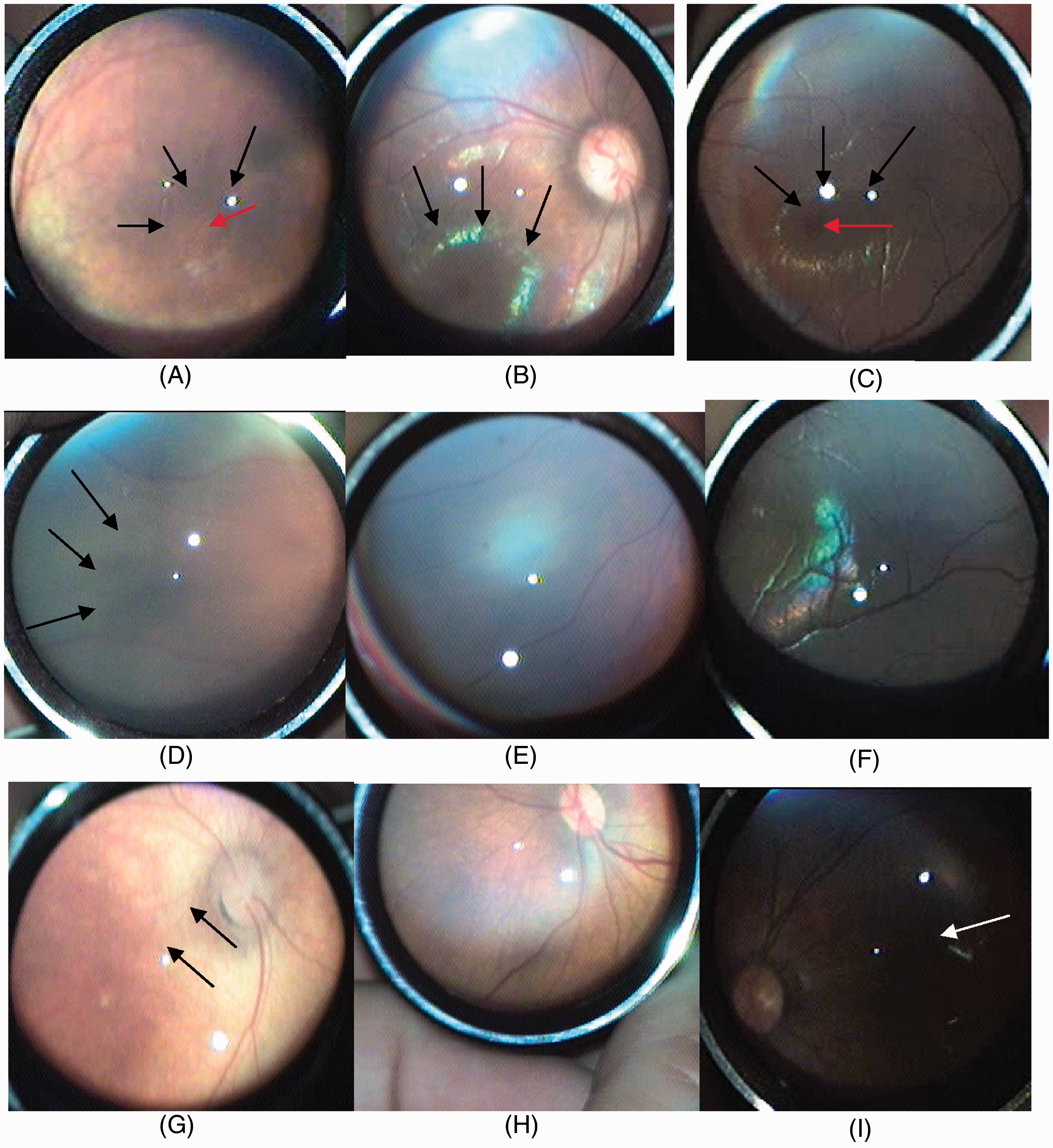
There were fewer retinal and choroidal pigment granules, and the retina appeared orange-red (similar to the albinism retina [choroidal type]), in all infants at postmenstrual age 33–34 weeks (Figure 1G). With increasing postmenstrual age, the retinal pigment granules increased and extended from the peripheral retina to the posterior pole, and the underlying choroidal vessels in the fundus were not visible. In 59.3% (51/86) of infants at postmenstrual age 35–38 weeks, only a few choroidal vessels underlying the posterior pole retina were observed (Figure 1H). A dark-brown fundus with no visible choroidal vessels (the scleral type) was observed in 8.6% (23/268) of infants at postmenstrual age 33–46 weeks, which was different from the fundus of the choroidal type or the retinal type (Figure 1I).
Analysis of retinal morphology development
Differences in the number of premature Chinese infants (gestation <37 weeks) with macular morphological changes, retinal vascularization, and normally pigmented retinas at different postmenstrual ages.

Data presented as n (%) infant incidence.
Between 41–42, 43–44, 45–46 weeks’ postmenstrual age; b41–42 versus 45–46 weeks’ postmenstrual age; cbetween 37–38, 39–40 and 41–42 weeks’ postmenstrual age; d37–38 versus 39–40 weeks’ postmenstrual age; e39–40 versus 41–42 weeks’ postmenstrual age; f41–42 versus 43–44 weeks’ postmenstrual age (all χ2-test).
NS, no statistically significant differences at P > 0.05 (χ2-test) between 39–40, 41–42, 43–44, 45–46 weeks’ postmenstrual age; or 39–40 versus 41–42 weeks, 41–42 versus 43–44, 43–44 versus 45–46 and 39–40 versus 43–44 weeks’ postmenstrual age.
Complete vascularization in the nasal retina was observed in 59.2% (29/49) of infants at postmenstrual age 37–38 weeks. The percentage of complete vascularization in the nasal retina increased with age, and reached 98% (48/49) at postmenstrual age 41 weeks. The percentages of complete vascularization were 59.2% (29/49), 87.3% (48/55), and 98% (48/49) for infants at postmenstrual ages 37–38, 39–40, and 41–42 weeks, respectively. There were statistically significant differences in the percentages of infants with complete vascularization between the three postmenstrual age groups (P < 0.05; Table 1).
Complete vascularization in the temporal retina III region was observed in 83.7% (41/49) of infants at postmenstrual age 41–42 weeks. The percentage of infants with complete vascularization in the temporal retina increased with age, and reached 98% (33/34) at postmenstrual age 43–44 weeks. A statistically significant difference was observed in the percentage of infants with complete vascularization between 41–42 weeks and 43–44 weeks (P = 0.013).
Retinas with a hypopigmentation-type appearance (the choroidal type) were observed in 100% (19/19) of infants at postmenstrual age 33–34 weeks. With increasing postmenstrual age, retinal and choroidal pigment granules increased, and pigment granules tended to form from the peripheral retina to the posterior pole. The percentage of this type of retina decreased with increasing postmenstrual age, and the normal pigmentation-type retinas (retinal type) were found in infants older than postmenstrual age 35–36 weeks. The percentages of normal pigmentation-like retinas were 74.5% (41/55), 81.6% (40/49), 82.4% (28/34), and 84% (21/25) for infants at postmenstrual age 39–40, 41–42, 43–44, and 45–46 weeks, respectively. There were no statistically significant differences in the percentages of infants with normally pigmented retinas between these postmenstrual age groups (P > 0.05; Table 1). The scleral type was observed in 8.6% (23/268) infants at PMA 33–46 weeks.
Discussion
The macula of the retina is immature at birth and develops until the Chievitz fibre layer completely disappears at 4 months following birth. 12 In the present study, macular morphology could not be clearly observed before postmenstrual age 33 weeks, but became more obvious with increasing postmenstrual age. After postmenstrual age 37 weeks, >95% of the infants had a macular halo. After postmenstrual age 43 weeks, >85.3% of infants’ central foveae were dark red in colour. Development of the human foveal depression is thought to involve the formation of a small foveal avascular zone, by late gestation, that actively enlarges as the pit remodels in the postnatal period. 13 The morphological change at this time is likely due to a shift of cells in the kernel layer and ganglion in the central fovea towards the periphery, leading to thinning of the macular centre and thickening of the periphery. 14 Because the macular centre is thin, the underlying dense distribution of pigment epithelial cells and choroidal blood capillaries can be observed by ophthalmoscopy, making the central fovea appear dark red in colour. 15 A study of 129 preterm infants showed that the macula was mature at ∼42 weeks postmenstrual age, 16 which is generally consistent with the findings of the present study regarding macular morphological changes.
Morphological changes in retinal vascularization, in Chinese infants born prematurely, were also investigated in the present study. Normal retinal vascularization starts from the posterior pole of the retina and proceeds to the periphery. 17 In full-term infants, vascularization can reach the ora serrata in the nasal retina at 36 weeks postmenstrual age, and complete vascularization occurs in the temporal retina at 40 weeks postmenstrual age. 18 In the present study, nasal retinal vascularization was completed in 87.3% of premature infants at postmenstrual age 39–40 weeks, and temporal vascularization was completed in 83.7% of infants after postmenstrual age 41 weeks. The results of the present study suggest that complete retinal vascularization in premature Chinese infants is delayed by 3–4 weeks, relative to full-term infants, 18 although this study did not compare premature and full-term infants directly.
During fetal development, the range and proliferation of retinal pigment epithelial cells gradually increases from the periphery to the posterior pole, 19 and the development of retinal pigment epithelial cells in different parts of the retina is not synchronized. 20 Investigation of changes in fundus pigmentation in premature Chinese infants in the present study, revealed that 100% of infants possessed a fundus of the choroidal type (hypopigmentation) at postmenstrual age 33–34 weeks. With increasing postmenstrual age, retinal and choroidal pigment granules increased, and pigment granules tended to form from the peripheral retina to the posterior pole. At postmenstrual age 39 weeks, 74.5% of infants’ fundus were of the retinal type (normal pigmentation), and there were no significant differences in the percentages of infants with normally pigmented retinas between the postmenstrual age groups from 39–40 weeks, suggesting that normal pigmentation did not significantly change after this age. In addition, the scleral type fundus was observed in 8.6% of all infants. The RetCam system may have advantages over computer-assisted indirect ophthalmoscope imaging in the study of peripheral retinal vascularization in premature infants, with superior optical coherence tomography to detect early fine alterations in these patients, however, the purchase costs of such systems are relatively high.
Further research is required, to investigate and compare visual development problems in premature versus full-term infants.
In conclusion, the present study characterized changes in retinal morphology in premature Chinese infants at different postmenstrual ages, and provided image data relating to retinal development. These data may be helpful in the clinical study of retinal development and diagnosis and differential diagnosis of retinal diseases, such as early stage ROP in premature Chinese infants.
Footnotes
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This study was supported by the Science and Technology Project in Guangzhou, China (2012Y2-00017).
