Abstract
The incidence and range of spontaneous microscopic lesions were determined in the eyes of male and female control Sprague-Dawley and Han Wistar rats. Data were collected retrospectively from 1411, 817, 970, 658, and 3999 rats from control groups of 4-, 13-, 26-, 52-, and 104-week studies, respectively, carried out between 1997 and 2019. Microscopic lesions of the eye were rare in 4- and 13-week studies, uncommon in 26- and 52-week studies, and were of relatively higher incidence in 104-week studies. Neoplastic lesions were sporadic and were only observed in 104-week studies. In Sprague-Dawley rats, the most common lesions (>1% in 104-week studies) were retinal degeneration, retinal rosettes/folds, and lenticular degeneration. The Han Wistar rats presented a range of ocular lesions similar to the Sprague-Dawley rats. However, retinal degeneration occurred with an earlier onset and at higher incidences, ranging from >5% in 26-week studies up to 45.72% in 104-week studies. In both strains, females exhibited higher incidences and severities of retinal degeneration. It is hoped that reference to the incidences reported here will facilitate the differentiation of spontaneous lesions from test article–induced lesions in toxicology studies in these strains of rat.
Introduction
To assess the potential ocular toxicity of test articles, it is essential for the pathologist to be familiar with spontaneous lesions that may occur in the eyes of the laboratory animals routinely utilized in safety assessment studies. Sprague-Dawley (SD) and Han Wistar (HW) rats are 2 of the most commonly used rat strains in preclinical toxicology studies, but few publications address the incidence and morphology of spontaneous eye lesions in rodents. 1 -5 Spontaneous microscopic lesions of the eye, especially retinal degeneration, are common in long-term toxicity studies in laboratory rats. The incidence of these spontaneous lesions varies widely depending on a number of factors including strain, age, diet, gender, and management practices among others. Despite their widespread use for safety studies, there seems to be a paucity of information on the incidences of spontaneous microscopic changes in the eyes of SD 1,6 and HW rats. 7 Published literature with background data can help the pathologist to differentiate background pathology from test article–related lesions
In this article, data from control SD rats and HW rats of various age groups from nonocular toxicology and carcinogenicity studies carried out at Covance Huntingdon and Eye laboratories are presented. Additionally, the incidence and severity of spontaneous ocular microscopic lesions are discussed and compared between SD and HW rats.
Materials and Methods
The details of the studies from which these data were obtained are presented in Table 1 and Table 2. This report is based on eye samples from a total of 4110 SD rats (521 from 4-week, 515 from 13-week, 504 from 26-week, 320 from 52-week, and 2250 from 104-week studies) and 3744 HW rats (889 from 4-week, 302 from 13-week, 466 from 26-week, 338 from 52-week, and 1749 from 104-week studies) obtained from control groups of preclinical toxicological studies carried out between 1997 and 2019 at Covance Huntingdon and Eye. Crl: CD(SD) rats were obtained exclusively from Charles River UK. The majority (approximately 85%) of HW rats were obtained from Envigo RMS/Harlan UK, with approximately 15% sourced from Charles River UK. All the data presented here were obtained from control group animals studied in Good Laboratory Practice compliant preclinical toxicity studies. Prestudy indirect ophthalmoscopic examinations were done on all animals.
Details of Data Sources for Sprague-Dawley Rats.
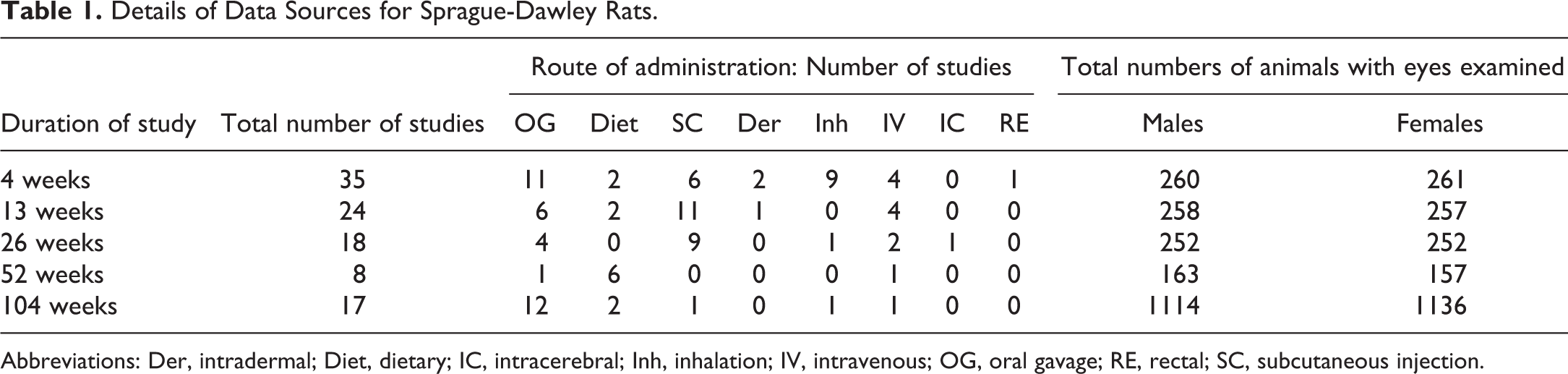
Abbreviations: Der, intradermal; Diet, dietary; IC, intracerebral; Inh, inhalation; IV, intravenous; OG, oral gavage; RE, rectal; SC, subcutaneous injection.
Details of Data Sources for Han Wistar Rats.
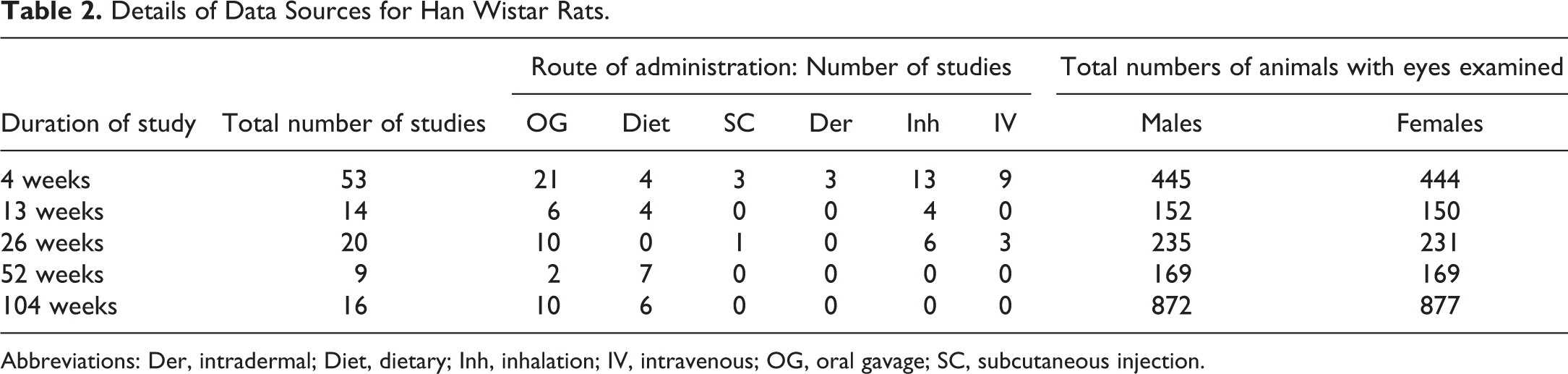
Abbreviations: Der, intradermal; Diet, dietary; Inh, inhalation; IV, intravenous; OG, oral gavage; SC, subcutaneous injection.
Control animals were dosed with commonly used vehicles (eg, methylcellulose, corn oil, sterile 0.9% sodium chloride, lactose, and air) which are considered to have no effect on the occurrence of eye lesions. For the 13-week studies, control groups comprised 6 to 25 SD or 9 to 20 HW rats per sex. For 26-week studies, control groups comprised 4 to 38 SD or 7 to 20 WH rats per sex. For the 52-week studies, control groups comprised of 12 to 20 SD or HW rats per sex, and for the 104-week studies, control groups comprised at least 60 SD or 50 HW rats per sex. All husbandry procedures including light intensity and cage rotation were similar between SD and HW studies. Animals of the same sex were housed 4 per cage in Association for Assesment and Accreditation of Laboratory Animal Care-accredited facilities. Animal room temperature and humidity were automatically controlled at 19 °C to 25 °C and 40% to 70%, respectively, and there was a supply of filtered, not recirculated, air. An automatic 12-hour light/dark cycle was maintained. Animals had free access to potable water from the public supply in bottles with sipper tubes and were fed an ad libitum commercial rodent diet. Aspen Chew Blocks (soft white untreated wood blocks) and a plastic shelter were offered to all animals for environmental enrichment.
The in-life experimental procedures to be undertaken during the course of these studies were subject to the provisions of the United Kingdom Animals (Scientific Procedures) Act 1986 Amendment Regulations 2012 (the Act), which conforms to the European Convention for the Protection of Vertebrate Animals used for experimental and other scientific purposes (Strasbourg, Council of Europe). The number of animals used was the minimum that is consistent with scientific integrity and regulatory acceptability, consideration having been given to the welfare of individual animals in terms of the number, and extent of procedures to be carried out on each animal.
Results
The range and incidence of the microscopic ocular lesions encountered in control SD rats and HW rats from 4-, 13-, 26-, 52-, and 104-week studies are presented in Table 3 and Table 4, respectively. In both SD and HW rats, the most common lesions were retinal degeneration and lens degeneration with an age-related increase in incidence. Congenital retinal rosettes and folds were infrequent in both SD and HW rats. Neoplastic lesions were very rare and only seen in 104-week studies. Other lesions were almost exclusively observed in animals from 52- and 104-week at a very low incidence (<1% for all).
Incidences (%) of Microscopic Findings of the Eye in Sprague-Dawley (CD) Rats.
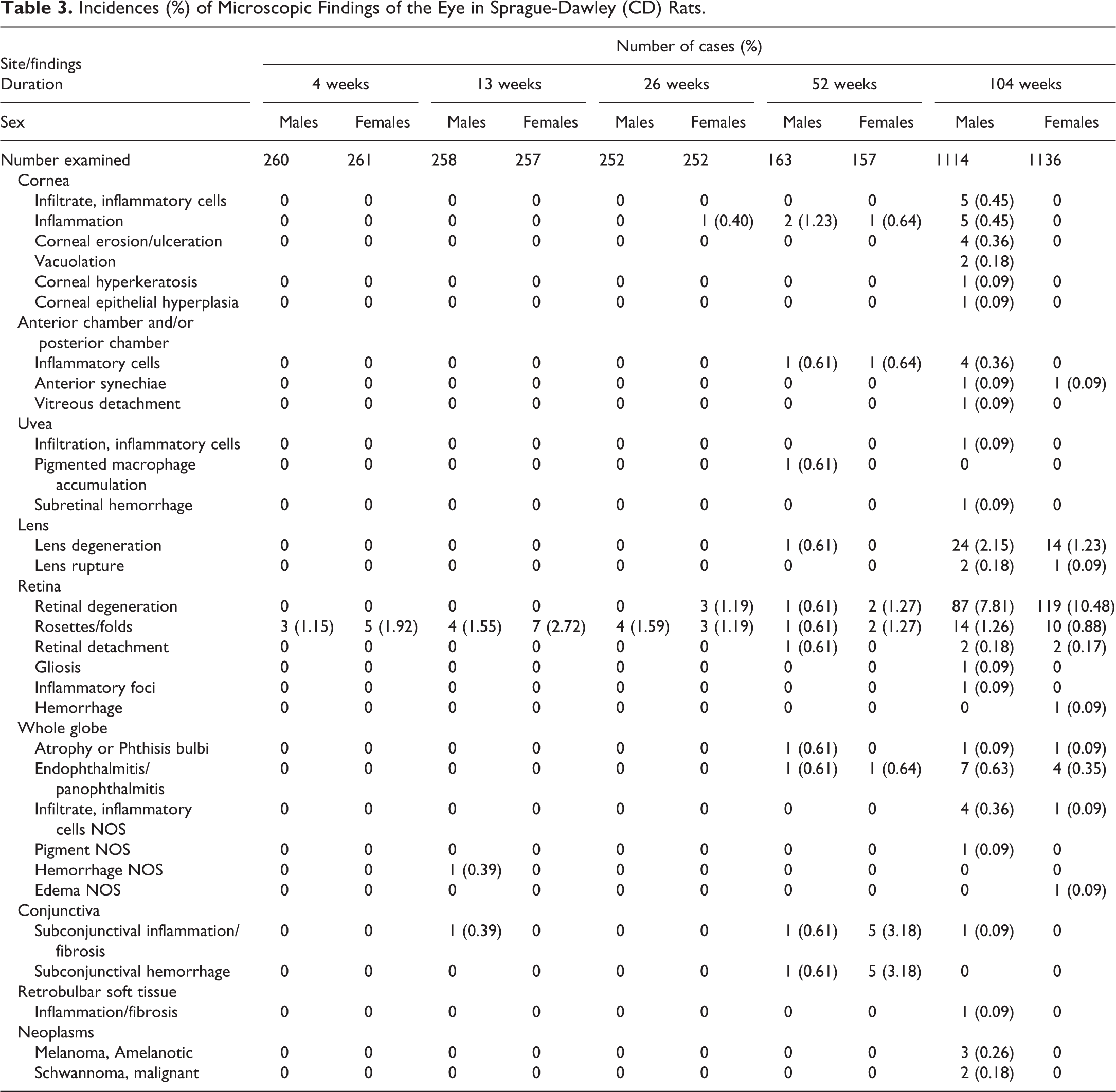
Incidences (%) of Microscopic Findings of the Eye in Han Wistar Rats.
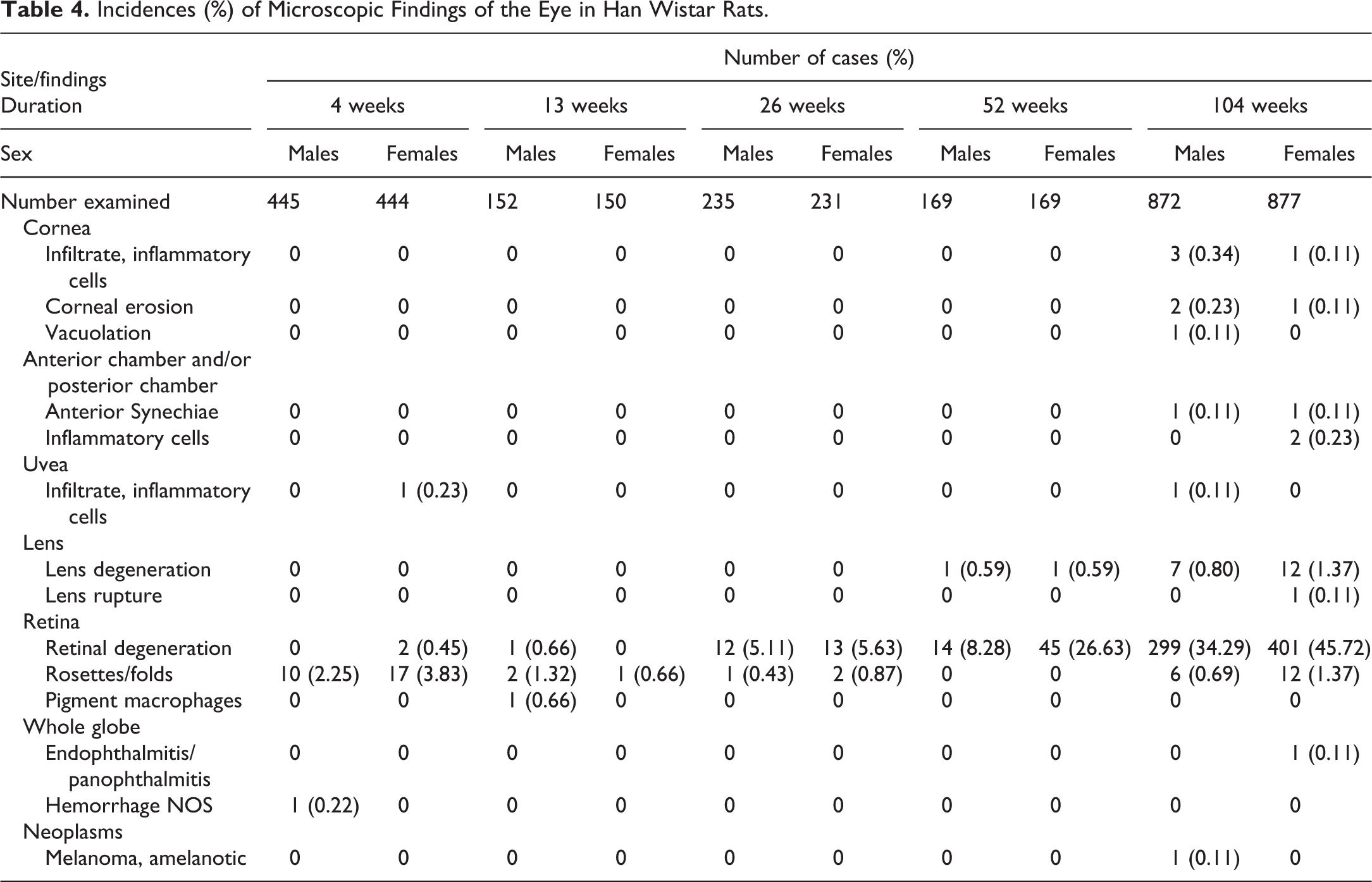
Nonneoplastic Lesions
Cornea
Lesions of inflammatory nature were the most common corneal lesions seen in SD rats and were seen in 26-, 52-, and 104-week studies. In 104-week studies, inflammatory cell infiltrate (Figure 1) was seen at the same incidence as inflammation, followed by corneal erosion/ulceration (Figure 2), vacuolation, hyperkeratosis, and epithelial hyperplasia. There was a difference between sexes in the incidence of corneal lesions in 104-week studies, with no record of lesions in females.
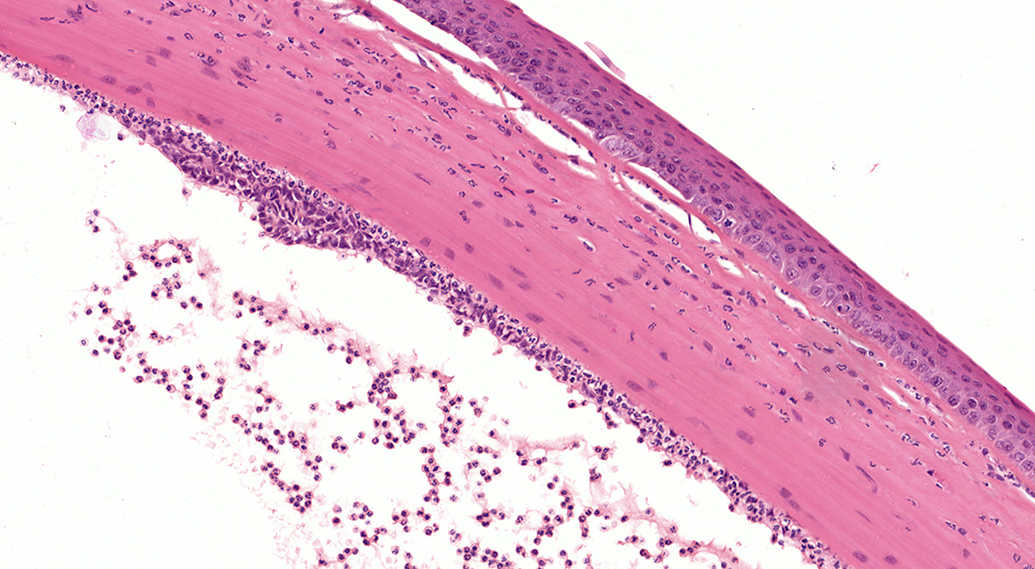
Inflammatory cell infiltrate in the cornea and the anterior chamber from a Sprague-Dawley (SD) rat (hematoxylin and eosin, H&E). Small numbers of neutrophils infiltrate the outer corneal stroma and accumulate within the anterior chamber and under the corneal endothelium. The corneal epithelium is minimally hyperplastic. Neutrophils in the anterior chamber are admixed with fibrin. Focally, the corneal endothelium is hyperplastic. Original scan ×20.
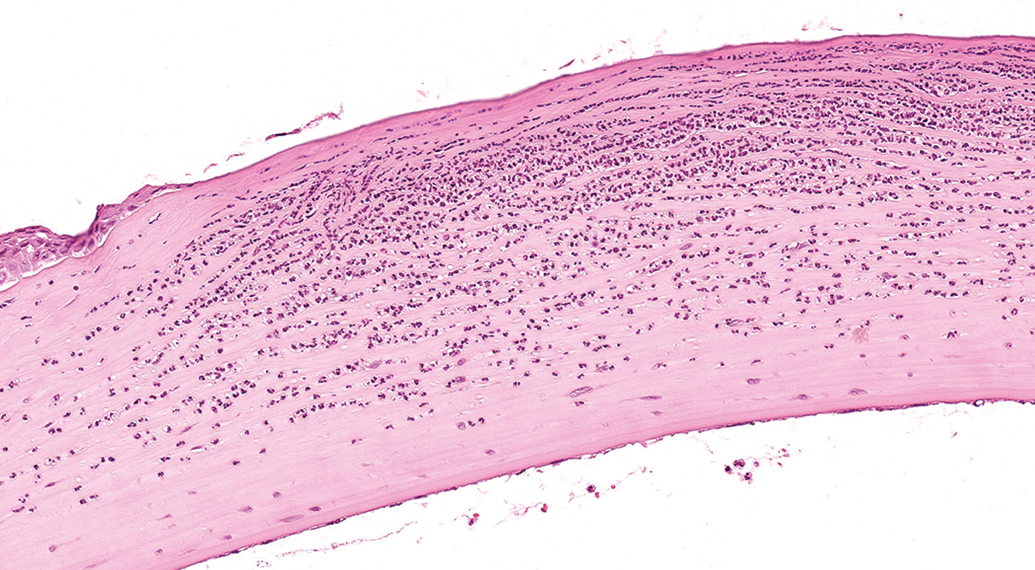
Corneal erosion from a Han Wistar (HW) rat (hematoxylin and eosin, H&E). In a locally extensive area, the corneal stroma lacks corneal epithelium. Below the eroded corneal surface, large numbers of degenerate neutrophils separate and replace the stromal keratinocytes. Original scan ×20.
Corneal lesions were occasionally seen in HW rats from 104-week studies only. The most common finding was inflammatory cell infiltrate with a minimally higher incidence in males than females. Other lesions included corneal erosion and vacuolation.
Uvea
Uveal lesions were generally seen at a low incidence in SD rats in 52-week (accumulation of pigmented macrophages) and 104-week studies (inflammatory cell infiltrate and subretinal hemorrhage).
From all studies examined, only one female HW rat from a 4-week study and one male HW rat from a 104-week study exhibited a lesion (inflammatory cell infiltrate) affecting the uvea.
Lens
Lens (fiber) degeneration (cataract; Figure 3) was the predominant finding in the lens and was noted in both strains, predominantly in 104-week studies. In 52-week studies, lens degeneration was seen in 1 SD male, 1 HW male, and 1 HW female. For 104-week studies, the incidence was 2.15% in SD males, 1.23% in SD females, 0.8% in HW males, and 1.37% in HW females. Lens (capsule) rupture was less common and occurred only in 104-week studies in both strains.
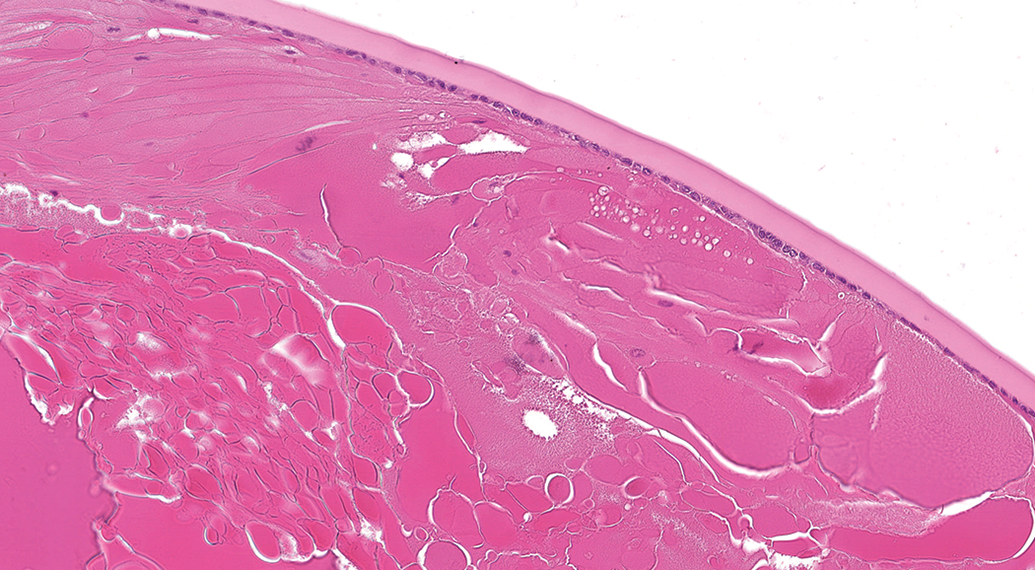
Lens degeneration in a Sprague-Dawley (SD) rat (hematoxylin and eosin, H&E). The lens fibers are swollen or replaced by released lens protein forming spherical droplets (Morgagnian globules). Original scan ×20.
Retina
In SD rats, retinal degeneration (Table 5, Figure 4) was the most common eye lesion recorded, particularly in 104-week studies, where the incidence was highest (7.81% in males and 10.48% in females). In 4-week and 13-week studies, retinal degeneration was not recorded; whereas, in 26- and 52-week studies it was seen at low incidence, predominantly in females. Incidence and severity of retinal degeneration increased with study duration, indicating a strong correlation with age, and a greater incidence and severity in females. Retinal rosettes/folds was the second most common change seen in SD rats and it was recorded across all study durations. Retinal detachment was seen at low incidence in both 52- and 104-week studies. Gliosis, inflammatory cell infiltrate, and hemorrhage were seen only in 104-week studies, at low incidences.
Incidence (%) and Severity of Retinal Degeneration in Sprague-Dawley Rats.
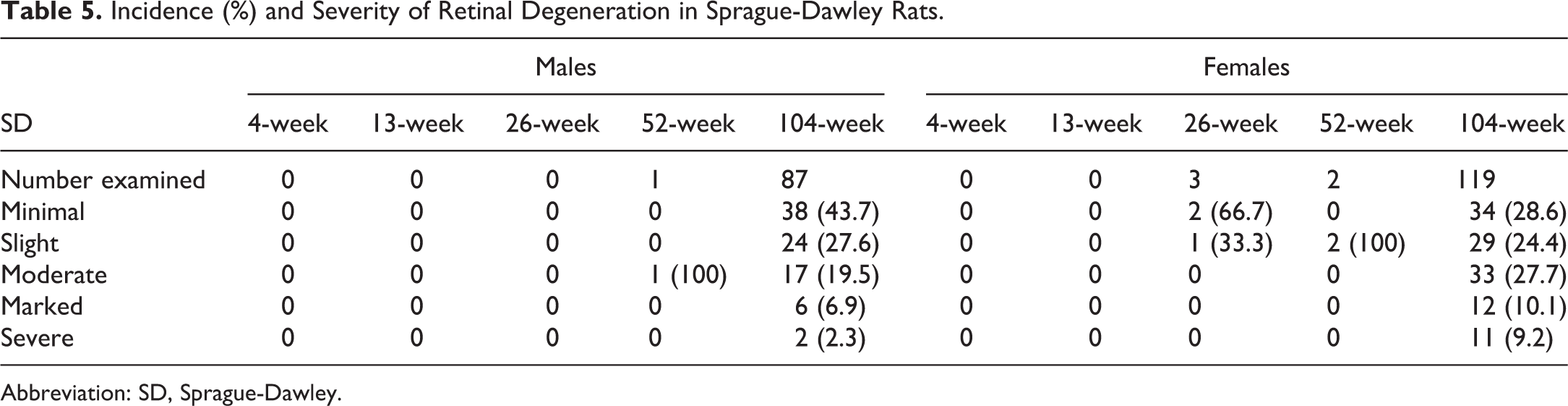
Abbreviation: SD, Sprague-Dawley.
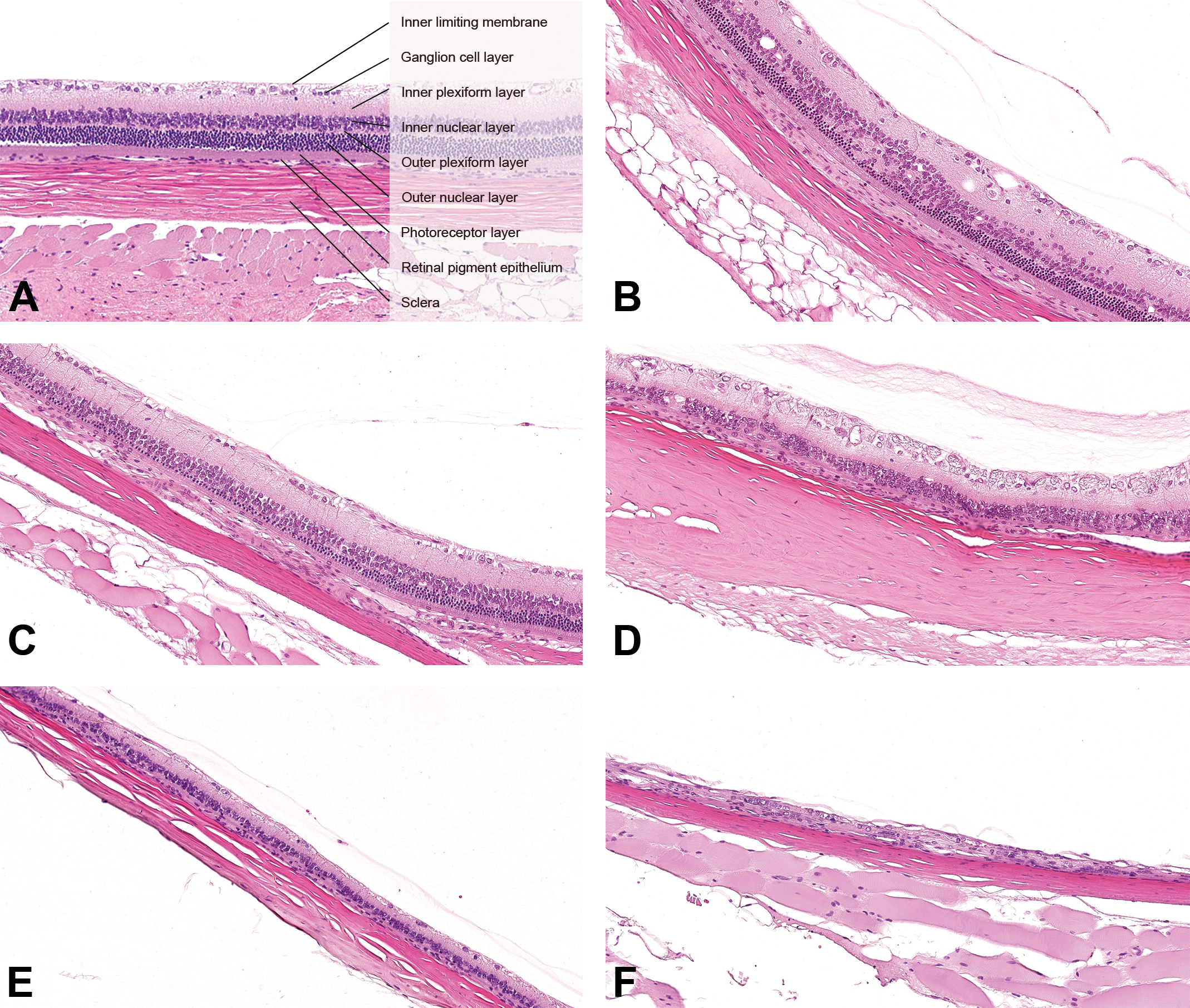
Retinas of Sprague-Dawley (SD) rats and Han Wistar (HW) rats (hematoxylin and eosin, H&E). (A) Normal retina. Original scan ×20. (B) Minimal retinal degeneration. Focally, the outer nuclear layer is reduced in thickness and the overlying outer plexiform layer is poorly demarcated. Original scan ×20. (C) Slight retinal degeneration. In a locally extensive area, the outer plexiform layer is inconspicuous and the outer nuclear layer and the photoreceptor layer are both reduced in thickness. Original scan ×20. (D) Moderate retinal degeneration. Diffusely, the outer plexiform layer, the outer nuclear layer, and the photoreceptor layer are lost. The inner nuclear layer is irregular in thickness. Original scan ×20. (E) Marked retinal degeneration. Diffusely, the outer plexiform layer, the outer nuclear layer, and the photoreceptor layer are lost. The inner nuclear layer and the inner plexiform layer are reduced in thickness. Original scan ×20. (F) Severe retinal degeneration. Diffusely, the outer plexiform layer, the outer nuclear layer, the photoreceptor layer, the inner nuclear layer, and the inner plexiform layer are lost. Original scan ×20.
In HW rats, retinal degeneration was also the most common retinal lesion, with a higher incidence than in SD rats, and also showing a strong age relationship. It was present in only 2 females in the 4-week studies and in 1 male in the 13-week studies. In 26-week studies, retinal degeneration was seen at a similar incidence in both sexes (5.11% in males and 5.63% in females). A female predisposition was apparent in 52-week studies, with 26.62% females affected in comparison with 8.28% males, and this was confirmed in 104-week studies where 45.72% HW females were affected in comparison with 34.29% HW males. Although the majority of both males and females exhibited minimal retinal degeneration (Table 6, Figure 4B), the pathological process appeared to progress with age, with higher incidences of slight to severe retinal degeneration in longer studies. Severity of retinal degeneration had a tendency to be higher in females. At an early stage, degenerative changes were restricted to the outer retinal layers with photoreceptor loss and partial outer nuclear layer loss (Figure 4B and C). Progressively, in addition to the total loss of the outer retinal layers, there was a partial loss of the inner nuclear layer (Figure 4D and 4E). In the most severe cases, there was a total loss of the inner nuclear layer (Figure 4F).
Incidence (%) and Severity of Retinal Degeneration in Han Wistar Rats.
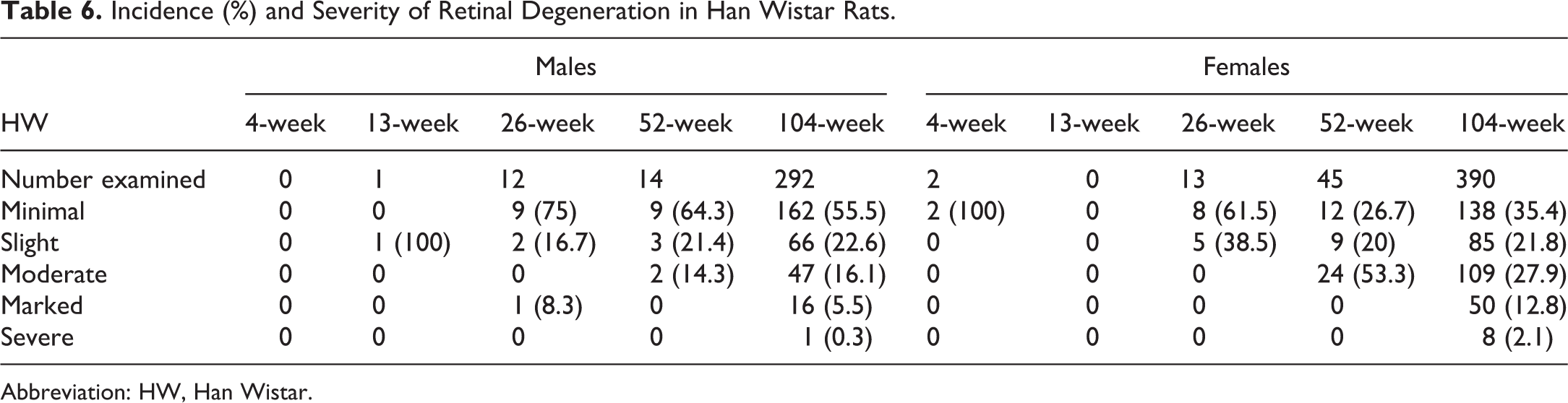
Abbreviation: HW, Han Wistar.
The second most common retinal lesion in HW rats was retinal rosettes (Figure 5) and folds, which were present at all durations with the exception of 52-week studies. When present, the incidence of retinal rosettes and folds was similar among groups, ranging from 0.43% to 3.83%. Pigmented macrophages were recorded in the retina of a single HW male from a 13-week study and likely represented hemosiderin accumulation after spontaneous retinal microhemorrhage. 8,9
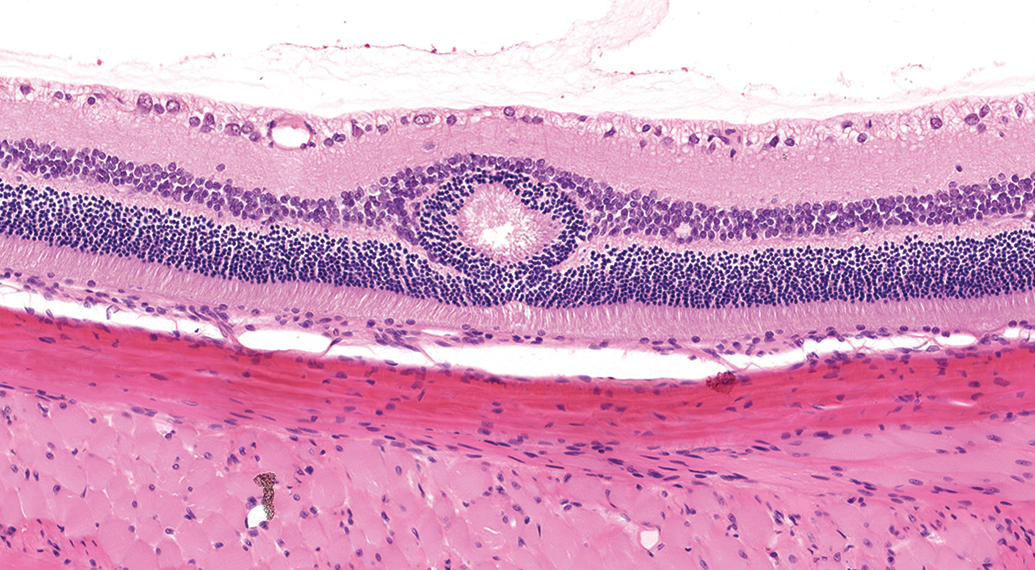
Retinal rosette from a Sprague-Dawley (SD) rat (hematoxylin and eosin, H&E). A focal rosette-like structure arising from the outer nuclear layer expands and distorts the inner and outer nuclear layers. Eosinophilic linear structures resembling photoreceptors inner segments in a radiate pattern are present within the center of the retinal rosette. Original scan ×20.
Whole globe
In SD rats, whole globe lesions were generally seen in 52- or 104-week studies. Endophthalmitis/panophthalmitis (Figure 6) was the most common whole globe change and was seen predominantly in 104-week studies, with isolated incidences in 1 male and 1 female on 52-week studies. A single incidence of hemorrhage (site unspecified) was recorded in a male from a 13-week study. Other lesions, such as atrophy/phthisis bulbi, inflammatory cell infiltrate, pigment, edema, were seen at low incidence in 52- and/or 104-week studies.
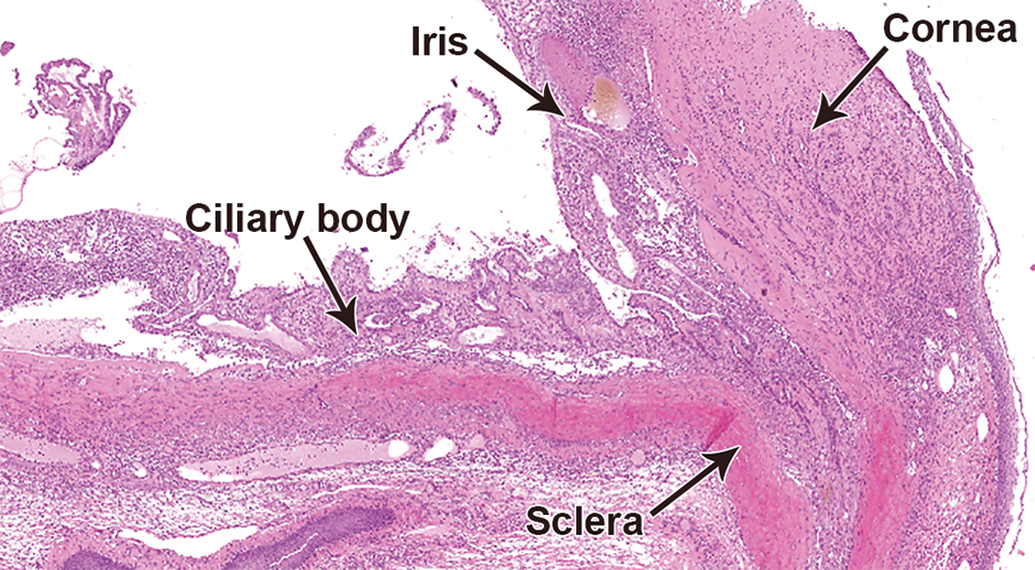
Panophthalmitis from a Han Wistar (HW) rat (hematoxylin and eosin, H&E). The corneal and uveal structures are profoundly distorted by florid mixed inflammatory cell infiltrate. Original scan ×5.
In HW rats, whole globe lesions were almost absent, with only one case of panophthalmitis in a single male from a 104-week study, and hemorrhage (site unspecified) in one male from a 4-week study.
Anterior and posterior chambers
Very few animals of either strain exhibited lesions affecting the anterior or posterior chamber. Isolated or very low incidences of anterior synechia and/or inflammatory cell infiltrates (Figure 1) were seen in both strains in 104-week studies, and in SD rats in 52-week studies.
Neoplastic lesions
Neoplastic lesions were only recorded in 104-week studies. The incidence of primary ocular neoplasms was low, and in both strains only males displayed tumors. Incidence was slightly higher in SD male rats, comprising amelanotic melanoma (0.26%; Figure 7) and malignant schwannoma (0.18%). In HW male rats, a single amelanotic melanoma was recorded.
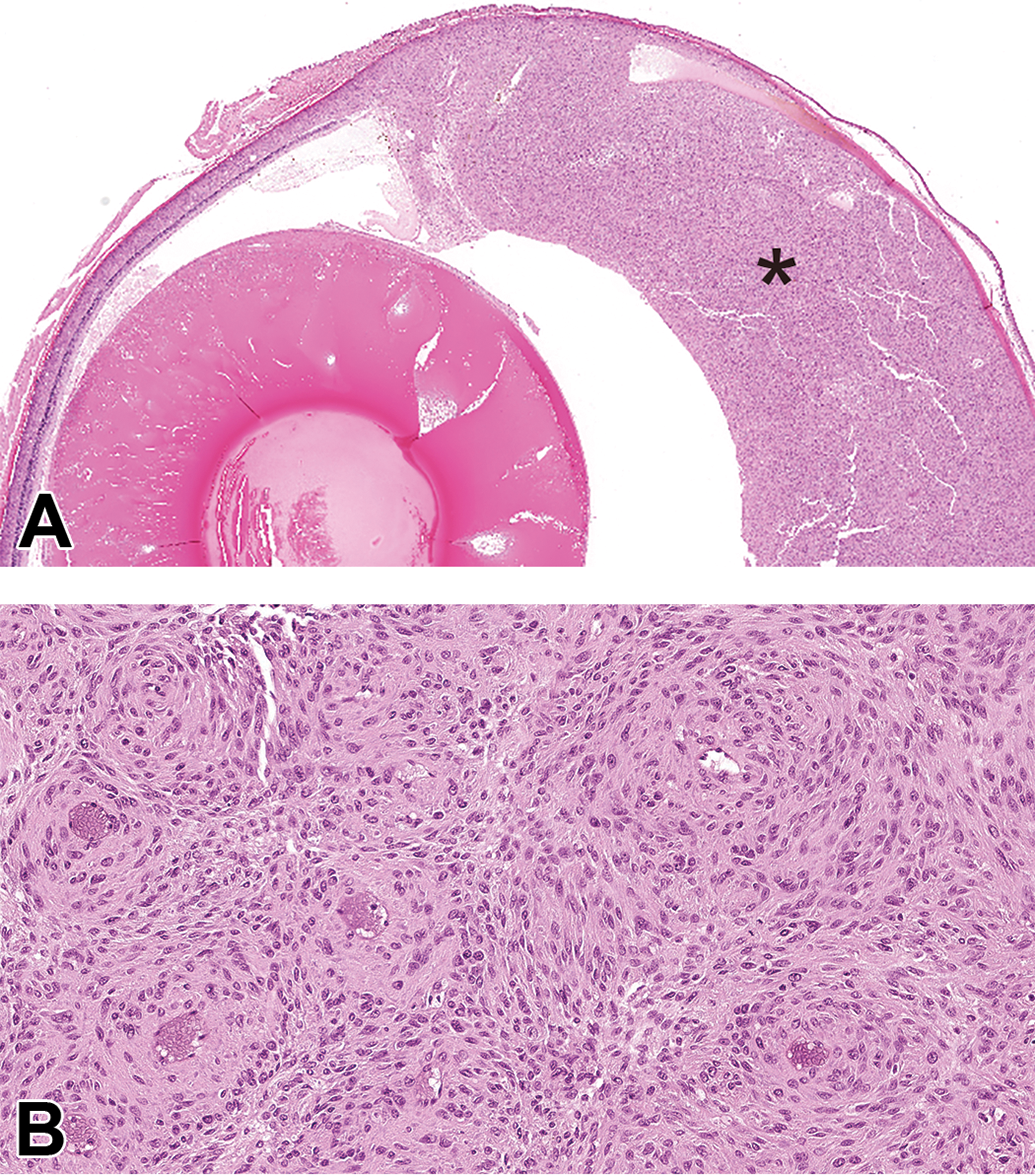
Amelanotic melanoma from a Han Wistar (HW) rat (hematoxylin and eosin, H&E). (A) An infiltrative, nonencapsulated and densely cellular neoplastic mass (black asterisk) expands and replaces the anterior uvea and the anterior ocular chamber. Original scan ×2. (B) Higher magnification of Figure 7A. The neoplastic spindle-shaped cells are arranged in short streams and perivascular whorls. Original scan ×20.
Discussion
Microscopic ocular lesions were uncommon in 4-, 13-, and 26-week studies but were of higher incidence in 52- and 104-week studies. The widest range of ocular lesions was recorded in 104-week studies. Retinal rosettes and folds were detected as early as 4 weeks in both rat strains and presented a relatively constant incidence from 4- to 104-week studies, in accordance with the congenital origin of these lesions. Depending on the toxicologic pathologists’ practices, retinal rosettes and folds may not be consistently recorded. Inconsistent recording of these background lesions may result in underestimation of their incidences.
Retinal degeneration, also described as retinal atrophy in the International Harmonization of Nomenclature and Diagnostic Criteria (INHAND) guidelines, 10 was the most common spontaneous lesion in both HW rats and SD rats with the highest incidences in 104-week studies. Retinal atrophy is the result of a degenerative process in the retina leading to cell loss and collapse of the retinal cell layers. Microscopically, the retina is thinner, with focal to diffuse decreased cell density and loss of its layered architecture. The earliest lesions of retinal degeneration occurred in 4-week studies in HW rats, with 2 females affected. In 26-week studies, retinal degeneration was noted in female SD rats (1.19%) and in both sexes of HW rats (5.11% in males and 5.63% in females). This is a higher incidence than seen in HW rats in the literature. 11 Retinal changes increased in incidence and severity with age in both HW rats and SD rats. A female predisposition for retinal degeneration was apparent in 52-week studies in HW rats, and in 104-week studies in both HW rats and SD rats. Han Wistar rats showed an earlier onset and a higher incidence of retinal degeneration than SD rats in both sexes at all time points. In 104-week studies, both HW and SD female rats showed higher incidences of retinal degeneration than males, indicating a sex predisposition. A similar sex predisposition has been reported in the literature, 12 suggesting females are more susceptible to age-related or light-induced retinal degeneration. It has been reported that ovariectomized female rats are less sensitive to light-induced retinal damage than intact females and estrogen supplementation overcomes the protective effect of ovariectomy, 13,14 and this may explain the female predisposition to retinal atrophy.
Spontaneous retinal degeneration is considered to be multifactorial in laboratory rats, with a range of potential influences. Albino rats are more susceptible to age-related or light-induced retinal degeneration than pigmented strains. 15,16 Microscopically, light-induced retinal injury is not uniform, at least in the early stages, and affects firstly the central retina, especially the superior temporal region. 16 By contrast, age-related retinal degeneration is usually located in the peripheral region. 17 Age-related retinal injury is thought to be related to alterations of the retinal pigment epithelium and of the glia. 18,19 Since the study by Noell et al in 1966, 20 light-induced retinal degeneration has been extensively studied in most common laboratory rat strains. In preclinical studies, the distance between the cages and the light source may vary between animals or cages and can introduce a bias. Therefore, regular cage rotation is performed as a standard management practice to avoid this bias.
Interspecies and intraspecies differences in susceptibility to phototoxicity have been observed in laboratory mice and rats. 21,22 The high incidence of retinal degeneration in HW rats compared to SD rats shown in this report supports this observation and suggests that genetic factors are involved in the pathogenesis of retinal degeneration.
In HW rats, the high incidences of retinal degeneration in chronic preclinical toxicity studies, particularly in 52- and 104-week studies, can complicate interpretation of a drug-induced ocular finding. Therefore, if ocular toxicity is expected with a test item, use of the HW rat and HW-derived strains as animal models should be avoided if possible.
Incidences of primary ocular tumors in both SD and HW rats are rare 10 with melanomas being most frequently reported. 23,24 In this survey, the types of ocular tumors (melanoma, schwannoma) seen in both HW and SD rats, and their presence in males only, are consistent with the literature. 12
Although infrequent, drug-induced ocular changes can be caused by topical or systemic administration of a xenobiotic, directly or via the indirect action of a metabolite. A range of chemicals and pharmaceuticals can cause retinal damage, either by direct or indirect mechanisms, or by exacerbating spontaneous retinal lesions.
To identify and help interpret the cause of retinal damage, the laterality and location of retinal degeneration should be recorded by the study pathologist. Recording of whether a lesion is unilateral or bilateral provides invaluable information and should be done as standard practice. Unless administration is to one eye only, a unilateral change is highly unlikely to be test item linked. Distribution, whether focal or diffuse, can also indicate the pathogenesis of an ocular lesion. For example, focal retinal degeneration is more likely to be spontaneous, whereas diffuse changes to the retina are more suggestive of a drug-induced effect, and similarly with hyperplastic changes in the cornea. 25 In addition, topographic location (central, peripheral, or diffuse) and specification of the cell layer/s affected (inner retina, outer retina or global) can provide clues to the pathogenesis of retinal lesions. As mentioned earlier, although both affect the outer retina, age-related retinal degeneration is usually peripheral, unlike light-induced degeneration which typically affects the center of the retina. 10,16 Outer retinal degeneration is often secondary to photoreceptor cell toxicity or RPE toxicity, whereas inner retinal degeneration can be secondary to increased intraocular pressure, compression/degeneration of the optic nerve, or occasionally direct retinal toxicity. 10
The pathologist should also look for specific cytological and histological changes induced by the drug which may differentiate it from spontaneous degeneration. For example, vacuolation is not usually a significant feature of spontaneous retinopathies, but is often seen in drug toxicities due to cationic amphiphilic compounds, both in the retina and in other ocular structures including the cornea. To differentiate drug induced from spontaneous retinal degeneration, it is also essential to compare the incidence of the lesion in the study with background data at the laboratory, particularly in studies where there are no specifically test item-related features of retinal degeneration.
Conclusion
In conclusion, from the historical data of our laboratories, retinal degeneration was the most common spontaneous ocular microscopic finding in both SD rats and HW rats in chronic toxicity studies. In HW rats, retinal degeneration had an earlier onset and was of higher incidence in comparison with SD rats. In both rat strains, retinal degeneration showed a female predisposition with a higher incidence and severity.
Other ocular microscopic lesions were rare, and with the exception of retinal rosettes and folds, the incidences of ocular lesions increased with age. Primary ocular neoplasms were rare in both strains and comprised schwannomas and amelanotic melanomas. Ocular tumors were only recorded in males of both strains, with a slightly higher incidence in SD rats.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
