Abstract
Reconstruction of auricular deformities and facial scars after burns is a challenging undertaking for surgeons. Excessive scar tissue, a poor blood supply and the paucity of available skin are all substantial difficulties that should be considered before the operation. Expanded neck flaps provide comparatively larger and thinner flaps for the simultaneous treatment of auricular deformities and facial scars in burn patients. In this article, the authors introduced the use of an expanded neck flap as coverage tissue for ear reconstruction and face resurfacing in 2 burn patients. The operation consisted of 3 stages. In the first stage, the expander was implanted subcutaneously under the skin of the neck to create adequate skin and soft tissue. In the second stage, the expander was removed, and the expanded flap was transferred to cover defects on the auricle and face. The third operation to repair the reconstructed ear and thick flap could be performed according the willingness of the patients and surgeons. Esthetically satisfactory results were achieved in both of the patients. The flaps survived completely, and the skin color, texture, and flexibility were well matched to those of the peripheral tissue. Six months postoperatively, the flaps did not shrink, and subsequent contractures did not recur. Both of the patients experienced high satisfaction, and no adverse effects were detected.
Introduction
Nearly 11 million people suffer from burns severe enough to require medical attention throughout the world, and more than 300 000 die each year because of burns. 1 The advancement of medical technology in the field of burn care has led to a reduction in burn-related mortality and simultaneously brought about a challenge associated with tissue and organ reconstruction after burns. The face plays a pivotal role in maintaining a personal image as well as for identity recognition, while external ears are important in both maintaining facial symmetry and collecting sound waves. Therefore, facial scars and auricular deformities severely affect a patient’s physical and psychological health and pose a heavy economic burden due to repeated surgeries and long hospitalizations. 2
The methods of using autogenous costal cartilage or porous polyethylene as an ear framework are similar to those for treating congenital microtia,3-6 while auricle defects caused by burns remain a tough problem mainly because of the poor blood supply and reduced elasticity of the skin in and around the auricular region. In this study, we introduced our experience with the expanded neck flap in the simultaneous repair of facial scars and auricular deformities for the first time.
Surgical Techniques
The operation consists of 3 stages. Preoperative assessments of the surgical areas and the patients’ general condition were of equal importance when considering the risks and benefits of all steps. Realistic objectives should be set so that extremely high expectations can be avoided. The detailed design and procedures are explained as follows.
Stage 1: Expander Implantation and Water Inflation
Following general anesthesia induction, the patients were placed in a supine position. After a subcutaneous injection of tumescent fluid throughout the dissection area, a subcutaneous pocket was created above the platysma through a 4-cm incision line along the demarcation line between the facial scars and normal skin in the neck. The dissection area was 1-cm wider than the expander. The dissection area was checked carefully so that strict hemostasis was achieved, and then the expander was inserted horizontally into the expanded cavity. The infusion port was placed beneath the scarred skin on the face, and a tube used for negative pressure drainage was placed at the lowest point of the dissected cavity to prevent postoperative hematoma. The drainage tube was removed 3 days postoperation, and the sutures were removed after 7 days. Then, saline inflation was started 4 days later and was normally performed twice a week. The inflation volume varied each time and was controlled so that the patient did not complain of significant discomfort, such as skin pressure or significant pain, and the expanded skin did not become pale, which was mainly based on clinical experience and observation. The whole procedure took 2 to 3 months until the expanded flap was thought to be sufficient. A static expansion phase lasted for approximately 20 days after full expansion to prevent the expanded flap from developing contracture after the transfer and ensuring that the second stage of the operation would be performed.
Stage 2: Ear Reconstruction and Scar Repair
In the second stage, general anesthesia was administered, and the patients were positioned in the same way as in the first stage. Autogenous costal cartilage was harvested and carved into the ear framework according to the residual and contralaterally normal ear, which has been reported in multiple studies.3,4 After removing the expander, the expanded flap was longitudinally divided into 2 pedicled flaps: the anterior flap was rotated and advanced to repair the wound after resecting the facial scars, and the remaining flap was used to cover the ear stent during auricle reconstruction. The posterior flap should be prioritized, and the size of the flap must be large enough to cover the ear stent without tension. The ear framework was connected with residual ear cartilage using titanium wire after removing the hyperplasia tissue on the margin of the residual cartilage. Then, the posteriorly expanded skin flap was advanced to wrap the ear stent and cover the defects after excising the scars in the mastoid region. The area of the scarred lesion to be excised on the face should correspond with that of the remaining flap. If any scarred lesion remained unsurfaced, a further operation would be required to eliminate the residual defects. Two drainage tubes were placed beneath the donor site and posterior surface of the cartilage framework and then removed 5 days later. A light dressing and a soft neck collar were applied.
Stage 3: Reconstructed Ear Repair and Flap Debulking
A third operation to repair the reconstructed ear and thick flap could be performed 6 to 12 months after the second stage. The items of this stage may vary widely among individuals, usually including forming the tragus using the remnant ear, deepening the concha, and debulking the transplanted flap. If necessary, the uneven junction between the constructed and original auricular cartilage could be repaired.
Case Report
Two male patients with defects on the face and external ear underwent reconstruction with expanded neck flaps between 2014 and 2016. The reconstructive procedures, defect characteristics, and complications were collected and analyzed. All patients or their parents provided written informed consent. Both of the patients lost their right auricles and damaged their ipsilateral facial skin by flame burn injuries when they were just over 1-year old. One of the 2 patients (29 years old) had a 200-mL tissue expander inserted in his right neck, and after over 3 months of full expansion to 506 mL, the flap reached a satisfying dimension. After a 25-day static expansion duration, the second stage was conducted, and the expander was removed. The expanded flap was divided into 2 and transferred for ear reconstruction and face repair. This patient underwent follow-up by telephone for 6 months because of a long distance to the hospital. Good cosmetic outcome and high satisfaction were obtained during the follow-up period. The other patient was a 5-year-old boy who presented with deformity of the right ear accompanied by scars on the right side of the face. A 200-mL expander was implanted into his right neck region and filled to 500 mL over a 2-month period. The static expansion phase lasted for 20 days, and the second stage was performed. The third stage was conducted 1 year later. The flap survived completely without any complications, such as necrosis of the skin flap, poor wound healing, or stent exposure; after more than 6 months of follow-up, the contour and color of the flaps were esthetically satisfactory, and a normal cervicomental angle was obtained. Figure 1 shows the outcome of the 5-year-old boy.
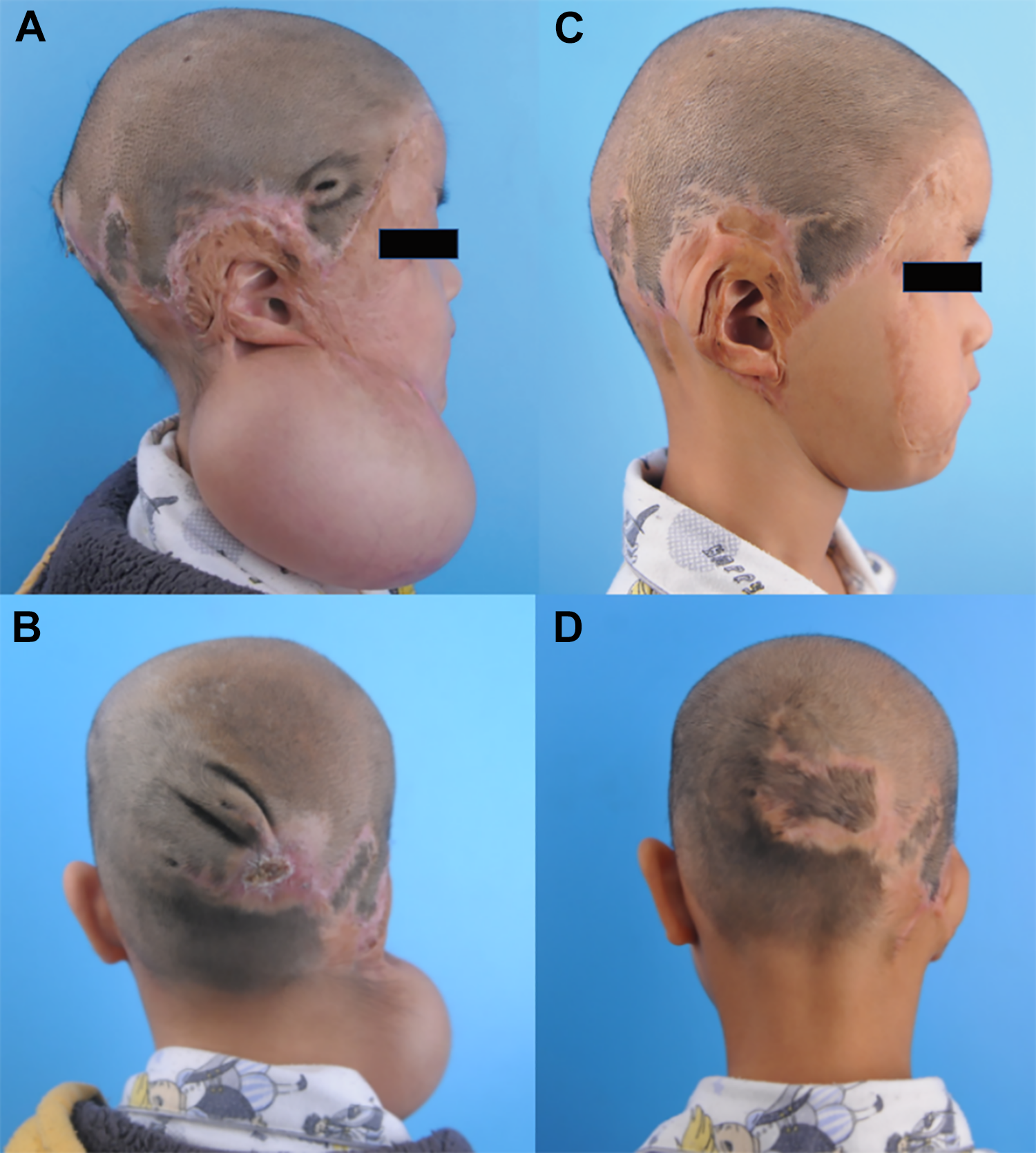
Ear reconstruction of a 5-year-old boy after a flame burn. A and B, The expander was filled to 500 mL, and the static expansion phase lasted for 20 days. C and D, Three months after the third stage.
Discussion
Facial burns greatly affect self-identity as well as social interactions, and the reconstruction of deformities caused by burns in the facial regions is related not only to aesthetic appearance but also to anatomic and social function. Involvement of the external ear is more complicated because of its intricate anatomical structure. When selecting donor flaps for facial resurfacing, the principle of “matching, large size, and thin thickness” should apply.7,8 Based on this principle, the color and texture of this flap should match those of the recipient region, the size should be sufficient to cover massive defects, and the tissue thickness should be thin enough to reveal the delicate contours of the facial region and permit emotional expression.
Multiple reconstructive methods have been used for the treatment of facial and auricular deformities caused by burns. The anterior thoracic regions provide optimum skin flaps due to their large dimensions, matched color and texture, and various flaps have been explored in this region. The deltopectoral and supraclavicular flaps are both highly suitable coverings for facial injuries and have been widely used in the treatment of cervicofacial scars. Deltopectoral flaps of various types have been viewed as workhorse tissues due to the readily available tissue source and minimal donor site morbidity.9,10 However, compulsive positioning may not be avoided because of the short length of the pedicle and the long distance between the donor and recipient sites, which increases both the chances of a delayed operation and patient suffering. The supraclavicular flap has a higher pivot point and longer pedicle, allowing for a farther transfer. This flap was reported for the first time in 1979 by Lamberty 11 and has been considered a suitable material for head and neck reconstruction.12,13 Skin transplants have limited application because of graft contractures and a mismatched texture and color with facial skin, although the operation method is much simpler.
Similar to ear reconstruction in patients with congenital microtia, burned ear reconstruction also involves the creation of a pliable framework and reliable soft tissue coverage. Although the use of autologous costal cartilage or prefabricated porous polyethylene for framework fabrication has been repeatedly reported, the poor blood supply and elasticity of skin around the auricular region make burned ear reconstruction one of the greatest challenges for plastic surgeons. The postauricular area or mastoid area is commonly reported for providing soft skin coverage in ear reconstruction. The advantageous properties of this flap, which include its adjacent position, thin thickness, and matched color, make it the best candidate as a skin flap donor for ear reconstruction. 4 However, severe scar contracture following burn injuries in this area may reduce the blood supply and elasticity and lead to a high incidence of complications. Although the superficial temporal fascia has also been used in burned ear reconstruction surgery for its reliable blood supply and minimal donor site morbidity,14,15 it is difficult to obtain an alternative material in case of framework exposure after removing the fascial flap. Free flaps, such as contralateral superficial temporal fascial flaps and radial forearm fascial flaps, have also been reported as good choices to cover the framework.16,17 However, the long learning curve of microsurgery may limit the usage of this approach. Moreover, the long operative duration and significant donor site morbidity cannot be ignored when using these flaps.
In this study, we performed ear reconstruction and facial scar repair simultaneously using an expanded neck flap in 2 patients. Over a follow-up time of more than 6 months, both patients achieved a good aesthetic appearance and high satisfaction. The skin in the neck is nourished by a subdermal vascular network formed by the facial artery, submental artery, posterior auricular artery, occipital artery, transverse cervical artery, and cutaneous branches from the superior thyroid artery.18-20 Therefore, the flap has a rich blood supply and can easily survive. The neck skin is similar to the facial skin in terms of texture, color, and elasticity. The short distance from the pivot point to the defect is another advantage, so this flap can be easily rotated and advanced to reach the target destination. The fact that neck skin is hairless makes it a suitable flap for both facial and auricular reconstruction. The application of the expander could provide a flap with abundant tissue volume, similar thickness and well-matched color to meet the needs for covering both the facial defects and the cartilage framework.
Several points should be noted during the operation. In our design, the incision for expander implantation should be made along inferior facial scars for an inconspicuous appearance. In this study, the expander was placed between the superficial layer of the platysma and subcutaneous fat of cervical skin so that the flap would not be easily pulled back by the platysma and the expansion rate would be effectively improved. When dissecting the expansion cavity, the subcutaneous fat in the neck should be carefully preserved to ensure the integrity of the subdermal vascular network. Furthermore, the fibrous capsules should be partly removed to encourage revascularization between the flaps and wound beds. The patient’s neck was usually secured to avoid removal of the flap and to protect the flap pedicle once the expanded flap had been transferred.
Supplemental Material
sj-jpg-1-ear-10.1177_0145561320963592 – Supplemental Material for Application of the Expanded Neck Flap for Face and Ear Reconstruction in Burn Patients: A Report on 2 Cases
Supplemental Material, sj-jpg-1-ear-10.1177_0145561320963592 consent_form for Application of the Expanded Neck Flap for Face and Ear Reconstruction in Burn Patients: A Report on 2 Cases by Peipei Guo, Bo Pan, Leren He, Haiyue Jiang, Qinghua Yang and Lin Lin in Ear, Nose & Throat Journal
Footnotes
Acknowledgments
The authors thank all the patients for their participation and permission in this study.
Authors’ Note
The study was approved by the Ethics Committee of the Plastic Surgery Hospital, Chinese Academy of Medical Sciences, and Peking Union Medical College.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by the Non-profit Central Research Institute Fund of Chinese Academy of Medical Sciences (3332019142); CAMS Innovation Fund for Medical Sciences (2016-12M-1-002); and The Foundation of Science and Technology Department of Sichuan Province (2018JZ0049).
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
