Abstract
Keywords
Introduction
Cerebrospinal fluid (CSF) leakage occurs when there is a tear or defect in the dura mater, resulting in the passage of CSF from the subarachnoid space into the extracranial space. 1 Patients with CSF leakage may present with significant rhinorrhea or otorrhea, as well as neurological symptoms such as headache, tinnitus, or meningitis. 1 CSF otorrhea, although rare, can be spontaneous or caused by trauma, tumor, or iatrogenic surgical injury. 2 If left untreated, CSF leakage can lead to intracranial infection and potentially become life-threatening. The treatment of CSF otorrhea involves both nonsurgical and surgical methods. 3 Nonsurgical treatment is usually effective and sufficient for most patients. However, surgical intervention is necessary for those with persistent CSF otorrhea for over 3 weeks despite nonsurgical treatment. Currently, the commonly used surgical approaches for treating CSF otorrhea include transmastoid process, middle fossa craniotomy, or a combination of both. 4 Nevertheless, with the advancement of minimally invasive ear, nose, and throat surgery, the selection of surgical treatment for CSF otorrhea is no longer limited to traditional surgical methods. 5 The choice of surgical approach should be based on the location and size of the defect. Identification and complete exposure of the defect are critical for achieving complete closure and healing. 6 In the present study, we proposed 3 surgical methods for treating CSF otorrhea: local repair of the defect, local repair of the defect combined with sealing of the tympanic sinus entrance, and closure of the eustachian tube and the external auditory canal. Our focus was on the local repair of the primary meningeal defect, and when local repair surgery was unsuccessful, closure of the nasopharyngeal tube and external ear canal served as a last resort. This case series aimed to report on patients with CSF otorrhea who underwent 3 surgical methods, offering less invasive surgical options for appropriately selected patients with CSF otorrhea.
Methods and Materials
Patients
A retrospective analysis was conducted on patients who underwent surgery for CSF otorrhea in the Department of Otolaryngology and Head and Neck using the surgical database from June 2012 to June 2022. All clinical data were obtained from the surgical databases of the Department of Otolaryngology and Head and Neck. This case series study was approved by the Ethics Committee of our hospital, and informed consent from patients was exempted.
Surgical Methods and Postoperative Treatment
The selection of specific surgical methods, including local defect repair, local defect repair combined with sealing of the tympanic sinus entrance, and local defect repair combined with sealing of the eustachian tube and the external auditory canal, primarily depended on the patients’ hearing status, the specific location of the leak, and other patient characteristics. The decision-making process also relied on the experience and judgment of the surgeon. The local repair method of defects was suitable for patients with small defects, while for patients with large defects, a combination of local repair of defects and sealing of tympanic entrance was often chosen. In cases where patients had large defects and an incomplete posterior wall of the external auditory canal or severe deafness, repair of defective meninges using temporalis muscle or temporal fascia could be performed simultaneously with the closure of the eustachian tube and the external auditory canal.
A local repair of the defect: This method included 2 approaches, the transauricular approach (Figure 1) and the transmastoid approach (Figure 2). In the transauricular approach, the tympanic flap of the ear canal was elevated, and a portion of the shield plate was removed to expose the vestibular window area. The stapes were removed, and a temporalis muscle, approximately twice the diameter of the vestibular opening, was utilized for the repair into the vestibular cistern. One end of the muscle was fixed to the bottom of the internal auditory canal, while the other end, forming a dumbbell shape, was secured in the vestibular window. After confirming no CSF leakage, the tympanic flap of the external ear canal was repositioned. In the transmastoid approach, a posterior ear incision was made, and the mastoid process was contoured while preserving the posterior wall of the external auditory canal. Upon locating the defect, a temporal muscle or mastoid periosteum tissue twice the diameter of the defect, was utilized for repair. Approximately two-thirds of the tissue was placed inside the dura mater, and the remaining one-third outside the dura mater. After ensuring no CSF leakage, the surface was covered with temporal fascia and finally secured with fibrin glue (Bixiu, Guangzhou Bixiu Biotechnology Co., LTD, China).
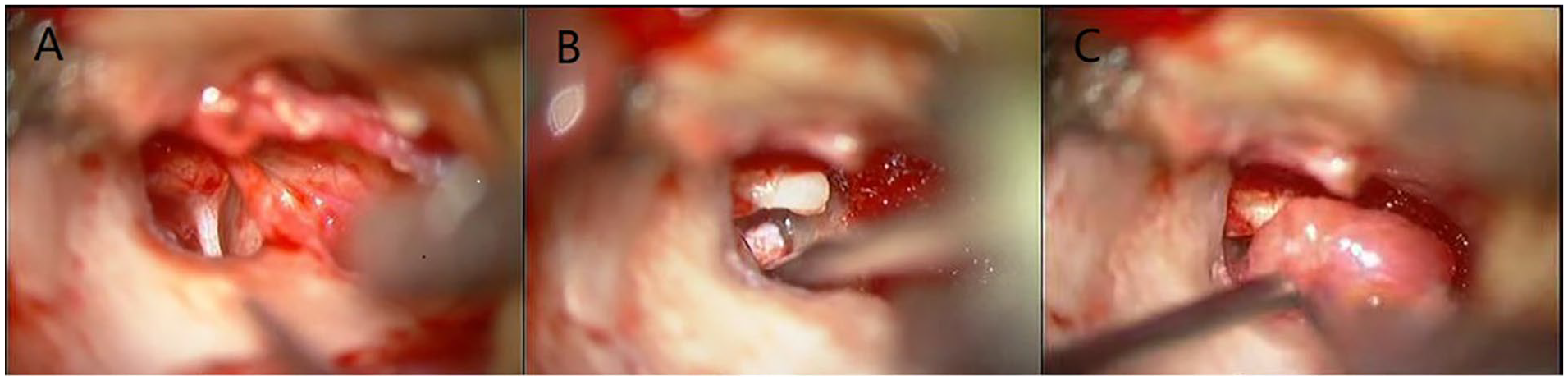
Local repair of the defect by the transauricular approach. (A) The tympanic flap of the external auditory canal was lifted, a portion of the shield plate was removed, and the vestibular window area was exposed. (B) The stapes were removed, revealing a leak in the stapes baseplate. (C) The temporalis muscle, approximately twice the diameter of the vestibule, was placed into the vestibular cistern, with one end reaching the bottom of the internal auditory canal, and the other end forming a dumbbell shape, was stuck in the vestibular window.
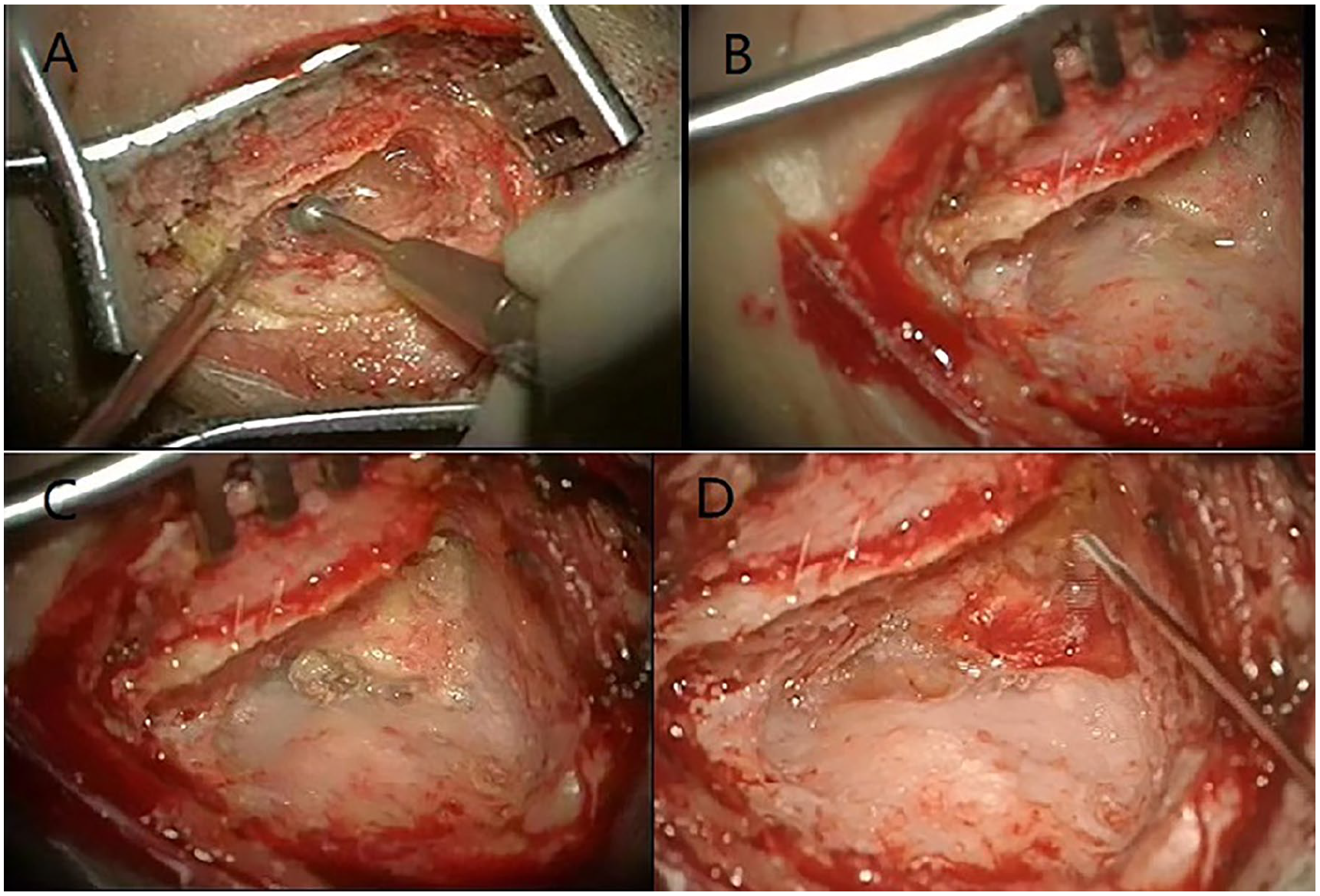
Local repair of the defect by the transmastoid approach. (A) The surgery was performed through a retroauricular incision using the mastoid approach. (B) The preservation of the posterior wall of the external auditory canal was observed. (C) After identifying the hiatus, the defect was repaired using temporalis muscle or mastoid periosteum tissue, which was twice the diameter of the hiatus. (D) After ensuring no cerebrospinal fluid leakage, the surface was covered with temporal fascia and fixed with fibrin glue.
A local repair of the defect combined with sealing of the tympanic sinus entrance (Figure 3): a posterior ear incision was made, and the mastoid process was contoured, while preserving the posterior wall of the external auditory canal. Upon locating the defect, a temporalis muscle or mastoid periosteum tissue, twice the diameter of the leak hole, was used for repair. The entrance of the tympanic sinus was closed with muscle or mastoid periosteum tissue, and the mastoid cavity was repaired with adipose tissue.
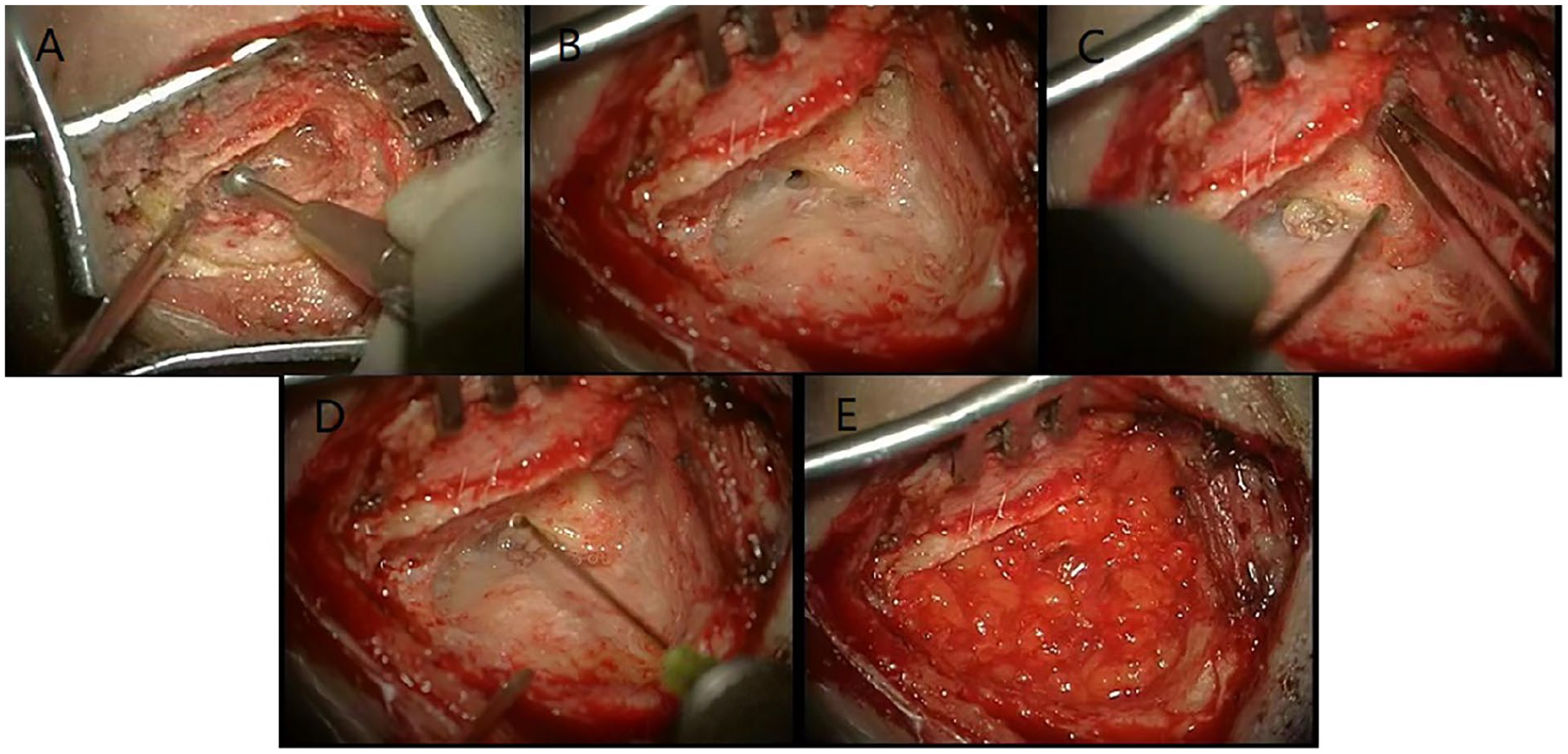
Local repair of the defect combined with sealing of the tympanic sinus entrance. (A) A retroauricular incision was made, and the mastoid process was contoured. (B) The posterior wall of the external auditory canal was left intact. (C) After identifying the defect, it was filled with temporalis muscle or mastoid periosteum tissue, which was twice the diameter of the defect. (D) The defect was fixed with fibrin glue. (E) The entrance to the tympanic sinus was sealed with muscle or mastoid periosteum tissue. (F) The mastoid space was packed with adipose tissue.
Closure of the eustachian tube and the external auditory canal (Figure 4): a posterior ear incision was made, and the mastoid process was contoured without preserving the posterior wall of the external auditory canal. The repair materials were applied to address the leakage, and the defective meninges were repaired using sutures with temporal fascia. The skin of the external auditory canal was incised in the middle segment, and the skin of the internal segment of the external auditory canal and the mucous membrane of the middle ear cavity were completely removed. The eustachian tube was closed with muscle tissue or mastoid periosteum tissue. Bone wax was applied to reinforce the eustachian tube orifice, and fibrin glue was applied into the orifice of the eustachian tube. The temporal fascia was used to reinforce the eustachian tube orifice, and adipose tissue were used to repair the mastoid cavity.
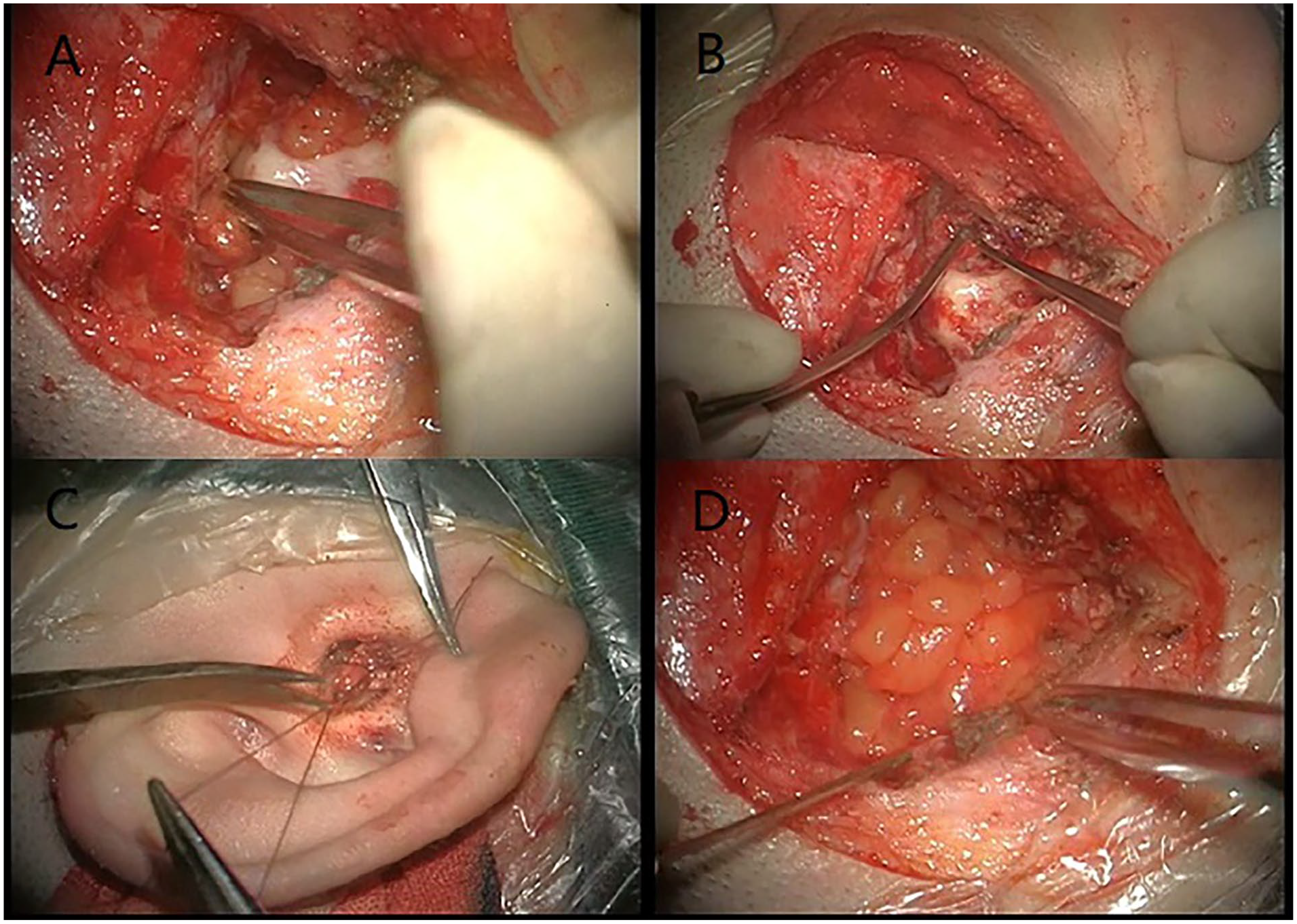
The closure of the eustachian tube and external auditory canal. (A) The leaks were caulked. (B) Closure of the eustachian tube. (C) Closure of the external auditory canal. (D) Intraoperative fat packing.
After the surgery, all patients were placed on bed rest with a 30° head elevation for 1 week. The surgical site was bandaged with pressure for 6 to 7 days, and postoperatively, Ceftriaxone sodium (2g IV qd) was administered to prevent potential infections. Intermittent or continuous lumbar cisterna drainage was routinely employed, and rapid intravenous infusions of 15% to 25% mannitol solution was administered to treat increased intracranial pressure. Stitches were removed approximately 10 days after surgery.
Data Collection
Data collection involved obtaining the basic demographic characteristics of the patients, including gender, age, chief complaints, location of the leaky hole, otoscopy results, skull base thin-slice computed tomography (CT) examination results, and causes of CSF otorrhea. All patients were followed up for more than 6 months after surgery and were considered cured if there was no recurrence of CSF otorrhea within 6 months.
Statistical Analysis
Statistical analysis was conducted using SPSS 26.0 software (Stata Corp., College Station, TX, USA). Measurement data were presented as minimum to maximum values, while categorical data were expressed as n (%).
Results
A total of 26 patients with CSF otorrhea who underwent surgical treatment in the Department of Otolaryngology and Head and Neck between June 2012 and June 2022 were included in this retrospective case series report. The study comprised 13 (50%) male and 13 (50%) female patients, with ages ranging from 4 to 85 years.
Etiology Analysis of CSF Otorrhea
The etiology of CSF otorrhea in the patient group was as follows: spontaneous CSF otorrhea in 10 (38%) cases (including 2 (8%) cases of congenital inner ear deformity and 8 (31%) cases of no obvious cause), traumatic injury in 5 (19%) cases, cholesteatoma complications in 6 (23%) cases, postoperative complications of brain tumor in 3 (12%) cases, radiotherapy in 1 (4%) case, and malignant tumor in 1 (4%) case.
Chief Complaints
The patients presented with the following chief complaints: ear flow in 11 (42%) cases [including 2 (8%) cases following eardrum catheterization], ear discharge in 6 (23%) cases, hearing loss in 8 (31%) cases, recurrent headache and fever in 2 (8%) cases, tinnitus in 2 (8%) cases, and CSF rhinorrhea in 1 (4%) case.
Outcomes of Preoperative Otoscopy, Hearing Test, and Skull Base CT Examination
Preoperative otoscopy revealed tympanic membrane perforation in 15 (58%) cases, with pulsing fluid resembling water gushing out in all of them. Ventilation ducts were seen in 4 (15%) cases. The tympanic membrane was intact in 6 (23%) cases, while middle ear effusion was present in 5 (19%) cases. Results of preoperative pure tone hearing test results indicated that 6 (23%) of the 26 patients had profound deafness in the affected ear. Moreover, thin-slice CT examination prior to surgery revealed loss of intervertebral septa between the base of the internal auditory tract and the vestibular space in 2 (8%) cases (Figure 5), and bone defects at the base of the skull in 24 (92%) cases (Figure 6).
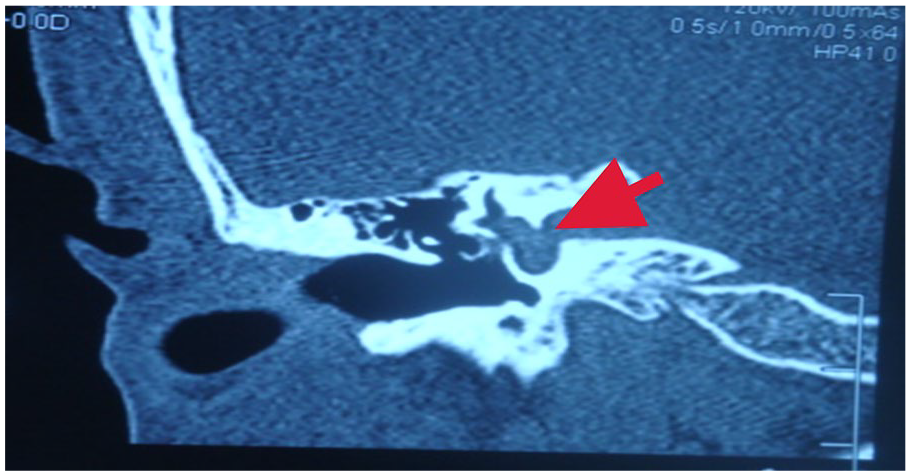
The red arrow showed the absence of space between the floor of the internal auditory canal and the vestibular bone.
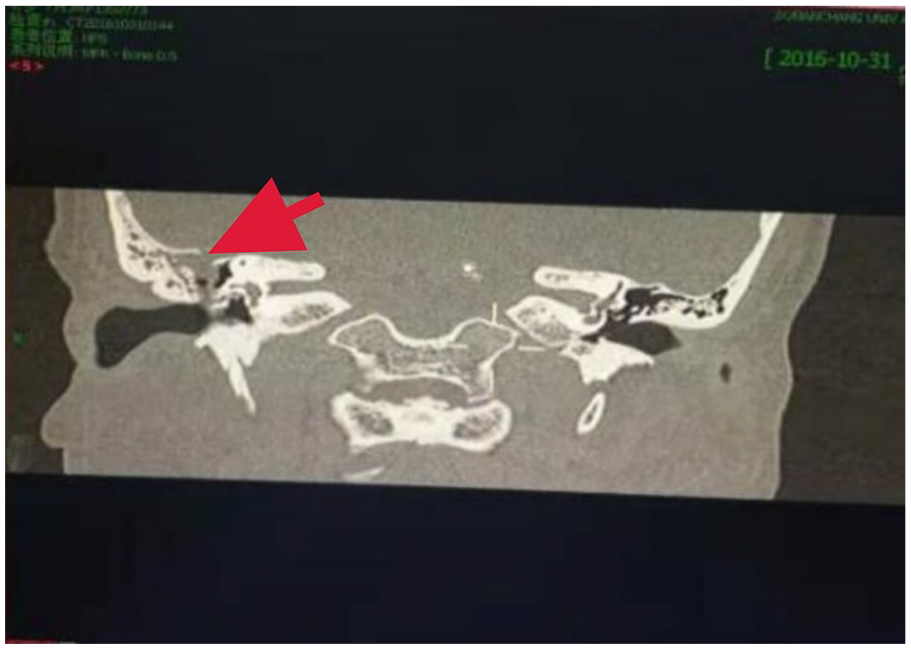
The red arrow showed the bone defect in the right eardrum sinus cap.
Location of the Leaky Hole and the Selected Surgical Methods
Among the patients, 12 (46%) cases underwent local repair of the defect, with 2 (8%) cases treated using the transauricular approach and the remaining 10 (38%) cases treated using the transmastoid approach. In 1 (4%) patient with apical fluid leakage, local repair of the defect was performed while preserving the posterior wall of the external auditory canal, with no recurrence. For 3 (12%) cases of CSF otorrhea, local repair of the defect was combined with sealing of the tympanic sinus entrance, while closure of the eustachian tube and the external auditory canal was performed in the remaining 11 (42%) cases.
During the surgical procedures, the leaky holes were identified as follows: oval window in 2 (8%) cases, tympanic sinus cover in 14 (54%) cases, tympanic cover in 7 (27%) cases, superior recess of the eustachian tube in 1 (4%) case, anterior superior recess of the tympanic tube in 1 (4%) case, and meninges of the posterior fossa in 1 (4%) case (Table 1).
Clinical Data of 26 Cases With Cerebrospinal Fluid Otorrhea.
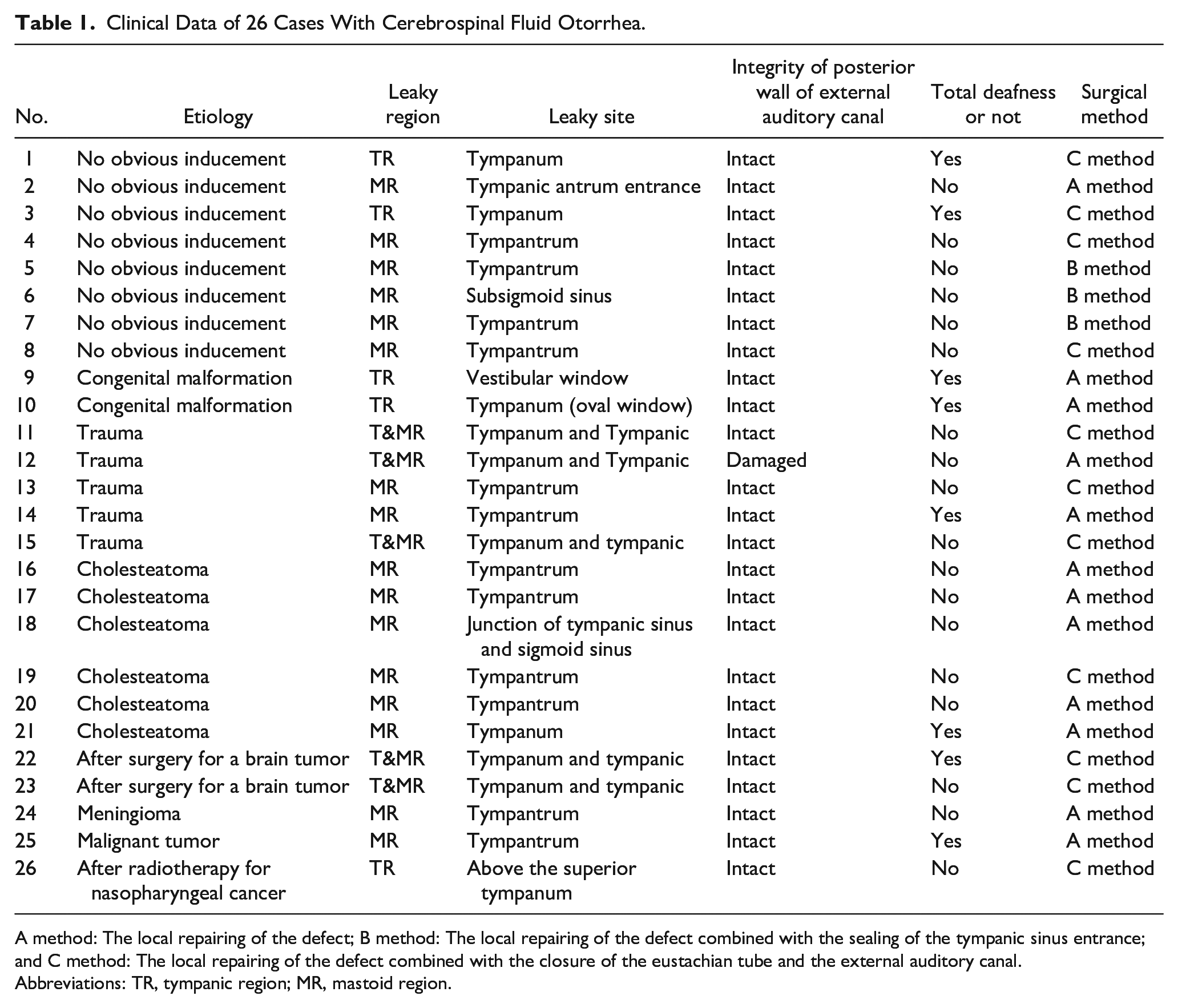
A method: The local repairing of the defect; B method: The local repairing of the defect combined with the sealing of the tympanic sinus entrance; and C method: The local repairing of the defect combined with the closure of the eustachian tube and the external auditory canal.
Abbreviations: TR, tympanic region; MR, mastoid region.
Surgical Results and Follow-Up
All 26 patients achieved successful repair after a single procedure, and no recurrence of CSF otorrhea occurred after surgery. None of the patients showed clinical manifestations of increased intracranial pressure postoperatively. The follow-up period ranged from 6 months to 10 years, and no instances of CSF otorrhea recurrence were observed after surgery.
Discussion
This case series report presented 3 surgical procedures for the treatment of CSF otorrhea and reported their application in 26 patients. Despite differences in age, etiology, chief complaints, and location of the defect, the appropriate surgical method was selected based on the location of the CSF leak and the integrity of the posterior wall of the external auditory canal, ultimately achieving a standard cure.
The leaky hole of CSF otorrhea may serve as a portal for bacterial invasion of the meninges, potentially leading to intracranial infection, thus requiring active treatment. 1 The surgical approach and intraoperative repair methods for CSF otorrhea primarily depend on the location and size of the leaky hole. 6 Therefore, accurate identification of the leaky hole is crucial for successful surgery. Complete exposure of the leaky hole allows for thorough repair using the temporalis muscle, effectively closing the defect and achieving the desired outcome. 6 We believe that caulking or sealing the stenosis of the CSF outflow channel is an effective method for treating CSF otorrhea. In the current study, we divided the middle ear into 2 regions: the tympanic region and the mastoid region (MR), separated by the posterior wall of the external auditory canal. In cases of CSF otorrhea occurring in the tympanic region, the primary focus of repair was on the meningeal defect, followed by addressing the opening of the eustachian tube tympanic and the external ear canal as secondary barriers. For CSF otorrhea occurring in the MR, the repair process involved addressing the meningeal leak hole as the first barrier, followed by sealing the entrance to the tympanic sinus and then the eustachian tube tympanic orifice and the external ear canal orifice. Therefore, 3 surgical methods were employed for treatment of CSF otorrhea: local repair of the defect, local repair of the defect combined with sealing of the tympanic sinus entrance, and local repair of the defect combined with closure of the eustachian tube and the external auditory canal. Repairing the meningeal defect served as the fundamental surgical method, while closure of tympanic foramen, eustachian tube, and external auditory meatus served as an important supplementary surgical method. For CSF otorrhea occurring in the tympanic area, the local repair method was typically used if the hole was located in the vestibular window area or the tympanic cover and the meningeal hole was small. This type of CSF otorrhea was found to be highly associated with congenital inner ear malformations, such as incomplete compartmentalization of the inner ear, resulting from the absence of a base in the internal auditory canal and vestibular bone septa. 7 According to Liao et al, 8 the vestibular cistern should be repaired with muscle tissue approximately twice the diameter of the vestibular cistern. This approach not only repaired the bottom of the internal auditory canal and closed the internal fistula but also prevented high CSF pressure from flushing out the packing muscle through the external fistula. Wu et al 9 suggested removing the stapes and repairing the vestibular window with muscle tissue. We encountered a case of postoperative meningioma with a leaky hole located in the superior recess of the eustachian tube and another case of nasopharyngeal carcinoma with radiotherapy and the leaky hole located in the anterior superior recess of the tympanum. In these cases, when repairing the leaky hole with the temporalis muscle, the muscle covered the eustachian tube orifice. However, as there was still a small amount of CSF leakage after the repair and the patient had poor hearing, we opted for a combined approach of local repair and sealing of the eustachian tube and the external auditory canal. In instances of CSF otorrhea occurring in the MR, Savva et al 10 suggested that a complete wall mastoid operation should be the main procedure, and the mastoid cavity should be repaired and closed using muscle and abdominal fat tissue. When dealing with CSF otorrhea in the MR, the operation was performed to locate the leaky hole. For cases with small leakage holes, the local repair method of the defect was adopted. However, for patients with large defects in the meninges of the tympanic sinus cover or cerebellar meninges, the approach involved combining local repair of the defect with sealing the entrance of the tympanic sinus, and repairing the leaky hole with muscle tissue as much as possible during the operation. If the air chamber of the cryptic nerve on the opposite nerve was exposed, it was sealed with bone wax to prevent CSF outflow from the posterior tympanum. Likewise, if the abdominal ampulla and vestibule of the semicircular canal were exposed, the vestibule cisterna was repaired with muscle tissue to prevent CSF outflow from the vestibule and cochlear windows. Deng et al 11 also emphasized that using large muscles could not only block the floor of the internal auditory tract but also close the internal fistula. For patients with large defects in the meninges of the tympanic sinus cover and cerebellum, an incomplete posterior wall of the external auditory canal, and severe or total deafness, repairing the leak hole with temporal muscle or suturing the defective meninges with temporal fascia could be complemented by the closure of the eustachian tube and the external auditory canal. Intraoperative cavity repair could be performed using fat tissue. Lovin et al 12 depicted that the closure of the external auditory canal was highly effective for the treatment of CSF otorrhea, especially in cases of recurrent CSF otorrhea. To prevent CSF leakage from the incision, Zhang et al 13 recommended cutting abdominal fat into a cord shape, with one end facing inward and the other end facing outward and slightly higher than the mastoid plane. Sealing the eustachian tube and the external auditory canal has been considered as the safest and final option for repairing CSF otorrhea, although it should be avoided in patients with remaining hearing. In addition to muscle, fascia, fat, bone wax, cartilage, and bone pieces, mastoid periosteum tissue has emerged as a new option in recent years. 14 It is the soft tissue collected from the mastoid surface when the bone is removed, containing periosteum, muscle, and bone fragments. The use of mastoid periosteum for caulking the leakage has been found to be easier and more effective, warranting further study. 14
In conclusion, the selection of surgical repair methods for CSF otorrhea should take into account the size and location of the leaky hole, as well as the patients’ hearing status, and the integrity of posterior wall of the external auditory canal. Once the appropriate surgical method was selected, the outcomes of surgical treatment for CSF otorrhea could be satisfactory.
There were a few limitations to acknowledge in this case series report. Firstly, the limited number of CSF rhinorrhea cases resulted in a wide age range among the reported patients, leading to significant heterogeneity. Secondly, there was a lack of comparison with conventional surgical treatments for CSF otorrhea. Thirdly, the follow-up period for some cases was relatively short, and the focus was primarily on the recurrence of CSF otorrhea, overlooking the investigation of postoperative neurological function and quality of life.
Conclusion
Taken together, the 3 surgical treatment methods for CSF otorrhea, namely local repair of the defect, local repair of the defect combined with sealing of the tympanic sinus entrance, and local repair of the defect combined with sealing of the eustachian tube and the external auditory canal, demonstrated the ability to successfully treat CSF otorrhea in appropriately selected patients. These methods offered less invasive surgical options for the management of CSF otorrhea.
Footnotes
Data Availability Statements
The datasets generated and analyzed during the current study are available from the corresponding author on reasonable request.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by National Natural Science Foundation of China (No. 82101237) and Jiangxi Provincial Health Commission Fund (No. 20203227).
Ethical/Consent Statement
The study protocol was approved by the Ethics Committee of First Affiliated Hospital of Nanchang University. Informed consent was obtained from all the study subjects before enrollment.
