Abstract
Optic atrophy describes a group of diseases of retinal ganglion cells and axons that eventually lead to loss of vision. Optic atrophy has both congenital and acquired causes, and its diagnosis (or differential diagnosis) is complicated. This case report describes a 20-year-old man who presented with a 1-year history of progressive vision loss in both eyes and no obvious systemic symptoms. Fundus examination revealed bilateral optic atrophy. Based on clinical characteristics, visual field analysis and pattern visual evoked potential examination, the presumptive diagnosis was Leber hereditary optic neuropathy (LHON). Analysis of mitochondrial DNA indicated the absence of all of three common mutations associated with LHON (m.3460G>A, m.11778G>A, m.14484T>C). Detailed questioning of the patient revealed a history of prolonged language development and poor balance. Neurological examination indicated abnormal co-ordination, suggesting the presence of inherited spinocerebellar ataxia (SCA). Analysis of the SCA7 gene revealed a high number of trinucleotide repeats [(CAG)n, n > 64], confirming the diagnosis of SCA. The aetiology of optic atrophies is complicated and the molecular genetic detection approach provides the best information for diagnosing these diseases.
Keywords
Introduction
Optic atrophy describes a group of ocular fundus diseases of retinal ganglion cells and axons with a variety of congenital and acquired causes, characterized by ganglion cell apoptosis, optic nerve degeneration and eventual loss of vision. 1 It is the ultimate outcome of several local or systemic lesions including Leber hereditary optic neuropathy (LHON), 2 optic neuritis, 3 glaucoma, 4 intracranial hypertension, 5 inflammation, 6 tumour, 7 haemorrhage, 8 diabetes,9,10 cerebellar ataxia 11 and trauma. 12 Affected individuals have vision loss or blindness, visual field impairment and changes in visual electrophysiology. Juvenile onset hereditary optic atrophy is painless 13 and may eventually progress to serious disturbance of vision. The aetiology of juvenile optic atrophy is complicated and variable, and early diagnosis and prompt intervention are crucial for preventing visual impairment. 13 The present case report describes a young male patient with optic atrophy whose diagnosis was confirmed by molecular detection of the causative genetic mutation.
Case Report
Approval to report the patient's data was provided by the Ethics Committee of Wuhan General Hospital of Guangzhou Military Command, Wuhan, China, and the patient provided written informed consent.
A 20-year-old man presented with a 1-year history of progressive vision loss. The patient reported no distending pain in the eyes, headache, nausea, vomiting, iridization or scieropia, and had no history of systemic or ocular disease or trauma. He was conscious, spoke fluently and acted freely. Ophthalmological examinations were performed, including best-corrected visual acuity (6/60 for both eyes), eyeball motion (both moved freely), anterior segment observation (no misalignment or nystagmus) and intraocular pressure (15 mmHg in both eyes). Fundus examination revealed a pale optic papilla with an obvious boundary, no retinal haemorrhage or exudation and no macular oedema (Fig. 1). Visual field examination (Humphrey® 750 Visual Field Analyzer; Carl Zeiss Meditec, Oberkochen, Germany) revealed off-centre scotomas in both eyes (Fig. 2). Pattern visual evoked potential (P-VEP) examination (RETI-port; Roland Consult, Brandenburg, Germany) indicated increased P100 latency (right eye 111 ms, left eye 113 ms). The resulting presumptive diagnosis of LHON was further investigated by mitochondrial DNA mutation analyses (Applied Biosystems® 7500 Real-Time PCR system; Life Technologies®, Foster City, CA, USA), but the three most common mutations associated with LHON (m.3460G>A,14,15 m.11778G>A 16 and m.14484T>C 17 ) were absent. Detailed questioning of the patient revealed delayed acquisition of speech (aged 3 years) and poor balance (for example, when riding a bicycle). The patient's father and grandfather also had a history of balance problems. Neurological examination of the patient showed movement co-ordination abnormalities in the finger–nose test, heel– knee tibial test and Romberg test, indicative of spinocerebellar ataxia (SCA). Mutations in several genes are associated with SCA, including the SCA7 gene, which leads to cerebellar ataxia, visual extinction and retinal and optic nerve degeneration. 18 SCA7 gene analysis was performed using an automated pyrosequencer system (PSQTM 96MA; Biotage, Uppsala, Sweden) and revealed the genotype (CAG)10/(CAG)n (n > 64), confirming the diagnosis of SCA.
Photographs showing the fundus (of both eyes) in a 20-year-old man with a 1-year history of progressive bilateral vision loss. The optic papilla was pale with an obvious boundary (arrows). Macular oedema, retinal haemorrhage and exudation were absent Visual field examination in a 20-year-old man with a 1-year history of progressive bilateral vision loss, showing off-centre scotoma in both eyes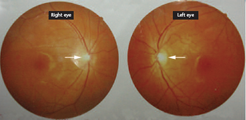

Discussion
Optic atrophy is the ultimate outcome of various retinal and optic neuropathies and systemic diseases. Many systemic or local diseases can induce optic atrophy and it is therefore difficult to establish the cause of a given case and decide on the best treatment. Hereditary optic atrophy is particularly difficult to diagnose, 19 therefore it is crucial to identify the aetiological factors accurately and promptly in order to improve the prognosis. LHON is a maternally inherited disease mainly affecting young men, that causes rapid, painless visual loss simultaneously in both eyes, accompanied by impairment of the central visual field and colour vision. 2 The clinical features of the present case were similar to those of LHON, and this was therefore the initial diagnosis. LHON is associated with many mitochondrial (mt)DNA mutations,20,21 but is caused by one of three primary mutations in 90 – 97% of patients. 22 These include a G>A substitution at position 11 778 (m.11778G>A),16 a G>A substitution at position 3460 (m.3460G>A)14,15 and a T>C substitution at position 14 484 (m.14484T>C).17 The current patient was found to be free from all three of these mutations and was therefore considered unlikely to have LHON.
A detailed family history and neurological examination of the patient suggested the presence of an inherited SCA. These diseases are characterized by a wide range of clinical manifestations including cerebellar ataxia, progressive external ophthalmoplegia and dystonia with rigidity, optic atrophy, retinitis pigmentosa, pyramidal and extrapyramidal signs, and distal muscular atrophies. 23 SCAs can manifest at a relatively young age 24 and are inherited in an autosomal-dominant manner. 25 Several genes and genotypes have been associated with SCAs, 11 including SCA7. Mutation in SCA7 leads to cerebellar ataxia and obvious ocular lesions, including visual extinction and degeneration of the retina and optic nerve. 18 SCAs result from trinucleotide repeat (CAG) expansions in the causative gene, 26 from 7 – 17 repeats in unaffected individuals to 38 – 138 repeats in patients with SCA. 27 This leads to the expansion of a polyglutamine tract in the corresponding disease protein, with the resulting toxicity being important in pathogenesis. 28 The SCA7 gene in the present patient was found to have 64 CAG repeats, confirming the diagnosis of SCA. In China, SCA is most commonly associated with SCA7 mutation. 18 A diagnosis of SCA should be considered when changes in the retina and optic nerve are observed in the fundus, and care should be taken to exclude other ocular or systemic diseases (such as LHON, age-related macular degeneration, diabetic retinopathy or multiple sclerosis). The molecular genetic approach can provide the best evidence for the diagnosis of these hereditary diseases.
Footnotes
Acknowledgement
Dr Zhongshan Chen was supported by a grant from the Nature Science Foundation of China (no. 30900446).
The authors had no conflicts of interest to declare in relation to this article.
