Abstract
Objective:
To investigate the clinical and prognostic significance of protocadherin-10 (PCDH10) promoter methylation in serum-derived DNA from patients with bladder cancer.
Methods:
PCDH10 promoter methylation status was determined using methylation-specific polymerase chain reaction of DNA extracted from serum of patients with bladder cancer, and age- and sex-matched controls. Clinical and pathological details of bladder cancer were recorded.
Results:
PCDH10 promoter methylation was detected in 59/117 (50.4%) of patients with bladder cancer, and none of 37 (0%) controls. Methylation was significantly associated with advanced stage (T2 - T4), high grade (G3), tumour recurrence and larger tumour size (> 3 cm). In addition, methylation was associated with significantly worse survival and was an independent predictor of overall survival.
Conclusion:
Serum-based analysis of PCDH10 promoter methylation may represent a useful noninvasive biomarker of malignant behaviour and outcome in bladder cancer.
Introduction
Bladder cancer is one of the most common malignant genitourinary tumours worldwide and is associated with high morbidity and mortality. 1 Histologically, > 90% of bladder cancers are transitional cell carcinomas, about 70% of which present as nonmuscle-invasive tumours (stages Ta, Tis or T1). 2 Of these tumours, 50 – 70% will recur and 10 – 20% will progress to muscle-invasive disease (stages T2, T3 or T4). 2 Bladder cancer mortality increases with tumour invasiveness, with the 5-year overall survival rate decreasing from 90% for nonmuscle-invasive disease to 60% for T2, 35% for T3 and 25% for T4 disease stages.3 – 5 Progression is difficult to predict, as tumours with similar morphologies behave differently.6,7 New molecular biomarkers are therefore required for the accurate recognition and treatment of high-risk patients.
Protocadherin-10 (PCDH10) acts as a tumour suppressor in several human cancer types8 – 12 and is involved in inhibition of cell proliferation, induction of apoptosis and suppression of tumour invasion.13 – 15 The DNA methylation of gene promoter sequences has been shown to be associated with the silencing of tumour suppressor genes in carcinogenesis. 16 Methylation of the PCDH10 promoter has been demonstrated in a variety of human cancers and is associated with malignant behaviour.8 – 15 Promoter DNA methylation can be used as a diagnostic, prognostic or surveillance biomarker, in particular where methylation silences tumour suppressor genes.16 – 18 DNA isolated from serum has a similar methylation status to DNA in tumour tissues, and may therefore be useful as a noninvasive biomarker in patients with malignant disease.19 – 22
The present study used methylation-specific polymerase chain reaction (PCR) to explore the methylation status of PCDH10 in serum-derived DNA from patients with bladder cancer, and healthy age- and sex-matched controls. The clinical significance of methylation status was determined by correlation with demographic, clinical and pathological features, and disease outcome.
Patients and methods
Study Population
Consecutive patients with primary bladder transitional cell carcinoma who attended the Department of Urology, Third Hospital of Hebei Medical University, Shijiazhuang, China, between March 2004 and March 2007, were recruited to the study. Tumour diagnosis, staging, treatment and follow-up were completed according to international standards. 23 Inclusion criteria were: histopathological diagnosis of transitional cell carcinoma of the bladder; no anticancer therapy before blood sampling; no other prior tumour; availability of follow-up data. An age- and sex- matched control group was recruited from patients with bladder calculi and no prior tumours, who were admitted to the same hospital.
The study was conducted in accordance with the Declaration of Helsinki 24 and approved by the Ethics Committee of the Third Hospital of Hebei Medical University. All participants provided written informed consent for inclusion in the study.
Study Definitions
Overall survival was defined as the time from the date of diagnosis to the date of death from any cause, or last contact if the patient was still alive. Recurrence was defined as any evidence of tumour in a retained bladder ≥ 3 months after treatment.
Methylation-Specific PCR
Peripheral blood (10 ml) was collected into plain sterile tubes from all study participants, before any surgery or treatment. Serum was isolated and stored at –80 °C until use. DNA was extracted from 500 μl of serum (QIAmp DNA Blood mini kit; Qiagen, Valencia, CA, USA) then treated with bisulphite, to convert any unmethylated (but not methylated) cytosine residues to uracil (EpiTect® Bisulfite Kit; Qiagen). Methylation-specific PCR was performed using primers for methylated and unmethylated PCDH10 as previously reported,25 – 27 using a GeneAmp® DNA Amplification Kit with AmpliTaq® Gold (PE Applied Biosystems, Foster City, CA, USA). Primer sequences were: methylated, forward 5′-TCGTTAAATAGATACGTTACGC-3′ and reverse 5′-TAAAAACTAAAAACTTTCCGCG-3′; unmethylated, forward 5′-GTTGTTAAA TAGATATGTTATGT-3′ and reverse 5′-CTAAA AACTAAAAACTTTCCACA-3′. The cycling programme involved preliminary denaturation at 95 °C for 15 min, followed by 40 cycles of denaturation at 94 °C for 30 s, annealing at 54 °C for 30 s, and elongation at 72 °C for 30 s, followed by a final elongation step at 72°C for 10 min. PCR products were separated via 2% agarose gel electrophoresis, stained with ethidium bromide and visualized under ultraviolet illumination. Samples were scored as methylation positive if bands were present in the methylated DNA lane and methylation negative when bands were present only in the unmethylated DNA lane. PCR was performed a minimum of three times per sample.
Statistical Analyses
Between-group differences in PCDH10 methylation status were compared using Fisher's exact test, and the χ2-test was used to assess the relationship between PCDH10 methylation and clinicopathological features. Kaplan–Meier survival analysis and the log rank test were used to assess differences in overall survival between methylated and unmethylated PCDH10 groups. Multivariate Cox proportional hazard analysis, controlled for tumour stage, grade, size and recurrence, was used to estimate the independent prognostic effect of PCDH10 methylation. Statistical analyses were performed using SAS® statistical software, version 8.0 (SAS Institute, Cary, NC, USA) for Windows®. A P-value < 0.05 was considered to be statistically significant.
Results
The study included 117 patients with bladder cancer (79 males/38 females; mean age 69.0 ± 5.9 years; age range 27 – 88 years) and 37 age- and sex-matched controls (25 males/12 females; mean age 68.0 ± 6.5 years; age range 25 – 87 years). There were no statistically significant between-group differences in demographic data. Representative methylation-specific PCR findings are shown in Fig. 1. PCDH10 promoter methylation was detected in 59/117 (50.4%) of patients and none of 37 (0%) controls (P < 0.0001).
Representative methylation-specific polymerase chain reaction results for protocadherin-10 (PCDH10) promoter methylation in serum-derived DNA of five patients with bladder cancer. M, methylated; U, unmethylated; bp, base pairs. Cases 72, 73 and 75 exhibited PCDH10 promoter methylation
Table 1 shows the correlations between PCDH10 promoter methylation and demographic, clinical and pathological features. Methylation was significantly associated with advanced stage (T2 – T4 vs Ta – T1; P = 0.0009), high grade (G3 vs G1/G2; P = 0.0212), tumour recurrence (P = 0.0070) and larger tumour size (> 3 cm diameter; P = 0.0106). There was no correlation between methylation and patient age, sex, tumour morphology or tumour number.
Correlations between protocadherin-10 (PCDH10) promoter methylation in serum-derived DNA, and demographic, clinical and pathological characteristics in patients with bladder cancer (n = 117)
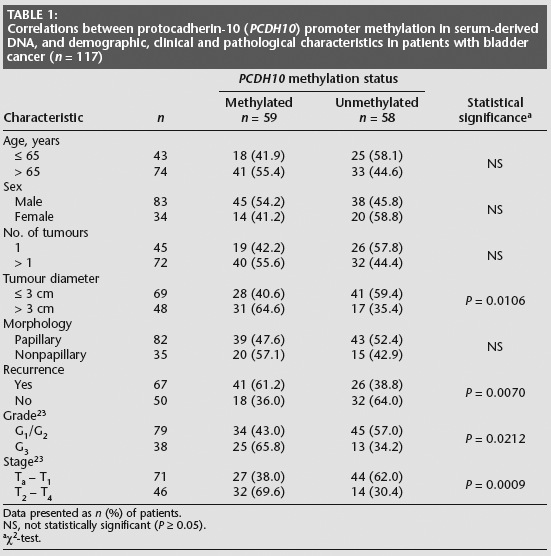
Data presented as n (%) of patients.
NS, not statistically significant (P ≥ 0.05).
χ2-test.
Overall survival was assessed in patients with bladder cancer. Patients with PCDH10 promoter methylation had significantly shorter survival times than those without methylation (P < 0.0001, Fig. 2). Multivariate regression analysis revealed that PCDH10 promoter methylation (hazard ratio [HR] 3.719; 95% confidence intervals [CI] 1.328, 10.426; Table 2), late stage (HR 3.593; 95% CI 1.438, 9.032) and high grade (HR 2.931; 95% CI 1.011, 8.567) were independent predictors of overall survival in bladder cancer.
Kaplan–Meier survival curves for patients with bladder cancer (n = 117), stratified according to protocadherin-10 (PCDH10) promoter methylation status assessed in serum-derived DNA. P < 0.0001; log rank test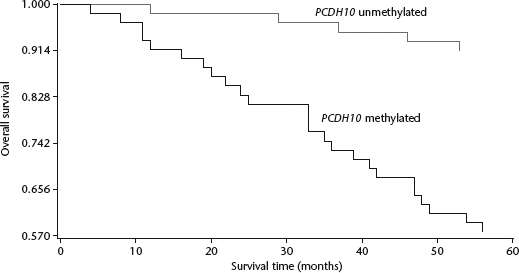
Multivariate Cox proportional hazard analysis of prognostic factors in patients with bladder cancer (n = 117)

PCDH10, protocadherin-10.
Discussion
The systematic evaluation of PCDH10 promoter methylation status in the current study revealed methylation in 50.4% of patients with bladder cancer, compared with a total absence of methylation in the control group. This finding suggests that PCDH10 methylation is cancer specific. Methylation was significantly associated with advanced stage, high grade (poor tumour differentiation) and large tumour size (> 3 cm) in the present study, all of which are known risk factors for progression and poor prognosis in bladder cancer.2,28 Studies in other cancers have found similar associations between PCDH10 promoter methylation and malignant behaviour.9 – 15 The association between PCDH10 methylation and tumour recurrence in the present study suggests that methylation could represent a useful predictor of relapse. The high recurrence rate in bladder cancer is a major factor known to influence prognosis. 29
Methylated DNA recovered from sera from patients with malignant disease is known to reflect DNA alterations in tumour tissue.19– 21,30 PCDH10 promoter methylation has been associated with poor prognosis in patients with gastric cancer, and can be used as an independent prognostic factor. 15 Data from the current study indicated that PCDH10 methylation in DNA extracted from serum correlated with malignant behaviour in bladder cancer. Patients with PCDH10 methylation had significantly shorter survival times than those without methylation. In addition, methylation was an independent predictor of overall survival in the present study.
In conclusion, the present study indicates that PCDH10 promoter methylation occurs frequently in patients with bladder cancer, and significantly correlates with malignant behaviour and poor prognosis. Serum-based analysis of PCDH10 promoter methylation may represent a useful noninvasive biomarker of malignant behaviour and outcome in bladder cancer. Aggressive postsurgical intervention should be performed in patients found to have PCDH10 promoter methylation, in order to achieve a better outcome.
Footnotes
Conflicts of interest: The authors had no conflicts of interest to declare in relation to this article.
