Abstract
Objective:
This study investigated levels of interleukin (IL)-34, a proinflammatory cytokine, in patients with coronary artery disease (CAD).
Methods:
Following coronary artery angiography, 91 patients with CAD (including stable and unstable angina pectoris) were divided into two groups, the CAD group (coronary artery stenosis ≥ 50%) and the control group (coronary artery stenosis < 50%). Serum levels of factors including IL-34 and high sensitivity C-reactive protein (hs-CRP) were measured.
Results:
IL-34 and hs- CRP levels were significantly higher in the CAD group than in the control group (191.3 ± 17.9 pg/ml versus 125.4 ± 14.8 pg/ml and 3.08 ± 1.81 mg/ml versus 1.42 ± 1.01 mg/ml, respectively), with a significantly positive correlation between IL-34 and hs-CRP levels in the CAD group. Multiple regression analysis showed that IL-34 and hs-CRP levels were independent predictors of CAD (IL-34: odds ratio [OR] 2.073, 95% confidence intervals (CI) 1.419, 2.672; hs-CRP: OR 1.878, 95% CI 1.172, 2.531).
Conclusions:
IL-34 levels were significantly increased in patients with CAD, and positively correlated with hs- CRP levels, suggesting that IL-34 may be an independent predictor of CAD.
Introduction
Atherosclerosis is characterized by a complex multifactorial pathophysiology. Although formerly considered to be a disease caused by lipid accumulation, it is now known to involve ongoing inflammatory responses, which play pivotal roles in the pathogenesis of atherosclerotic coronary artery disease (CAD). Vascular inflammation is a predominant factor in the initiation, progression and final steps of atherosclerosis.1,2 Several proinflammatory cytokines (including tumour necrosis factor [TNF]-α, interleukin [IL]-6, IL-18, high mobility group box 1 [HMGB1] protein and high sensitivity C-reactive protein [hs-CRP]) have been shown to be predictors of atherosclerotic CAD,3–7 suggesting that proinflammatory cytokines may play important roles in the pathogenesis of this disease.
Interleukin-34 was first found to stimulate monocyte viability in 2008, where it functioned like macrophage colony-stimulating factor (M–CSF), stimulating the release of proinflammatory cytokines. 8 Increased levels of IL-34 were discovered in bone tissue giant-cell tumours where it was shown to play a key role in receptor activator of nuclear factor κB ligand-induced osteoclastogenesis. 9 Results from these investigations suggested that IL-34 a necessary and sufficient mediator of inflammation and functions as a novel proinflammatory cytokine. The present study investigated whether there were changes in serum IL-34 levels in patients with CAD.
Patients and methods
Study Population
This study included consecutive patients with suspected CAD or CAD, attending the Central Hospital of Huangshi, Huangshi, China between 1 Feb 2011 and 31 Dec 2011. Coronary artery angiography was performed in all patients. Patients with suspected CAD or CAD included those who had stable angina pectoris or unstable angina pectoris, except for patients with variant pectoris and myocardial infarction.
Unstable angina was diagnosed in accordance with the 2007 Chinese Society of Cardiology guidelines, 10 which are in line with recommendations of the American Heart Association, as: (i) resting angina, angina occurring at rest and prolonged, usually > 20 min; (ii) new-onset angina, angina that had occurred < 1 month previously, spontaneously or with exertion and was of at least class III severity; (iii) increasing angina, previously diagnosed angina that had become distinctly more intense, more frequent, longer in duration or lower in threshold (i.e. increased by one or more class to at least class III severity). In addition, unstable angina was in accordance with a diagnosis of acute coronary syndrome excluding myocardial infarction (i.e. myocardium enzymes greater than threefold above the upper limit of normal). Stable angina was defined as angina typically aggravated by exertion or emotional stress and relieved by nitroglycerin, usually prolonged for > 3 months, with ischaemic ST-T wave changes ( 1 mm of ST-segment depression). Variant angina was classed as angina that usually occurs and relieves spontaneously with transient ST-segment elevation. According to a previous study, 11 patients with coronary artery stenosis of severity < 50% served as the control group (except those with unstable angina pectoris patients). Exclusion criteria included patients aged < 20 or > 75 y, or those with a history of any of the following conditions: myocardial infarction; cardiac dysfunction; peripheral vascular disease; fever; liver or renal dysfunction; autoimmune disease; cancer.
The clinical protocol was approved by the Medical Ethics Committee of the Central Hospital of Huangshi and the study was conducted according to the guidelines outlined in the Declaration of Helsinki. All participants provided written or verbal informed consent.
Sample Collection and Biochemical Investigation
For patients presenting with unstable angina pectoris, blood samples were taken > 24 h after symptom onset. For all patients, 2 ml venous blood samples for biochemical analysis of basal serum components were obtained between 07.00 h and 08.00 h after an overnight fast. Serum samples were prepared by allowing the sample to stand for ∼1h at 4 °C, before the serum was harvested. Samples were then aliquoted and stored at –70 °C for ∼ 1 month until use. All samples were thawed only once. Serum total cholesterol, triglycerides, high-density lipoprotein cholesterol (HDL-C), low-density lipoprotein-cholesterol (LDL-C) and hs-CRP levels were measured using standard laboratory techniques on a Hitachi 912 Chemistry Analyzer (Roche Diagnostics, Mannheim, Germany). Serum IL-34 levels were determined with a commercially available enzyme-linked immunosorbent assay kit (USCN Life Science, Wuhan, China), according to the protocol supplied.
Statistical Analyses
Statistical analyses were performed using the SPSS® software package, version 13.0 (SPSS Inc., Chicago, IL, USA) for Windows®. All values were expressed as mean ± SD or numbers and percentages. χ2-test or Fisher's exact test were used to compare categorical variables; Student's
Results
A total of 91 patients, age range 40 – 72 years, were enrolled into the study: 51 into the CAD group and 40 into the control group. Patient characteristics and basal serum biochemistry data are shown in Table 1. There were no significant between-group differences in terms of age, gender, body mass index (BMI), lipid levels (total cholesterol, triglycerides, HDL-C and LDL-C) and medication. IL-34 and hs-CRP levels were significantly higher in the CAD group compared with the control group (
Characteristics and baseline serum biochemistry profiles of patients with coronary artery disease (CAD), with coronary artery stenosis < 50% (control group) or coronary artery stenosis 50% (CAD group)
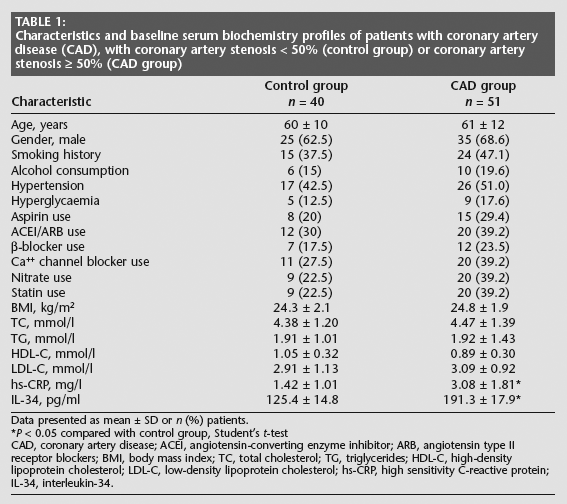
Data presented as mean ± SD or
CAD, coronary artery disease; ACEI, angiotensin-converting enzyme inhibitor; ARB, angiotensin type II receptor blockers; BMI, body mass index; TC, total cholesterol; TG, triglycerides; HDL-C, high-density lipoprotein cholesterol; LDL-C, low-density lipoprotein cholesterol; hs-CRP, high sensitivity C-reactive protein; IL-34, interleukin-34.
Correlations between IL-34 levels and several cardiovascular disease risk factors in CAD patients are shown in Table 2. There was a significant positive correlation between hs-CRP and IL-34 levels (
Pearson's correlation coefficient values for interleukin-34 levels compared with cardiovascular risk factors, in patients with coronary artery stenosis 50% (
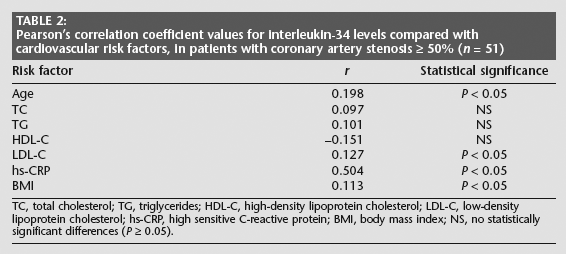
TC, total cholesterol; TG, triglycerides; HDL-C, high-density lipoprotein cholesterol; LDL-C, low-density lipoprotein cholesterol; hs-CRP, high sensitive C-reactive protein; BMI, body mass index; NS, no statistically significant differences (
Both the IL-34 and hs-CRP levels were independent predictors for CAD (IL-34: odds ratio [OR] 2.073, 95% confidence intervals [CI] 1.419, 2.672; hs-CRP: OR 1.878, 95% CI 1.172, 2.531).
Discussion
Inflammation plays a critical role in the pathogenesis of atherosclerotic CAD and various studies have demonstrated that many proinflammatory cytokines are predictors of this disease.3–7 In addition to M–CSF, IL-34 has been shown to induce the release of chemokines such as interferon inducible protein-10, IL-8 and monocyte chemo -attractant protein-1 in human whole blood, through binding to the colony stimulating factor 1 receptor. IL-34 also promotes increases in IL-1β, IL-6 and TNF-α levels 12 and stimulates monocyte viability, promoting the release of proinflammatory cytokines. 8 A further study has shown that the proinflammatory cytokines IL-1β, IL-6 and TNF-α can induce IL-34 in osteoblasts. 13 This suggests that there is crosstalk between IL-34 and other proinflammatory cytokines, such that some proinflammatory cytokines promote the release of IL-34 while IL-34 induces other proinflammatory cytokines, thereby reinforcing the inflammatory process.
The present study showed that IL-34 levels were significantly increased in patients with CAD and this increase was positively correlated with hs-CRP levels. This suggested that IL-34 may be a novel proinflammatory cytokine for CAD and, like other proinflammatory cytokines, may be involved in the pathogenesis of atherosclerotic CAD.
The present study also revealed that the IL-34 level was an independent predictor of CAD, in addition to the hs-CRP level (which is known to be an important predictor for CAD). 6 Several proinflammatory cytokines (including TNF-α, IL-6, HMGB1 protein and hs-CRP) are predictors of CAD3–7 and there is crosstalk between IL-34 and these cytokines,12,13 which further suggests that IL-34 may be an important predictor for CAD. Whether IL-34 levels could predict the occurrence of cardiovascular events needs to be verified with further research.
A limitation of the present study was that it included a small group of Chinese patients. Future investigations to understand the precise mechanisms underlying the observations made in the present study and their clinical significance require a larger cohort. Another limitation was that, although there are many risk factors for CAD, the present study only included a few typical risk factors.
In conclusion, the present study showed that IL-34 levels were significantly increased in patients with CAD, and that this increase was positively correlated with hs-CRP levels. This finding indicates that IL-34 may be a proinflammatory cytokine and an independent predictor for CAD, and requires further study.
Footnotes
The authors had no conflicts of interest to declare in relation to this article.
