Abstract
Regulatory guidelines for nonclinical neurotoxicity testing require spinal cord evaluation but do not specify a trimming scheme. The Society of Toxicologic Pathology (STP) “best practices” for nervous system sampling during nonclinical general toxicity studies recommend that spinal cord be assessed in both longitudinal/oblique and transverse sections. This article defines possible longitudinal/oblique orientations, describes their benefits and challenges, and provides an expert recommendation regarding suitable trimming planes. Longitudinal parasagittal (LP) sections follow a vertical plane just lateral to the midline, revealing sensory and motor tracts but little gray matter. Longitudinal horizontal sections transect only sensory or motor tracts and variable quantities of gray matter. Oblique vertical (OV) sections angle across the spinal cord from side to side. Oblique transverse (OT) sections slant through from top (dorsal [posterior]) to bottom (ventral [anterior]). Compared to longitudinal planes, oblique orientations demonstrate considerably more gray matter and white matter. Current STP “best practices” explicitly recommend the LP and OV options; the OT orientation also will yield suitable sections while permitting assessment of anatomic symmetry. Selection among the LP, OT, and OV planes should be at the discretion of the study pathologist. The bilaterally symmetrical OT sections likely will be analyzed most easily by nonneuropathologists.
Current regulatory guidelines for nonclinical neurotoxicity testing mandate assessment of the spinal cord, and sometimes specific spinal cord segments, but do not specify the orientation in which the tissue must be trimmed for evaluation (U.S. Environmental Protection Agency 1998a, 1998b, 1998c; U.S. Food and Drug Administration 2000; Organisation for Economic Co-operation and Development 1995a, 1995b, 1997, 2007). The Society of Toxicologic Pathology (STP) “best practices” for nervous system sampling from regulatory-type nonclinical general toxicity studies recommend that spinal cord should be surveyed in a cross-sectional (transverse) plane as well as in either a longitudinal or oblique orientation (Bolon et al. 2013). The reasons for endorsing inclusion of a longitudinal/oblique section are that (1) it exposes more tissue for analysis than does a single cross section and (2) subtle changes often are best detected in sections where nerve fibers can be examined over extended distances. The author’s experience has demonstrated that the preferred alignment of the longitudinal/oblique section varies among institutions. This opinion piece discusses potential advantages and disadvantages of the main longitudinal/oblique orientations for spinal cord trimming, discusses their concordance with the STP “best practices” recommendations, and offers an expert opinion regarding which orientation might be most suitable for inclusion in institutional standard operating procedures (SOPs) for spinal cord processing.
The first option is a longitudinal parasagittal (LP) orientation, in which the section represents a vertical plane from top to bottom (where “top” is the dorsal [posterior] surface and “bottom” is the ventral [anterior] surface; Figure 1). The plane of section typically is located approximately 1 to 2 mm (for rodents) to 3 to 5 mm (for nonrodent species) lateral to the midline. The major advantage to this orientation is that it highlights the primary white matter domains (i.e., key sensory [dorsal funiculi] and motor [ventral funiculi] tracts) that may be damaged by exposure to some neurotoxic agents. A second benefit is that the spinal cord possesses an elliptical cross section in that it is slightly flattened on the dorsal and ventral surfaces; cord specimens may be positioned and immobilized more easily when placed on such a level surface, which permits more consistent siting of the LP trimming plane. A third advantage is that it is easy to find the midline of each sample using the dorsal median sulcus and/or ventral median fissure as external landmarks, which means that interindividual variation in placement of the LP trimming plane should be minimal. The only major disadvantage for the LP orientation is that parasagittal sections just lateral to the midline will demonstrate very little gray matter. However, the several advantages of the LP trimming plane make it a preferred approach for spinal cord trimming at many institutions. The LP orientation is one of the “best practices” for spinal cord trimming advocated by STP (Bolon et al. 2013).

Longitudinal parasagittal (LP) sections employ a vertical trimming plane that is located just lateral to the midline, extending from the dorsal (posterior) surface (shown here at top) to the ventral (anterior) surface (at bottom). This longitudinal/oblique orientation is an acceptable trimming option in the existing Society of Toxicologic Pathology “best practices” recommendations (Bolon et al. 2013).
The second option is a longitudinal horizontal (LH) orientation, in which the plane of section represents a horizontal plane extending from one lateral face (“side”) to the other (Figure 2). The chief advantage to this orientation is that the horizontal plane can be positioned to highlight specific parts of the spinal cord, commonly either the sensory tracts and dorsal horn gray matter or the motor tracts and ventral horn gray matter. However, a major disadvantage is that multiple LH sections are required to evaluate all the key white matter tracts which are known to be targeted by neurotoxicants. A lesser drawback is that the rounded lateral surface of the spinal cord may allow samples to shift (“roll”) slightly during trimming, which can increase the variability among sections obtained for different animals. The LH orientation is not an STP-recommended practice for regulatory-type nonclinical toxicity studies. Instead, in my experience, the LH approach is only used in discovery-type experiments designed to target specific regions of the spinal cord and is employed rarely even for this purpose.

Longitudinal horizontal (LH) sections represent a level plane extending from one lateral face (“side”) to the other across the middle of the spinal cord. This orientation cannot demonstrate all principal spinal cord domains in one section and thus is not an effective longitudinal/oblique trimming option for regulatory-type nonclinical studies.
The third option is the oblique vertical (OV) orientation, in which the section represents a vertical plane that angles across the spinal cord from side to side (Figure 3). In my experience, the trimming angle (using the lateral margin of the specimen as the baseline) should be 30°; if the cut is initiated adjacent to a spinal nerve root, this choice should permit the trimming plane to traverse at least one full spinal cord segment in common vertebrate species. The main advantage to this orientation is that it unveils more gray matter (both horns on both sides) and white matter (all tracts in all 3 funiculi on both sides) than do LP or LH orientations. As with LP sections, the ability to place samples on the flattened dorsal or ventral surface for trimming affords more stability when undertaking an OV cut. Minor disadvantages to this trimming method are that the oblique angle can make it difficult to precisely localize findings to a specific spinal cord domain and that a new mental “map” of regional anatomy must be built by practitioners since standard training programs impart spinal cord anatomy in purely longitudinal and transverse orientations. The capacity to view all spinal cord zones in a “longitudinal” orientation makes the OV option a favored strategy at many institutions. The OV orientation is the second STP-recommended “best practices” option for spinal cord trimming (Bolon et al. 2013).
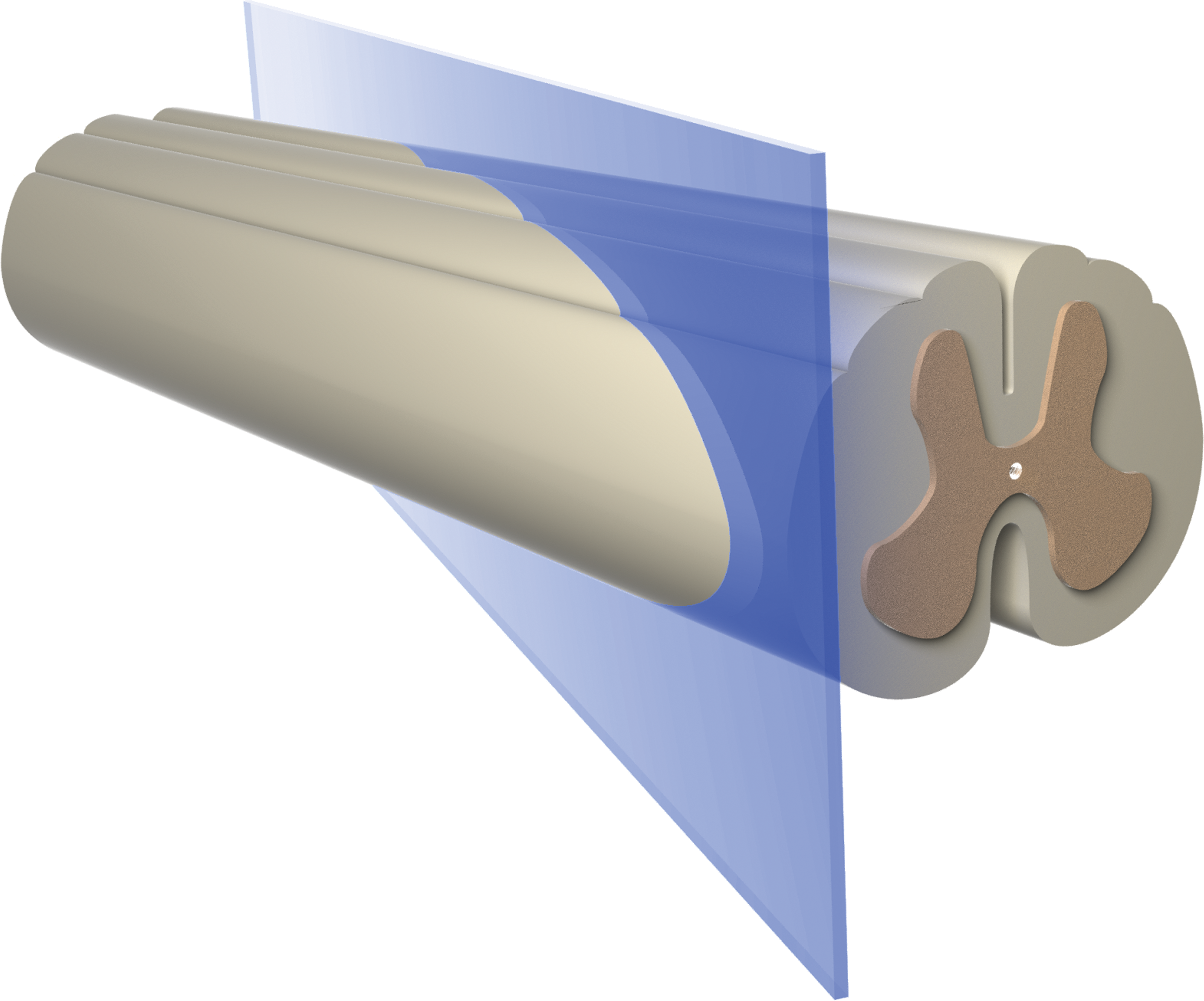
Oblique vertical (OV) sections are produced using a vertical plane that slants across the spinal cord from side to side at an approximately 30° angle (when using the middle of a lateral surface as the baseline). This orientation is another suitable longitudinal/oblique trimming option in the existing Society of Toxicologic Pathology “best practices” recommendations (Bolon et al. 2013).
The last option is the oblique transverse (OT) orientation, in which the section represents an inclined plane traversing the spinal cord from top to bottom (Figure 4). As with the OV plane, the trimming angle for the OT orientation should be 30° (using the dorsal or ventral surface of the specimen as the baseline), and starting the slice near a spinal nerve root should permit the trimming plane to traverse at least one full spinal cord segment. The cut typically is started from the dorsal surface and extended caudally. The reason for this approach is that the cranial end of the section will contain the dorsal funiculi (i.e., sensory tracts). Lesions in the sensory tracts are a common manifestation of neurotoxicant-induced nerve fiber damage, and such changes often are detected more readily in the cranial portion of the spinal cord, which is enlarged as it contains axons from both limbs and the trunk (Krinke 2011). As with the OV approach, the OT strategy discloses more gray matter and white matter than do LP or LH sections. An additional advantage unique to the OT plane is that evaluation of symmetry is feasible for all structures in the section, rendering the OT orientation equivalent to a modestly tilted transverse section. The possibility for bilateral comparison in OT sections should assist practitioners to localize lesions. The only minor disadvantage to the OT approach relative to the LP and OV options is that OT samples will need to be trimmed while balanced on a lateral (i.e., curved) surface. This orientation is used already by some institutions, and the ability to assess lesion symmetry suggests that more organizations may adopt it in the future. The current STP “best practices” for spinal cord trimming do not mention the OT orientation, but in my estimation, the OT approach acceptably meets the intent of the STP recommendations with respect to providing a longitudinal/oblique section for analysis.
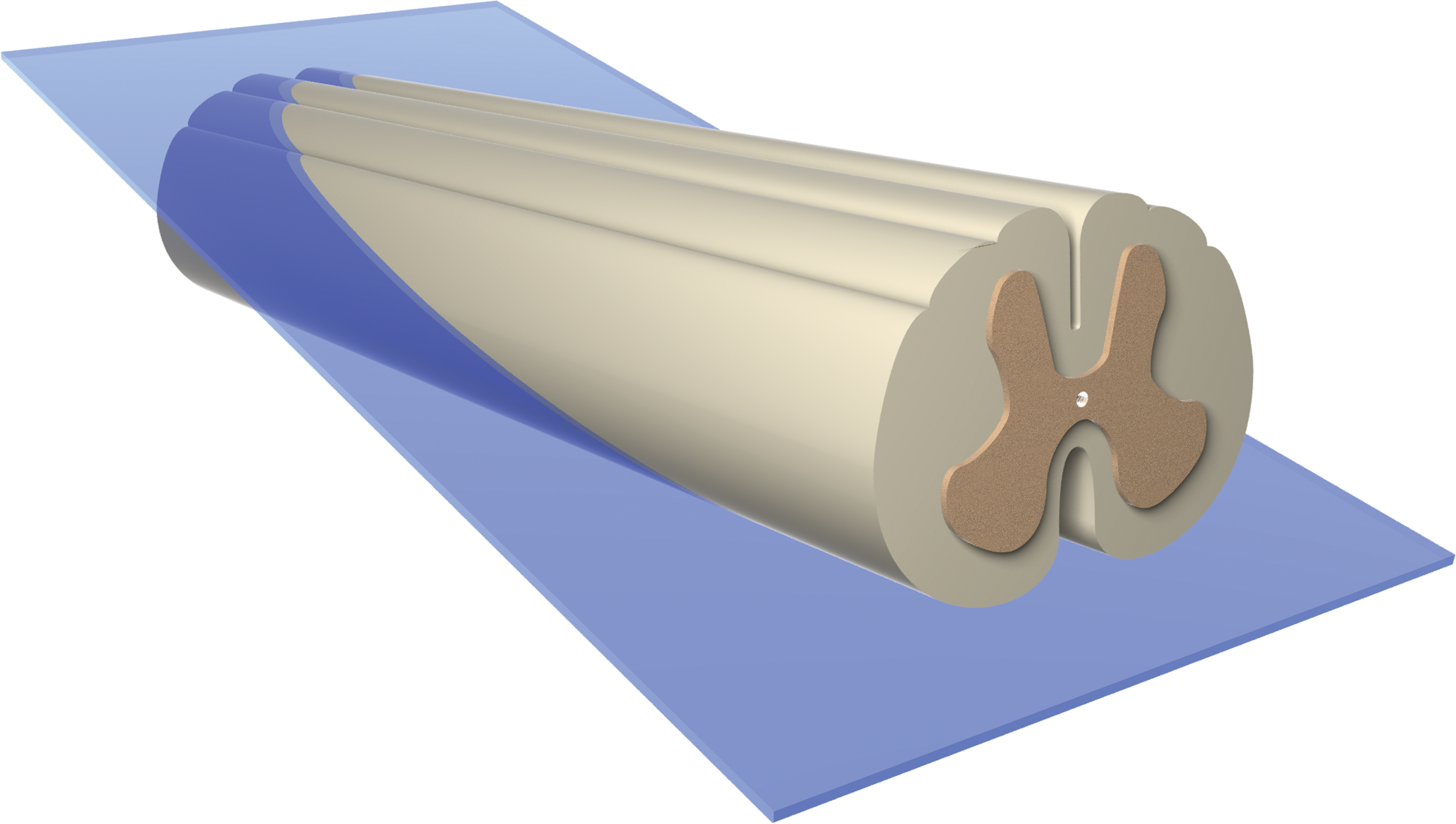
Oblique transverse (OT) sections follow an inclined plane traveling through the spinal cord from the dorsal (posterior) surface to the ventral (anterior) surface at approximately a 30° angle (when using the dorsal or ventral surface as the baseline). The cut typically is started from the cranial end of the specimen (shown here at left) on the dorsal surface (at top) and then extended caudally and ventrally. All spinal cord regions can be evaluated for bilateral symmetry using this strategy. This orientation is not mentioned in the Society of Toxicologic Pathology (STP) “best practices” but effectively meets the STP recommendation that longitudinal/oblique spinal cord sections be assessed.
In summary, current STP “best practices” state that spinal cord should be evaluated during regulatory-type nonclinical toxicity studies not only in cross section but also in longitudinal or oblique orientation and explicitly acknowledge the LP (Figure 1) and OV (Figure 3) trimming planes as providing acceptable longitudinal/oblique sections of spinal cord. Logic and geometry show that the OT trimming plane (Figure 4) will yield analogous sections, indicating that the OT approach also should be judged to be an acceptable strategy for preparing longitudinal/oblique specimens of spinal cord in regulatory-type nonclinical toxicity studies. Selection among the LP, OV, and OT orientations should be left to the preferences of the study pathologist and institution. For clarity, the chosen orientation should be stated in the study protocol, the methods section of the pathology report, and/or an institutional SOP. My view is that any of these orientations provides a suitable screen for examining additional spinal cord tissue, but in my opinion, the two best approaches would be the OT and OV options (which show all parts of the spinal cord), and for non-neuropathologists the OT plane (which permits ready recognition of structural features due to the bilateral albeit elongated symmetry of the anatomic regions).
The primary factor for success in using any of these longitudinal/oblique orientations will be ensuring that the alignment of the trimming plane—and especially the angle for making the OT and OV cuts—is consistent among animals, so that microscopic comparison of features is feasible across sections from different animals within and among treatment groups. The necessity for both accuracy and precision in this setting is comparable to that required for brain trimming, in which meticulous attention to detail is necessary to generate highly homologous sections for analysis. Therefore, once the institutional choice of a preferred longitudinal/oblique orientation has been made, spinal cord trimming could be readily implemented as an SOP to ensure selections are taken consistently in the appropriate orientation.
Footnotes
Acknowledgment
The author thanks Mr. Timothy Vojt for his graphic design talents in creating the figures.
Author Contribution
The author (BB) contributed to conception or design, data acquisition, analysis, or interpretation; drafted the manuscript; and critically revised the manuscript. All authors gave final approval and agreed to be accountable for all aspects of work in ensuring that questions relating to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
