Abstract
The limited physical and mechanical properties of polymethyl methacrylate (PMMA), the current gold standard, necessitates exploring improved denture base materials. While three-dimensional (3D) printing offers accuracy, efficiency, and patient comfort advantages, achieving superior mechanics in 3D-printed denture resins remains challenging despite good biocompatibility and esthetics. This review investigates the potential of innovative materials to address the limitations of 3D-printed denture base materials. Thus, this article is organized to provide a comprehensive overview of recent efforts to enhance 3D-printed denture base materials, highlighting advancements. It critically examines the impact of incorporating various nanoparticles (zirconia, titania, etc.) on these materials’ physical and mechanical properties. Additionally, it delves into recent strategies for nanofiller surface treatment and biocompatibility evaluation and explores potential future directions for polymeric composites in denture applications. The review finds that adding nanoparticles significantly improves performance compared to unmodified resins, and properties can be extensively enhanced through specific modifications, particularly silanized nanoparticles. Optimizing 3D-printed denture acrylics requires a multifaceted approach, with future research prioritizing novel nanomaterials and surface modification techniques for a novel generation of superior performance, esthetically pleasing, and long-lasting dentures.
Keywords
Introduction
Polymethyl methacrylate (PMMA) has long dominated the landscape of denture fabrication, serving as the material of choice for patients with complete or partial tooth loss. While widely accepted, conventional compression and injection molding techniques have inherent limitations. Multiple appointments, bulky prostheses for maxillofacial patients, increased susceptibility to bacterial colonization, and noticeable polymerization shrinkage prompted extensive research efforts to overcome these disadvantages.1,2
Digital dentistry has revolutionized the field, presenting novel solutions to the shortcomings of traditional techniques. In 1990, Goodacre introduced computer-aided design (CAD)-computer-aided manufacturing (CAM) as a transformative technology, encompassing two primary approaches: subtractive and additive. 3 Initially, the subtractive technique prevailed, but its drawbacks prompted the emergence of the additive process. This advanced method, known as the CAM step, builds objects layer by layer, making it a versatile tool across medical, engineering, and dentistry domains. 4 Unlike subtractive approaches, the additive technique leverages three-dimensional (3D) model data to join materials precisely, facilitating the utilization of diverse materials like polymers, metals, and ceramics without limitations. 4 Stereolithography, employing UV light, is a commonly used printing method offering impressive resolution, enabling the precise printing of small items (50 mm). Additionally, the rapid photo-curing process contributes to efficient model production. 5
The 3D-printing technology can enhance denture base resin by incorporating biocompatible resins with enhanced strength and flexibility. It also allows the integration of miniaturized, cheap, and sensitive sensors into denture base resins, thus monitoring bite force and distribution, pH for tracking oral health, and the condition of the denture itself; however, confirming the safety and biocompatibility is necessary. 6 The 3D-printing technology's self-contained and user-friendly system allows the creation of customized porous structures through which self-healing polymers containing nanoparticles can be passed. 7
While 3D printing boasts numerous advantages, the inherent qualities of the resins pose challenges compared to conventional materials like heat-cured acrylic and CAD-CAM resin.8,9 To address these limitations, researchers have turned to nanoparticle reinforcement. Nanoparticles hold immense potential due to their exceptional durability and corrosion resistance. Furthermore, manipulating their size can further optimize their properties. 10 Polymeric nanocomposites, incorporating nanoscale components into the polymer matrix, can impart novel physical, mechanical, and biomedical characteristics.11,12
Including various nanofillers into 3D-printed denture base resins, often through grafting techniques, has significantly improved material properties.13,14 The nanoparticles’ type, structure, and size significantly influence the resulting composite 15 characteristics. 15 While nanomaterials often possess exceptional physical properties (e.g. high density), their mechanical attributes can be lacking. Extensive research in nanocomposites focuses on addressing this issue, aiming to enhance physical and mechanical properties. 16
This literature review investigates the vast body of research exploring the reinforcement of 3D-printed denture base resins with nanoparticles. It examines the modified properties of the resulting composites, surface treatment, processing techniques, biocompatibility assessment, and possible future recommendations for polymeric 3D-printed denture base resin composites.
Coupling agents
The growing field of 3D-printed denture base materials holds immense promise for revolutionizing dental prosthetics. However, optimizing their mechanical properties and performance requires meticulous attention to the interface between the organic resin matrix and inorganic fillers. This critical junction, often reinforced by coupling agents, is pivotal in transferring stress, influencing water absorption, and ultimately determining the material's long-term functionality. 17
A positive correlation between nanofiller concentration and the mechanical characteristics of composite resins has been emphasized. Increased filler content typically enhances wear resistance and improves physical properties.14,18 However, achieving uniform dispersion and preventing aggregation throughout processing and service life remains a significant challenge for effective nanofiller utilization.5,16
Fortunately, advancements in surface modification techniques offer a valuable solution to the dispersion problem. By tailoring the surface chemistry of inorganic fillers (e.g. silanization), improved filler-resin bonding and overall composite properties have been accomplished.19–21
The hydrophobic nature of organic resins demands hydrophilic fillers to achieve optimal adhesion. Silane coupling agents, a category of organosilicon compounds, address this disparity by binding to hydroxyl groups on inorganic fillers and organic polymer chains.5,22 This molecular bridge fosters enhanced bonding strength, improved dispersibility, and, ultimately, reinforced mechanical properties within the composite resin.5,23 Figure 1 shows the three reaction sites of the titanate treatment mechanism, while the silane treatment mechanism shows one reaction site. 10

(a) The three reaction sites are depicted in the titanate-treated mechanism. (b) One reaction site is illustrated by silane treatment. 10
Multiple studies have documented the multifaceted benefits of surface modification. For instance, Kamonkhantikul et al.
24
observed superior antifungal properties, improved flexural strength, and reduced
Coupling agents are critical in enhancing the performance and functionality of 3D-printed denture base resins. Through surface modification techniques like silanization and exploring alternative agents like titanium coupling agents (TCAs), researchers are paving the way for a new generation of durable, high-performing denture materials. Continued research in this area holds immense potential for improved patient satisfaction and longevity of dental prosthetics. Figure 2 shows Fourier-transform infrared spectroscopy (FTIR) analysis of silane-coated and nonsilane-coated titanium dioxide nanoparticles (TiO2 NPs). 25

FTIR analysis of (a) silane-coated TiO2 NPs and (b) nonsilane-coated TiO2 NPs. 25 FTIR: Fourier-transform infrared spectroscopy; NPs: nanoparticles.
Nano additives reinforcement
Despite the rising prominence of 3D printing in dentistry, in vitro investigations focusing on the material properties and dimensional accuracy of 3D-printed denture bases remain scarce. This impedes the optimization of this promising technology in clinical settings. While 3D-printed denture base materials demonstrate considerable potential as an alternative to conventional heat-cured resins, further advancements are needed to realize their capabilities fully. 13
Nanotechnology presents a compelling avenue for enhancing the properties of 3D-printed dentures, leading to potentially longer service life and improved patient satisfaction. This approach offers a solution to address the limitations inherent in traditional materials. Several studies have already explored the incorporation of various nanoparticles into denture acrylics, resulting in demonstrably improved physical and mechanical characteristics of the 3D-printed resin.13,18,26,27
Despite the improved mechanical and physical properties of nanoparticle-reinforced denture base resin. The results showed that this reinforcement can be affected by the versatility of nanoparticles in structure, surface chemistry, type, concentration, aggregation rate, and nanoparticle surface treatment. A systematic review in 2021 showed that nanoparticle agglomeration negatively impacts denture base material's properties. 28 Kango et al. 29 mentioned the importance of standardization of nanoparticle production methods and characterization of nanoparticle-polymer matrix interaction, which are essential for consistent material behavior.
In fact, integrating nanomaterials in denture base resins faces significant challenges in clinical applications. Highlighting the need for rigorous testing into the long-term biocompatibility, mechanical characteristics, potential toxicity, and other physical and chemical features of the newly innovated nanomaterials to ensure patient safety. 30 Additionally, applying these nanoscale materials should coincide with the principles of green nanotechnology and balance potential benefits with potential social costs, including environmental, public, and occupational health risks. 31 Umapathy et al. 31 showed that silver nanoparticles in resin-based composites can leach rapidly, and the oral epithelium may become hypersensitive to nanoparticles. Therefore, future in vivo experimentation would be essential for evaluating the long-term biocompatibility of such novel composites.
Innovative denture base materials offer the potential for improved patient experience and denture performance, but Hooshiar et al. referred that the initial cost might be higher; these include increased material costs due to the complexity of manufacturing processes, the potential for increased lab fees due to the need for technician training, and specialized equipment for processing or finishing. 32 However, Weighing the cost implications against the potential advantages for patients and dental professionals is important. This review proposes consideration of innovative denture materials’ cost-effectiveness for future research and clinical application.
Before considering the nano additives’ enhancements in clinical practice, several key points need to be considered, including the enhanced material's properties, such as durability for long-term performance, chemical stability inside the patient's mouth, and biocompatibility for ensuring tissue safety. Toxicity occurs from nanosized fillers leaching from the material, affecting surrounding tissue cells. 30 Therefore, further research is crucial to clinically ensure these innovative materials’ long-term safety and efficacy, evaluating their mechanical stability and aging characteristics over extended periods.
Conclusively, the effectiveness of these nanoscale additives hinges on numerous factors, including their size, type, shape, and concentration. Consequently, further research is necessary to investigate the potential of additional fillers for reinforcing 3D-printed denture base resin. Such investigations should prioritize a comprehensive understanding of the complex interplay between nanoparticle characteristics, resin composition, and resulting material properties. 33
Zirconia nanoparticles
A promising recent approach for improving the properties of acrylic resins involves incorporating zirconium oxide (also known as zirconia, ZrO2) as a filler. Extensive research confirms its biocompatibility, making it an excellent option. Moreover, zirconia outperforms metal fillers in esthetics, leading to a more natural look and offering a clear advantage.34,35
Studies have found that flexural strength, impact strength, and hardness can be significantly enhanced by incorporating fillers into the resin.27,36–38 The scanning electron microscope analysis shows that both denture-base resins produced in 3D (ASIGA and NextDent groups) exhibited a uniform and effective dispersion of nanoparticles within the resin matrix at lower concentrations. In comparison, some particle clusters were evident on the surfaces at greater concentrations, as shown in Figure 3. 27 However, Khattar et al. suggested that a lower concentration would be preferable for optimal optical properties. Further research to optimize ZrO2NP use for dentures is needed. 18

SEM images of the ASIGA group with varying ZrO2NP concentrations (0, 0.5, 1, 3, and 5 wt.%). (a) PMMA, (b) 0 wt.% ASIGA, (c) 0.5 wt.% ASIGA, (d) 1 wt.% ASIGA, (e) 3 wt.% ASIGA, and (f) 5 wt.% ASIGA. Scale bars represent 100 µm. 27 SEM: scanning electron microscope; PMMA: Pure polymethyl methacrylate; NPs: nanoparticles.
Hada et al. studied the impact of adding highly translucent zirconia filler to 3D-printed denture base resins. They used different concentrations of (3%, 5%, and 10%) and found that flexural strength steadily increased to a 5% zirconia concentration, making the dentures stronger. Beyond 5%, the strength plateaued, suggesting no further benefit at higher concentrations. 38 This finding aligns with the Alshaikh et al. 27 study, which observed that ASIGA resin's strength is directly correlated with ZrO2NP concentration. In contrast, NextDent resin peaked in strength at a 1% ZrO2NP concentration, with no significant difference between 3% and 5% additions. This difference in flexural strength could be ascribed to the varying compositions of the 3D-printed resins. While zirconia strengthens dentures, finding the optimal concentration is crucial. Future research should investigate different resin–zirconia combinations to pinpoint the ideal maximum strength and durability ratios.
Adding zirconia nanoparticles (ZrO2 NPs) to 3D-printed dentures makes them more challenging but less translucent. Figure 4 shows how NextDent resin becomes less translucent as ZrO2NP concentration increases. 18 Previous studies also found that various concentrations of ZrO2, Al2O3, and SiO2 fillers had an unpredictable negative impact on transparency. It's all about the physical properties of ZrO2 NPs and how they're distributed within the material. Future research can explore alternative materials or optimize ZrO2 NP distribution to achieve strength and esthetics in 3D-printed dentures.39,40

Demonstrative photographs of the NextDent resin samples arranged according to ZrO2 NP concentration. 18 NPs: nanoparticles.
Adding ZrO2 NPs to 3D-printed resin resulted in a notable rise in roughness (Ra). 41 The outcomes results align with previous studies.42,43 Compared to all the 3D-printed resins, heat-polymerized PMMA showed the lowest surface roughness. 27 This discrepancy could be attributed to the layer-by-layer printing technique, which could have played a role in the increased Ra. Furthermore, the specimens’ surfaces were roughened because the printing orientation (90°) produced more compact sequential edges. 14
Khattar and colleagues have illuminated the promising prospect of incorporating ZrO2 NPs into 3D-printed denture resins to combat microbial growth without compromising cell viability who reported a substantial decrease in
Al-Sammraai et al. investigated the impact of incorporating nano-sized zirconia (nanoZrO2) particles on both the diametral compressive strength and the adaptation properties of 3D-printed denture base resin. Their findings revealed a significant difference in these properties. While denture adaptation increased with the addition of nano ZrO2, the mean diametral compressive strength decreased at 2% and 3% weight percentages of the nanoparticles. 34
Further clarifying these mechanisms of action, particularly at varying ZrO2 NP concentrations and surface modifications, warrants further investigation.
The aforementioned studies highlighted the potential of ZrO2 NPs for improving the hygienic properties of 3D-printed dentures and the importance of maintaining biocompatibility. Aati and colleagues confirmed that including ZrO2 NPs does not adversely affect the resin's biocompatibility. 44 This opens the door for exploring the clinical translation of these antimicrobial 3D-printed denture materials, potentially leading to significant advancements in oral hygiene and patient comfort.
Titanium dioxide nanoparticles
The incorporation of TiO2 NPs into acrylic denture base resin used in 3D printing has been widely investigated.19,25 The focus is improving fundamental material properties like hardness, fracture toughness, flexural strength, and antibiofilm activity. This approach aims to create more vital, resistant, hygienic dentures for improved patient comfort and longevity.
Even though adding TiO2 NPs offers exciting possibilities for combating fungal infections in dentures, a delicate balance is needed, demonstrating that concentrations between 0.4% and 2.5% effectively suppress
The synergistic effects of incorporating TiO2 and polyetheretherketone (PEEK) into denture base resin that is 3D manufactured have been explored. 5 The composite demonstrated superior antibacterial activity to pure PMMA, suggesting a potential TiO2-mediated mechanism against dental pathogens. Additionally, enhancement in mechanical strength was observed within a specific range of (1 wt.% TiO2 and 1–3 wt.% PEEK), highlighting the critical ratio for optimizing this property without compromising others. Mainly, the PMMA-TiO2 (1%)-PEEK (1%) composition arose as a promising applicant for functional dental restorations due to its unique mechanical robustness, improved antibacterial efficacy, and minimal cytotoxic effects, necessitating further investigation for clinical applications. 5
In the meantime, Altarazi et al.
13
verified a promising approach for preventing fungal infections in 3D-printed dentures by including TiO2NPs into the denture base resin, creating a biocompatible composite material. These nanoparticles effectively inhibit the growth of
A comprehensive investigation of the effects of incorporating TiO2 NPs into NextDent 3D-printed denture base resin observed noteworthy improvements in various properties relative to the unmodified material regarding solubility, Vickers hardness, impact strength, and flexural strength/modulus. Remarkably, the ideal concentration for these improvements was 0.1 wt.% TiO2NPs. While saliva sorption and Marten's hardness remained statistically unaffected. Increasing TiO2 concentration beyond 0.1 wt.% led to a decline in properties. 25 This finding aligns with previous research on incorporating several types of NPs into 3D-printed dental resins.5,14,47 The decrease at higher concentrations is ascribed to nanoparticle clustering inside the resin matrix, generating stress spots and deteriorating the material's internal structure.12,48
AlGhamdi and colleagues demonstrated a distinct trade-off relationship between flexural strength and stiffness/hardness in their study. While flexural strength increased with TiO2 NP concentration, exceeding 2 wt.% resulted in a decline in elastic modulus and hardness, underscoring the importance of identifying the optimal TiO2 NP dosage that balances sufficient strength with adequate stiffness and hardness for specific application requirements. 49
Longer curing times strengthen and harden 3D-printed denture resins; benefits show up to 120 min, though results might plateau after 60 min.25,49,50 Though postcuring and TiO2 NPs offer promising opportunities to improve 3D-printed denture quality, further investigation is crucial. Other researchers explored shorter curing times and observed strength improvements, suggesting further optimization potential. 51 A comprehensive understanding of mechanical, biological, and physical characteristics is needed before recommending these materials for clinical use. 51
Zinc oxide nanoparticles
The distinct biological, optical, chemical, electrical, biocompatible, economical, nontoxic, and environmentally stable properties of ZnO nanoparticles have sparked significant interest, making them a versatile choice among inorganic nanoparticles. 52
A study conducted by Al-Douri and coworkers demonstrated a dose-dependent relationship between the concentration of ZnO nanoparticles and the flexural strength of resin. The 3% ZnO group achieved the highest value (126.11 ± 5.25 MPa), statistically significant compared to the control group (111.43 ± 4.78 MPa). Interestingly, exceeding 3% (4% group, 106.33 ± 5.42 MPa) led to a decline in strength 53 aligning with the observations of Khan's research, which reported that incorporating high concentrations (5–20%) of ZnO nanoparticles in PMMA denture base resin led to a reduction in flexural strength. These results suggest a potential upper limit for optimal nanoparticle inclusion, beyond which agglomeration or other factors might negatively impact the material's mechanical properties. 54
The observed increase in flexural strength within the experimental groups can be attributed to the multifaceted role of the incorporated nanoparticles. They act as fillers, effectively plugging micro-voids and preventing crack initiation within the resin matrix. 55 Secondly, their proper dispersion allows them to infiltrate and interact seamlessly with the polymer chains, restricting their mobility and enhancing the material's flexural strength. 56
Enhancement of flexural strength with ZnO addition was approved by Salahuddin's investigation that found adding ZnO nanoparticles to PMMA composites improved flexural strength at low concentrations (<1%). Still, at 4% concentration, flexural strength decreased due to reduced cross-sectional area and stress concentration. 57 Incomplete resin wetting and interference with the polymer matrix integrity also contributed to the decline in flexural strength. 58
Al-Douri et al.'s findings show no significant impact on hardness, even with nanoparticle addition. 53 This contradicts other reports that observed increased hardness.57,59 They confirmed a decrease in surface roughness with added ZnO as seen in Figure 5, 53 matching previous research. 60 However, this opposes Cierech et al.'s work, which saw no difference in roughness. 61
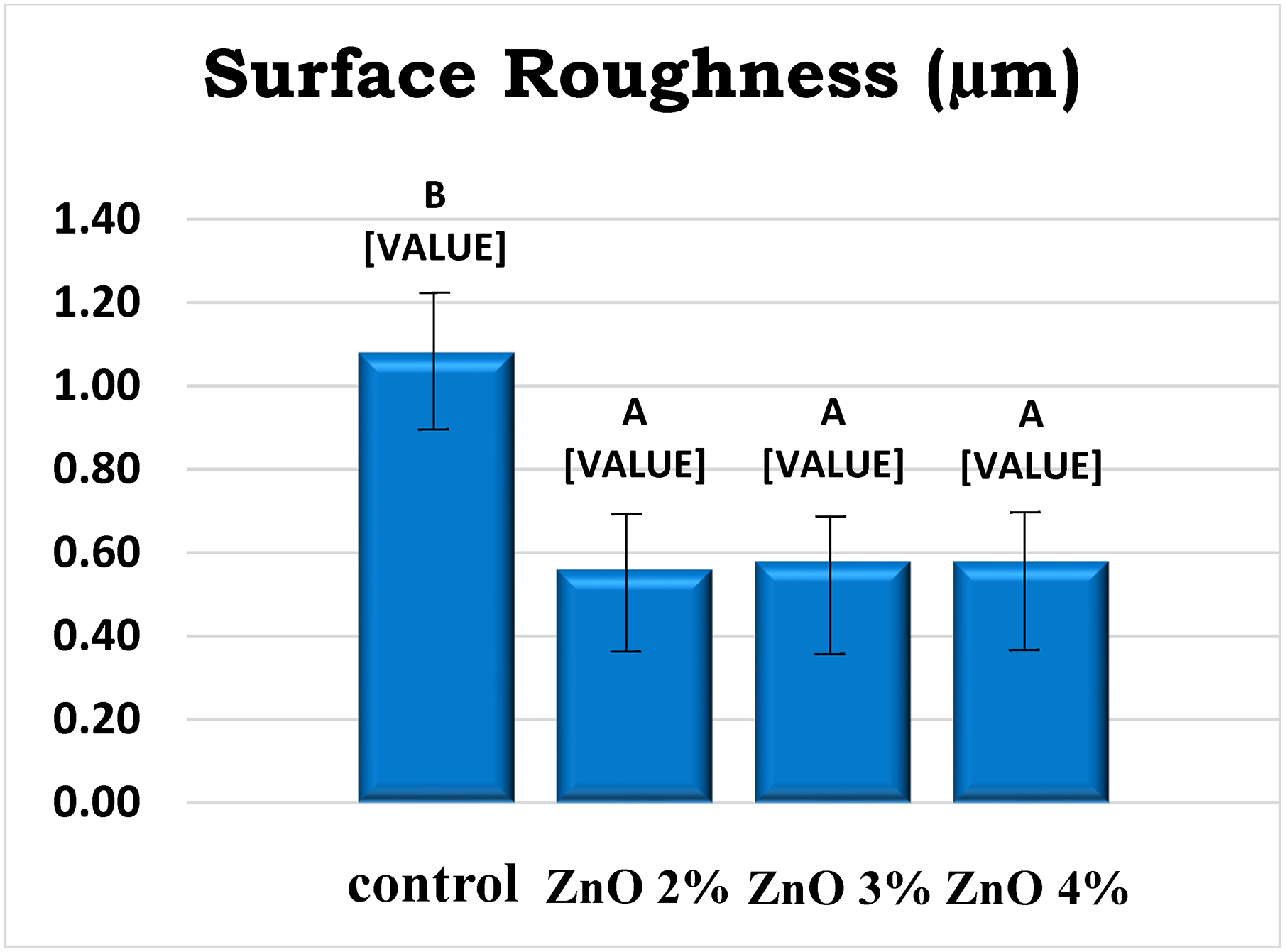
Duncan's multiple surface roughness range tests. 53
Harie Priya and Muthukumar 2 addressed a challenge of 3D-printed resins, by adding microscopic porospheres and zinc oxide particles; they significantly improved the material's ability to withstand compressive strength. This research aligns with Alshaikh et al.'s 27 observations and opens doors for developing stronger and more versatile 3D-printed materials for various applications.
Silver nanoparticles
Silver nanoparticles (Ag NPs) have been shown to provide a broad-spectrum antibacterial effect on both gram-positive and gram-negative organisms. 62 Chen and colleagues created a unique PMMA composite resin that has improved biocompatibility, antibacterial activity, and mechanical characteristics. The microscopic analysis confirmed the even distribution of cellulose nanocrystals (CNCs) and Ag NPs, which contributed to significant improvements in strength. Tests showed both excellent biocompatibility and potent antibacterial activity. Notably, the 0.1 wt.% CNCs-Ag NPs composite (PMMA-CNCs-AgNPs-0.1) exhibited the optimal balance of properties due to the homogenous distribution of Ag NPs. This promising material holds potential as a new functional dental restoration material with broader medical applications. 26
Aati et al.'s study sheds light on a novel strategy for optimizing 3D-printed denture base resin. Integrating silver nanoparticles within mesoporous silica carriers improved hardness, crack resistance, and, potentially, antimicrobial properties. While higher nanoparticle concentrations slightly impacted flexural strength, the overall results highlight the potential of this innovative material for creating stronger, cleaner, and longer-lasting dentures.
63
Figure 6 confocal laser scanning microscopy (CLSM) images reveal the viability of

CLSM images of
They also revealed that while water absorption remained unaffected, the presence of fillers slightly decreased water solubility, suggesting better material stability in aqueous environments. Interestingly, surface roughness increased significantly at Ag/MSN concentrations above 1.0 wt.%, potentially due to the increased particle density. However, this roughness proved advantageous, leading to a dramatic reduction in biofilm formation by
Silicon nanoparticles
Gad et al. 14 studied adding silicon nanoparticles (SNPs) to 3D-printed denture bases resin in 2022. Compared to unmodified resin, the nanocomposite resin showed notable gains in hardness, impact strength, and flexural strength. Notably, surface roughness remained unaffected. Despite a slight decrease in performance under thermal cycling, the enhanced mechanical properties and long-term durability suggest great potential for this innovative material in future denture applications. 14
Compared to conventionally heat-polymerized resins, the 3D-printed resin with 0.25% SNPs exhibited a remarkable and persistent increase in flexural strength, even after thermal cycling. After thermal cycling, the flexural strength of all 3D-printed/SNP groups exceeded the ISO recommendation of 65 MPa, effectively removing limitations on their clinical use. This remarkable improvement can be attributed to the unique characteristics of SNPs, including their nanoscale size, large surface area, and uniform distribution within the resin matrix facilitated by the silanization process. 16
Gad et al.'s study opens doors for utilizing SNPs to improve the impact resistance of 3D-printed resin. While higher concentrations might initially offer more significant benefits, thermal cycling reveals that even the lower SNP doses significantly enhance impact strength compared to unmodified resin. 14 This finding, consistent with Mangal et al.'s work on nano-diamonds, strengthens the case for using SNPs as a promising strategy to create more robust 3D-printed biomedical appliances. 64
Understanding surface hardness as a crucial indicator of denture strength and stability is vital. Studies reveal that 3D-printed resins currently show lower hardness than heat-treated alternatives.14,65 This highlights the need for further optimization of 3D-printed resins to ensure their ability to withstand daily wear and tear and maintain hygienic properties for long-lasting function and patient comfort.
Essential oil microcapsules
Microencapsulation offers a transformative technology for encasing core materials within functional shells, preserving their inherent properties while enabling controlled delivery to specific sites and times. 66 This holds immense promise for diverse applications, particularly in biomaterials. Natural essential oils have garnered significant interest among potential core materials due to their well-documented anesthetic, antiseptic, antimicrobial, and anti-inflammatory properties. 66
The feasibility of incorporating microcapsules containing plant essential oils within 3D-printed denture base resins has been explored in a recent study, aiming to investigate the resulting mechanical properties. 67 While the study revealed a decrease in flexural strength and surface roughness due to the microencapsulation (MCP) incorporation, flexural modulus and Vickers hardness remained largely unaffected. These findings offer valuable insights into the potential trade-offs and considerations when integrating therapeutic essential oils into 3D-printed biomaterials. 67
Nanocarbon
Nanotechnology encompasses various branches, and nano-carbon is a prominent one among them. However, using nanocarbon to enhance PMMA is rare due to its cytotoxic nature, challenging handling and polishing, and lack of esthetic appeal. 10
Mohamed et al. indicated that denture base resins created using 3D printing exhibit diminished mechanical properties compared to conventional and milled resins. This presents a significant obstacle to their widespread use in clinical applications. 68 A decrease in the flexural strength of the 3D printed resins suggests that the polymerization technique is crucial in the final material properties.14,65,69 Further investigation is required to optimize the curing process to balance density and flexibility in this material. 70 Despite the advantages of 3D-printing resin, Keble et al. highlighted their limitations regarding air inclusions and inherent mechanical properties. Addressing these weaknesses through advanced printing techniques or alternative curing methods holds immense potential for enhancing the strength and reliability of 3D-printed resin parts.69,71
The incorporation of silane-coated nanoglass particles and multiwalled carbon nanotubes (MWCNTs) into 3D-printed resin was studied by Mohamed et al. in 2023. Different percentages of these fillers were utilized, including a control group with no modification. Resin modified with 0.25 and 0.5 wt.% nanoglass particles, and resin modified with 0.25 wt.% and 0.5 wt.% MWCNTs and a combination group with 0.25 wt.% of both fillers were utilized. The group with 0.5% nanoglass exhibited the most significant decrease in properties following thermocycling while also experiencing the highest increase in surface roughness (Ra) after aging. 68
By introducing nanoglass and MWCNTs, the resin utilized in 3D printing experienced a significant improvement in flexural strength (FS), elastic modulus, and impact strength (IS). Out of all the test groups, the combination group displayed the least percentage variation in flexural strength and impact strength, suggesting a behavior that falls between intermediate and ductile failure. Following thermocycling, the control group exhibited the most minor percentage change in elastic modulus, although its peak values were lower than those of the other groups. 68 Table 1 summarizes the addition of fillers and its influence on 3D-printed denture base resin.
The summary of nano additives fillers and their effect on 3D-printed denture base.

Potential and concerns of nanotech in dentures
Incorporating nanoscale particles can act as a reinforcing agent, improving the denture's function, 36 adaptation, 34 and antimicrobial properties. 44 They act as reinforcing agents within the denture base, increasing flexural strength, fracture toughness, and hardness of denture base material. Thus, it enhances patient acceptance and comfort 34 and increases the denture's thermal conductivity, significantly affecting parotid gland secretions and, consequently, the sense of taste. 72
The newly developed core/shell nanomaterials hold immense potential to improve electrochemical enzyme biosensors, creating next-generation intelligent dentures with advanced functionalities. 73 These innovative materials can provide real-time feedback by monitoring pressure distribution, temperature, and oral pH, helping to detect pressure points or infection signs early. 74 Incorporating nanomaterials into self-healing systems could create smart dentures that can repair minor cracks and damage, thus increasing the life span of dentures and minimizing the need for replacement. This technology is expected to pave the way for the fabrication of self-healing polymers through additive manufacturing technology. 75
Incorporating nanomaterials in denture bases has the potential for a new revolution in prosthodontics. However, due to their nano size, unpredicted health consequences, and possible organ accumulations, alarming concerns have been raised about integrating nanomaterials in denture base resins. These nano-scale particles can travel from the denture base and enter the bloodstream or be inhaled. 31 Foldbjerg et al. 76 revealed that certain nanoparticles may possess intrinsic toxic properties, like silver or zinc oxide. In terms of safety, vigorous biocompatibility testing is needed, and for preventing environmental contamination, monitoring nanomaterial production and disposal needs to be considered in future research.
Limitations of the study
This review highlights the lack of long-term clinical investigations. Most of the studies were in vitro, with limited bioactivity and clinical consequences. These studies also highlight the need for an in-depth understanding of nanoparticles’ influence on biocompatibility and potential toxicity, making it difficult to conclude their effectiveness over traditional materials.
Conclusion
In conclusion, optimizing 3D-printed denture base materials demands a multifaceted approach. Future research focusing on enhancing mechanical properties and resisting aging for long-term durability; developing strategies to overcome esthetic shortcomings and improve retention; refining printing technology to address resolution limitations and enable occlusal adjustments; exploring novel nanomaterials and surface modification techniques for improved filler dispersion and interfacial bonding, optimizing hybrid material systems for synergistic property improvements.
A thorough evaluation of the enhanced material's properties is crucial prior to considering nano-additives in clinical practice by assessing durability for long-term wear, chemical stability inside the patient's mouth, and biocompatibility for ensuring tissue safety.
Addressing these challenges and capitalizing on the immense potential of 3D printing and nanotechnology can pave the way for enhanced esthetics, improved longevity, and highly performing dentures.
Footnotes
Acknowledgements
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
