Abstract
Background:
The Analgesia Nociception Index device may serve as a guide to a person’s parasympathetic activity via the heart rate variability. It is used to assess the level of discomfort of non-communicative patients at the end of life. Although the index’s acceptability in palliative care have been demonstrated, the healthcare professionals and the patient’s relatives did not have direct, continuous access to the monitor screen.
Aim:
To evaluate how healthcare professionals and patients’ relatives in a palliative care unit perceived the use of the Analgesia Nociception Index.
Design:
A qualitative, comprehensive, two-centre study was based on individual, semidirective interviews. The interview data were evaluated in a reflexive, thematic analysis.
Setting/Participants:
We interviewed (i) healthcare professionals who used the Analgesia Nociception Index in their routine practice and (ii) the relatives of patients who had been monitored with the tool during their stay in the unit.
Results:
A total of 28 interviews were conducted. The device was perceived mainly to be an additional medical technique for increasing a person’s level of comfort. Some professionals highlighted a risk of re-medicalizing the end of life, with a display screen that distracted attention from the person. A few relatives stated that the changes on the screen were a way of staying in touch with their loved one’s perception. The tool helped to increase the value of the relatives’ support.
Conclusion:
The present results might help clinicians to tailor the monitoring to each patient’s situation and to communicate more effectively with both care teams and relatives.
Keywords
What is already known about the topic?
Devices for the automated, non-subjective assessment of discomfort (e.g. continuous monitoring of the parasympathetic nervous system) are used increasingly in palliative care units.
The Analgesia Nociception Index is currently used to monitor pain, although parasympathetic activity is also known to indicate stress and other emotions when the person is awake.
The results of this qualitative study suggest that palliative care specialists and proxies accept parasympathetic activity monitoring as a surrogate for overall physiological comfort.
The role of continuous monitoring in palliative care is complex; the use of this technique can induce anxiety and distract caregivers or relatives.
Relatives sometimes used this tool for relational purposes; they interpreted the Analgesia Nociception Index as an indicator of a person’s responsiveness to their loved ones at the end of life.
Parasympathetic nervous system monitoring has benefits in palliative care but may have to be redesigned to suit the needs and perceptions of healthcare professionals and relatives.
Our results might help to improve the quality of the information and support that healthcare professionals can give to relatives when this type of tool is being used.
This study opens up new areas of research, such as better defining parasympathetic comfort, determining the types of symptom reflected by parasympathetic tone, and establishing whether the presence of loved ones can influence parasympathetic tone.
Introduction
Addressing suffering at the end of life is a major societal challenge. Suffering can become invisible at the end of life when the person is unable to communicate due to neurological failure, sedation, or dying process. Although it is impossible to objectively measure another person’s suffering, clinicians attempt to make a relevant assessment of person discomfort, defined as the presence of a distressing symptom (including pain or anxiety). Discomfort can be assessed using behavioural scales, but the latter’s reliability for the evaluation of people at the end of life has not been fully validated.1–5 It is generally based on clinical judgements by nurses or physicians or non-clinical judgements by family members. Hence, there is growing concern about how comfortable non-communicative person really are. 6
Researchers have developed other types of tools for evaluating discomfort in a palliative setting in general and in non-communicative people in particular. These tools are based on non-subjective measurements of neurophysiological variables thought to reflect the body’s state of relaxation and level of discomfort.7–9 For example, the Analgesia Nociception Index device can be used to assess pain in sedated people. The index is based on the non-invasive measurement of parasympathetic tone via heart rate variability and has proven to be reliable for the assessment of pain during general anaesthesia10–12 or in critically ill people in the intensive care unit. 13 Only a few studies have examined the use of neurophysiological pain indices in the palliative care unit.14,15 Firstly, a prospective study of 12 palliatively sedated people found that the Analgesia Nociception Index detected pain more frequently than caregiver or family assessments and that the various assessments were not significantly correlated. 16 Then, parasympathetic monitoring has been studied in a population of non-communicative people, not necessarily sedated. Indeed, it has also been shown that parasympathetic tone decreases significantly when people are awake and exposed to stressful emotional stimuli.17,18 The Analgesia Nociception Index may then be used to make a more global assessment of discomfort. 19 A second study (retrospective and non-blinded) of 33 non-communicative people in a palliative care unit found that approximately 20% of Analgesia Nociception Index measurements were inconsistent with the clinical assessment of discomfort and resulted in changes in prescriptions. 20 Lastly, the results of another prospective, blinded study of 20 non-communicative end-of-life people (five of whom were sedated) showed that during painful procedures, the Analgesia Nociception Index decreased significantly and more consistently than proxy pain assessment scales. 21
The result of a qualitative pilot study of palliative care confirmed that a patient’s carers and relatives accepted the use of a neurophysiological monitor. 22 However, the carers and relatives could not see the data displayed on the monitor. 22
Some teams use the Analgesia Nociception Index routinely in palliative medicine unit. In parallel, critics have raised concerns about the growing medicalisation and increasing technicality of dying. The Lancet Commissions warned of the risks of medicalisation and a lack of human support and ethical discussion, exacerbated by the structural constraints of the healthcare system. 23 In contrast, palliative care offers a human-centred approach grounded in the ethics of care. 24 It values personal attention, emotional support, and often-invisible caregiving practices. The use of technical and technological tools (such as the Analgesia Nociception Index) could be viewed as a shift away from usual care practices. 19 In a context of impending death, this use has prompted a number of questions and highlighted the need for in-depth studies of how the tool is perceived by the stakeholders.
Methods
The objective of the present study was to explore perceptions of the use of the Analgesia Nociception Index in a palliative care unit. The study forms part of a broader research project on the relevance of parasympathetic monitoring in palliative care, which includes a prospective, observational study conducted during painful procedures 21 and a patient and public involvement study.
Study design
The design of this qualitative study reflects the constructivist belief whereby the perception of reality is influenced by individual, social and historical contexts. 25 The palliative care unit was considered to be a special case, that is, a micro-society (including healthcare professionals, relatives, and patients) for which the Analgesia Nociception Index was not initially developed. 26 This is why an inductive, comprehensive approach was chosen, so that we could question a multitude of stakeholders and assess a group in this particular context.27–30
Setting
The study was conducted at two palliative care units: the unit at Lille University Hospital (Lille, France) had been using the Analgesia Nociception Index in routine practice for over five years, while the unit at Loos Hospital (Loos, France) had been using it for less than a year.
In France, key legislative milestones have shaped end-of-life suffering management for decades. The 1986 Laroque circular established the right to palliative care and was followed by the 2002 Kouchner Act, which prioritised pain relief. The 2005 Leonetti Act introduced therapeutic proportionality and allowed sedative and analgesic treatments that may hasten death in strictly controlled conditions. These laws define sedation practices as proportionate and appropriate responses to refractory suffering. The 2016 Claeys-Leonetti Act reinforced these rights, enabled people to request deep, continuous sedation until death when suffering is refractory and stated that only the patient can judge the unbearable nature of their suffering. 31 The Act reflects a societal stance against end-of-life suffering and a commitment to ensuring a peaceful death.
Population
The close relatives of non-communicative people (whether sedated or not) having been monitored with the Analgesia Nociception Index were considered to be eligible for the present study. The relative had to have (i) supported the person during their stay in the palliative care unit and (ii) met the medical team during this period. Healthcare professionals (including physicians, nurses, and nurse assistants) were eligible if they had cared for at least one patient monitored with the Analgesia Nociception Index in the month preceding the interview.
Sampling
We sought to sample a diverse range of healthcare professionals in terms of age, gender, profession, workplace, level of professional experience, and exposure to the Analgesia Nociception Index. We also sought to sample a diverse range of relatives in terms of age, relationship to the patient, and type of Analgesia Nociception Index use (e.g. as part of a clinical study vs solely in routine practice, during painful treatments over shorter vs longer periods, or during sedation or not).
Recruitment
The relatives were contacted first by telephone and then by e-mail between 6 weeks and 3 months after the patient’s death, in order to allow them to grieve but also to minimize memory bias.32–34 The healthcare professionals were recruited via e-mail or telephone as the study progressed.
Data collection
Interviews were conducted between June 2023 and April 2024. Two researchers (CP’H and MD, both physicians with experience of qualitative research and backgrounds in clinical ethics and palliative care) conducted comprehensive, face-to-face interviews 35 at the interviewee’s home or workplace or in the investigator’s office, depending on the interviewee’s preference. If a face-to-face interview was not possible, videoconferencing could be used (notably for the relatives). Although some of the relatives were interviewed individually, two members of the same family could be interviewed at the same time. All the relatives were interviewed by the principal investigator (CP’H), who was not the attending physician. The healthcare professionals were interviewed individually by CP’H or (when the interviewee worked in the same centre as CP’H) by MD.
The interview guide was developed by a multidisciplinary group of researchers (Supplemental File 1). It explored the representation of suffering and discomfort, commitment to third-party assessment, and the personal relationship with the tool. The interview duration ranged from 25 to 55 min (mean: 37 min). The interviews were digitally recorded (with the interviewee’s permission), transcribed word for word (while taking account of pauses and signs of emotion) by CP’H and MD, and anonymised.
Data analysis
Throughout the research, data were collected and analysed in a cyclical, interrelated fashion. The analysis followed Braun and Clarke’s Reflexive Thematic Analysis Reporting Guidelines.36,37 The analysis was performed interview by interview, in order to detect categories inductively. Three researchers – CP’H (all interviews), MD (interviews with professionals), and FD (interviews with relatives) – familiarized themselves with the data by reviewing and transcribing audio recordings. The initial codes were developed in parallel, in order to capture key elements aligned with the study objectives (mainly at the semantic level) and take account of latent interpretations. Using NVivo software (QSR International, Burlington, MA, USA), 1134 codes were classified into four levels. Coding discrepancies were resolved through discussion and refinement of the codebook. Themes were generated by discussing, reviewing, refining and grouping codes and writing definitions (accompanied by illustrative quotes), until a consensus between CP’H and FD or MD was reached.
Interpretive conceptual categories were subsequently developed by CP’H, by moving beyond thematic description to uncover underlying meanings in the participants’ accounts. These categories were continuously revisited in the light of new data, enabling adaptation of the interview guide and participant selection. To enhance reflexivity and deepen the interpretation, portions of transcripts and emerging conceptual categories were shared with two other (non-investigating) researchers in psychology and sociology. Their feedback prompted further thoughts on the investigator’s assumptions. To ensure rigour and validity, an interdisciplinary team (FP, PS, MD, FD, and CP’H) assessed conceptual saturation, defined as the point at which three consecutive interviews yielded no new category properties. The principal categories were discussed and reviewed with a group of palliative care professionals from recruitment centres, and the last five participants during interview. This process ensured that interpretations were robust and reflected a range of participant perspectives.
In terms of positionality, CP’H had over five years of experience with the Analgesia Nociception Index in routine practice and had conducted quantitative research on its application in palliative care. This background allowed her to develop an informed perspective while maintaining critical distance during interviews. Throughout the analysis process, CP’H engaged in self-reflection, supported by a reflective journal and supervision from FP and PS, which helped her remain aware of her subjectivity and foster an open, creative approach.
Ethical issues
Each participant received an appropriate study information sheet and a consent form. In compliance with the French legislation, the study protocol was approved by an independent ethics committee (CPP Sud Ouest et Outre Mer II, Bordeaux, France; approval reference: 2022-A00631-42). The study database was registered with the French National Data Protection Commission (Commission nationale de l’informatique et des libertés, Paris, France). The participants’ travel costs were reimbursed, when necessary.
As CP’H had a dual role (that of a researcher and a clinician), ethical concerns were considered to ensure the authenticity of the families’ and care providers’ lived experiences in author narrations. The principal investigator (i) clarified her role and the absence of a conflict of interest with use of the Analgesia Nociception Index, and (ii) did not wear scrubs, so that the setting was conducive to discussion and mutual respect. Her position as a palliative care physician further supported the study’s relational ethics, particularly through her familiarity with grief and her ability to respond to personal questions from bereaved relatives.
Analysis
In total, 28 interviews were performed: 14 with healthcare professionals (identified hereafter by a ‘P’ and a number) and 14 with relatives (identified hereafter by an ‘R’ and a number) (Table 1).
Characteristics of the study participants.
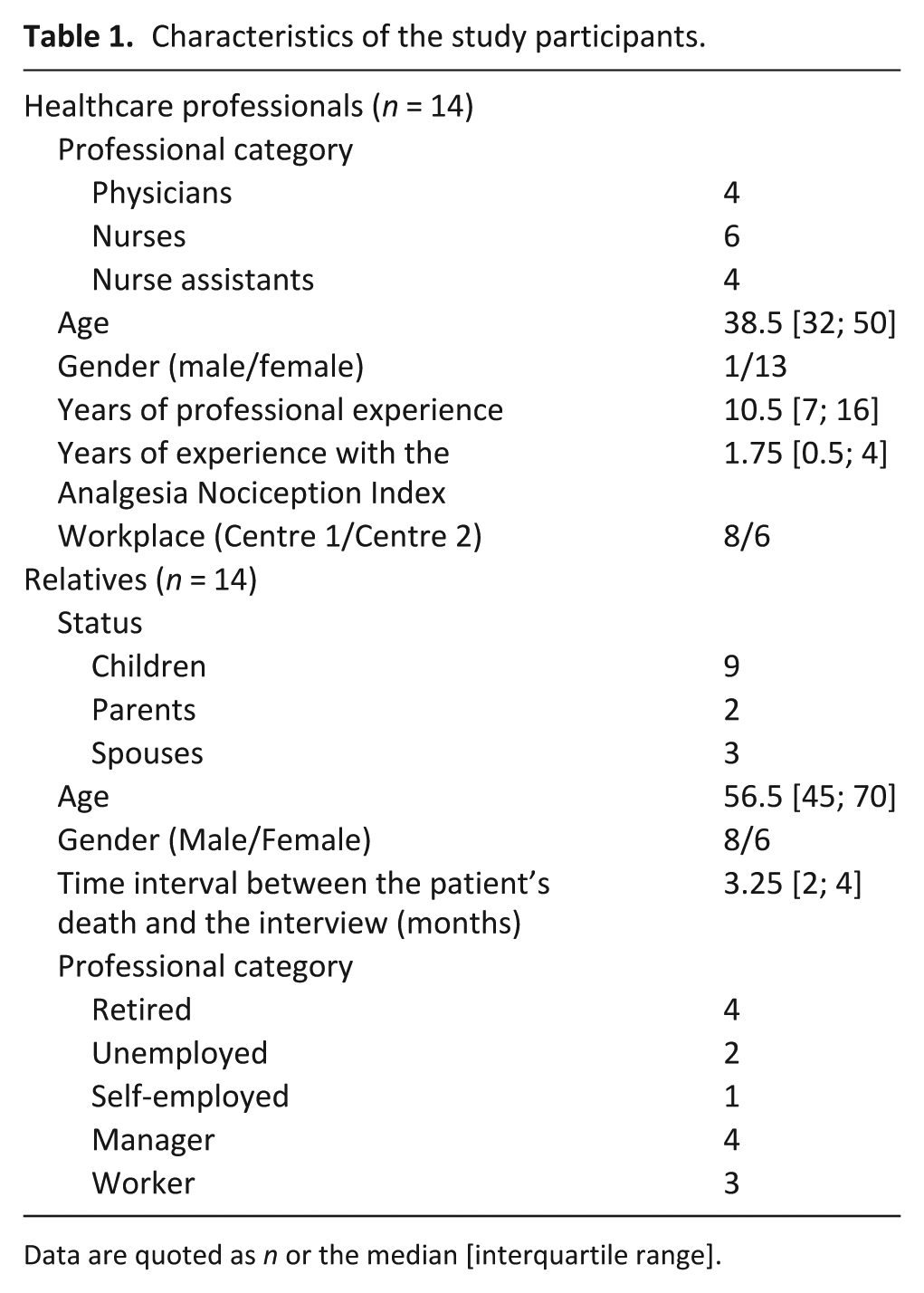
Data are quoted as n or the median [interquartile range].
Nineteen close relatives of people having been successively monitored with the Analgesia Nociception Index were invited to participate in the study. Five were not included: two did not have time for an interview, two did not reply, and one did not remember the Analgesia Nociception Index being used.
All 14 invited healthcare professionals agreed to be interviewed. Eight had between 2 and 5 years of experience of the use of the Analgesia Nociception Index.
Theme 1. Multiple perceptions of well-being
The first theme described how relatives and professionals were heavily involved in assessing people’s discomfort and sometimes used similar procedures to form an assessment (crying, facial expression, gestures, behaviour, breathing, change from previous state. . .). However, their representations of wellbeing varied, as did the vocabulary used (‘discomfort’ for healthcare professionals and ‘suffering’ for relatives). Healthcare professionals believed that they could alleviate people’s discomfort by adjusting their position, addressing sensory perceptions such as smell, sound, and thermo-tactile sensations, and managing certain symptoms, including (but not be limited to) pain. P4: ‘It’s true that when I talk about a patien’s discomfort, I often tend to associate it with pain. But there are many other possible causes. Psychologically, there may also be discomfort’. For them, the ANI tool seemed appropriate for assessing discomfort, referring to ‘parasympathetic wellbeing’ (rest, calm and serenity as opposed to stress and pain). P1: ‘This was one of the first times that we had noticed ANI to be correlated not only with pain, but also with anxiety. In any case, the hypothesis is that it could be correlated with general well-being’, On the contrary, relatives rarely used the concept of discomfort in their discourse, instead emphasising suffering – a broader concept with an important existential dimension, in their view. The ANI tool was unable to assess all dimensions of suffering for participants. P11: ‘For me, suffering encompasses something broader, with psychological and existential elements that are difficult to translate objectively and quantify’, In total, the underlying concept of suffering or wellbeing differs between study participants. This affected the interest and the interpretation of the tool. R7: ‘No, for me, it didn’t change anything. It wasn’t my concern. It was just an extra device that was there, and it didn’t bother me or give me any information. I already knew that she wasn’t suffering anymore since she had been sedate’.
Theme 2. Additional care in a trusting environment
The second theme related to perceptions of the Analgesia Nociception Index monitor as an additional clinical tool in patient-centred care. The healthcare professionals interviewed during the study used the Analgesia Nociception Index as a tool to provide additional information and as a guide to the patient’s discomfort but which did not replace the carer’s expertise. P10: I find that it’s an additional source of help, it’s not. . . I won’t base my judgement just on that.
Many benefits of the Analgesia Nociception Index were described during the interviews. The device contributed to the assessment of discomfort, which the interviewees considered to include (but not be limited to) pain. It helped to distinguish between comfort situations and discomfort situations and to determine the cause of discomfort. In the interviewees’ opinion, the tool could also be used to avoid drug over-dosing and hastening death. The Analgesia Nociception Index was perceived as a reassuring tool for healthcare professionals and relatives. Lastly, the Analgesia Nociception Index was occasionally used to mediate between differing clinical assessments by members of the care team.
As we had doubts about discomfort, we first administered a bolus of midazolam to see if it had any effect, and then a bolus of morphine, or vice versa, to see if that made any difference. Because we wonder if it’s anxiety or pain, but since we can’t interact with them, we have no way of knowing.
It corresponded to what she wanted and what we wanted, namely providing her with some comfort without. . . without going. . .without going too far.
The support provided by the healthcare professionals with regard to use of the tool demonstrated that everything was being done to take care of the person at the end of life; this reassured the relatives and was greatly appreciated. R6: In fact, if the staff are relaxed, we’re relaxed. And having this machine there, well, that helped too because we said to ourselves, right, they’re putting things in place. So that she suffered as little as possible, whereas we could tell that she was in a state where. . .. ‘Is she suffering or not’, You see? And so, we kept on giving her support and, yeah, that’s what put my mind at rest, to have the whole team around us.
Furthermore, some relatives stated that they accepted the tool because they trusted the healthcare team using it. R12: We trusted them, we said to ourselves that it was a work tool for them.
The adverse effects of using the device were so limited that, from a professional point of view, it did not appear to be necessary to seek consent from relatives and patients – even though the tool was presented to them and they had the option of refusing it. P1: I don’t really remember there being any problems with the relatives. We explained things, of course - we always explain things. Everyone was satisfied because he was comfortable afterwards.
Theme 3. An anxiety-inducing intrusion into end-of-life care
While analysing the interviews, we observed that the Analgesia Nociception Index could be considered as an intrusive technique in the palliative care unit. Some healthcare professionals feared turning the person into a stream of data and mentioned the risk of depersonalization. The tool was seen as being futile or as boiling down the concept of suffering to mere bodily or physiological well-being – far from the attention to psychological or existential suffering at the end of life. P13: And then bear in mind that it’s a machine and that we don’t treat a machine. That is an oversimplification and it’s not necessarily very coherent with the message, we can’t judge the patient’s pain, it’s subjective, it’s linked to their lived experience, their personal experience and then all of a sudden we pull out a machine with a figure. It’s difficult to make the two compatible!
Some healthcare professionals reported that the Analgesia Nociception Index can over medicalize end-of-life, which is not always in line with the spirit and objectives of palliative care. One of the interviewed relatives remembered the tool as being disturbing because it was noisy and flashing; in reality, the Analgesia Nociception Index does not make any noise and does not have any flashing lights. This distorted memory can be interpreted as a negative reaction to the Analgesia Nociception Index’s intrusion into a space devoted to something else, such as human relationship or the pain of losing someone. P10: Yes, of course, whatever hospital ward it is, when you go into a room with a line of machines, it always makes you anxious. You say to yourself ‘oh wow, there are cables and leads all over he’. They’re from machines that are to there to help, of course, but it hits you like a hammer when you see that she’ll all wired up. The best thing is to go into a room where there’s nothing.
We observed that the Analgesia Nociception Index was associated with a risk of distracting the healthcare professionals’ or relatives’ attention at the end of life: the data and the figures on the screen were reported to be more attractive than a face or an ‘unfathomable’ body. P4: I told myself that perhaps it was an obstacle to our way of monitoring our patients. Because suddenly there’s this screen, and the first thing we do when we enter the room is to look at the screen which is on. . . I said to myself ‘Ah yeah, tha’s strange all the same, we don’t usually do that, we don’t look at the figures - we look at our patient’. The device might have led to a loss of expertise in ‘reading’ the patient’s body and assessing the level of comfort. Some carers or relatives reported that they felt an almost irresistible attraction to the device’s screen and read the numbers or the Analgesia Nociception Index curve in real time. This could create an uneasy feeling of distraction that drove them to turn the screen away or to ask to have the screen switched off. R9: in fact, I was attracted by the graphs - so, at a certain point, I pushed it away so that I didn’t look at the graphs anymore because, in fact, well, it had become an obsession.
The Analgesia Nociception Index seemed to induce more stress when the relatives had little knowledge about how the device worked and how the data could be interpreted. R14: We knew very well that death was imminent and we said to ourselves ‘what do the sensors really mean because they do’,t detect anything?’. Does it means that it’s about to happen, right now? Does it means that in fact, she’s breathing really weakly? In the end, perhaps it caused us to worry more because it saying ‘Right, i’s strange all the same, it’s strange’.
Some healthcare professionals avoided using this device when relatives were present, to avoid disturbing them. P3: And it’s true that I tend to end up. . . well, when the patient is stable. . . removing the ANI when the family is there. Because I really feel that they focus on it and it becomes their sole focus, to the point that they even forget. . . Before, they would touch the patient, do a few things, and now they’re more focused on that.
Theme 4. Reimagining the use of the Analgesia Nociception Index: a new means of communication?
Our study showed that there was another way of using the parasympathetic monitoring in palliative care – a way that didn’t focus on comfort assessment. Some relatives intuitively reinterpreted the Analgesia Nociception Index as a way for their unconscious loved one to communicate with them. They viewed the device as a last means of maintaining some sort of relationship and observed that being present, speaking to the patient, or touching the patient had an impact on the Analgesia Nociception Index. R7: that, well, when I talked to her, that it made me feel better and, in fact, seeing that I got a reaction! Not a physical reaction because she didn’t squeeze my hand, she didn’t. . . but there you are, when I was there and I talked, I could see a reaction.
Acknowledging the impact of the relative’s presence via the device reinforced the importance of their role as supporting their loved one and added meaning to their continued presence. R5: it helped me all the same to see whether he knew that I was there, if he realised that I was present. . .
This ‘relational’ use of the Analgesia Nociception Index was not noticed by most of the healthcare professionals; only one mentioned it but doubted whether this perception was of value and suggested that the relatives might be misusing the device.
According to another relative, this ‘relational’ use sometimes led to conflict with the staff: whereas the staff used the ANI to assess patient comfort only when they deemed it necessary, the relative needed it on at other times for relational purposes. R5: Even once it had been unplugged, I asked to have it on. . . because they didn’t turn it on all the time. I think that they should at least ask before unplugging it. I would really have liked it not be unplugged.
Discussion
Main findings
The results of this qualitative study showed that health care professionals trust the parasympathetic monitoring to add to their assessment of overall comfort (and not only pain assessment) in non-communicative patients at the end of life (Figure 1). Although numerous benefits of parasympathetic monitoring have been identified, the technique should be used with care so that suffering is not objectifying. The role of the Analgesia Nociception Index in palliative care is complex; continuous monitoring can induce anxiety and be a distraction for healthcare professionals and relatives. However, our results revealed that relatives used the tool for relational purposes; this novel use was not noticed by the healthcare professionals. Continuous measurement of parasympathetic nervous system activity was seen as an indicator of a person’s responsiveness to loved ones at the end of life, and thereby promoted support.
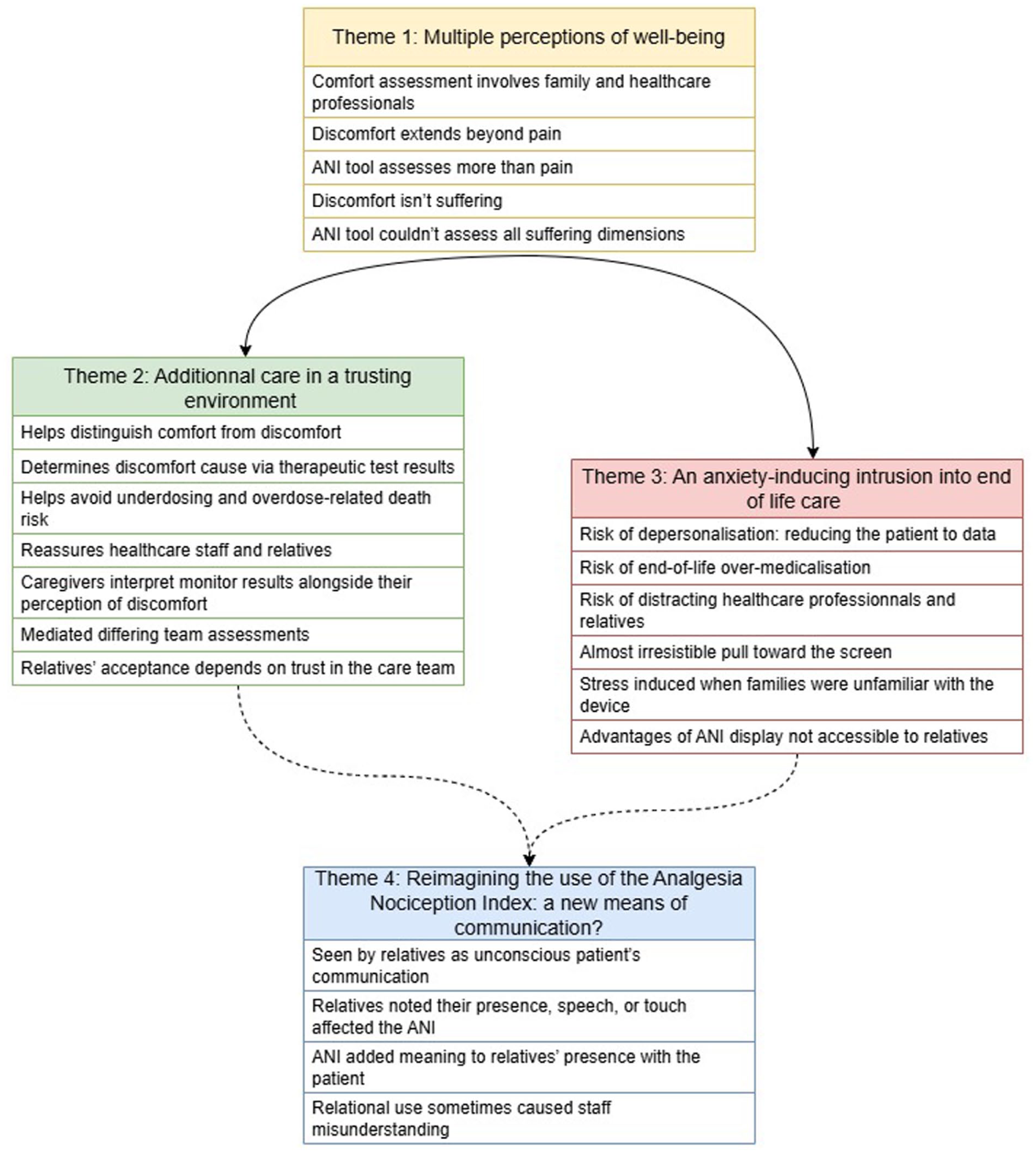
Conceptual framework.
Strengths and limitations
To enhance the robustness of our results, we employed various qualitative research tools: crystallization, member reflections, a critical friend, and the use of reflexive diary-keeping by the principal investigator throughout the analysis period.36,37 Given that the principal investigator works at one of the two investigating centres, her personal experience might have influenced her reflective analysis. Furthermore, staff members and relatives might not have been fully sincere when interviewed.
The results of the present study may open up avenues for qualitative research in other contexts and other populations. In fact, we found that the level of trust in the palliative care unit and its staff with regard to the attention given to end-of-life people fostered the device’s acceptance by the relatives. It would be interesting to use the Analgesia Nociception Index in other contexts, such as neurology, geriatric medicine, and less medicalized settings like care homes. The results of the present study cannot necessarily be extrapolated to other settings, and so further research is warranted.
What this study adds
The results of this qualitative study indicated that in palliative care units, parasympathetic activity monitoring is used to assess the overall or physiological comfort (and not solely pain) in non-communicative patients (whether sedated or not). Although it is impossible to objectively measure another person’s suffering, clinicians expect that these tools can significantly improve comfort assessments.14–16,20 Comfort is an ambiguous concept and varies from one individual to another as a function of backgrounds, desires, cultures, and family dynamics.38,39 The Analgesia Nociception Index highlights comfort linked to parasympathetic balance and reflects physiological well-being. This raises questions about perceptions of another person’s comfort, which can differ when comparing healthcare professionals, patients, and the patients’ relatives.
Six et al. evidenced showed good acceptance of the tool. 22 The present study shows that the role of technology-based monitoring in palliative care is complex: continuous access to the device’s screen may induce anxiety and distract caregivers or relatives. With reference to good practice guidelines on telemetrics in intensive care, some healthcare professionals appeared to think that the Analgesia Nociception Index might focus the relatives’ attention away from their loved one and towards the screen.40,41
Furthermore, it appeared that differing interpretations of the Analgesia Nociception Index’s value in the palliative care unit can create misunderstandings between healthcare professionals and relatives. Although the primary (medical) use is better assessment of discomfort at the end of life, some of the relatives imagined that the device had a more relational function. In fact, they saw the Analgesia Nociception Index as a reflexion of the person’s inner experiences, emotions, and reactions. 42 These relatives used the tool to re-establish contact with the patient after the latter had lost the ability to communicate. In fact, one can hypothesize that because the tool facilitates the family’s support and meaningful presence at the end of life, it contributes to a ‘good death’ 30 and helps with the grieving process.
Implications for practice, theory or policy
Given the benefits of parasympathetic nervous system monitoring in palliative care, it could be more readily deployed if adapted to suit the perceptions of healthcare professionals and relatives. Our results highlighted the range of perceptions linked to the use of parasympathetic monitoring at the end of life. This finding might help clinicians to tailor the tool’s use to each given situation and to communicate more effectively with both care teams and relatives.
Our findings suggest that tool developers should modify the design to better suit end-of-life situations. We identified a risk of excessive attention and concern about the device among distressed relatives, suggesting features like standby mode or modified graph access. Further research on the ergonomics for healthcare professionals and relatives is needed.
This exploratory, qualitative study opens up new research avenues for monitoring the parasympathetic nervous system in non-communicative people receiving palliative care and increasing the relevance of these techniques in end-of-life situations. These avenues include the definition of patient comfort at the end of life, and understanding the types of distressing symptoms that parasympathetic nervous system monitoring could reveal in non-communicative, non-sedated patients. Furthermore, quantitative research could usefully explore (i) whether the Analgesia Nociception Index is influenced by the presence of loved ones and, if so, under which conditions, and (ii) how the use of parasympathetic monitoring can help loved ones provide support to patients. The Analgesia Nociception Index’s relational use may be relevant in contexts like neonatology, where such devices are used regularly. 43 We hypothesize that the Analgesia Nociception Index might promote skin-to-skin care and might provide support for the parents of children with a life-limiting or life-threatening condition.44,45
Conclusion
‘Is he/she suffering?’ ‘Can he/she sense my presence?’ In palliative care units, these are common questions asked by relatives and healthcare professionals with regard to non-communicative patients. According to the interviewees, the continuous monitoring of parasympathetic nervous system activity might help to answer these questions, provide support, and improve the care of non-communicative patients at the end of life. This qualitative research might guide future research on the benefits of parasympathetic monitoring in this context.
Supplemental Material
sj-docx-1-pmj-10.1177_02692163251393576 – Supplemental material for ‘It showed me that he sensed I was there. . .’, The ‘relational’ use of an electrophysiological tool for evaluating the level of discomfort of people at the end of life: A reflexive thematic analysis
Supplemental material, sj-docx-1-pmj-10.1177_02692163251393576 for ‘It showed me that he sensed I was there. . .’, The ‘relational’ use of an electrophysiological tool for evaluating the level of discomfort of people at the end of life: A reflexive thematic analysis by Chloé Prod’homme, Flore Homey-Dusautois, Manon Denié, Licia Touzet, Claire Pasqualini, Magali Pierrat, François Puisieux and Philippe Sabot in Palliative Medicine
Footnotes
Acknowledgements
We thank all the palliative care professionals at Lille University Hospital and Loos General Hospital (particularly Dr Luc Chevalier and Dr Helene Lesaffre) and all the relatives who participated in the study. We also thank Esther Sansone and Nicolas Pujols (University of Lille, Lille, France) for helpful discussions. Furthermore, we thank the members of the METRICS lab who helped to design the interview guide and the methodological quality analysis plan: Jean-Baptiste Beuscart, Carla Di Martino, Christine Moroni, Vincent Caradec, and Marc Bayen. Lastly, we thank David Fraser (Biotech Communication SARL, Ploudalmézeau, France) for copy-editing assistance.
Ethical considerations
The study was approved by an independent ethics committee (the study protocol was approved by an independent ethics committee (Comité de Protection des Personnes Sud Ouest et Outre Mer II (Toulouse, France) on July 22, 2022 (reference: 2022-A00631-42).
Consent to participate
All participants received a study information sheet and gave their written, informed consent to participate before enrolment in the study. In accordance with French legislation, the participants’ demographic data were anonymized.
Author contributions
CP’H, LT, FP, and PS designed the study, MP, PS, and FP supervised the study. CP’H, PS, and FP drafted the interview guide, CP’H was responsible for recruitment, CP’H reviewed and corrected the interview guide, CP’H performed the qualitative analysis, MD and FD cross-checked datasets, CP’H drafted the manuscript, PS and FP supervised the study, and all authors reviewed the manuscript.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by the Cellule d’animation régional des soins palliatifs en Hauts-de-France non-profit organisation (Lille, France).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The qualitative data used to support the findings of this study are available on reasonable request from CP’H.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
