Abstract
Background
In addition to its hemostatic and stabilization role, biodegradable nasal packing can be used as a carrier for drugs after functional endoscopic sinus surgery (FESS). The aim of this study was to compare the influence of biodegradable synthetic polyurethane foam (NasoPore) soaked with ciprofloxacin, or betamethasone, or both to the same foam soaked with saline after FESS.
Methods
120 adults with chronic rhinosinusitis, with and without polyps, directed for bilateral full-house FESS were enrolled for the study. The patients were randomized and blinded into 3 groups, depending on the type of postoperative procedure applied. Thus, NasoPore soaked with antibiotic was provided to the first group; in the second group, the steroid was used; and the combination of both, in the third group. In each case, the aforementioned procedure was administered on one side of the nose, while NasoPore was soaked in saline on the other, at the end of the surgery, respectively. The patients were requested to complete a questionnaire during their postoperative visits at 2, 10, 30, 90, and 180 days, scoring the level of complaints on the VAS scale, separately for each side. The evaluation of the healing process was performed at each visit using rigid endoscopy and subsequently rated on numerical scales.
Results
Decreased mucosal edema and secretion; reduced Lund-Kennedy score; and favorable influences on facial pressure, nasal blockage, and smell were most evidently seen in the group receiving the antibioticsteroid combination.
Conclusions
The application of biodegradable nasal packing with betamethasone and ciprofloxacin in sino-nasal surgery has positive effects not only on the healing process but also impacts patient’s comfort. To optimize it, however, further research is needed.
Introduction
Since the early beginnings of endoscopic sinus surgery, the wound-healing process has been considered a crucial determinant of a successful outcome of the procedure. As long as the possibility of programming the healing process remains unavailable, the doctor’s efforts tend to be concentrated around the avoidance of healing complications, such as postoperative bleeding, inflammation, infection, meatal obstruction, and synechia formation.1–9 The use of nasal dressings, originally non-absorbable, today biodegradable, seems to decrease the frequency of complications, but does not eliminate them.1,3,8 Thus, additional interventions, pharmacological and non-pharmacological, are often introduced. Rudimental groups of substances include antibiotics, steroids, antihistamines, decongestants, and anti-inflammatories.10–13 Currently, humanized monoclonal antibody treatment also tends to be used, yet predominantly in patients with nasal polyps and coexisting asthma. 14
Possible drug admission ways are divided into systemic and topical, but considering the possible side effects, local application is preferred. However, topical admission, usually by nasal drops or nasal sprays, is characterized by poor penetration of the drug into tissues after endoscopic sinus surgery.10,15–20 This problem can be solved by using the nasal dressing as a carrier for topically applied drugs. 11 The aim of our study was to evaluate the effects and morbidities of using NasoPore combined with antibiotic (ciprofloxacin), steroid (betamethasone), or the combination of both on the postoperative healing process and the quality of life in adult patients, after endoscopic sinus surgery.
Materials and methods
A prospective, randomized, double-blind, placebo-controlled trial was conducted on patients with chronic rhinosinusitis, with and without polyps, having undergone FESS procedure. In all cases, the extent of the surgery was comparable. Therefore, antrostomy, anterior and posterior ethmoidectomy with sphenoid sinus opening, and surgery of the frontal recess type Draf 2a or 2b was performed.
Participants were recruited randomly from the adult patients diagnosed with chronic rhinosinusitis, both with and without polyps, having received refractory to maximal medical treatment and qualified for bilateral FESS.
Exclusion criteria were patients with signs of acute infection. Swabs were not routinely collected. Patients with purulent nasal discharge were not included in the study.
Ethics approval was obtained from the Nicolaus Copernicus University Collegium Medicum Bioethical Committee, and written consent was taken from all the patients before the enrollment.
The disease advancement was assessed in Lund-Mackay and Lund-Kennedy scales. Additionally, anamnesis on the record of allergy, asthma, and former medical treatment was taken.
The enrolled patients were randomized by a computer-generated program and having been assigned their numbers, allocated to 3 groups, 40 participants each, according to the following code: antibiotic (A)—ciprofloxacin (Ciprinol 10 mg/mL; manufacturer, Krka Poland), steroid (S)—betamethasone (Diprophos 7 mg/mL; manufacturer, MSD Poland) and the combination of both (AS). Ciprofloxacin was chosen for its efficacy in treatment of a wide spectrum of nose-colonizing bacteria, including Staphylococcus aureus, while betamethasone was selected due to its strong local activity. At the end of the FESS procedure, NasoPore dressing soaked with the proper drug was placed in one nasal cavity, while the opposite was treated with saline-soaked NasoPore, serving as a placebo. In each group, the sides were randomly assigned, with the amount of the drugs being a constant dose of 10 mg of ciprofloxacin and 7 mg of betamethasone. The preparation of the dressings was conducted by the operating theatre nurse, previously trained. Neither the surgeon nor the persons who performed the follow-up visits knew about the drugs applied or their allocation until the end of the follow-up.
All the patients were given the same postoperative recommendations after the surgery, that is, rinsing the nose with saline solution once a day for 2 weeks and using a nasal steroid for 3 weeks following the surgery.
Postoperative healing was evaluated on 2, 10, 30, 90, and 180 days after the surgery. The data collected consists of subjective complaints rating separately to each side (headache, nasal pain, pressure, nose blockage, itching, bleeding, and smell) using the VAS (Visual Analogue Scale) 10° scale, with 0 meaning no complaints at all and 10 marking the strongest and most severe symptoms a patient could imagine. The sense of smell was checked using scent markers, whereas the endoscopic evaluation of the healing process (bleeding, mucosae edema, secretion, package resorption, need for debris suction, synechiae formation, crusting, granulation, and lateralization) was performed using the numerical and Lund-Kennedy scales. The only exception was the second postoperative day—here, only the bleeding and resorption of the package were validated during the endoscopic examination.
To ensure proper group size, a statistical analysis of the size of the test sample was carried out. Thanks to that, statistical significance at the level of P < .05 and the test power for .80 using the Statistica version 13.1 program (Cracow. Poland) were determined. The statistical analysis was performed with the SPSS software for Windows, while the MannWhitney test was used for paired analysis, and KruskalWallis for unpaired analysis, both with P < .05 value.
Results
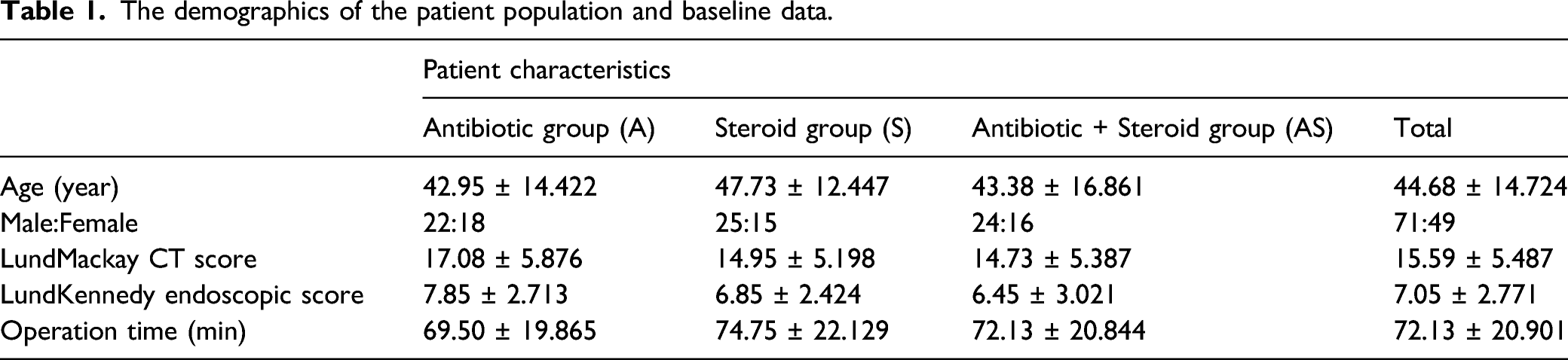
The demographics of the patient population and baseline data.
Endoscopic findings
The analysis of endoscopic findings (mucosae edema, secretion, crusts, and points in the Lund-Kennedy scale) in postoperative days.
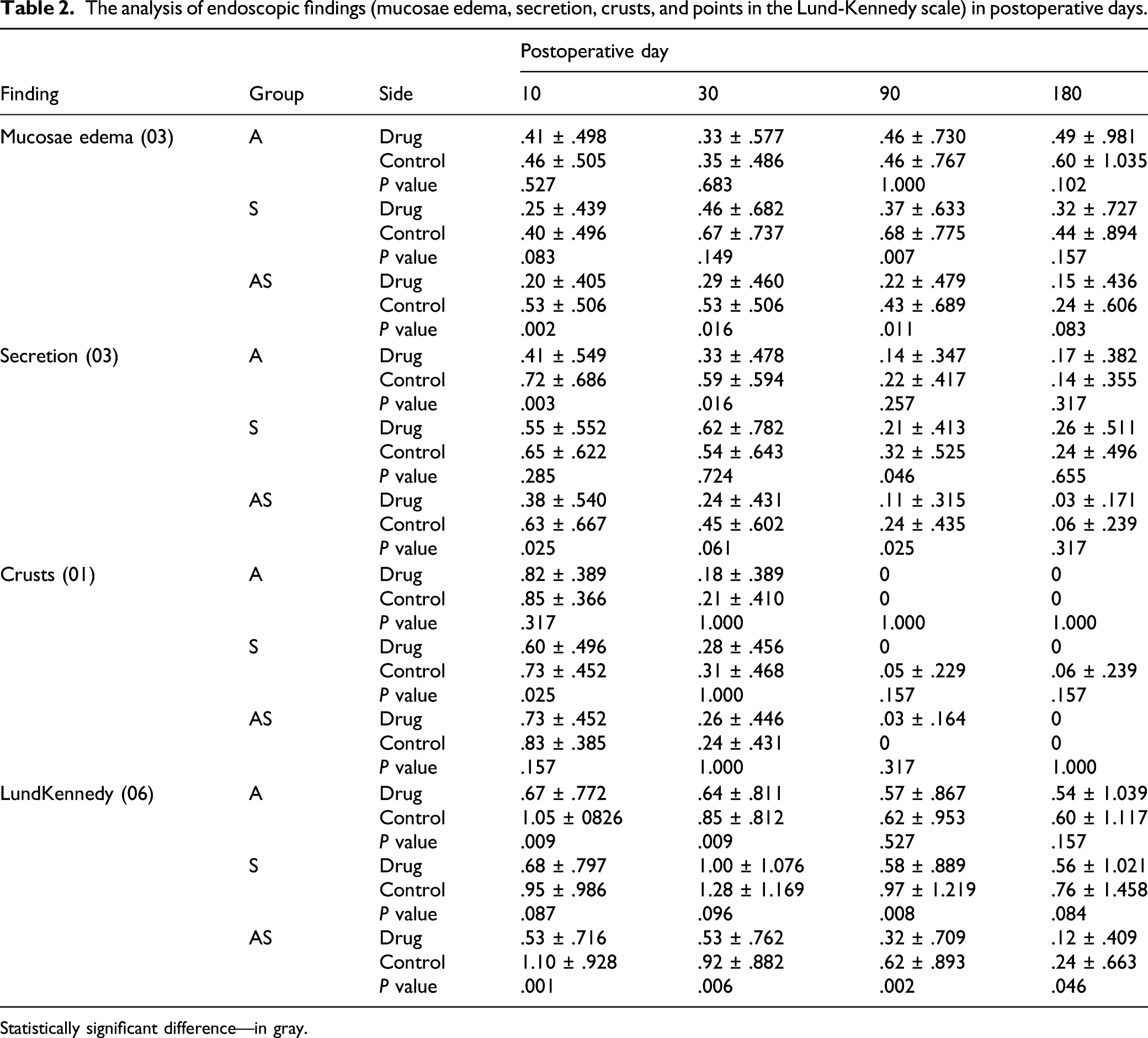
Statistically significant difference—in gray.
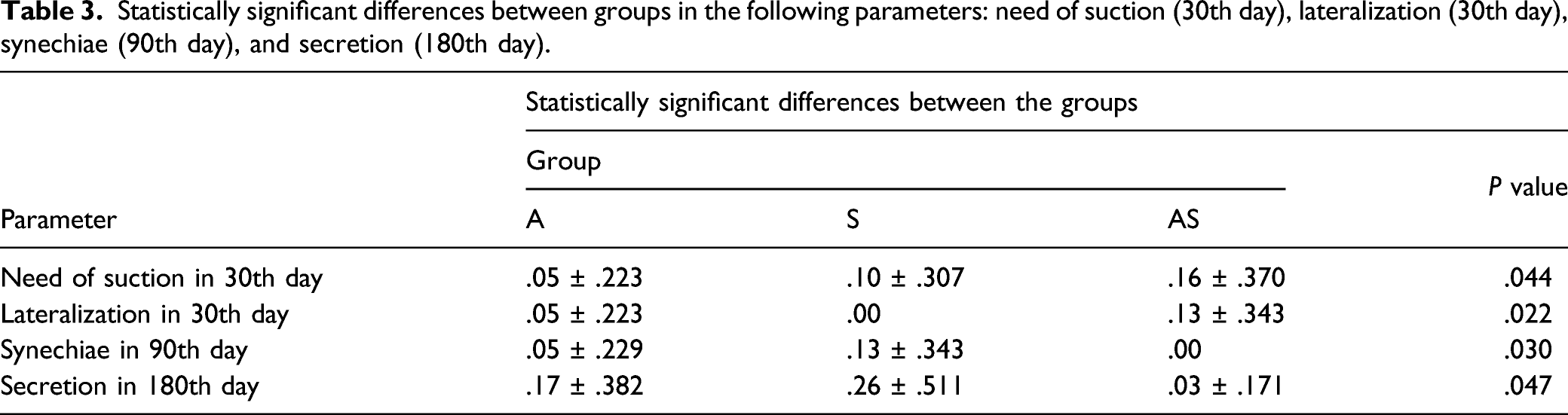
Statistically significant differences between groups in the following parameters: need of suction (30th day), lateralization (30th day), synechiae (90th day), and secretion (180th day).
Patients’ complaints
Statistical significance of patients complaints (feeling of facial pressure, nasal blockage, and sense of smell) in postoperative days.
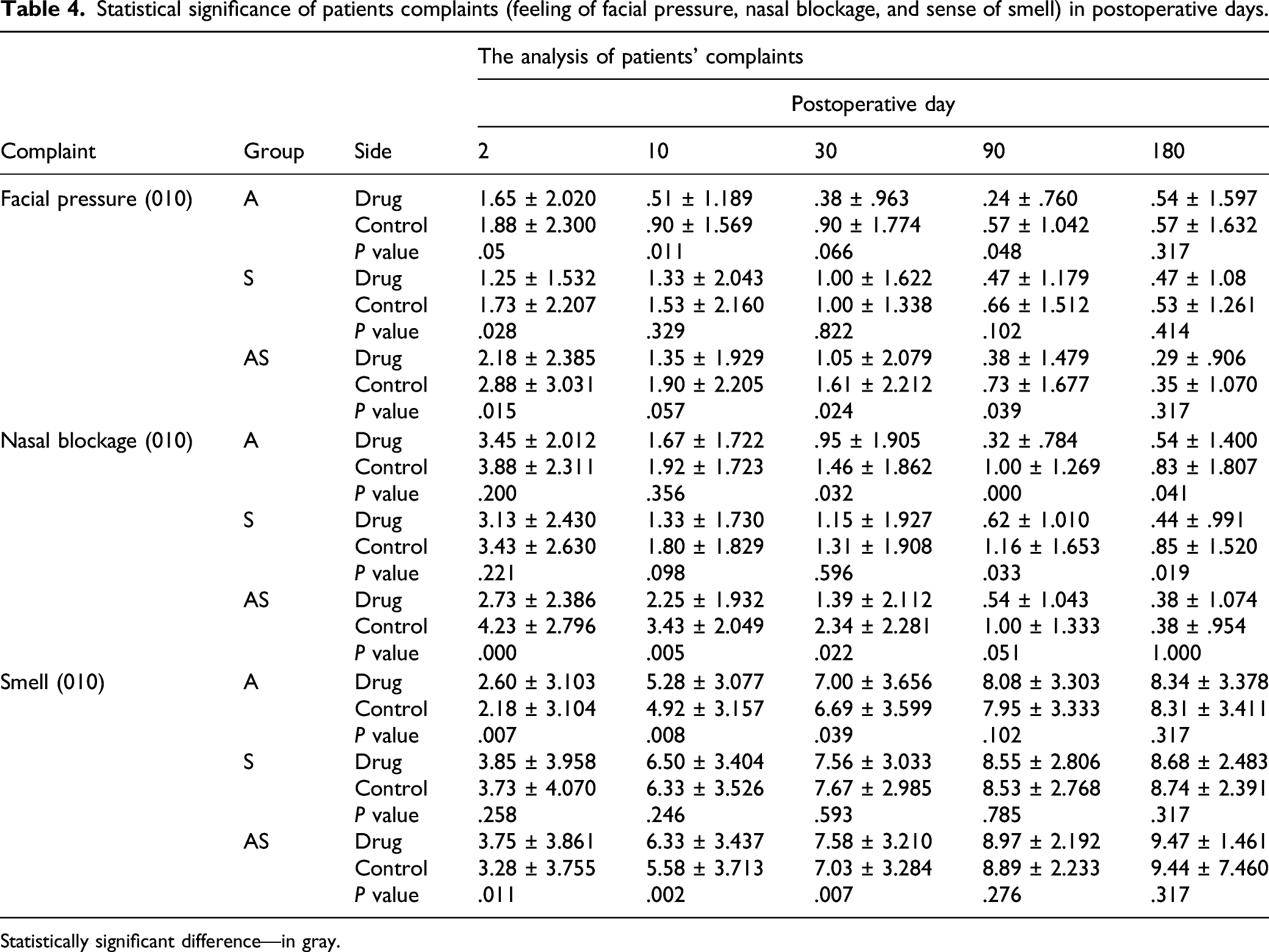
Statistically significant difference—in gray.
The study revealed that all the differences occurred in 3 parameters: facial pressure, nose blockage, and smell. No differences were observed in headache intensity, nasal pain, itching, or bleeding severity.
The analysis between groups showed 2 statistically significant differences: in nasal blockage on 10th day (P = 0.042)—the smallest in the steroid group, and in itching on second day (P = 0.041)—the rarest in the antibiotic group. No significant differences were observed between the remaining parameters.
Discussion
Success in outcomes of endoscopic sinus surgery in patients with chronic rhinosinusitis is highly dependent on the type of the postoperative care, in particular, focused on the avoidance of healing complications, such as postoperative bleeding, inflammation, infection, meatal obstruction, and synechiae formation.
The advantages and disadvantages of biodegradable nasal packing are still controversial. Comparing NasoPore and non-packing strategy in a double-blind, prospective, randomized trial, Kastl et al 7 revealed no differences in postoperative bleeding frequency, but significant reduction of pressure feeling in 2 and 3 postoperative day. Comparison of NasoPore and non-absorbable Merocel foam in prospective, double-blind, randomized trial accomplished by Shoman et al did not show differences in patients’ complaints, including pain, pressure, blockage, swelling, bleeding, or discomfort on removal. Neither did the amount of bleeding differ significantly. The only discrepancy was noticed in mucosal healing, having improved after 4 weeks in Merocel side, which disappeared in the 12th week. 21
The systematic review and meta-analysis of biodegradable nasal packings in endoscopic sinus surgery by Yan et al did not favor the use of biodegradable packing over no packing at all, but, in view of patient’s comfort, it is more advantageous when compared to non-absorbable. However, no beneficial effects on mucosal healing have been confirmed. 22
While the absorbable nasal packing itself does not totally eliminate the complications, additional interventions are frequently needed. One of them being the use of pharmaceutics within the packing.
Shikani et al. reported that even a single application of a drug inside the nasal dressing had a potential to change the local healing conditions. Using Corticosporin (suspension of polymyxin, neomycin, and hydrocortisone) for extending the Merocel package at the end of the endoscopic sinus surgery reduced the number of positive cultures after the surgery in 36% of patients. However, the frequency of recurrence of sinusitis during the study, although different in individual groups, did not reach statistical significance. 23
Predominance of gauze-applied, local admissions of high-dose corticosteroids over intranasal topical corticosteroid spray in prevention of recurrent nasal polyps was proven by Kang et al (ibid.) on a group of 32 patients, with recurrent nasal polyposis. Significantly higher recurrence rate was observed in the topical corticosteroid spray group. Moreover, neither blood pressure elevation nor cortisol and ACTH serum levels abnormalities in either of the groups were reported. 24 Topical admission of triamcinolone in nasal dressing was also investigated in randomized, double-blinded, placebo-controlled study, performed by Côté et al. Postoperative healing, rated in LundKennedy and POSE scores, was improved in the group of triamcinolone at the 7 and 14 postoperative day, and at 3 and 6 months after the surgery. The difference lacked statistical significance at postoperative day 28. 5
The present study attempts to combine the benefits of absorbable nasal dressing with mucosal healing improvement achieved by topical drugs, deposited inside the dressing. Decreased mucosal edema and secretion; reduced Lund-Kennedy score; and favorable influences on facial pressure, nasal blockage, and smell were most evidently seen in the group receiving the antibioticsteroid combination.
No significant bleeding, granulation, or delayed resorption of package incidents was observed, confirming the safety of drugNaso-Pore combination.
Nevertheless, the optimum concentration of the drugs remains to be clarified in order to achieve the best clinical results and avoid possible complications or side effects at the same time.
Conclusions
The results of this study revealed a significant improvement in postoperative healing and patient satisfaction after endoscopic sinus surgery using a combination of betamethasone-and-ciprofloxacin-impregnated bioabsorbable nasal dressing. Further research aimed at establishing the most satisfactory standards of the dressings used seems essential.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
