Abstract

Keywords
The pectoralis major myocutaneous flap (PMMF) is one of the workhorse flaps in reconstructive surgery and is essential in patients undergoing salvage surgery or for those who are not free flap candidates. Although total flap necrosis in PMMFs is uncommon, partial necrosis has been reported at rates up to 29%. 1 Accordingly, others have described modifications to the traditional PMMF-harvesting technique, with a focus on addressing vascular insufficiency.2,3 For instance, Makiguchi et al described the “supercharged” PMMF wherein the lateral thoracic vessels are cut and then anastomosed to cervical vessels to provide additional blood supply. 4 Like other modifications, this method attempts to avoid partial flap necrosis by improving vascular inflow.
In this report, we describe an anatomic variant of a PMMF and a solution to address vascular outflow. Specifically, we detail (1) a PMMF whose skin paddle was found to be reliant on intercostal perforator veins for venous drainage and (2) the use of a coupled intercostal perforator vein to correct early severe intraoperative venous congestion.
Case Presentation
This study (IRB00161557) was exempt by the Johns Hopkins Institutional Review Board. A 72-year-old man with a history of hypertension and emphysema presented with squamous cell carcinoma of the right retromolar trigone. This patient underwent a composite hemimandibulectomy and selective neck dissection. While he was originally scheduled to undergo reconstruction with a free flap, the patient developed severe hypotension intraoperatively, requiring fluid boluses and vasopressors for stabilization. Given these considerations, we proceeded with a PMMF.
While the pectoralis muscle was elevated, a 1.5-mm intercostal perforator vein was encountered and ligated. Within minutes, the cutaneous paddle turned mottled and purple, with brisk, dark bleeding on pinprick. However, there was clear venous outflow from the pectoral vein and a strong doppler signal along the pectoral branch of the thoracoacromial artery. The compromised skin paddle appeared to directly overlie the clipped intercostal perforator vein. This was seen prior to sacrifice of the lateral thoracic pedicle, which was ligated to increase the reach of the PMMF.
The decision was made to achieve a second source of venous outflow through the clipped perforator vein. Hence, the intercostal vein was anastomosed to the common facial vein with a 1.5-mm venous coupler (
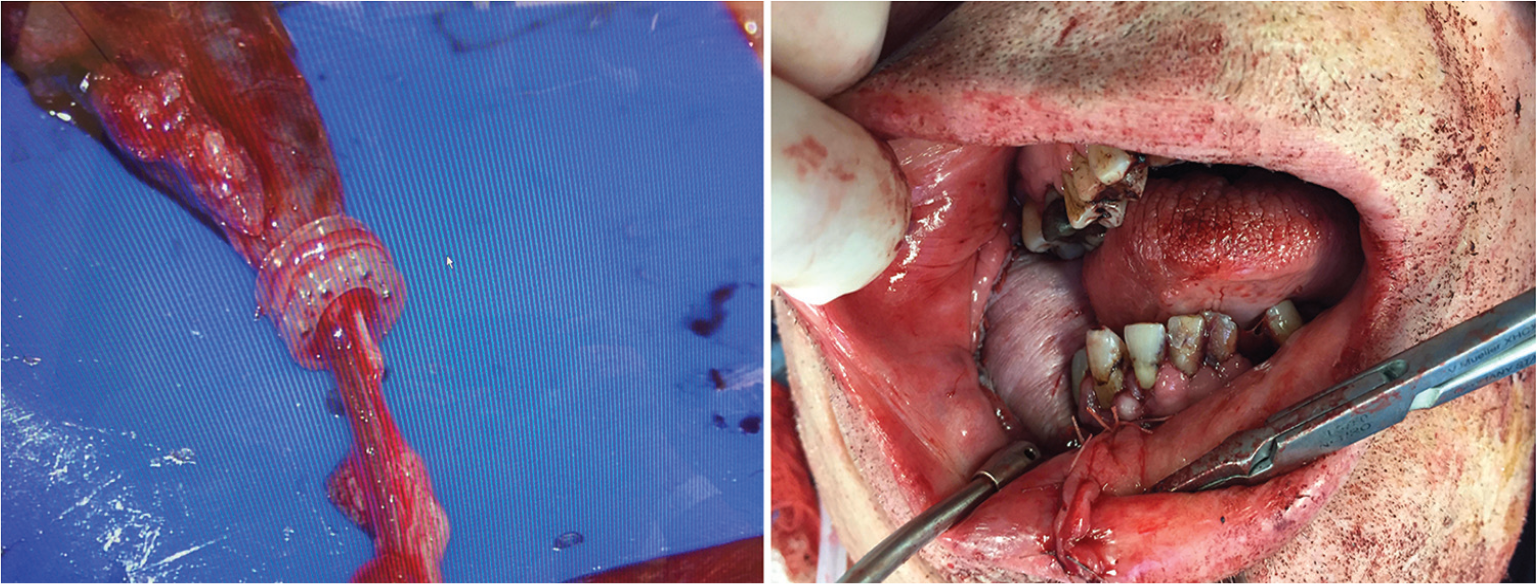
(left) Coupler anastomosis of the common facial vein (4-mm diameter) to the intercostal perforator (1.5-mm diameter). Note successful anastomosis despite the size mismatch. (right) Pectoralis major myocutaneous flap after anastomosis and inset with improved venous outflow.
Discussion
Partial flap necrosis of PMMFs is predominantly related to vascular insufficiency stemming from poor blood flow to the distal aspect of the flap. This may be due to the variable vascularization of the PMMF, combined with the need to harvest sufficient tissue caudally to obtain a sufficient arc of rotation. The pectoral branch of the thoracoacromial artery supplies the upper aspect of the PMMF, while the lateral thoracic artery and anterior intercostal branches of the mammary artery supply the skin territory overlying the lower aspect of the PMMF. In our case, however, vascular compromise was due to dominant venous outflow from an intercostal perforating vein.
Vascular variations have led to modifications of flap-harvesting technique. Kiyokawa et al and Rikimaru et al designed a skin paddle that recruited a large number of perforating branches to maximize blood flow to the distal and marginal aspects of the flap.2,3 However, these variations are often not practical for head and neck reconstruction due to limitations in the arc of rotation. This led to implementing additional strategies, such as supplemental arterial anastomoses as in the “supercharged” PMMF described by Makiguchi et al. 4
The majority of the pectoralis muscle’s venous drainage is achieved by venae comitantes associated with the pectoral branch of the thoracoacromial artery. However, the skin overlying the muscle drains through venules accompanying arterial perforators.
5
In our case, the reliant venous outflow to the skin paddle was a single dominant intercostal perforator directly underlying the skin paddle. This marked a distinct watershed area or different angiosome from the thoracromial system, requiring unique intraoperative maneuvers to reestablish flow to this dominant intercostal venous drainage system, with a “superdrained” flap (
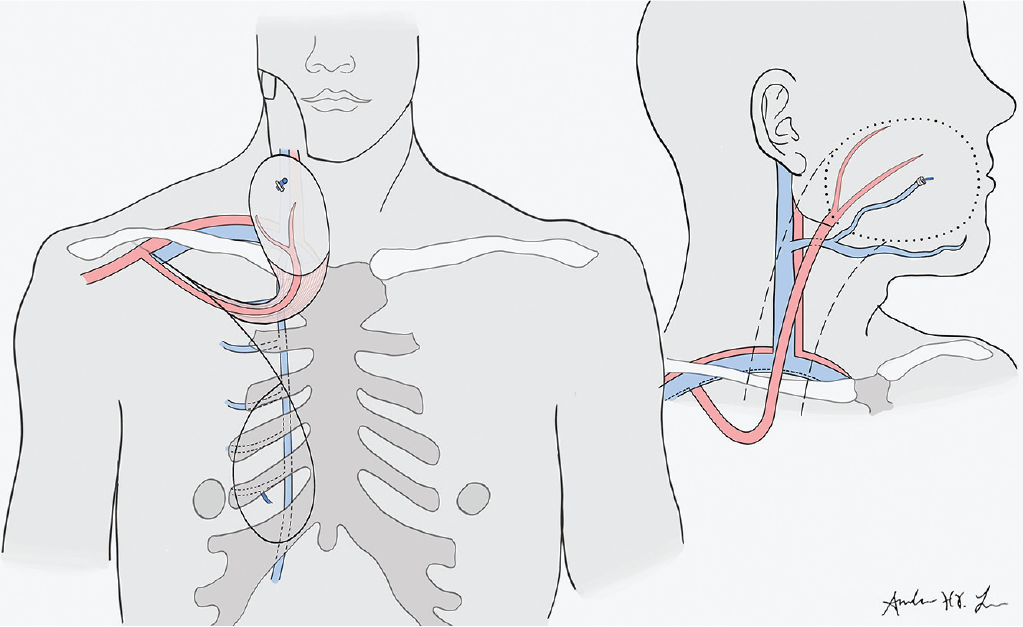
(left) Representative illustration of venous drainage of the pectoralis flap from an intercostal perforator, draining to the internal thoracic vein. (right) Inset supercharged pectoralis major myocutaneous flap with anastomosis of the intercostal perforator to the common facial vein.
Author Contributions
Disclosures
Footnotes
No sponsorships or competing interests have been disclosed for this article.
