Abstract
Most animal hazards in laboratories are widely recognized. These, together with zoonoses and other possible insults, are subject to the establishment of guidelines for the operation and maintenance of such facilities. Most of the infectious diseases described among laboratory animals are related to the inadequate implementation of preventive and quality control policies. These included surgical, respiratory and intestinal tract infections, and typically spread between animals. This report is about an outbreak of nosocomial bacterial infection in rats held in the research laboratory of a human hospital. Symptoms of general infection were runny nose and sneezing, excessive lachrymation, dyspnea, loss of appetite, limited activity and disheveled fur, which appeared in two rats initially, and spread to another 60. A common characteristic physical finding observed later was a lump under the skin, with subsequent ulceration. Mortality was 70%. Blood cultures were sterile. Accurate diagnosis was possible only after examination of tissue sampled from the diseased and dead rats. Histology showed an excessive proliferative and inflammatory reaction. Bacteriology analysis revealed the presence of three types of hospital-borne bacteria: enterococcus, coagulase-negative staphylococci and Acinetobacter radioresistens, with common sensitivity to ciprofloxacin and ceftazidime. Empiric antibiotic therapy was switched to a bacteriology-based regimen. Complete recovery was achieved among the diseased rats that survived the previous antibiotic therapy. This is the first written description of a nosocomial infection of laboratory animals caused by bacteria borne in a human hospital. Medical staff-to-animal transmission is suggested. A high index of suspicion and prompt diagnostic evaluation are essential for successful management, and preventive guidelines concerning such events need to be established.
Observation report
Concern about animal hazards in laboratory facilities has been widespread and longstanding. The main potential experimental hazards are biological agents (e.g. infectious agents or toxins), chemical agents (e.g. carcinogens and mutagens), radiation (e.g. radionuclides, X-rays and lasers), and physical injuries (e.g. needles and syringes). Other possible insults – such as animal bites, exposure to allergens, chemical cleaning agents, wet floors, cage washers and other equipment, lifting, ladder use and zoonoses – that are inherent in or intrinsic to animal use – have also been studied. All of these are subject to the establishment of guidelines for the maintenance and operation of laboratory animal facilities. 1
Infectious diseases among laboratory animals have been extensively discussed in the literature, mainly in the context of surgical infections,2,3 and also respiratory and intestinal tract infections which are typically spread between animals. Such events are related to inadequate implementation of preventive and quality control policies in the animal facilities of research and medical institutions. 4
We describe here an outbreak of bacterial infection in rats, held in a research laboratory animal facility in a general human hospital.
In the beginning of January 2011, we noticed two spontaneous-hypertensive rats (SHRs) with an unusual syndrome in our nephrology and hypertension laboratory. It consisted of runny nose and sneezing, excessive lachrymation, dyspnea, loss of appetite, limited activity and disheveled fur. After two days, these diseased rats developed lumps under their skin, with subsequent ulceration. By the end of the second week, this phenomenon spread to other rats. After blood cultures were taken, all the sick animals (60) were treated with amoxicillin + clavulanic acid for three weeks, and then by sulfamethoxazole + trimethoprim for an additional three weeks. Antibiotics were given in daily doses, adjusted to body weight, and dissolved in drinking water. Blood culture results were negative. We did not see any therapeutic effect;moreover, the mortality rate was 70%. At that stage, a pathological study of the lumps and internal organs of both surviving and dead animals was performed.
Major macroscopic findings, besides subdermal masses, were edema of the peritoneum, bowel, lungs and the subclavian region in all the animals, as well as enlargement of the submandibular glands in some of them.
Tissue samples from the subdermal masses were transferred to the hospital pathology and bacteriology laboratories for histology and microbiology examinations. Histological description of the specimens is presented in Figure 1. Bacteriology analysis revealed the presence of three types of bacteria: enterococcus, coagulase-negative staphylococci and Acinetobacter radioresistens, with common sensitivity to ciprofloxacin andceftazidime.
The specimen shows fibroblast proliferation with collagenous and relatively vascularized stroma and numerous scattered mast cells (a) highlighted by Giemsa stain (b).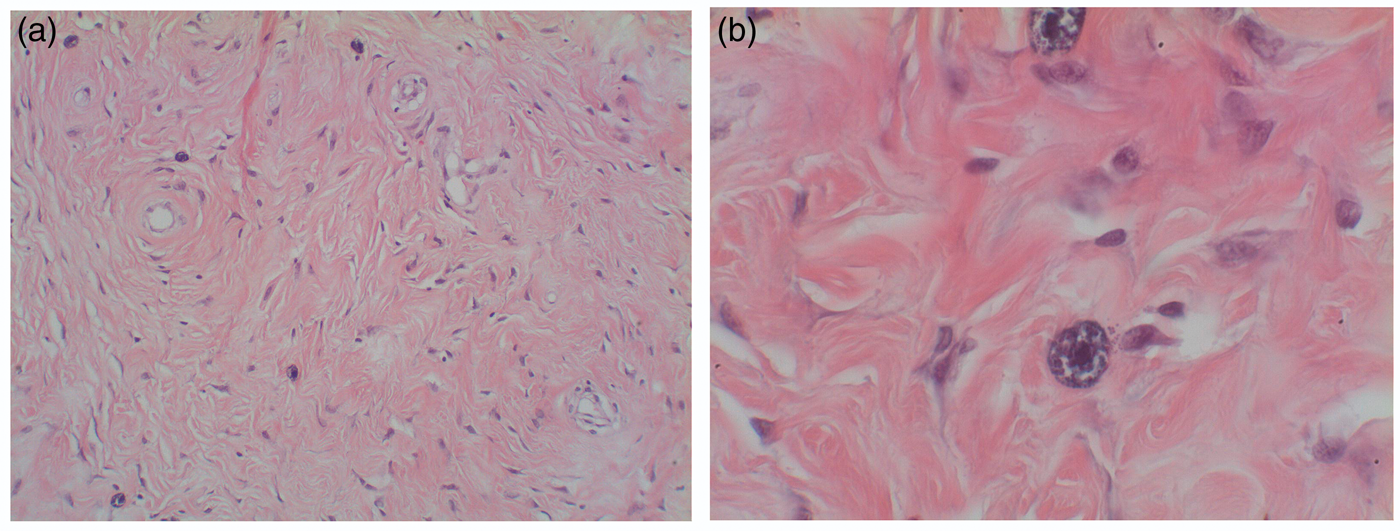
The surviving rats were switched to a bacteriogram-sensitivity adjusted antibiotic regimen for another three weeks, and made a complete recovery. Repeated blood cultures, taken two weeks after completion of the treatment program, were sterile.
In 2009, Pritchett-Corning et al. presented their serology and bacteriology results from samples using more than 80,000 rats submitted from pharmaceutical, biotechnology, academic and governmental institutions in North America and Europe. They found that the commonly detected infectious agents included mainly viruses. Helicobacter and Pasteurella specieswere the leading causative agents of bacterial infections. 5
These results emphasized the distinction of the bacteriological results in our report. Coagulase-negative staphylococcus is considered to be a typical flora within a hospital environment, especially in intensive-care units. 6 However, Acinetobacter radioresistens is quite rare in a hospital environment and also appears mainly in mechanically-ventilated patients. This bacterium is constantly mutating and its sensitivity to antibiotic treatment is quite low. 7 Most pathogenic nosocomial bacteria cause lethal pneumonia and sepsis. Their prevention represents a major challengein contemporary clinical practice in hospital medicine. 8
This unusual infectious spread among laboratory animals demonstrates the potential for hazardous contagion by medical staff who work in a research laboratory located in a hospital.
To the best of our knowledge, this is the first written description of a nosocomial infection of laboratory animals caused by human hospital-borne bacteria. Medical staff-to-animal transmission is, therefore, suggested. A high index of suspicion and prompt diagnostic evaluation including tissue examination (pathology and bacteriology) are essential for the successful management of such events while guidelines have to be established in order to prevent them.
Footnotes
Ethical statement
This study was conducted under the auspices of the supreme ethical committee supervising animal experiments within the Ministry of Health of the State of Israel.
Declaration of conflicting interests
None declared.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
