Abstract
OBJECTIVES:
To investigate retro spectively whether alterations of p53 upregulated mediator of apoptosis (PUMA) protein levels and somatic mutations of the PUMA gene are characteristic of pancreatic ductal adenocarcinoma (PDAC).
Methods:
Immunohistochemical analyses of PUMA were performed in pancreatic tumour tissue samples, and paired normal pancreatic tissue samples, from patients with PDAC. Apoptosis was detected using terminal deoxynucleotidyl transferase-mediated deoxyuridine triphosphate nick-end labelling assay.
Results:
A total of 70 patients with PDAC had samples available; 49 cases (70.0%) had high PUMA protein levels. PUMA was not detected in paired normal tissue samples. Significantly higher levels of PUMA protein were detected in low-grade tumours (tumour -node-metastasis stages I and II), compared with higher grade (stage III) tumours. Of the PDAC cases, the mean apoptosis index value for PUMA-positive specimens was significantly higher than that for PUMA-negative specimens. Overall survival was significantly associated with PUMA immunoreactivity.
Conclusions:
High levels of PUMA in PDAC tumour cells suggest that PUMA expression may play a role in pancreatic tumourigenesis.
Introduction
Apoptosis is a process of active cell death that takes place during a number of physiological events, such as cell development and normal cell turnover.1,2 The apoptotic pathway is separated for the most part into intrinsic and extrinsic pathways. 2 The intrinsic pathway is induced by various apoptotic stimuli including growth factor deprivation, hypoxia, radiation and anticancer drugs; it is regulated by B-cell lymphoma (Bcl)-2 family proteins, 2 which are comprised of pro- and antiapoptotic members. Proapoptotic members (such as Bcl-2-associated death promoter [BAD], Bcl-2-interacting domain [BID], Bcl-2 homology domain-3 [BH3]-only protein NOXA, and p53 upregulated mediator of apoptosis [PUMA]), share in common the BH-3 domain, which is an interacting domain that is both necessary and sufficient for the killing action.3 –7
Discovery of the PUMA gene and the mitochondrial protein that it encodes was made in 2001, by two independent groups, during the screening for p53-inducible target genes.7,8 Expression of PUMA causes rapid p53-dependent apoptosis and growth inhibition, induces cytochrome C release, and activates procaspase-3 and procaspase-9, suggesting a prominent role for PUMA in the intrinsic apoptotic pathway.7,8 Establishing PUMA as an important mediator of cell death suggests that it has a role in the pathogenesis of human cancers, through alteration of the PUMA gene or aberrant expression of PUMA. Overexpression of PUMA has been reported in gastric, hepatocellular and colorectal cancer cells,9 – 11 but not in normal tissue. It is possible that increased levels of PUMA protein in malignant tumour tissue may alter the regulation of cell death during tumourigenesis.
Most pancreatic cancers are pancreatic ductal adenocarcinomas (PDAC); the 5-year survival rate for patients with localized disease after surgical resection is 20%, whereas for those with metastatic disease the 5-year survival rate is only 2%. 12 Identification of molecules that may predict poor disease prognosis is important for selecting those patients who could clinically benefit from radical treatment or molecularly targeted therapy. Research on both the mutation status and the expression of the PUMA gene is limited, for PDAC. The present study investigated the relationship between PUMA protein levels and apoptosis, and whether alterations in PUMA protein levels are characteristic of PDAC.
Patients and methods
Study Population
This retrospective study included consecutive patients who had undergone curative resection for primary PDAC at the Department of Surgery, Shandong Provincial-owned Hospital, Jinan, Shandong, China, or the Department of General Surgery, Affiliated Hospital of Medical College Qingdao University, Qingdao, China, between October 1992 and August 2002. None of the patients included in the study had received prior radiotherapy or neoadjuvant therapies. There were no other specific inclusion or exclusion criteria. Surgically resected specimens were retreived from hospital archives and macroscopically examined to determine tumour location and size. Normal pancreatic tissue, taken from a distance of ≥ 1.5 cm away from the tumour, was used as paired control tissue.
The study was approved by the Ethics Committee of Shandong Provincial-owned Hospital and Affiliated Hospital of Medical College Qingdao University. All patients gave written informed consent for their participation.
Sample Preparation
Tissue samples were fixed in 10% formalin, embedded in paraffin wax, cut into 4-μm sections and stained with haematoxylin and eosin. The specimens were then reviewed by one of the authors (J. Z.) to determine histological differentiation and presence of lymph node metastasis. Pathological tumour–node–metastasis (TNM) staging was carried out according to the Guidelines of the International Union Against Cancer (1997). 13 All adenocarcinoma cells were categorized as well, moderately, or poorly differentiated (stages I, II and III, respectively). The postsurgical status of all patients was reviewed on 31 October 2009, to calculate overall survival rates from the date of surgical resection.
Immunohistochemistry
Immunohistochemistry was performed on 4-μm thick, formalin-fixed, paraffin wax-embedded tissue sections. The sections were deparaffinized and hydrated by passing through xylene (three times for 5 min), a graded ethanol series (once each for 5 min in 100%, 80%, 70% and 50% ethanol) and distilled water for 10 min. Endogenous peroxidase activity was blocked using 3% hydrogen peroxide in methanol (30 min) between the first two steps of washing with ethanol. Next, the sections were washed three times for 10 min with 0.5 M Tris-buffered saline (pH 7.6), then immersed in 10 mM citrate buffer (pH 6.0) and heated at 100°C for 30 min in a pressure cooker (Nordic Ware, Minneapolis, MN, USA) for antigen retrieval, before being cooled for 20 min.
After rinsing with 10% phosphate-buffered saline (PBS, pH 7.6), the slides were treated with 1% hydrogen peroxide in 50 mM PBS (pH 7.6) for 15 min at room temperature, to quench endogenous peroxidase activity. After washing with TNT buffer (0.1 mol/l Tris–HCl [pH 7.4], 0.15 mol/l sodium chloride and 0.05% Tween) for 20 min, the slides were treated with TNB buffer (0.1 mol/l Tris–HCl [pH 7.4], 0.15 mol/l sodium chloride and 0.5% hydrogen peroxidase) for 60 min at room temperature (Roche, Basel, Switzerland). Sections were incubated with a polyclonal rabbit antihuman PUMA antibody (1:100 dilution; Cell Signaling Technology®, Danvers, MA, USA) overnight at 4 °C. According to the manufacturer's information, this antibody detects a protein band of approximately 19-kDa molecular size, which may represent a PUMA protein. Sections were then incubated with biotinylated rabbit antimouse secondary antibodies (1:50 dilution; Sigma-Aldrich, St Louis, MO, USA) for 50 min at 37 °C. Signal amplification was carried out using the Renaissance Tyramide Signal Amplification indirect kit (NEN™; Life Science Products, Boston, MA, USA) according to the manufacturer's instructions. Briefly, streptavidin–peroxidase was applied for 30 min at room temperature, followed by biotinylated tyramide treatment for 7 min at room temperature. Each incubation step was followed by three washes for 5 min in TNT buffer. The reaction products were developed with 3′,3′-diaminobenzidine (DAB; Sigma-Aldrich) and counterstained with haematoxylin and eosin. Both positive and negative control specimens were also stained during the immunohistochemical protocol. In negative controls, the use of primary antibodies was omitted. Human colorectal carcinoma tissue samples known to express high levels of PUMA were used as positive controls for the PUMA protein. 11
The percentage of PUMA-positive cells was assessed in five randomly selected fields for each section using an optical light microscope (magnification × 200). Using the median value of 10% as a cut-off, a high level of PUMA protein was defined as cytoplasmic staining of ≥ 10% of the tumour cells, and a low level of PUMA protein was defined as cytoplasmic staining of < 10% of the tumour cells or no cytoplasmic staining. Data were analysed to determine whether there was any correlation between survival and staining for PUMA.
Determination of Apoptosis in Specimens
Apoptosis was evaluated by terminal deoxynucleotidyl transferase (TdT)-mediated deoxyuridine triphosphate nick-end labelling (TUNEL) assay, using the ApopTag® Peroxidase In Situ Detection Kit (Chemicon International, Temecula, CA, USA), according to the manufacturer's instructions. Briefly, the sections were deparaffinized, rehydrated in deionized water, then rinsed with 10 mM PBS (pH 6.0). Sections were treated with 20 μg/ml of proteinase K solution for 15 min at room temperature to digest the tissue protein, and with 3% hydrogen peroxide for 5 min to quench endogenous peroxidase activity. After washing with 50 mM PBS (pH 7.6), the equilibration buffer provided with the kit was added. The slides were then treated with TdT enzyme (12 U/ml) for 60 min at 37 °C, then incubated with preheated stop solution (provided with the kit) for 10 min, followed by antidigoxigenin peroxidase conjugate for 30 min. The signal was detected with metal-enhanced DAB, and the sections were counterstained with haematoxylin and then mounted. Control slides of TUNEL-positive breast cancer tissue were purchased from Serologicals (Norcross, GA, USA). The percentage of TUNEL-positive cells was assessed in five randomly selected fields for each section, using an optical light microscope (magnification × 200).
Statistical Analyses
Statistical analyses were performed using the SPSS® software package, version 11.5 (SPSS Inc., Chicago, IL, USA) for Windows®. Data were reported as mean values ± SD. Comparisons between clinicopathological factors and PUMA levels, and between apoptosis index and PUMA levels, were assessed using the χ2-test. Cumulative survival rates were calculated using Kaplan–Meier analysis and compared using the Cox– Mantel test. Kaplan Meier analysis was used to generate survival curves and differences in survival were analysed using the log-rank test, based on the PUMA protein levels. Univariate and multivariate analyses were carried out using the Cox proportional hazards model. A P-value < 0.05 was considered to be statistically significant.
Results
A total of 70 patients with PDAC had specimens of pancreatic cancer and paired normal pancreatic tissue available. The patients had a median age of 64 years (range 43 – 74 years) and comprised 39 males and 31 females. All cases were diagnosed as adenocarcinomas. Tumours were well differentiated (stage I) in 29 cases, moderately differentiated (stage II) in 24 cases and poorly differentiated (stage III) in 17 cases. Tumour size was 0 – 2 cm in 19 cases, 2 – 5 cm 43 in cases and > 5 cm in eight cases.
Immunostaining revealed that PUMA was localized in the cytoplasm of malignant cells. Of the PDAC tumour tissues, 70% (49/70) had high levels of PUMA protein (Fig. 1A) and 30% (21/70) had low levels (Fig. 1B) or no PUMA protein (Fig. 1C). None of the 70 paired normal pancreatic tissues showed PUMA immunostaining (Fig. 1D). No significant association was found between PUMA immunostaining in tumour tissue and lymph node metastasis, tumour stage or tumour size (data not shown). Significantly more tumours of TNM stages I and II (well and moderately differentiated, respectively) had high PUMA protein levels compared with those of a higher stage (TNM stage III, poorly differentiated) (χ2 = 5.027; P < 0.05).
Representative sections of immunhistochemical staining for p53 upregulated mediator of apoptosis (PUMA) protein in malignant and paired normal pancreatic tissue samples from patients with pancreatic ductal adenocarcinoma. Malignant pancreatic tissue samples showing: (A) high level of PUMA in the cytoplasm; (B) low level of PUMA in the cytoplasm; (C) no PUMA staining. (D) Normal pancreatic tissue sample showing no PUMA staining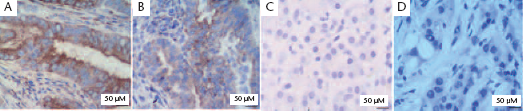
Among the PDAC cases, the mean ± SD apoptosis index value was significantly higher in the 49 cases with high PUMA protein levels than in the 21 cases with low PUMA protein levels 10.46 ± 2.42 versus 7.86 ± 1.84, respectively; P = 0.027).
The overall survival rate for patients with high PUMA protein levels was significantly longer than that for patients with low PUMA protein levels (P = 0.027; Fig. 2).
Effect of p53 upregulated mediator of apoptosis (PUMA) immunoreactivity on overall survival rates in 70 patients with pancreatic ductal adenocarcinoma (Kaplan–Meier curves): survival in cases with high levels of PUMA protein (PUMA-positive; n = 49) was significantly longer than that in cases with low levels of PUMA protein (PUMA-negative; n = 21) (P = 0.027)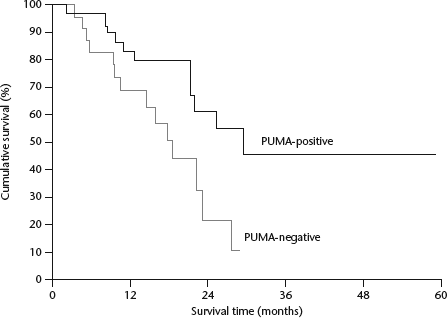
Discussion
Changes in PUMA protein levels were analysed as potential modulatory mechanisms of PUMA-induced apoptosis in patients with PDAC. Higher levels of PUMA protein were detected in pancreatic tumour tissue than in paired normal pancreatic tissue. Additionally, higher levels of PUMA protein were detected in tumours of TNM stages I and II (well and moderately differentiated, respectively) compared with those of TNM stage III (poorly differentiated), suggesting that increased expression of PUMA in PDAC cells may play a role in pancreatic tumourigenesis. These findings are in accordance with previous studies that reported high levels of PUMA protein in tumour tissues.9 – 11 Other studies have reported lower levels of PUMA protein in cutaneous melanoma and sporadic colorectal tumour tissue, compared with benign tumour or normal tissue, and that lower PUMA levels were associated with metastatic tumour tissue.14,15
Enhancement of cell proliferation and promotion of cell survival, via inhibition of apoptosis, is thought to play a key role in the initiation and progression of cancer.16 – 18 Due to the proapoptotic activity of PUMA proteins, a decrease in PUMA expression was expected in PDAC pancreatic tumour tissue compared with normal pancreatic tissue. In contradiction to this, the present study showed high PUMA levels in 70% of PDAC cases.
Cancer cells have been shown to acquire the ability to evade apoptosis during the development and progession of cancer, protecting themselves from various apoptotic stimuli. 2 Cancer cells without this ability could die during development and progression. It could be that PUMA expression in PDAC tissue contributes to the promotion of apoptosis and may produce selective pressure to over-ride apopotosis during carcinogenesis. It is conceivable that such selected PDAC cells might have resistant mechanisms against PUMA-dependent apoptosis. This, however, remains to be determined.
Functional inactivation of p53 is a very common event in many types of human cancer, including PDAC. It is estimated, however, that 50% of all cancers do not have a p53 mutation. 19 Elimination or functional inactivation of other participants in the p53-dependent pathway could also mimic altered or lost p53 function and contribute to malignant progression.19,20 p53 activates the intrinsic mitochondrial apoptotic pathway by upregulating Bcl-2 proapoptotic members, such as PUMA and NOXA. 5,7,8 In contrast, alterations of components in the extrinsic apoptotic pathway have been described in PDAC, including the overexpression of antiapoptotic molecules such as soluble Fas and Fas-associated phosphatase-1. 21 Taken together, these data suggest that apoptotic pathways in PDAC may be inhibited by alterations in the extrinsic apoptotic pathway, rather than alterations in the p53-inducible intrinsic pathway.
A high level of PUMA protein in PDAC cases was associated with a high apoptotic index and improved overall patient survival, in the present study. These findings suggest a relationship between PUMA expression and the malignant transformation of PDAC cells. Thus, the upregulation of PUMA may be a potential marker for PDAC diagnosis and a prognostic indicator for patient survival.
In summary, the present study demonstated an alteration of PUMA protein levels in PDAC malignant tumours. The differences in PUMA protein levels observed between malignant and normal pancreatic tissue samples suggest that regulation of PUMA expression may play a role in PDAC development. PUMA protein levels were associated with tumour stage, apoptotic index and prognosis in patients with PDAC, and may serve as useful diagnostic or therapeutic targets for PDAC.
Footnotes
Conflicts of interest: The authors had no conflicts of interest to declare in relation to this article.
