Abstract
We present the first documented acute bacterial sinus infection with Staphylococcus schleiferi in a 58-year-old male recovering from endoscopic sinus surgery recovering on postoperative oral corticosteroids. The patient reported, within 1 month of surgery, treating an outer ear infection in his dog that was culture positive for Staphylococcus schleiferi and Corynebacterium sp. and developing an acute exacerbation of his sinus symptoms with increased purulent drainage, facial pain, and increased aural fullness. Nasal endoscopy was notable for purulence and thick mucus in multiple sinuses, which was positive on culture for S. schleiferi. He underwent treatment with trimethoprim/sulfamethoxazole that resolved the active infection. S. schleiferi has shown only rare transmission to a human host in both immunocompetent and immunocompromised patients. Often, this bacterial pathogen will present as a skin infection or outer ear infection in canines and serves as the potential source of infection in humans as they treat their canine companions. This marks the first documented case of acute bacterial sinusitis caused by this bacterial pathogen in the human literature and warrants continued observation as another potential zoonotic pathogen that may cause sinus exacerbations in susceptible populations.
Introduction
Staphylococcus schleiferi is a coagulase-negative staphylococcus that rarely causes infection in humans, and it was first described by Freney et al. 1 Subsequent early reports have most often described S. schleiferi in the context of surgical site infections, most often impacting immunocompromised patient populations2,3 but more recent studies have raised concerns for the role of this pathogen in more severe infections. There are more recent reports of S. schleiferi as a causative organism in different clinical conditions, ranging from osteomyelitis of the vertebrae and extremities,4-6 endocarditis and disseminated bacteremia after pacemaker placement,7-9 pediatric meningitis, 10 and urosepsis. 11 A number of cases reported in the literature tended to involve animal contact, most commonly in the treatment of skin pustules or outer ear infections in canines by susceptible patients.10,12,13 We herein describe the first case of S. schleiferi acute bacterial rhinosinusitis in a postoperative endoscopic sinus surgery patient.
Case Presentation
The patient is a 58-year-old male who underwent an uncomplicated bilateral pan-sinus endoscopic sinus surgery for long-standing chronic rhinosinusitis with nasal polyposis that was unresponsive to multiple courses of oral steroids and antibiotics. His operative course was uneventful, and he was discharged with a prednisone taper given the presence of severe inflammation in the setting of nasal polyposis and a course of trimethoprim/sulfamethoxazole given the presence of preoperative Citrobacter koseri noted on preoperative cultures. There was still significant edema at his first postoperative debridement 12 days after surgery, and his prednisone course was subsequently extended for an additional week. Before his second postoperative appointment, close to a month after surgery, the patient sought veterinary care for otitis externa in his canine pet at home. During that appointment, a culture was performed that demonstrated pan-sensitive S. schleiferi and pan-sensitive Corynebacterium sp. within the dog’s aural drainage. The patient subsequently began topical treatments on his canine for this infection. During this time, the patient also noted worsening of his nasal symptoms with increased thick mucus, pain/pressure, and aural fullness (Figure 1). A culture was obtained which noted the growth of S. schleiferi that demonstrated some variations in the susceptibilities of that found in the canine otitis externa, but with the same underlying pathogen (Table 1). He was started again on an additional course of trimethoprim/sulfamethoxazole, and subsequent cultures were negative for S. schleiferi. The patient did have significant continued sinus edema despite treatment with topical steroid irrigations, oral steroids, and multiple antibiotic courses, leading to the initiation of dupilumab, which has more adequately controlled his sinonasal symptoms.
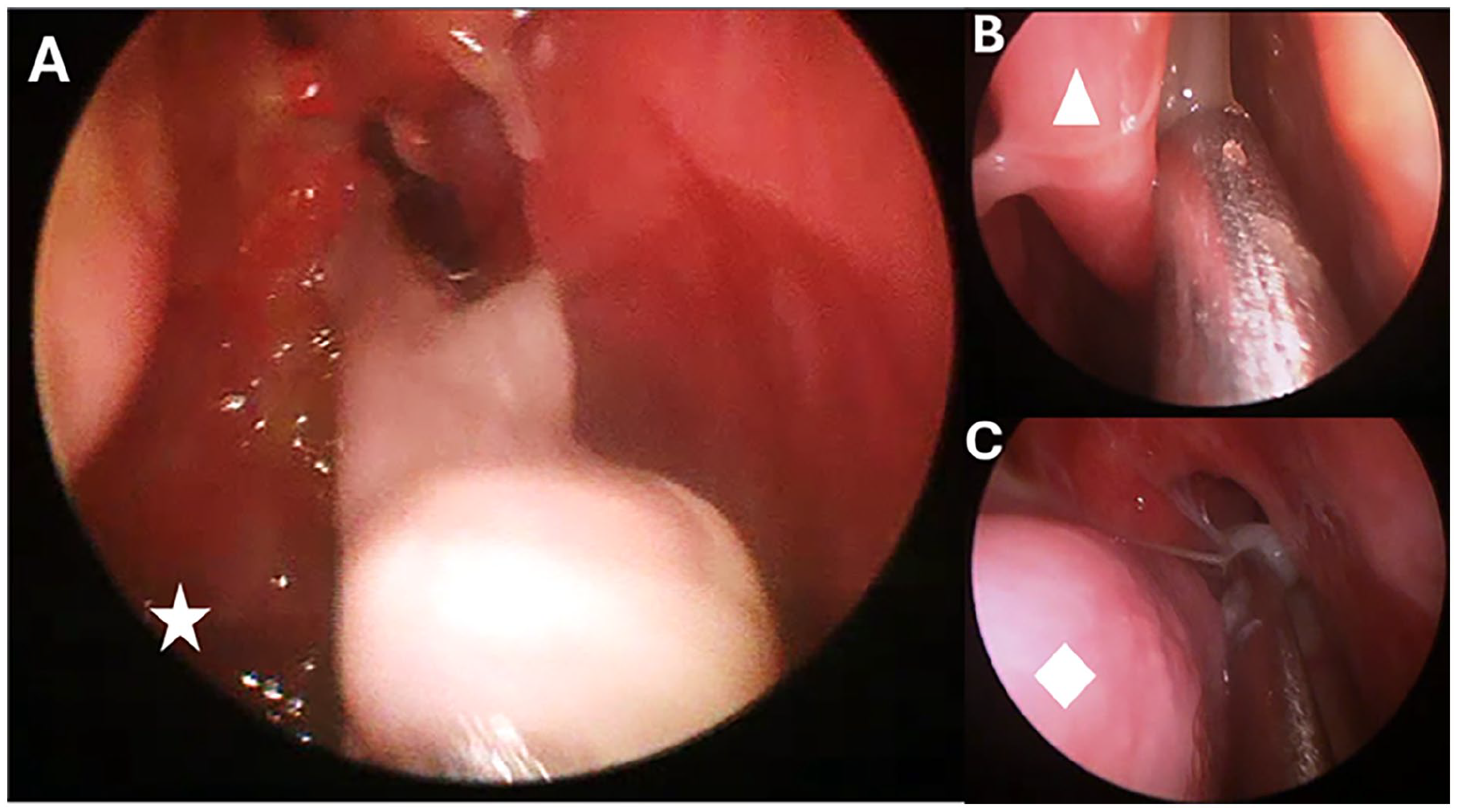
Endoscopic view with a 4 mm 30-degree endoscope of the operated paranasal sinuses during active infection. (A) depicts thick mucopurulent secretions within the right mid-ethmoids with a star denoting the approximate location of the maxillary sinus. (B) depicts the left middle meatus with purulent secretions draining into the frontal recess just lateral to the middle turbinate (white triangle). (C) depicts pooling purulent secretions in the nasopharynx just posterior to the inferior turbinate (white diamond).
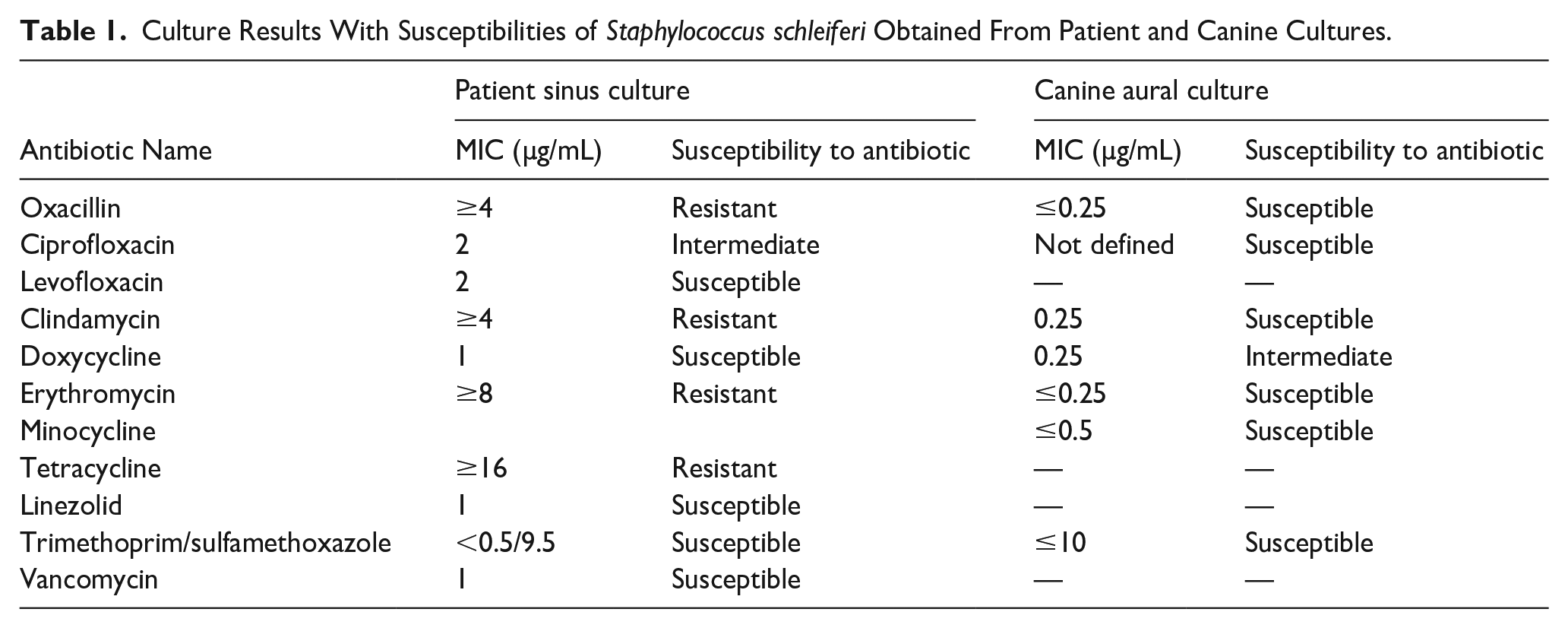
Culture Results With Susceptibilities of Staphylococcus schleiferi Obtained From Patient and Canine Cultures.
Discussion
We present the first documented case of bacterial rhinosinusitis caused by S. schleiferi. The patient presented in the peri-operative setting while still on a low-dose steroid taper after likely zoonotic transmission due to close proximity to canines at home while treating acute otitis externa caused by the same bacterium. The infection was successfully managed with trimethoprim/sulfamethoxazole, and the patient suffered no long-term consequences of this infection, and both the patient and his dog recovered without issue.
Zoonotic sinus infections are uncommon causes of acute bacterial sinus infections but should be considered within the differential for those infections that are refractory to standard treatment, or those in which there are discrete risk factors of zoonotic infection. It is estimated that up to 66% of American households have a pet, with 65.1 million households reporting owning a pet dog, and 46.5 million households owning a pet cat. 14 Therefore, a large number of patients in the United States are at risk of companion animal-related infections.
Staphylococcus pseudointermedius is an example of a previously documented zoonotic bacterium that can lead to sinus infections in humans. This bacterium colonizes the skin, mouth, nares, and anus of healthy canines and has been documented to cause multidrug-resistant sinus infections in humans. 15 One study examining rates of S. pseudointermedius infections found that dog ownership increased the risk of infection with S. pseudointermedius (P < .01) even in the absence of immunodeficiency. 16 Similar zoonotic infections have been documented with S. intermedius with canine exposure, 17 but there are a plethora of other potential zoonotic infections that can have head and neck manifestations, including the paranasal sinuses. 18
Data examining the role of S. schleiferi in human infection remain sparse. To date, the existing literature constitutes only small case series, case reports, and limited retrospective reviews. Despite this, the potential role of this bacterium has become increasingly investigated in the veterinary literature. One study examined isolates from 80 dogs (42 healthy, and 38 with otitis externa) and found that up to 40% of dogs with acute otitis externa had isolates positive for S. schleiferi compared to only 5% of healthy dogs. Methicillin resistance was present in up to 24% of isolates, and there was a strong propensity for biofilm formation, and up to 86% of isolates carried genes for staph enterotoxin. 19 The clinical significance of these findings, particularly in human infection, remains unclear, but it is worthwhile to note that our patient contracted his infection while actively treating otitis externa in his pet dog. Our case presentation is similar to other cases reported in a patient with direct exposure to his pet’s purulent otorrhea that resulted in severe bacteremia and subsequent septic shock in an otherwise immunocompetent patient, 20 and meningitis in a pediatric patient. 10
The role of immunodeficiency in human infection with S. schleiferi remains similarly unclear. Hernández et al., 3 in the largest case series of 28 patients with S. schleiferi infections to date, noted that over half of the infections occurred in patients who were immunosuppressed. Additional case reports have reported infections in immunocompromised hosts.5-8 Other reports have indicated that infections with S. schleiferi can occur within immunocompetent patients4,10,13,20 In the case of our particular patient, he had no known immunodeficiency aside from his recent surgical intervention 21 and oral prednisone use, 22 which would be expected in many patients undergoing endoscopic sinus surgery. It may be prudent to caution patients regarding the risks of close exposure, not only to sick human contacts but also to sick canine contacts in the context of these reports, albeit rare.
Conclusion
We report the first case of acute bacterial rhinosinusitis caused by zoonotic transmission of S. schleiferi in the perioperative period. This is an exceedingly rare infection in the human population, but it appears to have risks associated with direct exposure to infected animals, particularly those with active ear infections. Caution with exposure to infected animals in the perioperative period may be prudent to minimize the risks of zoonotic infection.
Footnotes
Consent to Participate
Written informed consent was obtained from the patient for the publication of this case report.
Author Contributions
All authors reviewed the case, contributed to writing and editing the manuscript, and approved the final version of the manuscript.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
N/A.
