Abstract
We report a case of a healthy 62-year-old male with no identifiable risk factors who presented with a 2-week history of progressive unilateral parotid gland enlargement and tenderness followed by subsequent otorrhea. A computed tomography scan and ultrasound confirmed a markedly enlarged posterior aspect of the parotid gland with the evidence of necrosis. The culture of aspirated fluid grew Staphylococcus aureus. Purulent fluid was then noted draining from the external auditory canal, via the fissure of Santorini. The patient was treated with antibiotics, pain management, and daily parotid massage with complete resolution of the parotitis. Acute bacterial parotitis with subsequent drainage and otorrhea through the fissures of Santorini is rare, with only a few reported cases in the literature.
Background
Acute bacterial parotitis (ABP) is an uncommon condition typically seen among newborns, elderly, hospitalized, or postoperative adults1,2 It is typically seen in individuals who have a history of dehydration, malnutrition, immunosuppression, sialolithiasis, neoplasm, or medications that decrease salivary flow (eg, anticholinergics). 3 The most common bacterial agent responsible for ABP is Staphylococcus aureus and mixed oral aerobes/anaerobes. Haemophilus influenza is thought to be a causative pathogen for community-acquired infections, while gram-negative anaerobes are believed to play a larger role in hospital-acquired infections. Clinical presentation is characterized by rapid progression of unilateral facial swelling and induration and occasional in the parotid region, often accompanied by erythema and tenderness. Trismus, fevers, and purulent drainage from Stenson’s duct are also common findings. Patients will often have an elevated WBC and C-reactive protein levels on bloodwork. Uncommon complications of ABP include respiratory obstruction and septic jugular thrombophlebitis due to spread of infection into the parapharyngeal space, facial weakness, skin breakdown over the parotid gland, and osteomyelitis of the mandible. Differential diagnosis for ABP includes viral parotitis, obstructive sialoadenitis from sialolithiasis or neoplasms (benign and malignant), systemic disorders such as alcoholism or diabetes, and autoimmune disorders such as Sjogren’s disease. Diagnosis is made by clinical presentation as well as by imaging, with ultrasound and computed tomography (CT) imaging with intravenous contrast being the most common modalities. Treatment for ABP includes treatment with broad-spectrum antibiotic therapy directed against S. aureus, H. Influenza, Streptococci, and other oral anaerobes. Patients with severe disease or complications described above should be treated with IV antibiotic therapy, with first-line therapy including ampicillin–sulbactam, or ceftriaxone or levofloxacin plus metronidazole. Vancomycin therapy is reserved for patients with known or suspected methicillin-resistant Staphylococcus aureus (MRSA) infection. Patients with less severe disease can be treated with oral agents such as amoxicillin–clavulanate, cefuroxime plus metronidazole, levofloxacin plus metronidazole, or moxifloxacin. Linezolid or trimethoprim–sulfamethoxazole can be added in suspected or known MRSA infections. The most common resolution of ABP is drainage through the duct of Stenson into the oral cavity. 1 The fissures of Santorini are naturally occurring defects that extend through the osseocartilaginous or cartilaginous junctions of the external auditory canal and provide a potential avenue between the external auditory canal and the superficial lobe of the parotid gland.4,5 Few cases of ABP with otorrhea via the fissures of Santorini have been reported in the literature. Recent reports include a parotid abscess with otorrhea in a 17-month-old infant, and another in a 40-year-old female with sialolithiasis.4,6 We describe a patient with acute suppurative bacterial parotitis and drainage via the fissures of Santorini.
Case
A 62-year-old male presented with progressive pain and swelling of the neck. Two weeks prior, he woke with right jaw/temporomandibular joint pain that was attributed to bruxism and improved with nonsteroidal anti-inflammatory drugs (NSAIDs). Over the next 14 days, pain gradually increased over the mastoid process and along the lateral aspect of the neck ultimately poorly controlled with NSAIDS and induration along the sternocleidomastoid muscle became appreciable. Patient was afebrile throughout and denied any associated upper respiratory or oral symptoms. Patient recalled having mumps as a child (prior to available vaccination). Patient had worn night guard regularly for bruxism for years. Physical exam notable for significant swelling below the right jaw and induration extending periauricularly. CT scan (Figure 1) and subsequent ultrasound confirmed a markedly enlarged posterior aspect of the parotid gland with evidence of necrosis. Ultrasound-guided aspiration yielded 3 cc of tenacious, purulent fluid. Patient was started on amoxicillin–clavulanic acid awaiting culture. Subsequent gram stain was notable for gram-positive cocci and cultures grew S. aureus. Antibiotic coverage was switched to high-dose, double strength, trimethoprim/sulfamethoxazole twice daily for 14 days. Thirty-six hours after the initial aspiration, purulent fluid was noted emanating from the right external auditory canal (Figure 3). Purulent drainage on Day 3 of diagnosis was noted from the anterior-inferior aspect of the external auditory canal, just lateral to the bony cartilage. Patient was able to apply warm compresses and milk the parotid over the next 2 days to express a significant amount of purulent drainage from the external auditory canal (estimated 10-20 cc total) with coincidental improvement in swelling, induration, and pain. Drainage tapered off over several more days. Subsequent follow-up and physical examination 2 weeks after initial presentation revealed complete resolution of the swelling and drainage. Follow-up CT imaging of the neck showed no residual inflammatory changes and no evidence of any underlying neoplasm (Figure 2).

Axial computed tomography image of neck at level of parotid gland prior to ultrasound-guided aspiration of left parotid abscess.

Axial computed tomography image of neck at level of parotid gland after completion of antibiotic therapy and spontaneous drainage from external auditory canal.
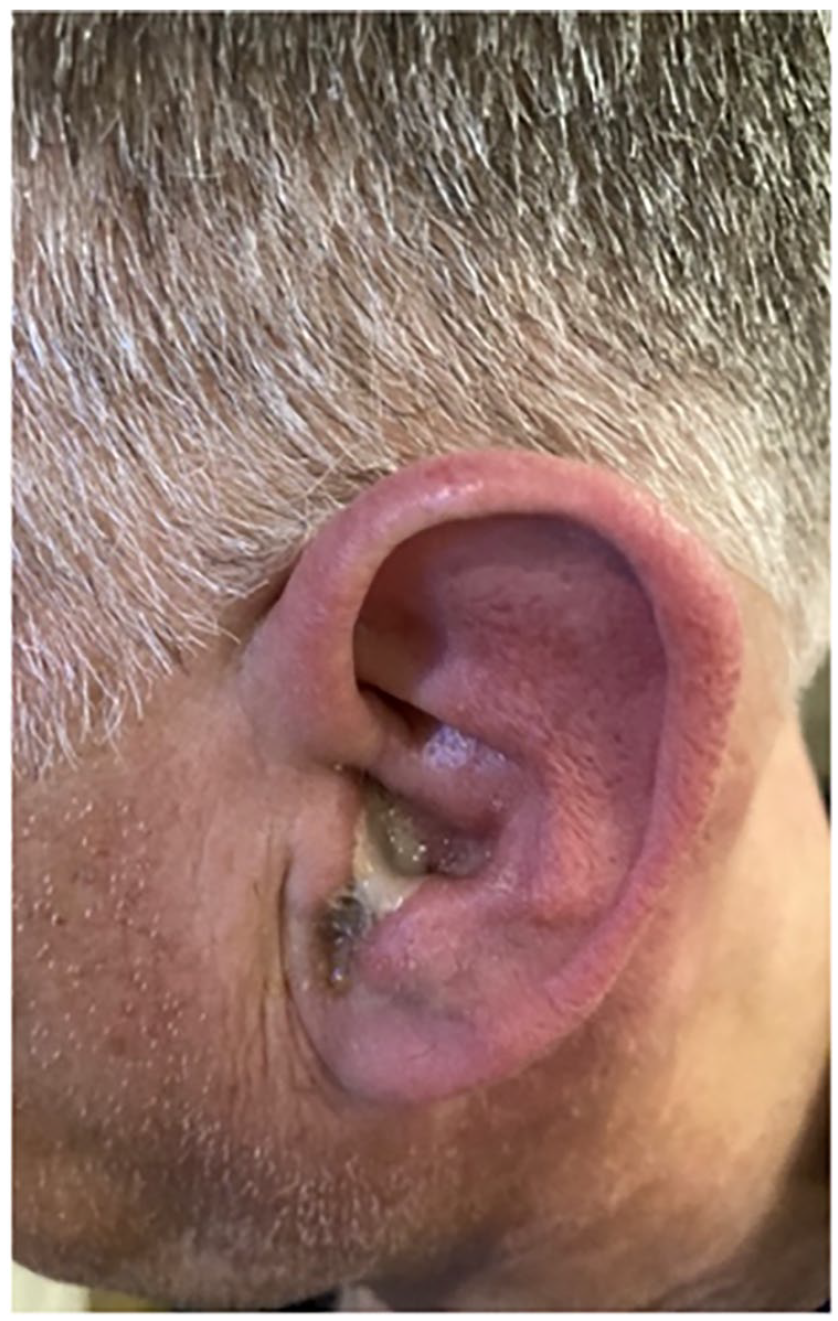
Purulent drainage out of external auditory canal.
Discussion
Parotitis is commonly caused by ductal obstruction (often via sialolithiasis) or by inflammatory conditions (namely Sjogren, rheumatoid arthritis, systemic erythematosus lupus) 1 Infections of the parotid gland can be bacterial, most often caused by bacteria such as S. aureus, anaerobes, and gram negatives. Viral parotitis has a number of etiologies including influenza, mumps, HIV, EBV, and many others.2,3 ABP is commonly seen in those who are dehydrated, malnourished, or hospitalized, and among newborns or the elderly.1,2 It is not reported to have a gender predominance. 1 Here we present an uncommon report of a previously healthy 62-year-old patient with no history of vascular disease, alcoholism, or inflammatory conditions, excellent oral hygiene, with no recent procedures, who is not immunocompromised, dehydrated, or malnourished presenting with ABP.
While this patient had no history of sialolithiasis and no stone or tumor was found on any imaging, the patient did present a couple of weeks after initial symptom onset leaving the possibility remaining that a stone could have initially obstructed the parotid gland inciting infection and subsequently passed on its own prior to the patient’s first clinic visit. However, the patient presented with indolent and constant pain not associated with eating, changes in salvation or a palpable stone—a presentation not typical for sialolithiasis.
In patients with ABP, purulence typically drains via the duct of Stenson, the primary duct of the parotid gland which exits into the oral cavity opposite to the crown of the upper second molar. 1 Parotitis leading to otorrhea is due to drainage via the fissures of Santorini, a rare condition and identified in only a few case reports including one in a 17-month-old infant, and another in a 40-year-old female with poor dental hygiene and sialolithiasis.4,6,7
The fissures of Santorini are a naturally occurring defect in the cartilaginous portion of the external auditory canal and provide a possible passage from the external auditory canal to the superficial lobe of parotid gland.4,5 The fissures of Santorini have been demonstrated to be avenues for infection and neoplasms from the external environment to the parotid gland classically seen in necrotizing external otitis, or as conduits for drainage of salivary fistulas.8 -11 It has been rarely reported as a conduit for drainage from a primary parotid infection.
ABP should be suspected in healthy patients without observed sialolithiasis, good oral hygiene, and no history of dehydration presenting with painful and progressively enlarging induration in the periauricular region or overlying the masseter muscle. When parotitis is coupled with otorrhea, drainage may occur via the fissures of Santorini.
Conclusion
The fissures of Santorini are an underappreciated route of drainage and resolution for infectious material originating from the parotid gland and result in an alternative clinical presentation to traditional drainage through the duct of Stenson.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Statement
Our institution does not require ethical approval for reporting individual cases or case series.
Patient Consent
Obtained.
Data Availability
All data and results are available as part of this article.
