Abstract
The incidence and range of spontaneous pathology findings were determined in the eyes of male and female control Crl:CD-1(ICR)BR mice. Data were collected from 250, 430, 510, and 2,266 mice from control dose groups of 4-, 13-, 80- and 104-week studies, respectively, carried out between 2005 and 2013. Lesions of the eye were very rare in 4- and 13-week studies, uncommon in 80-week studies, and were of relatively higher incidence in 104-week studies. No sex predilection in the incidence of eye lesions was apparent. No neoplastic lesions were observed, and congenital lesions were very rare. The most common findings were cataracts, retinal degeneration, mineral deposits in the iris, keratitis, anterior uveitis, and mineral deposits in the corneal stroma. These lesions were observed only in animals from 80- and 104-week studies, except retinal degeneration which was observed in animals from all age-groups. There are no previous reports of mineral deposits in the iris in this strain of mice. It is hoped that reference to the incidences reported here will facilitate the differentiation of spontaneous lesions from compound-induced lesions in toxicology studies in this strain of mouse.
Introduction
The incidence of spontaneous lesions of the eye in most toxicology studies is often low and variable. The incidence of these spontaneous lesions also depends on the strain and age of the mice. Some of these spontaneous lesions may resemble compound-induced lesions. This could complicate the interpretation of pathology results in toxicology studies. The CD-1 mouse is one of the most common strains of mice used for toxicology studies in Europe. However, despite their common usage, specific information on the incidence of spontaneous background pathology findings in the eye is not readily available. It is important for the pathologist to have available some reference material such as a historical control database with incidences of spontaneous findings in the CD-1 mouse.
The scope of this article is to summarize incidence of spontaneous eye lesions in Crl:CD-1(ICR)BR mice of various age-groups from studies carried out at Charles River Edinburgh, and also to give a brief morphological description of the most common lesions.
Material and Methods
Animals
The details of the sources of data are presented in Table 1. This report is based on eye samples from a total of 3,456 CD-1 mice (250 from 4-week, 430 from 13-week, 510 from 80-week, and 2,266 from 104-week studies) obtained from control groups of preclinical toxicological studies evaluated between 2005 and 2013 at Charles River, Edinburgh. All animals incorporated into the study were obtained from control groups of Good Laboratory Practice compliant preclinical toxicity studies. Prestudy indirect ophthalmoscopic examinations were done on all animals. In most studies, orbital sinus blood collection was performed; however, the proportion of animals that had orbital sinus blood collection performed and the frequency of blood collection were variable between studies.
Details of data sources.
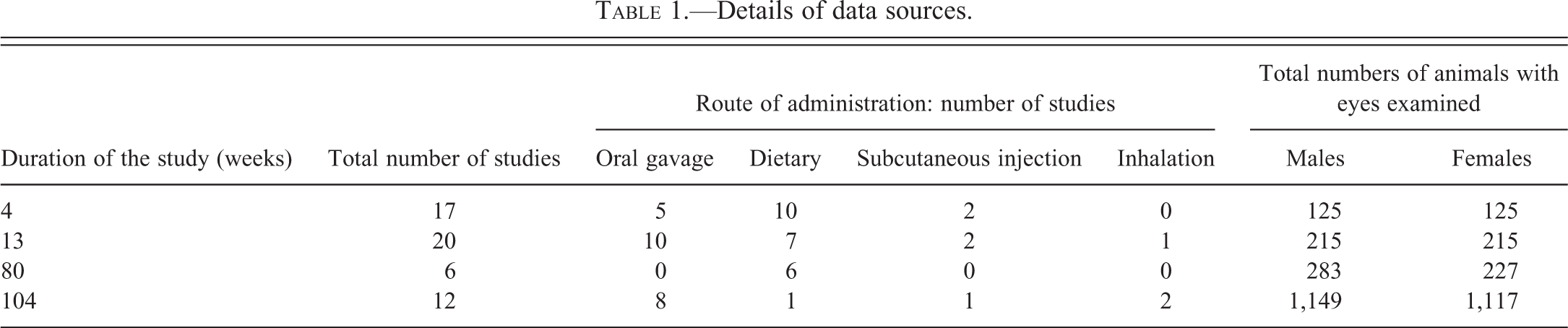
Control groups were untreated or received an appropriate vehicle. Control groups varied in size. For the 4- and 13-week studies, control groups comprised 10 to 15 animals per sex, and for the 80- and 104-week studies, control groups comprised at least 50 animals per sex.
Male mice were housed separately and female mice in groups of 3 animals per cage. Animal room temperature and humidity were automatically controlled at 19° to 23°C and 40 to 70%, respectively, with a minimum of 15 air changes per hr. An automatic 12-hr light/dark cycle was maintained. Animals had free access to tap water in bottles with sipper tubes and were fed an
All studies were conducted in accordance with the U.K. Animals (Scientific Procedures) Act 1986, which conforms to the European Convention for the Protection of Vertebrate Animals used for experimental and other scientific purposes (Strasbourg, Council of Europe).
Pathological Evaluation
Animals were humanely euthanized by a rising concentration of carbon dioxide and exsanguinated via femoral veins. Comprehensive necropsy was performed on all animals. Both eyes were fixed in Davidson’s fluid. The eyes were trimmed, processed routinely, embedded in paraffin, sectioned at 4 to 5 μm (1 section per eye), and stained with hematoxylin and eosin (H&E). Histopathological evaluation was performed by a board-certified veterinary pathologist or a veterinary pathologist with training and experience in laboratory animal pathology. Data from all studies were recorded by direct computer entry by the study pathologist using PLACES 2000 (Instem, Apoloco Limited Systems, Pennsylvania). Data presented here are from untreated control groups only. Lesions involving the conjunctiva, eyelids, optic nerve, lacrimal and Harderian glands, and periorbital tissues were not included.
Results
The variety and incidence of the spontaneous findings encountered in CD-1 mice from 4-, 13-, 80-, and 104-week studies are presented in Table 2. In general, there was an age-related increase in the incidence of most lesions. No sex predilection in the incidence of eye lesions was apparent. No neoplastic lesions were observed and congenital lesions were very rare. The most common lesions were cataracts, retinal degeneration, mineral deposits in the iris, keratitis, anterior uveitis, and mineral deposits in the corneal stroma. These lesions were observed only in animals from 80- and 104-week studies, except retinal degeneration that was observed in animals from all age-groups.
Histological findings of the eye in Crl:CD-1(ICR)BR mice.
Cornea
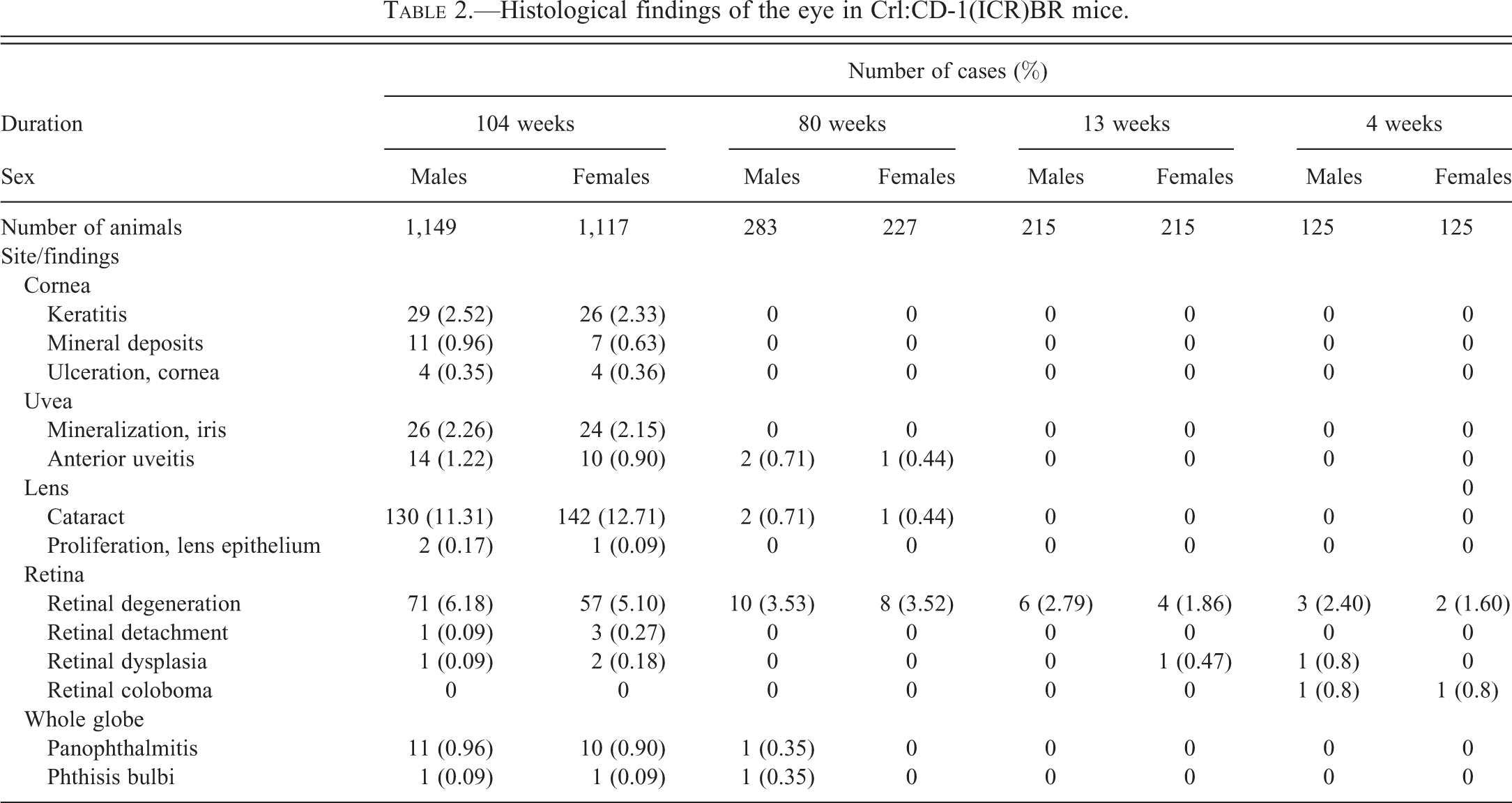
Lesions affecting the cornea were only observed in animals from the 104-week studies. The most common lesion was keratitis. Keratitis was classified as acute or chronic. Acute keratitis was characterized by infiltration with neutrophils and stromal edema, and chronic lesions were characterized by thickening and keratinization of the corneal epithelium and stromal fibrosis (Figure 1A and B). The second most common lesion was mineral deposits in the cornea. Mineral deposits were present as basophilic extracellular granules in the corneal stroma, and in some cases deposits were accompanied by minimal infiltration by macrophages, multinucleated giant cells or lymphocytes. Corneal ulceration was the third most common corneal lesion and was often associated with keratitis or corneal mineral deposits.
Histopathology of the corneas of CD-1 mice (H&E). (A) Chronic keratitis characterized by keratinization and necrosis of the corneal epithelium and infiltration of the cornea by neutrophils. Bar = 100 µm. (B) Severe chronic keratitis characterized by marked thickening and keratinization of the epithelium, and fibrosis and neovascularization of the stroma. Bar = 200 µm.
Uvea
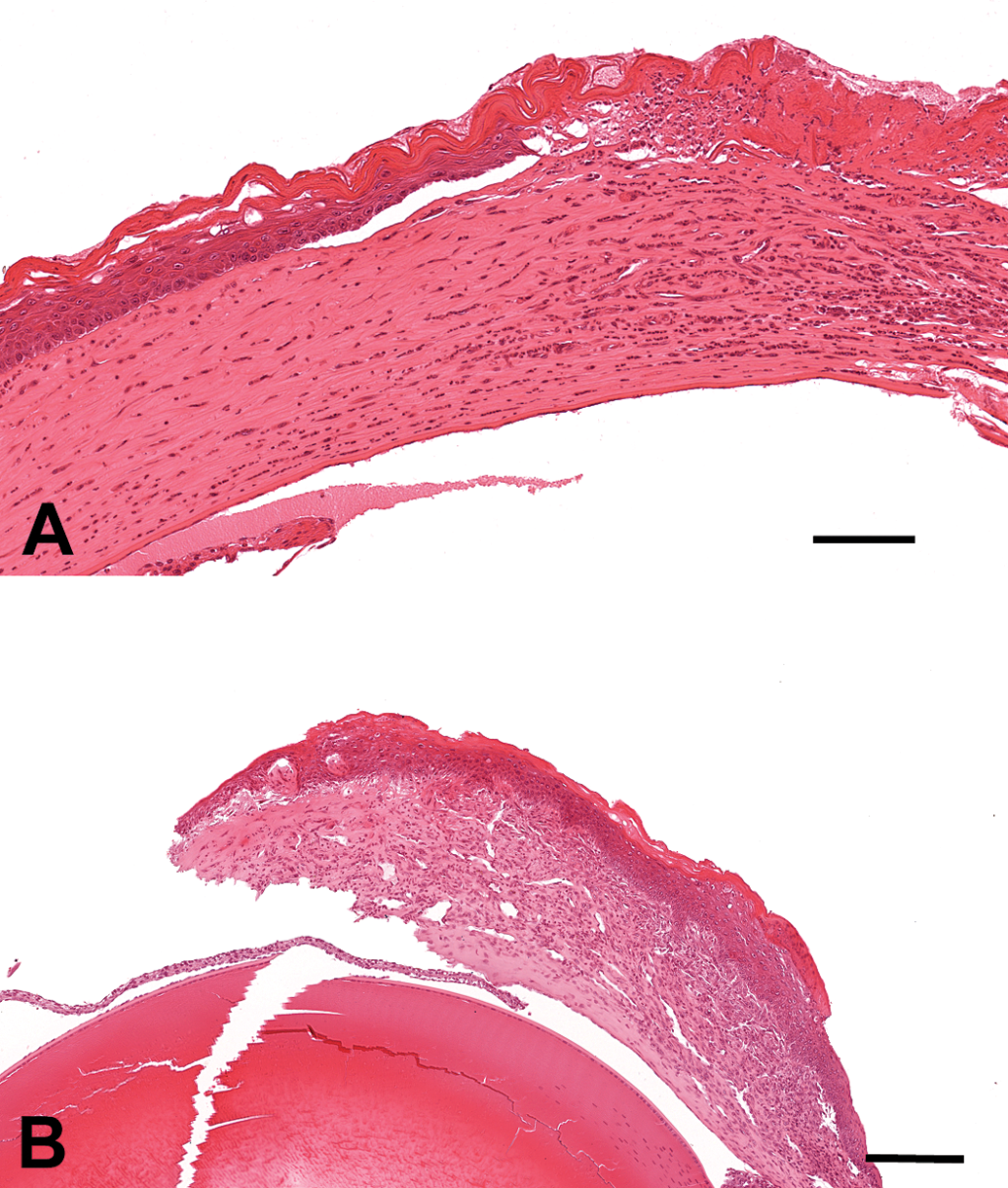
Only 2 lesions (mineral deposits in the iris and anterior uveitis) affecting the anterior uvea (iris and ciliary body) were observed, and no lesions affecting the posterior uvea (choroid) were recorded. Mineral deposition in the iris was the most common lesion recorded and was observed only in animals from the 104-week studies. Mineral deposits were present as basophilic concentric extracellular granules expanding the iris and were not associated with inflammation or other lesions (Figure 2A). Anterior uveitis was the second most common lesion and was observed only in animals from the 80- and 104-week studies. Most cases of anterior uveitis were fibrinosuppurative (Figure 2B). In severe cases, there were adhesions of the iris to the corneal endothelium or lens (anterior and posterior synechia), and fibrin and inflammatory cells were observed in the anterior and posterior chamber.
Histopathology of the anterior uvea of CD-1 mice (H&E). (A) Mineral deposits expanding the iris. Bar = 50 µm. (B) Anterior uveitis characterized by infiltration of iris and anterior chamber by neutrophils. Bar = 100 µm.
Lens
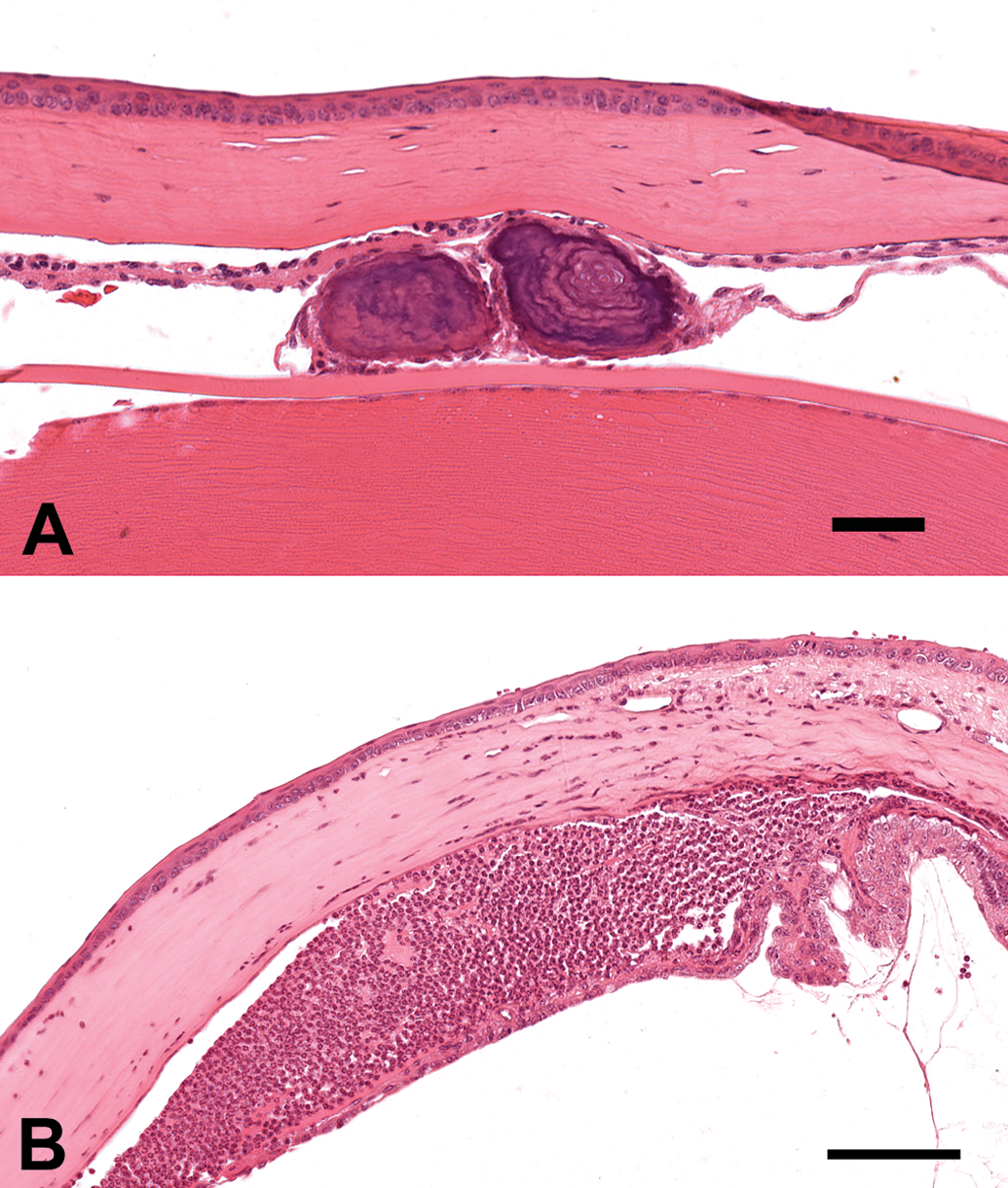
Cataract was the only lesion observed in the lens, and it was only observed in animals from the 80- and 104-week studies. Cataracts were characterized by variable degrees of lens epithelial cell proliferation (Figure 3A) or swelling (bladder cells), and anterior and posterior lens fiber fragmentation or vacuolation (Figure 3B). Severe cases of lens degeneration were often associated with other lesions such as ruptured lens and foreign bodies (Figure 3B), panophthalmitis, retinal detachment, keratitis, and uveitis. Lens epithelial cell proliferation, without fibrous metaplasia or other histomorphological features characteristic of cataracts, was observed in 3 animals (Figure 3A).
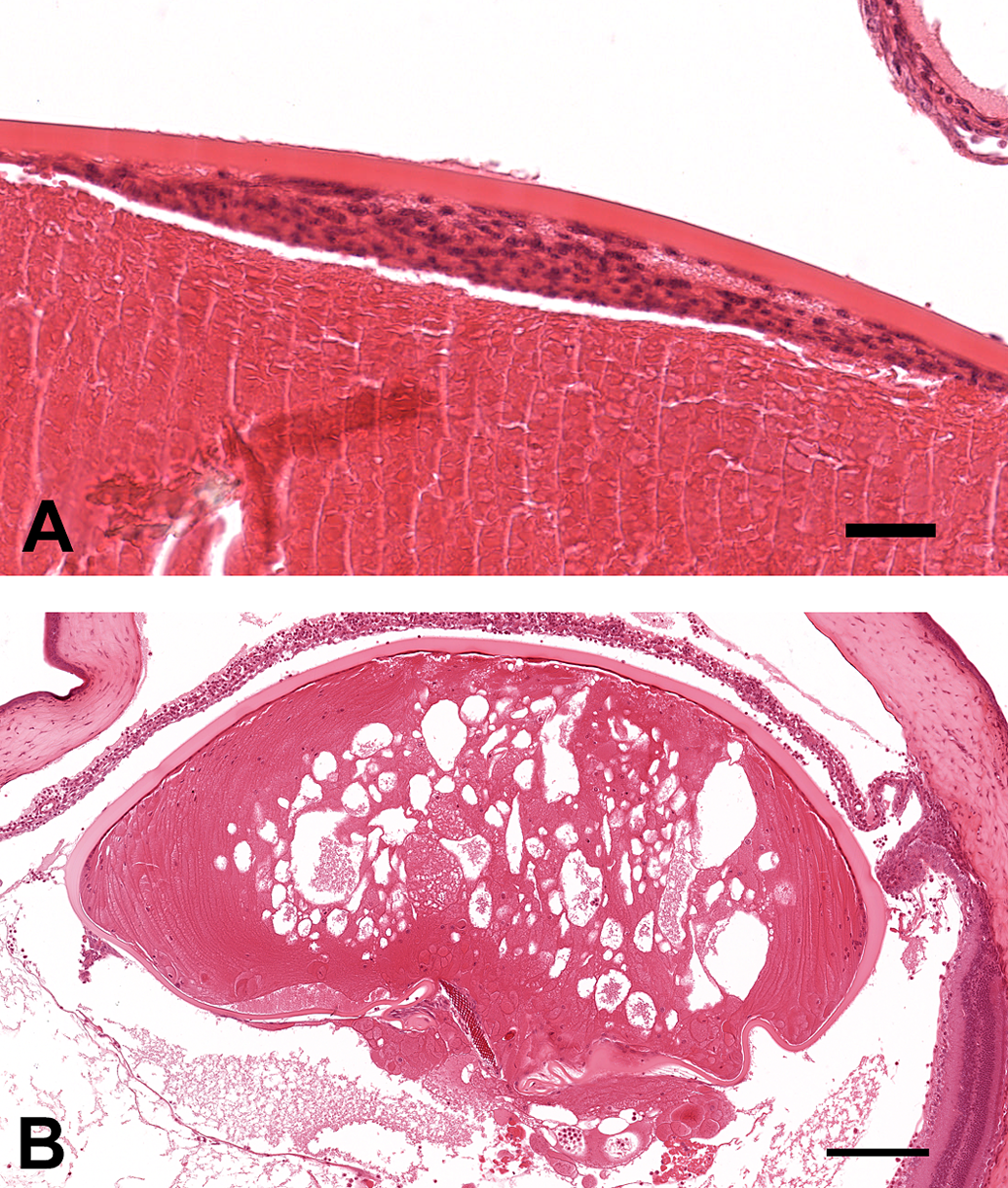
Histopathology of the lens of CD-1 mice (H&E). (A) Lens epithelium proliferation without fibrous metaplasia. Bar = 50 µm. (B) Cataract with lens rupture and foreign material. Bar = 200 µm.
Retina
The most common retinal lesion was retinal degeneration. Minimal to mild retinal degeneration was characterized by reduction in the outer layers of the retina (outer nuclear and outer plexiform layer). Moderate to marked lesions were characterized by complete loss of the outer nuclear layer and reduction of the inner layers (inner plexiform and inner nuclear layer) of the retina. Retinal degeneration was recorded in all age-groups, but the incidence was higher in animals from the 104-week studies compared to animals from other age-groups. In most cases, retinal degeneration was bilateral and was more prominent in the central retina than the peripheral retina. There was no difference in the incidence of retinal degeneration in males and females. There was an age-related increase in the severity of retinal degeneration. Most cases of retinal degeneration in mice from 4- and 13-week studies were graded as minimal (Figure 4B) or mild, and in 80- and 104-week studies, most cases were graded as moderate (Figure 4C) or marked (Figure 4D). There was a low incidence of other retinal lesions recorded across all the groups. These included retinal detachment, retinal dysplasia, and retinal coloboma. Retinal detachment was always found in association with lesions affecting other parts of the eye.
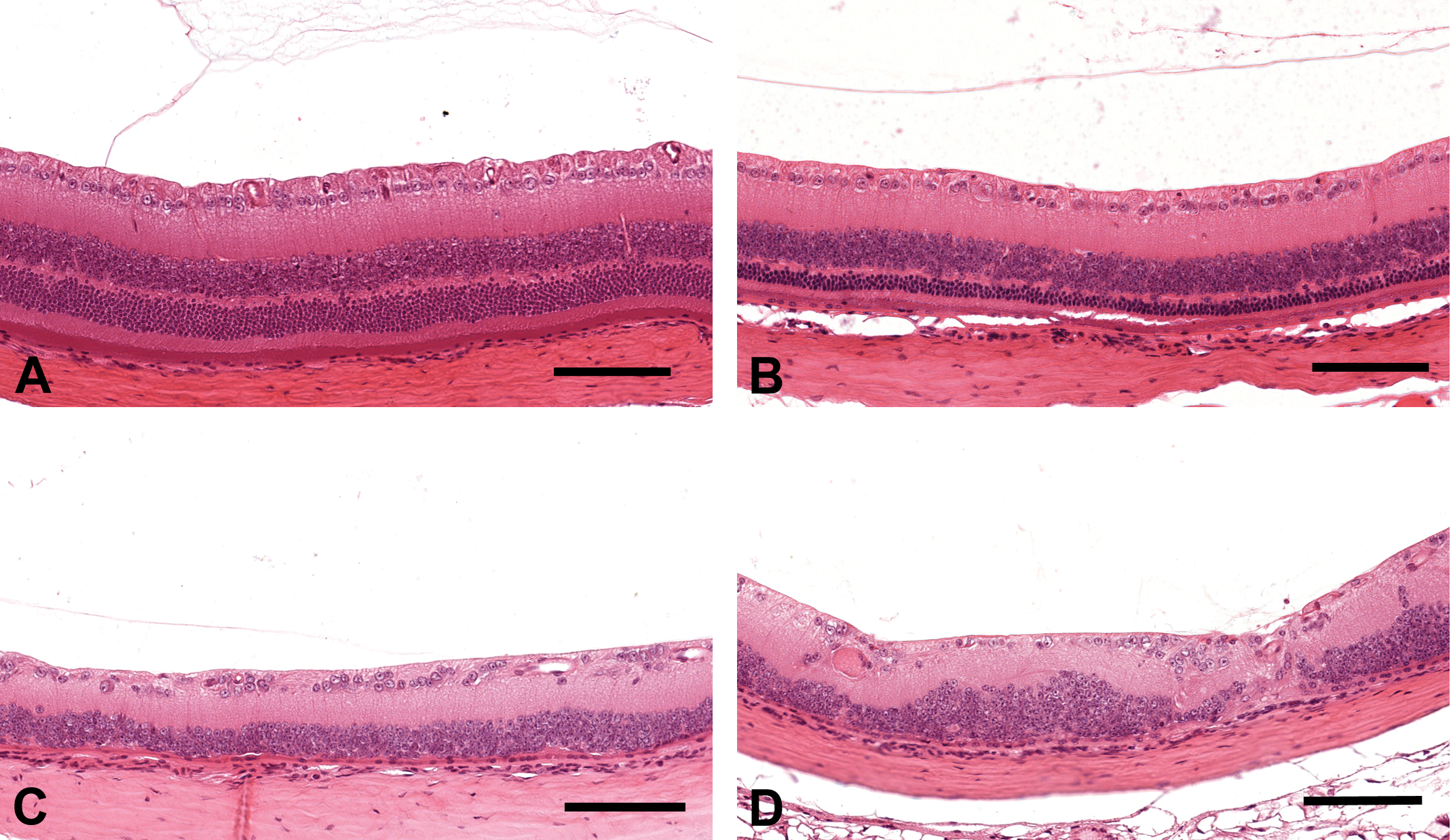
Histopathology of the central retina of CD-1 mice (H&E). (A) Normal central retina. (B) Minimal retinal degeneration characterized by reduction of the outer layer of the retina. (C) Moderate retinal degeneration characterized by complete loss of the outer nuclear layer. (D) Marked retinal degeneration characterized by complete loss of the outer nuclear layer and multifocal loss of inner nuclear layer. Bars = 100 µm.
Whole Globe
Panophthalmitis and phthisis bulbi were recorded in a few animals from the 80- and 104-week studies. These lesions were most likely a result of trauma produced by orbital sinus blood sampling.
Discussion
The eye is an important organ in rodent toxicology and carcinogenicity studies. The CD-1 mouse is one of the most commonly used mice strains in preclinical toxicology studies. The aim of this study was to determine the incidences of spontaneous findings affecting the eye in Crl:CD-1(ICR)BR mice used in chronic preclinical toxicology studies. There are few reports that describe the incidence and morphology of eye lesions found in rodents (Frame and Slone 1996; Taradach and Greaves 1984). This report presents up-to-date results of incidences and range of findings in Crl:CD-1(ICR)BR mice and can serve as a historical control reference for use in correspondence with regulatory authorities.
Lesions of the eye were uncommon in 4- and 13-week studies but were seen with a higher incidence in 80- and 104-week studies. The incidences of the lesions were similar in males and females. No neoplastic lesions were observed. Primary neoplastic lesions of the eye are rare in mice with only one ocular melanoma reported in B6C3F1 mice (Ward et al. 1979).
Keratitis was the most common lesion of the cornea. Keratitis can be caused by infectious agents. It can also develop secondary to corneal trauma or corneal drying. Corneal drying can occur in moribund animals or in animals anesthetized during orbital sinus blood sampling. Corneal drying can also develop secondary to loss of lacrimal and Harderian gland function. Keratitis has been observed in mice with Harderian gland neoplasms (Sheldon and Greenman 1980). Neoplasms of the Harderian gland can cause protrusion of the eye and proptosis of the eyeball, resulting in drying of the cornea and exposure keratitis (Carlton and Render 1991a). Mice are highly resistant to corneal infection and rarely develop spontaneous bacterial keratitis without physical disruption of the corneal epithelium (Klocke et al. 2011).
Mineral deposits in the corneal stroma were observed only in animals from 104-week studies. Mineral deposits in the corneal stroma generally occur after trauma or inflammation of the cornea (Carlton and Render 1991b); however, in this study, some deposits were not associated with corneal inflammation, ulceration, or vascularization, suggesting it may be a primary change. Spontaneous corneal mineralization has been previously reported in CD-1, CF1, C3H, DBA/2, CD2F1, and BALB/c mice (Sheldon and Greenman 1980; Van Winkle and Balk 1986), and is the most frequently reported microscopic lesion associated with corneal opacity in mice (Van Winkle and Balk 1986). Corneal mineralization has also been related to the frequency of cage cleaning and the ammonia levels in the cage (Van Winkle and Balk 1986).
Mineral deposition in the iris was the most common lesion affecting the anterior uvea. This change was not associated with inflammation or other lesions, suggesting that it is a primary change. To our knowledge, there are no previous reports of mineral deposits in the iris in this strain of mice. Anterior uveitis (inflammation of the iris and ciliary body) was the second most common lesion of the anterior uvea. Anterior uveitis can originate from the iris or ciliary body or can be secondary to corneal perforation. Most cases of anterior uveitis were not associated with perforation of the cornea or keratitis, and no intralesional bacterial colonies were observed.
The incidence of cataracts increased with age, and the incidence was relatively high compared to other lesions. This agrees with previously reported incidences, for example, a 25% incidence of cataracts in CD-1 mice by the age of 18 months (Taradach and Greaves 1984). Cataracts usually occur following trauma or inflammation of other parts of the eye, but can also occur as an inherited condition in several strains of mice (Peiffer 1991). It is rarely possible to give an etiological diagnosis of cataract by histopathology evaluation alone. Lens epithelial cell proliferation without fibrous metaplasia was observed in 3 animals. There are reports of similar proliferative plaques occurring in the lens of transgenic mice (Lovicu et al. 2002).
Retinal degeneration was observed in all age-groups. However, there was an age-related increase in the incidence and severity. Spontaneous age-related retinal degeneration occurs in many strains of mice and differs among strains due to genetic background (Danciger et al. 2007; Frame and Slone 1996). At Charles River Edinburgh, prestudy indirect ophthalmoscopic examinations in CD-1 mice have revealed a high incidence of retinal degeneration (confirmed by histopathology) in some particular stocks of mice (unpublished data). This suggests that retinal degeneration can occur as an early acquired lesion, and it is highly recommended that prestudy ophthalmoscopic screening be performed on CD-1 mice. The age-related increase in the severity and microscopic morphology of retinal degeneration suggests that this lesion is progressive, starting with loss of outer retinal layers followed by loss of inner nuclear layers. In the albino mice, retinal degeneration can also be induced by light, and different inbred strains of mice have a wide range of sensitivities to constant light exposure (LaVail, Gorrin, and Repaci 1987). However, in one study, light did not play a direct role in the progression of the retinal degeneration in Crl:CD-1(ICR)BR mice (Serfilippi et al. 2004). The microscopic morphology of spontaneous retinal degeneration seen in this study is similar to light-induced retinal disease; therefore, it is difficult to assess the relative contributions of age and light when considering the etiology of retinal degeneration. The ophthalmoscopic appearance and microscopic morphology of spontaneous retinal degeneration is similar to some compound-induced retinal degenerations (reviewed by Frame and Carlton 1991), and this may complicate interpretation in toxicology studies. However, reference to historical control incidences such as those presented in this study may assist in this interpretation.
In conclusion, spontaneous lesions affecting the eye of CD-1 mice are rare in 4- and 13-week studies, uncommon in 80-week studies, and relatively higher in 104-week studies. These lesions may complicate toxicology studies and must therefore be considered in long-term experiments involving CD-1 mice.
Footnotes
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
The author(s) received no financial support for the research, authorship, and/or publication of this article.
