Abstract
Denture base materials made using three-dimensional printing (3D printing) have expanded in availability, contributing to the meteoric rise of this innovative dental technique. Despite 3D-printed denture resins having good biocompatibility and esthetics, achieving superior mechanics in these materials is still difficult. This study aimed to find out how adding calcium carbonate (CaCO3) nanoparticles to 3D-printed denture base resin affected its surface hardness, impact strength, and flexural strength. The ninety 3D printed samples were allocated into three groups following the amount of CaCO3 NPs added to the resin: one control group had no CaCO3, and two modified groups—one had 1.5 wt.%, and the other group had 2 wt.%. Surface hardness, impact, and flexural strength were the three test specifications used to further divide each group into three subgroups. Analysis was also conducted utilizing energy dispersive X-ray spectroscopy (EDX) and field emission scanning electron microscopy (FESEM). All data were statistically analyzed. The results verified that adding CaCO3 NPs to the 3D-printed denture resin significantly boosted its impact strength, flexural, and surface hardness (
Introduction
One prevalent issue of oral health among the elderly is full edentulism. Prosthodontics has undergone an enormous transformation as a result of advancements in dental materials and processing technology. Even though there are several treatment choices, full dentures are still the recommended approach.1,2 For denture bases, polymethyl methacrylate (PMMA) continues to be the commonly utilized material. However, there are certain problems that must be fixed. These include water absorption, dimensional instability over time, fatigue susceptibility, low fracture toughness, possible allergic reactions, and polymerization shrinkage.3,4 Digital manufacturing has revolutionized dental technology, particularly with the rise of three-dimensional (3D) printing, which provides considerable benefits regarding quick prototyping, design flexibility, and the removal of traditional molds, as well as a significant reduction in material waste. Additionally, it improves accuracy by reducing lab work, eliminating human error in technician-driven processes, and potentially improving tissue adaptation. 5 3D-printable denture base resins must meet a set of essential mechanical, physical, and biological requirements to ensure safe and effective clinical performance. These materials are expected to provide adequate flexural strength, impact resistance, fatigue durability, and dimensional stability to withstand functional loading. They must also demonstrate low surface roughness, controlled water absorption and solubility, and long-term color stability to reduce microbial retention and maintain esthetics. Equally important are biocompatibility and minimal residual monomer release. 6 From a manufacturing perspective, 3D-printable resins must exhibit suitable viscosity, efficient photopolymerization, and reliable print accuracy across different printing orientations and layer thicknesses. Meeting these characteristics ensures that 3D-printed denture bases achieve the necessary clinical and performance standards required for routine prosthodontic. 7 However, 3D printed acrylic resins may exhibit worse mechanical and physical qualities than conventional PMMA, and most commercially available 3D-printable denture resins still struggle to meet essential clinical performance requirements, particularly flexural strength, impact resistance, hardness, and long-term stability, falling below or only marginally meeting ISO 20795-1 standards. 8 These disadvantages make 3D printed acrylics more vulnerable to wear and breakage. Additionally, the surface texture of 3D printed acrylics may be coarser, which could hinder both their usefulness and attractive look in particular applications. 9 To overcome these restrictions, several experiments have been carried out to enhance the denture base resin features by including various fillers. Despite their minor additions, inorganic nanoparticles significantly improve denture base properties, establishing polymeric nanocomposites as a novel denture base material class.10,11
Most 3D-printed denture base resins are light-curable photopolymer systems made up of several synergistic components. The primary methacrylate monomers form the polymer matrix and largely determine the mechanical strength, flexibility, polymerization shrinkage, and overall processing behavior of the material. Cross-linking agents are used to increase the cross-link density, which improves hardness, dimensional stability, and resistance to deformation. Photoinitiators act as light-activated catalysts that promote rapid curing and deeper polymerization during the printing process, ensuring adequate conversion and reducing porosity. Inhibitors are incorporated to avoid premature polymerization during storage, while stabilizers ensure color stability and long-term durability. The formulation is further enhanced with pigments for esthetics and additional additives intended to optimize printability and performance. 12
Incorporation of nanoparticles like zirconia, carbon nanotubes, and silicon carbide has been explored by several studies to enhance the properties of acrylic resins.13–15 Multiple factors influence the overall performance of nanocomposites, comprising the nature and inherent characteristics of the polymers used, the technique of processing the composites, the nanoparticles’ size, concentration, and distribution within the matrix, and the compatibility at the interface between the matrix and the nanoparticles. 16
Spherical mineral nanoparticles may have a high interfacial contact between the polymer matrix and filler as a result of their low aspect ratio and large surface areas. These particles were said to have the potential to greatly increase the polymer matrix's toughness, strength, and modulus.17,18 Because calcium carbonate nanoparticles are one of the most popular spherical nanoscale fillers with highly biocompatible and good reinforcing qualities in other polymers, like polypropylene, additionally, their color is white, which is unlikely to impede the esthetic appeal of the acrylic denture base. They were selected as reinforcing nano fillers in this study.19,20 Unlike previous studies that have primarily focused on reinforcing 3D-printed resins with ceramics, fibers, or carbon-based fillers, the present work introduces CaCO₃ NPs as a novel, cost-effective, and biocompatible reinforcement strategy. Calcium carbonate nanoparticles have not been widely explored in 3D-printed denture base materials despite their favorable characteristics. By evaluating different CaCO₃ concentrations and assessing their impact on hardness, flexural, and impact strength, this study delivers new evidence supporting the use of CaCO₃ NPs as a promising additive for elevating the performance of 3D-printed denture base resins and advancing their clinical applicability.
Materials and methods
The three groups of thirty 3D printed specimens were classified by the percentage of CaCO3 NPs added to the resin. These categories were used to classify a total of 90 specimens: control group without CaCO3, group containing 1.5 wt.%, and group comprising 2 wt.% CaCO3 NPs. Based on the test specifications for surface hardness, impact, and flexural strength, each group 10 was further split into three subgroups.
Preparation of nanocomposites mixture
Calcium carbonate nanopowder (Skyspring nanoparticles, Inc., USA) was added as an inorganic filler to 3D-printed denture base resin (ASIGA DentaBASE resin), which complies with ISO 20795-1:2013 and ISO 10993-1:2018, and verified to meet the applicable mechanical and biocompatibility requirements for denture base resins. According to the manufacturer's datasheet, the resin formulation includes 7, 7, 9 (or 7, 9, 9)-trimethyl-4,13-dioxo-5,12-diazahexadecane-1,16-diyl bismethacrylate, diphenyl(2,4,6-trimethylbenzoyl) phosphine oxide, and tetrahydrofurfuryl methacrylate. This photopolymer is compatible with DLP (Digital Light Processing) 3D-printing systems in order to create the nanocomposite denture base specimens for investigation. A particle size analyzer confirmed that the specimens had an average diameter of 87.5 nm.
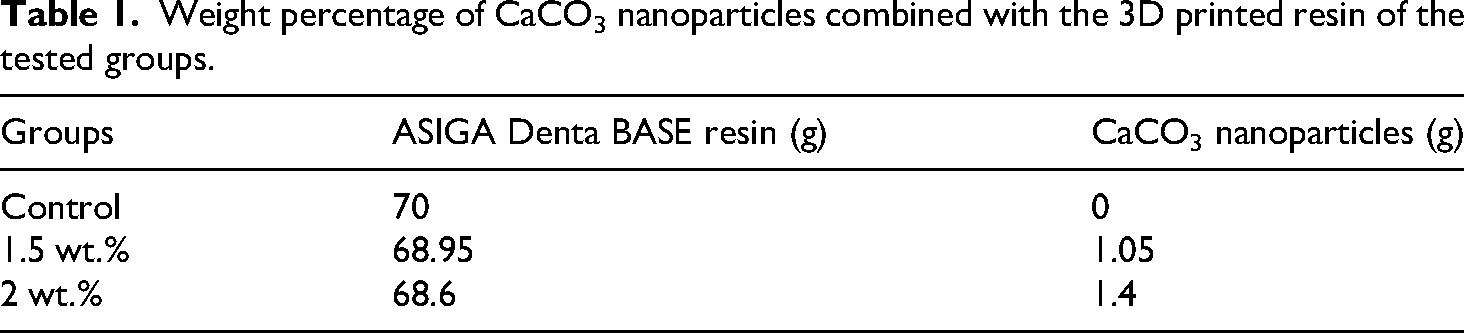
The pure resin was first mixed in an LC-3D mixer for 120 minutes to create nanocomposite mixes in order to guarantee the homogeneity of the 3D resin prior to the addition of nanoparticles. 21 Following that, one group was left without the addition of CaCO3 NPs (control group), while precisely weighed volumes of NPs were introduced to separate containers containing the 3D base resin at the specified concentrations (1.5 wt.% and 2 wt.%) (Table 1). A speed mechanical mixer is then used to rapidly mix the mixture for 5 minutes at 2500 rpm, employing a two-stage mixing process. 22
Weight percentage of CaCO3 nanoparticles combined with the 3D printed resin of the tested groups.
Preparation of specimens
To create the specimens, open-source CAD software was utilized, which was then exported into the STL file format, which is a popular file type for 3D printing. An ASIGA MAX UV 3D printer was then used to create the required specimens with the necessary measurements.
In accordance with 3D printing manufacturing requirements, each layer was produced in 1.6 seconds with a 50-µm layer thickness and a 0-degree orientation. 23 The layers were later exposed to ultraviolet (UV) radiation with a 405-nm wavelength to promote polymerization. In compliance with the company's directions, following a 99.9% isopropyl alcohol cleaning, the samples were soaked in glycerol and post-cured using an Ottoflash G171 UV light unit. The procedure involved two cycles of 2000 flashes in an environment of inert nitrogen gas, with a specimen turnaround following each cycle for 20 minutes in order to finish the polymerization procedure 24 as seen in Figure 1.

Fabrication process for 3D-printed specimens modified with calcium carbonate nanoparticles (CaCO3 NPs) (a) designing the 3D model. (b) Pouring the nanocomposite resin into the 3D printer and initiating the printing process (c), removal of printed specimens from the build platform once the printing is complete (d), and the post-curing process to ensure the specimens reach their full strength and durability.
After that, the support structures were eliminated using a low-speed rotating instrument. The samples were washed with water and graded utilizing silicon carbide grinding paper (800, 1500, and 2000 grit) before being polished with a lathe polishing tool. A single operator carried out the entire process to guarantee that the same circumstances were employed 25 times. For 48 hours, the samples were submerged at 37°C in distilled water before testing. 26
Testing procedure
Flexural strength test
Following ISO (20795-1:2013), thirty samples were prepared for the flexural strength test, along with dimensions of 3.3 mm thickness, 64 mm length, and 10 mm width. 27
A three-point bending test (Instron H50 KT Tinius Olsen) was utilized to measure flexural strength.
28
The horizontally positioned specimen is subjected to a concentrated load at its middle during the test until it breaks. Equation (1) is used to determine flexural strength (
Impact strength test
Thirty specimens had length, width, and thickness measurements of 80 × 10 × 4 mm, for the impact strength test as per the ISO (20795-1:2013).
27
To measure impact strength, Izod's Impact Strength Tester is used. Because the measurement provides the impact energy reading in joules. Estimating the Izod test in kilojoules per square meter (kJ/m2) is done using Equation (2)
29
:
Surface hardness test
For the surface hardness test, thirty specimens must be printed with dimensions of 3 mm in thickness, 12 mm in length, and 12 mm in width, following ISO (20795-1:2013). 27 A durometer that is approved for use with acrylic resins, a Shore D (HLX-AC), was utilized to gauge the surface hardness. The durometer has a 0.1-mm diameter indenter with a blunt point.
The durometer is held perpendicularly and supported by a sturdy surface to prevent instrument shock. During the testing procedure, the specimens will be exposed to a predetermined minor load of 44.5 N as quickly as possible. One second after maintaining consistent contact with the material, the hardness value will be digitally recorded.30,31 By averaging the results of five measurements, the Shore D hardness of each specimen is determined.
Field emission scanning electron microscopy (FESEM)
The size of the CaCO3 powder was examined utilizing a FESEM (FE.IS50) equipment, as well as the dispersion pattern of CaCO3 NPs within the 3D printed resin specimens. A CaCO3 powder specimen and three representative samples, one for each of the groups (1.5 wt%, 2 wt%, and the control), were examined.
Energy dispersive X-ray spectroscopy (EDX)
The elemental distribution and proportion of each component of CaCO3 nanoparticles are assessed using an EDX equipment (Axia Chem Sem, Thermos Scientific).
Statistical analysis
For this study, the researchers used version 26 SPSS (Statistical Package for the Social Sciences) software to examine the data. Statistical analyses encompass two main categories: Descriptive statistics, which provide a summary and highlight the key features of the data, including Standard error (SE), Standard deviation (SD), Mean (M), Maximum (Max), Minimum (Min), and Basic chart bars. The other category is the inferential analysis, where the Shapiro–Wilk test is utilized to assess whether a data distribution is normal. Comparisons of group means were made using ANOVA, which symbolizes one-way analysis of variance. The significance of the groups was assessed by means of Tukey's HSD post hoc test. A
Result
Flexural strength test
The data had a normal distribution with a

Bar chart represents the mean and SD values of the flexural strength test.
Descriptive statistics for the flexural strength test and

A one-way ANOVA exhibited a statistically significant difference (
One-way ANOVA test for the flexural strength test.

Impact strength test
According to descriptive statistics, the mean impact strength (9.640 kJ/m2) was lowest in the control group, while the group containing 2 wt.% CaCO3 NPs, as illustrated in Figure 3 and Table 4, had the highest mean value (16.800 kJ/m2).

Bar chat for impact strength test mean and standard deviation for all study peers. ***high significant
Descriptive statistics of the impact strength test and the F test using ANOVA.

A one-way ANOVA showed a statistically significant difference (
Tukey's multiple comparisons of the flexural strength outcomes for all groups.

One-way ANOVA test for the impact strength test.
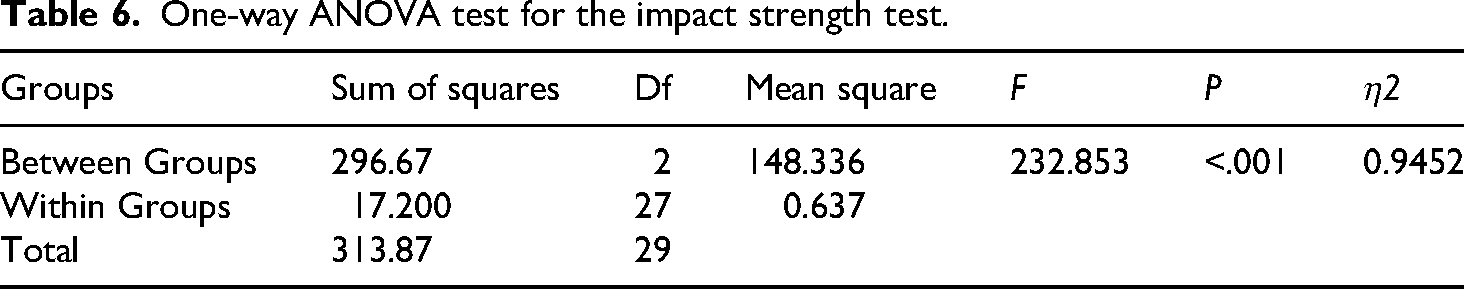
Tukey's multiple comparisons of the impact strength results for all groups.

Surface hardness test
The data were normally distributed as a result of the Shapiro-Wilk test, which yielded a

Bar chart represents mean and SD values of the surface hardness test.
Descriptive statistics for surface hardness test and

One-way ANOVA test for the surface hardness test.

Tukey's post hoc test of the surface hardness test for multiple comparisons.

Field emission scanning electron microscopy (FE-SEM) and energy dispersive X-ray spectroscopy (EDX)
The FE-SEM images revealed that the CaCO3 NPs seem to have a spherical form and a size of less than 100 nm at field-of-view scales of 500 nm and 1 µm, as shown in Figure 5.

FE-SEM images of CaCO3 powder: (a) at fields view 500 nm, (b) at fields view 1 µm.
Figure 6 illustrates the apparent variations in surface morphology among the CaCO3 modified groups and the control group based on FE SEM images of the test specimens’ broken surfaces for flexural strength.

FE-SEM revealed the morphology of the damaged surface of the samples at 500× magnification: (a) control group, (b) 1.5 wt.% CaCO3 group, and (c) 2 wt.% CaCO3 group.
Additionally, the CaCO3 nanoparticles seemed to be uniformly dispersed throughout the three-dimensional resin matrix. However, when the loading of nanoparticles increased to 2 wt.% CaCO3 NPs, some agglomeration took place.
EDX analysis is quantitatively and qualitatively characterized by all the produced nanoparticle content. The chemical composition of the CaCO3 NPs is shown in Figure 7. Carbon is (10.9 wt.%), oxygen is the most abundant element (50.7 wt.%), while calcium is (38.4 wt.%), according to the data in Table 11. The distribution of elements across the nanoparticles is further visualized in the chemical mapping image of Figure 8.

EDX analysis of CaCO3 NPs.

EDX analysis of the chemical mapping image of CaCO3 nanoparticles.
EDX analysis for the element percent of CaCO3 NPs.

Discussion
The present study assessed how adding calcium carbonate nanoparticles to 3D denture base resin affected the material's flexural strength, surface hardness, and impact resistance. According to statistical analysis, the CaCO3 NP-modified resin groups and the control group differed significantly (
The present study used a layer thickness of 50 µm and a 0-degree orientation. Printing orientation inherently influences anisotropy due to the layer-by-layer nature of vat-polymerized resins. To control this variable and avoid introducing orientation-dependent differences into the results, the study standardized the orientation at 0°. This provided consistency across all specimens while also taking advantage of the mechanical and time-efficiency benefits established in previous research. 32 Choosing the 0° orientation to minimize printing time was particularly important in the present work because prolonged fabrication increases the risk of nanoparticle precipitation in the resin tray, which could compromise filler distribution and consequently affect the mechanical properties. 33
CaCO3 NP were chosen as reinforcing nanofillers due to their excellent biocompatibility, excellent reinforcing properties in other polymers, such as polypropylene, and their white color, which is unlikely to negatively impact the acrylic denture base's esthetic appearance. 20
The sophisticated stresses of mastication of the oral cavity necessitate robust mechanical qualities for denture base materials to function properly, such as flexural strength, which is a mix of shear, tensile, and compressive strengths, so it reflects the load intraorally and demonstrates the denture base's resistance to breaking. 34 Because of that, high flexural strength is considered very important to obtain great clinical performance. 35
A minimum flexural strength of 65 MPa following ISO-20795-1:2013 is obligatory for effective clinical use. High flexural strength is ideal for the denture base so that it can tolerate masticatory stresses without permanently breaking or deforming. 36
According to flexural strength data, both experimental groups (1.5 wt.% and 2 wt.% CaCO3) outperformed the control group regarding flexural strength, and each group's percentage grew in direct proportion to the percentage rise. This result agreed with those of Kadhum and Hamad, who used barium titanate nanoparticles to create materials that are 3D-printed denture bases and observed similar improvements in flexural strength. 37 This shows that nanoparticles strengthen the material's resistance to fractures caused by stress by acting as reinforcing agents. The printed component's strength, stiffness, and overall structural integrity are all improved by filling the gaps between the polymer chains. According to earlier findings, improving the nanocomposite flexural strength may also depend on attaining a homogeneous distribution of nanoparticles with the resin matrix, as verified by FESEM.38,39 Because CaCO3-modified resins have better mechanical qualities, dentures made with them may last longer and be less likely to shatter or fracture. Adding a specific number of nanoparticles is effective and improves the 3D printed denture base's mechanical performance; however, a concentration greater than the saturation level degrades the composite qualities.40,41
Furthermore, impact strength property is crucial for denture base materials, as they are susceptible to breakage upon accidental drops onto hard surfaces. According to Powers and Sakaguchi (2006), impact strength measures the amount of energy a material absorbs following a sudden impact before breaking. 42
The 3D resin material's impact strength was considerably enhanced by incorporating CaCO3 nanoparticles at 1.5 and 2 wt.%. A direct association existed between the additional concentration and the enhancement of impact strength. The layer-by-layer printing technique, which creates spaces between the resin chains, may have contributed to the control group's reduced impact strength. Particle size analysis showed that the CaCO3 NPs had a nanoparticle size of 87.5 nm, which permits them to move between the polymer's linear macromolecular chains, which contributed to the enhancement. Additionally, FE-SEM examinations showed that the nanoparticles were evenly distributed throughout the substance, increasing the impact strength even more. Furthermore, as confirmed by Fatalla et al., 43 the high-level interfacial strength between the nanofiller and polymer base probably helps to improve impact strength because nanoparticles fill in the gaps between polymer chains, preventing displacement and dissipating energy that leads to crack propagation. These findings align with earlier research by Chen et al., 37 Mangal et al., 44 Gad et al., 45 and Alshaikh et al., 40 which noted that adding TiO2 and PEEK nanoparticles, aminated nanodiamonds, SiO2 NPs, and ZrO2 NPs to 3D-printed resins, respectively, increased impact strength.
Another important parameter to take into account when testing mechanical properties is hardness, which indicates how well the specimen's surface represents the material's surface strength and is resistant to abrasion; a material with lesser hardness is more vulnerable to resin surface degradation, scratches, and changes in dimensions brought on by scrubbing dentures or chewing tough foods. 46
The shore D hardness test results were significantly improved for the 1.5 and 2 wt.% CaCO3 modified groups. The greatest increase in surface hardness among the tested concentrations was accomplished using the addition of 1.5% by weight CaCO3 nanoparticles. Although the hardness decreases as the concentration of CaCO3 NPs is increased above the saturation level, it still exceeds that of the control.
The control group's hardness was lower. This decrease is explained by the 3D-printed denture base resins’ lower double-bond conversion in comparison with conventional denture base resins. 47 The 1.5 and 2 wt.% groups showed a considerable improvement in the shore D hardness test results. A rise in cross-linking density, making the polymer more rigid and impervious, may be the cause of the nanocomposite denture base resin's increased hardness. 43
Also, the addition of CaCO3 NPs reduces the spacing between the particles inside the matrix. As the distance between particles decreases, the particles’ bonding strength increases, and they cluster together, causing hard material particles (CaCO3NPs) to accumulate on the surface of resin matrix gaps and improving hardness. 48
Furthermore, the polymerization rate and the conversion degree have a direct relationship with the denture base resin hardness and strength. Perea-Lowery et al. claim that the 3D-printed denture bases’ conversion degree and mechanical properties were enhanced by the post-curing machine's conjunction of light and heat. In addition, post-curing in an environment of inert nitrogen lessens the negative effects of the oxygen inhibition layer. 49 Moreover, the notable improvement in hardness might have been favorably influenced by the layer thickness of 50 μm. 45
In contrast to the control and 2 wt.% groups, the shore D test for the 1.5 wt.% group showed a notable improvement and revealed a distinct pattern. Hardness may be reduced if the nanoparticle concentration rises above the saturation level. 50 These outcomes match with a prior research conducted by Altarazi et al. 51 and Chen. 37
As the filler percentage rose, FE-SEM showed that CaCO3 was well distributed within the resin matrix with some agglomeration, which aligned with Ahmed and Ali (2021), 52 Tukmachi et al. (2021), 53 and Kareem et al. (2024). 26 While agglomeration was only noticeable at higher percentages, and it employed various fillers in varying proportions, it differed from other studies. 54 The addition of CaCO3 nanoparticles in the polymer is verified by the EDX test.
Future research should expand upon these findings by conducting in vivo investigations to validate the clinical relevance and long-term performance of CaCO₃-reinforced 3D-printed denture base materials. Further studies are recommended to assess the effect of CaCO₃ nanoparticles on additional properties, including surface roughness, solubility, water absorption, color stability, denture adaptation, radiopacity, tensile strength, and diametral compression strength. Moreover, future work should explore the impact of saline pre-treatment of CaCO₃ nanoparticles before incorporation into the resin, as well as the influence of key processing parameters involving polishing methods, curing and post-curing protocols, printing orientation, storage conditions, and layer thickness.
Limitations of the study
This study had to deal with issues including selecting an appropriate dental lab and figuring out different 3D printers and resins. The success of the printing process depends critically on the resin's viscosity. Low viscosity and fluid resins can readily flow to the designated printing area in the time specified. Conversely, high viscosity resins show reduced fluidity, which could slow down printing or result in a failed print. So, managing resin viscosity is one of the study's limitations. Uncontrolled air entrapment in the resin fluid during the printing process resulted in holes forming in and between the printed layers, which negatively impacted the printed specimens’ mechanical qualities. Furthermore, the existing in vitro study was limited by evaluating mechanical characteristics under dry settings without taking into account noticeable aging in a variety of liquid media, like water, artificial saliva, or coffee, which fails to accurately represent oral performance in real life.
Conclusion
This work serves as the foundation for future research. Our study focused on a single type of 3D-printed resin, one nanoparticle, and one printing orientation. When 3D-printed resin is mixed with 1.5 wt. % and 2 wt.% calcium carbonate nanoparticles, the flexural and impact strengths are greatly increased at 2 wt.%, and the improvement level is directly correlated with the concentration of CaCO3 nanoparticles. Additionally, the 1.5 wt.% modified group exhibited the greatest improvement in the shore D hardness of the 3D-printed denture base resin.
Footnotes
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
