Abstract
Determination of regional blood flow by the injection of microspheres in sepsis models is crucial for the experimental evaluation of the influence of experimental treatment strategies on organ perfusion. However, multiple injections may critically increase the total quantity of microspheres, thereby restricting regional microcirculation and altering the results of blood flow measurements. This study was designed to compare the results of multiple versus single injections of microspheres in an established ovine sepsis model. Injury was induced by smoke inhalation and instillation of Pseudomonas aeruginosa into the lungs. Twenty sheep were studied for 4, 8, 12, 18, or 24 h, respectively. Microspheres were injected at the end of the study period and the animals were euthanized and organ tissues were harvested. Another four sheep were studied for 24 h and multiple microsphere injections were performed at the above indicated time points in the same animals. Tracheal blood flow significantly increased and blood flow to the pancreas and ileum significantly decreased versus baseline in both groups (P < 0.05 each). Blood flow to the ileum, renal cortex and skin did not significantly change versus baseline in both groups (P > 0.05). Blood flow was higher to the trachea in the multiple injection group at 18 h (P = 0.048) and to the ileum at 12 h (P = 0.049), and lower to the skin at 18 h (P = 0.015). In conclusion, the results indicate that multiple versus single microsphere injections induced no or negligible alterations during ovine sepsis. This finding may help reduce the quantity of animals needed in future experiments.
Determination of regional blood flow in large animal models of sepsis is frequently used for the experimental evaluation of the influence of experimental treatment strategies on organ perfusion. Multiple methods have been employed in measuring organ blood flow; however, the most often utilized technique is dependent on the injection of microspheres. The reason for the widespread acceptance of the microsphere method is mostly due to the limitations of the alternative techniques of blood flow measurement. 1
It has been demonstrated that microspheres labeled with radioactive nuclides or fluorescent microspheres are distributed in direct proportion to organ blood flow in various animal and physical models. 2 –4 Nevertheless, the microsphere technique is associated with potential sources of error. The size of the microspheres must be adequate in relation to the studied species. If the size of the microspheres is too large, they may obstruct the vascular bed and interfere with microcirculatory blood flow. If the spheres are too small, they may disappear from the tissue and not allow accurate measurements. It has been suggested that a microsphere size of 15 µm is appropriate for blood flow measurement in large animals. 5
Importantly, the quantity of microspheres injected is also crucial. On the one hand, it must be ensured that the tissue of interest receives a sufficient amount of spheres. On the other hand, too large a quantity of microspheres may generate microcirculatory impairment. The optimal amount of microspheres probably varies with animal size. For blood flow measurements in the sheep model, a figure of approximately five million fluorescent microspheres per injection is established. 6,7 In this regard, multiple injections may increase the total quantity of microspheres up to a critical amount, thereby restricting regional microcirculation and impairing organ function over time. The maximum amount of microspheres that does not cause significant changes in blood flow is not known.
The present study investigates the possible impact of multiple microsphere injections on microcirculation, using an established ovine model of pneumonia-induced sepsis by instillation of live Pseudomonas aeruginosa into the lungs.
Animals
This study was approved by the Animal Care and Use Committee of the University of Texas Medical Branch and conducted in compliance with the guidelines of the National Institutes of Health and the American Physiological Society for the care and use of laboratory animals.
A total of 24 adult female sheep of the Merino breed (Talley Ranches, Uvalde, TX, USA) (mean body weight, 32 ± 3 kg) were included in this study. The sheep were maintained in metabolic cages during the experiments.
Materials and methods
Surgical preparation and injury
The model of ovine acute lung injury by smoke inhalation and pneumonia-induced sepsis by instillation of Pseudomonas aeruginosa into the lungs has been previously described in detail. 8 –10 In brief, sheep were deeply anesthetized and surgically prepared for chronic study using a femoral artery catheter, a pulmonary artery thermodilution catheter, and a left atrial catheter. After a recovery period of 5–7 days, the animals were deeply anesthetized, received a tracheotomy and were subjected to inhalation of 48 breaths of cotton smoke (<40℃) using a modified bee smoker. 11 Then, a stock solution of live Pseudomonas aeruginosa (2–5 × 1011 colony-forming units from a burn patient at Brooke Army Medical Center, San Antonio, TX, USA) suspended in 30 mL of 0.9% NaCl solution was instilled into the right middle and lower lobes and left lower lobe of the lung (10 mL each). Anesthesia was then discontinued, and the sheep were allowed to awaken.
Experimental protocol
The study was designed to compare the results of multiple versus single injections of colored fluorescent microspheres for the determination of microvascular blood flow to various organs in an established ovine model of sepsis. Therefore, the following two groups were studied:
Multiple injection group (n = 4): Microspheres were applied in the same sheep before (baseline) and at 4, 8, 12, 18 and 24 h after induction of sepsis (baseline plus five microsphere injections). Following the 24 h microsphere injection, all animals were euthanized and organ tissues were harvested. Single injection group (n = 20): In all sheep, microspheres were applied before induction of sepsis to serve as a baseline measurement. Afterwards, sepsis was induced in all the animals. Microspheres were injected at 4, 8, 12, 18 or 24 h (baseline plus one microsphere injection) and the sheep were euthanized at the respective time point to obtain organ tissues (n = 4 at each time point).
All the sheep were mechanically ventilated (Servo Ventilator 900 C, Siemens, Elema, Sweden) with a tidal volume of 12–15 mL/kg and a positive end expiratory pressure of 5 cmH2O. The respiratory rate was initially set at 20 breaths per minute and adjusted according to blood gas analysis. All the animals were fluid resuscitated, initially started with an infusion rate of 2 ml/kg/h lactated Ringer's solution and adjusted to maintain the hematocrit at baseline values of ±3%. During the study period, the animals had free access to dry food, but not to water. After completion of the study period, the animals were deeply anesthetized with ketamine (15 mg/kg, KetaVed, Phoenix Scientific, St Joseph, MO, USA) and euthanized by intravenous injection of 60 mL saturated potassium choride.
Measurements
Hemodynamic variables were determined from the femoral and pulmonary artery catheters using pressure transducers (Baxter-Edwards Critical Care, Irvine, CA, USA) and recorded on a hemodynamic monitor (monitor V24C, Philips Medicine System Bollinger, Bollinger, Germany). Cardiac output was measured in triplicate using the thermodilution technique (Monitor 9530, Baxter–Edwards Critical Care). Cardiac index and systemic vascular resistance index were calculated by standard equations.
Immediately after euthanization, representative standardized tissue samples were obtained from the trachea, pancreas, spleen, ileum, right renal cortex, and from the skin over the right back limb. Organ blood flows were measured by injection of fluorescent colored microspheres as previously described.
6
In brief, approximately five million microspheres (15 ± 0.1 µm, E–Z TRAC, Interactive Medical Technology, Los Angeles, CA, USA) were injected into the left atrium. Calibration of microsphere activity per unit of blood flow was accomplished by withdrawing a reference sample of aortic blood (10 mL/min), starting 30 s before injection of the microspheres and continuing for 120 s. The different colors of the microspheres were administered in a random order. The tissue samples were analyzed by Interactive Medical Technologies by determining the weight of each tissue sample, digesting the entire sample in a high concentration of NaOH, and measuring the total number of different colored spheres using flow cytometry. Regional blood flow in mL/min/g was then calculated using the following formula:
Regional blood flow = total tissue spheres/([tissue weight, g] × [reference spheres/mL/min]).
Statistical analysis
All values are expressed as means ± standard error of the mean. Results were compared by a t-test or one-way analysis of variance (ANOVA) followed by a post hoc Dunnett's test as the multiple comparison method where appropriate. A value of P < 0.05 was regarded as statistically significant.
Results
There were no significant differences between groups in baseline values of cardiac index, systemic vascular resistance index, and regional organ blood flow (P > 0.05 each).
Hemodynamic variables
Changes in systemic and pulmonary hemodynamic variables.
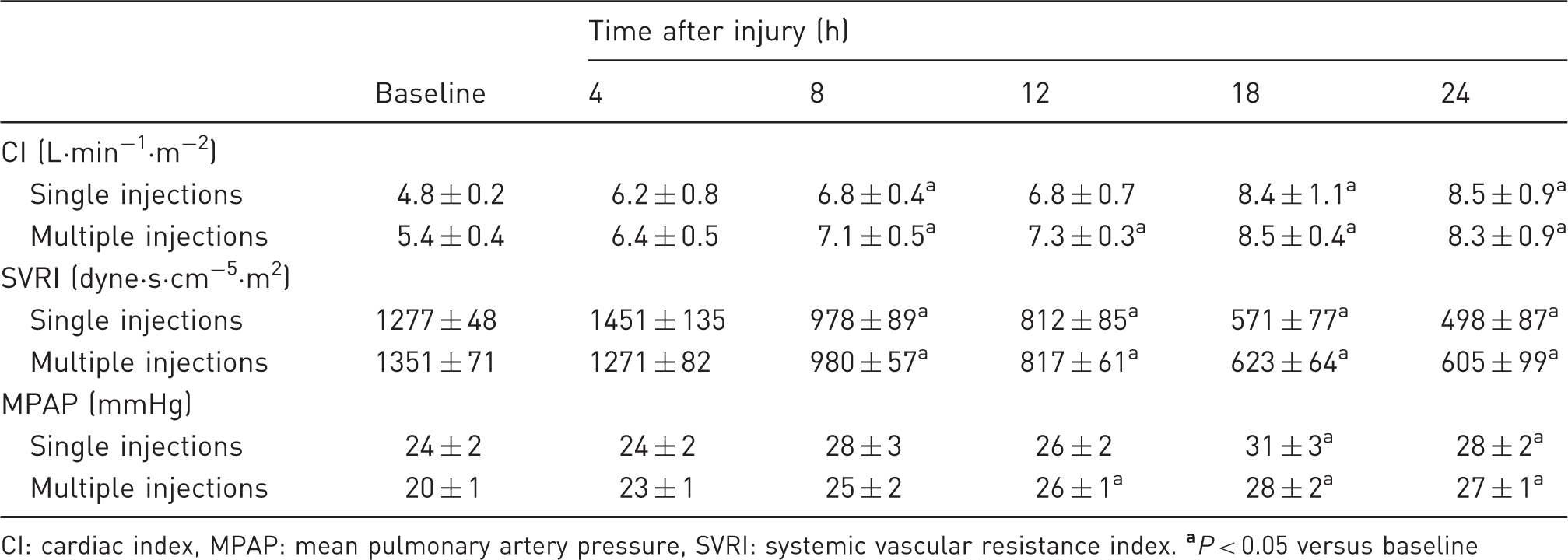
CI: cardiac index, MPAP: mean pulmonary artery pressure, SVRI: systemic vascular resistance index.
Regional blood flow
The blood flow to the trachea was significantly increased versus baseline at various time points during sepsis in both groups. However, blood flow to the trachea was significantly higher in the multiple injection group at the 18 h time point (Figure 1).
Regional blood flow (RBF) to the trachea at various time points after the induction of sepsis determined by single versus multiple injections of fluorescent microspheres. The data are presented as % of baseline values. Baseline is represented by the dotted line. Differences between groups were detected by t-test. *P < 0.05 versus baseline.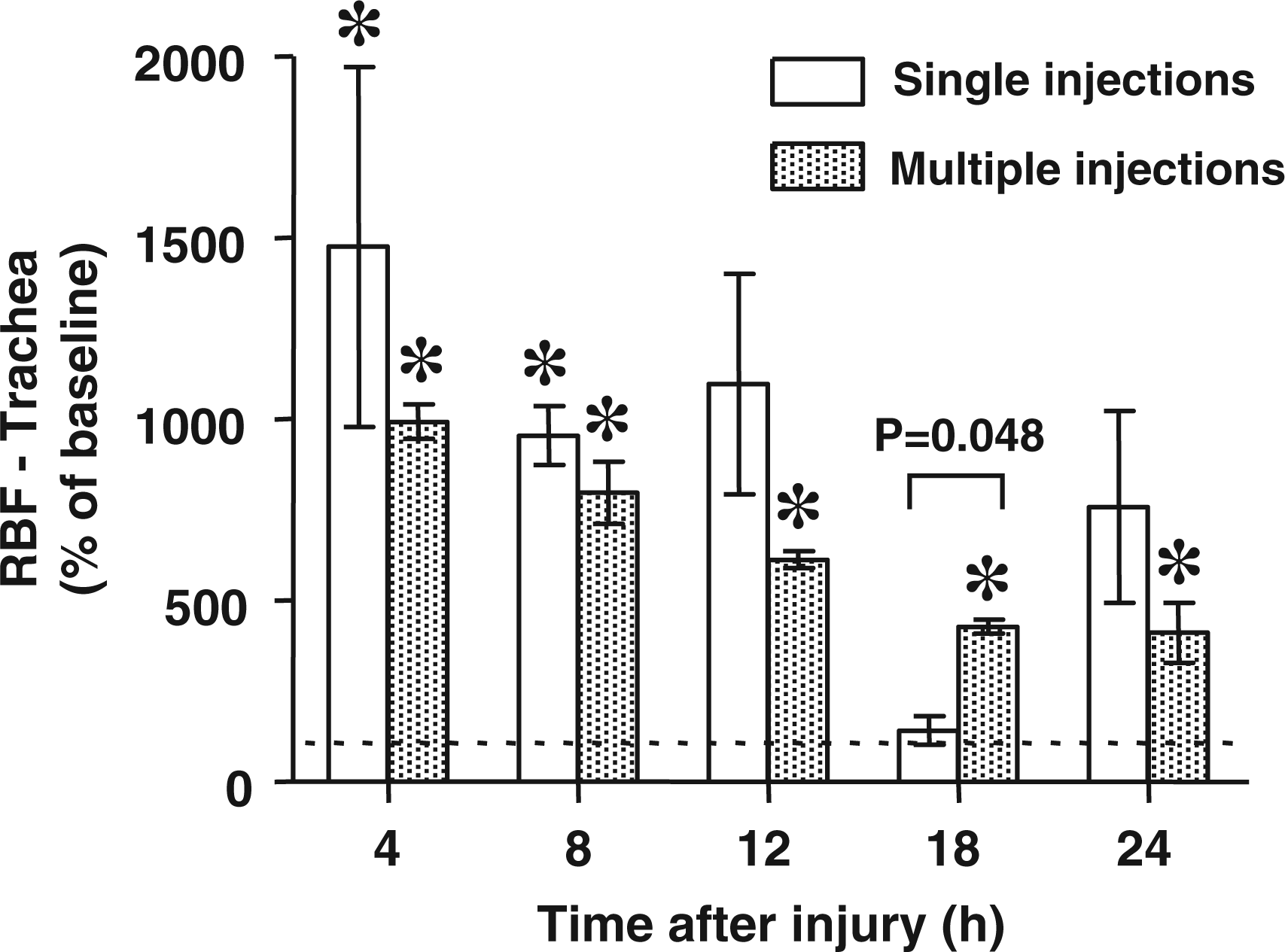
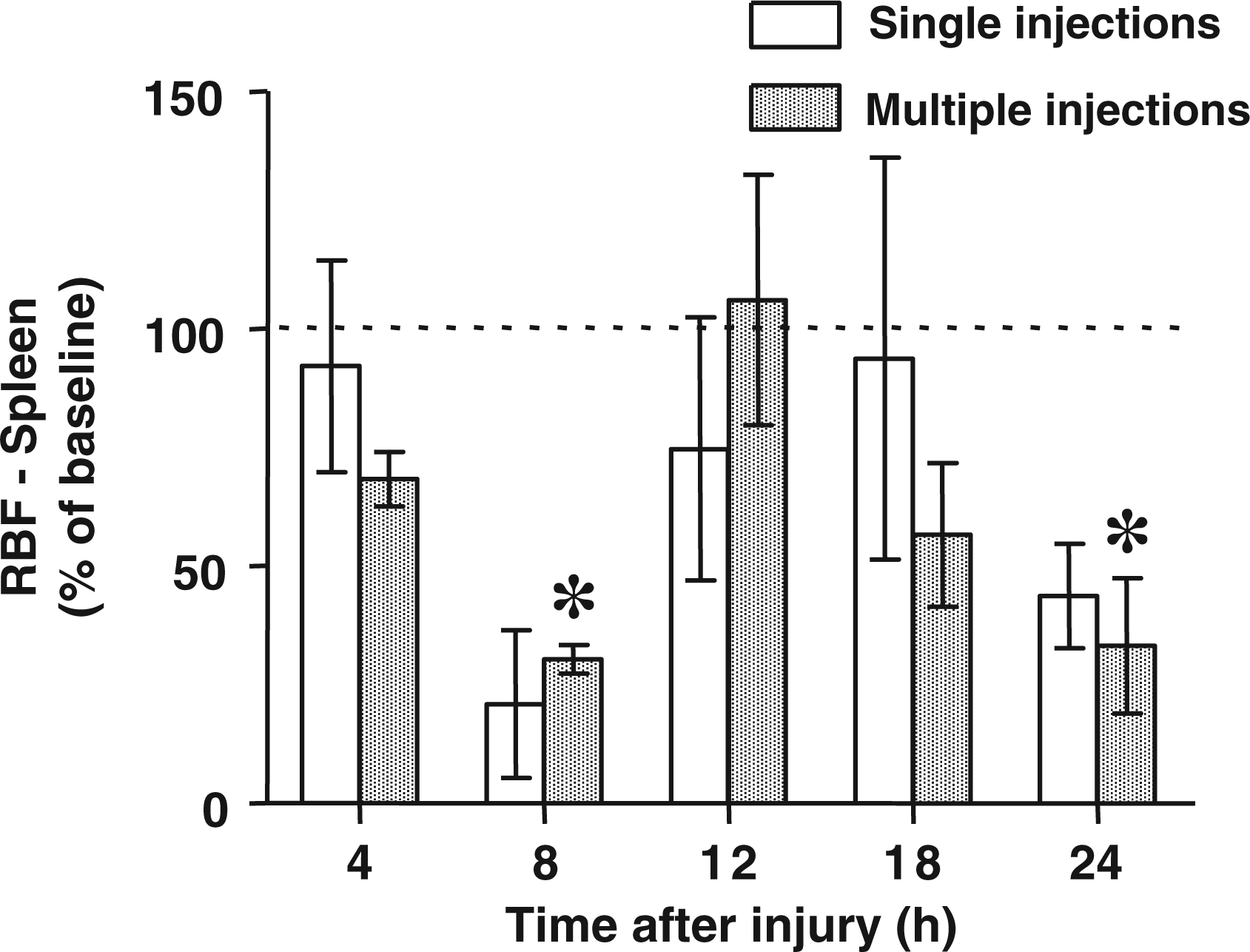
The regional blood flows to the pancreas and spleen were significantly decreased versus baseline values at various time points after the induction of sepsis without significant differences between groups (Figures 2 and 3).
Regional blood flow (RBF) to the pancreas at various time points after the induction of sepsis determined by single versus multiple injections of fluorescent microspheres. The data are presented as % of baseline values. Baseline is represented by the dotted line. Differences between groups were detected by t-test. *P < 0.05 versus baseline. Regional blood flow (RBF) to the spleen at various time points after the induction of sepsis determined by single versus multiple injections of fluorescent microspheres. The data are presented as % of baseline values. Baseline is represented by the dotted line. Differences between groups were detected by t-test. *P < 0.05 versus baseline.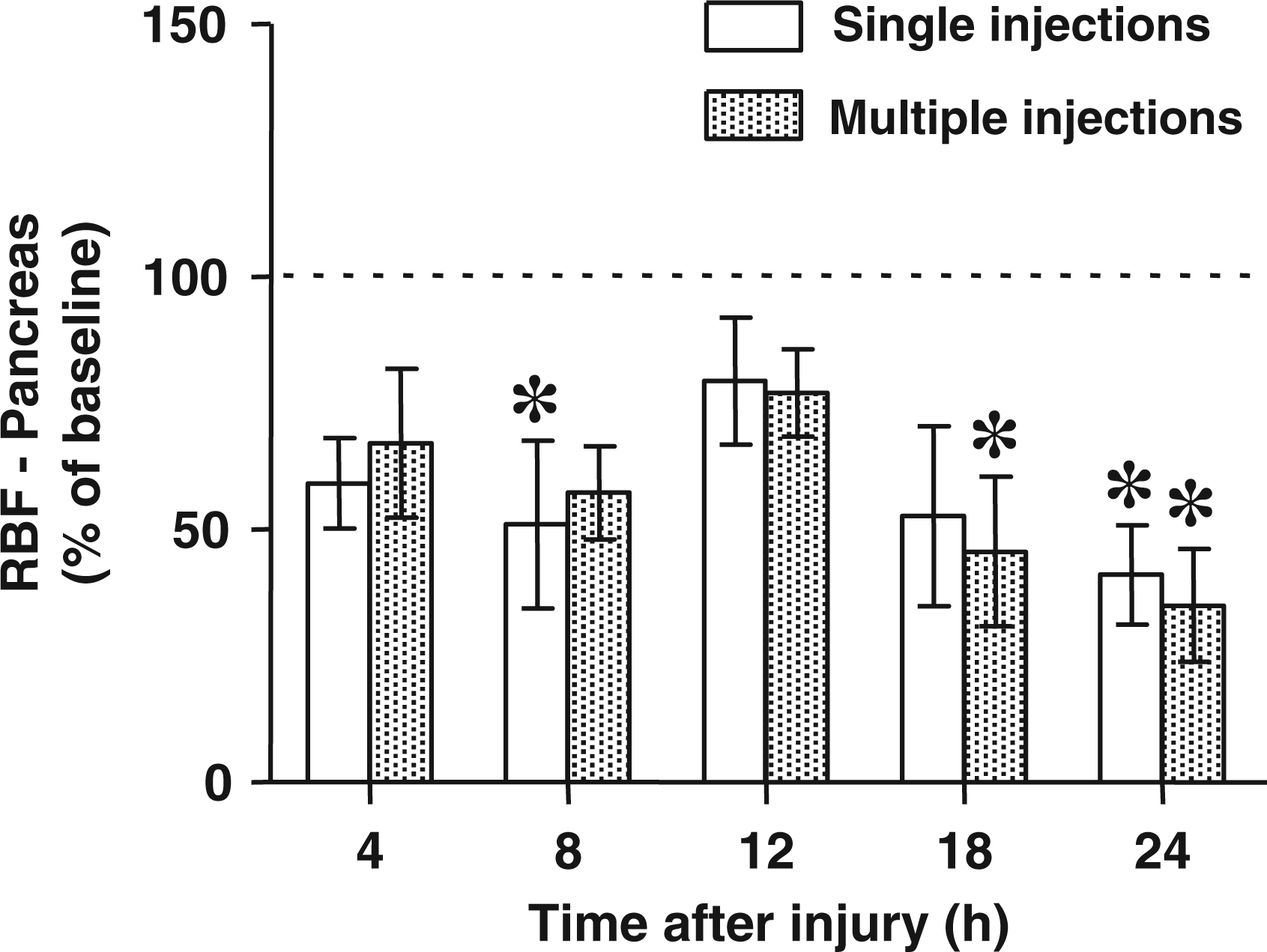
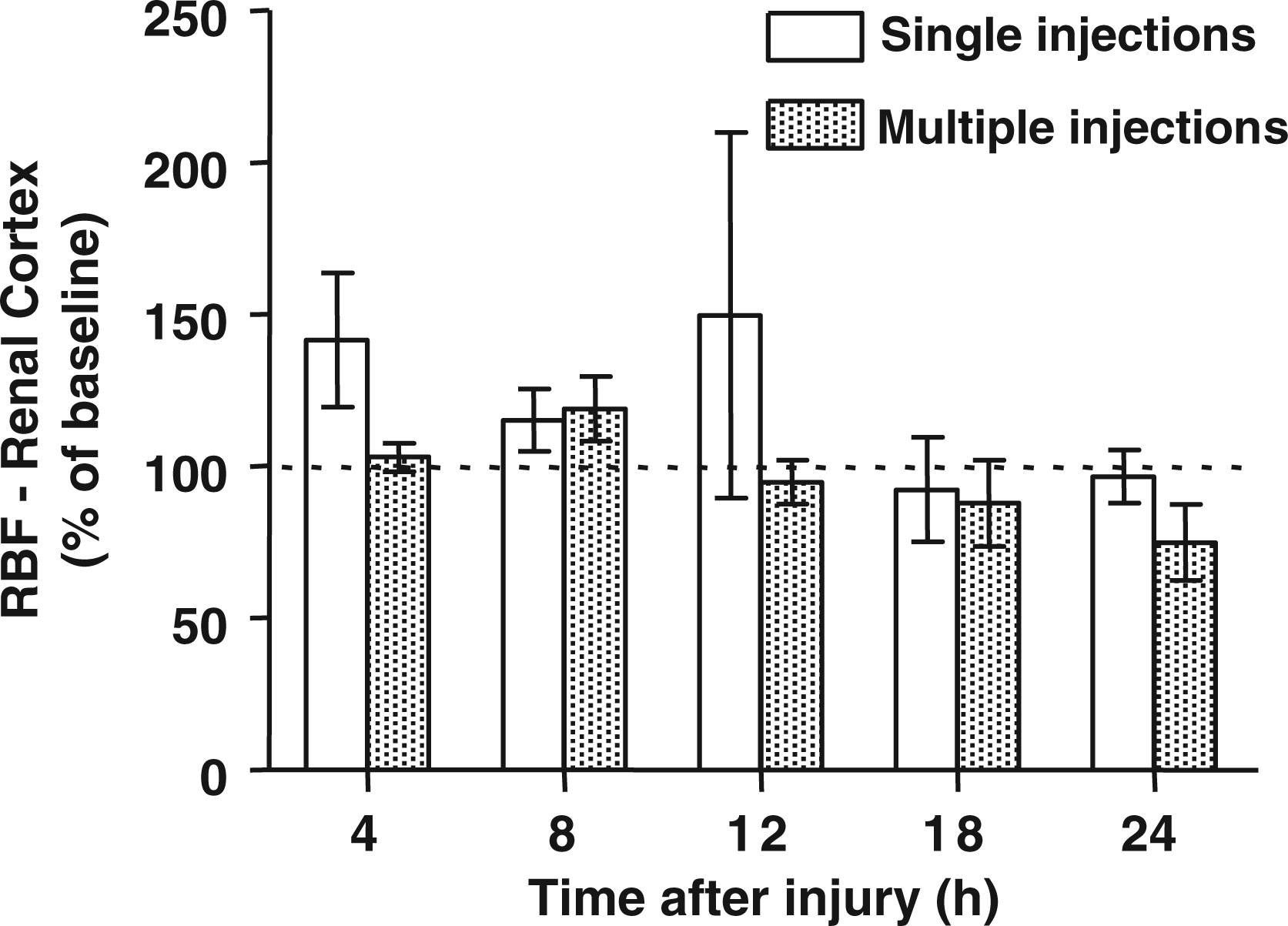
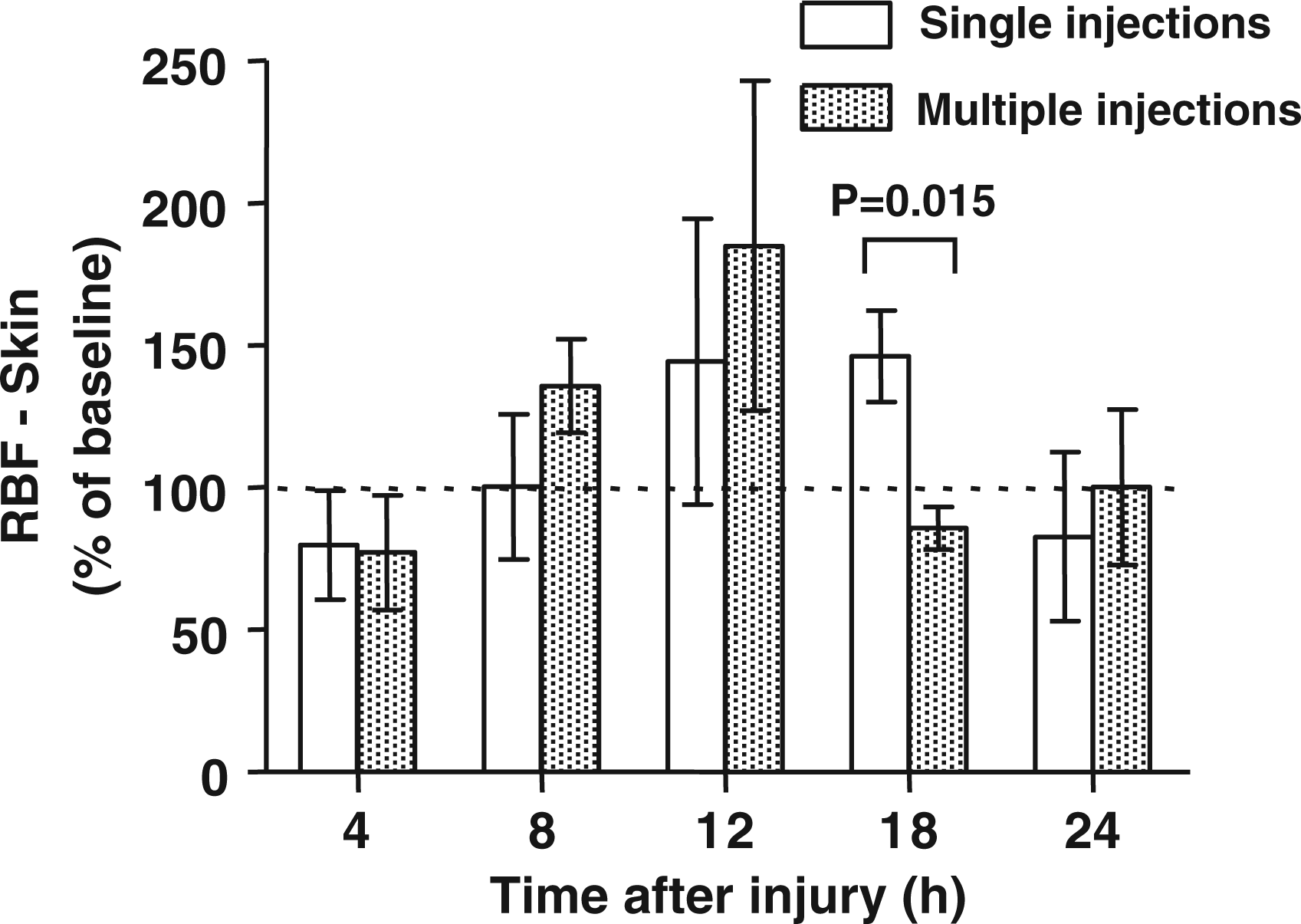
The blood flows to the ileum, renal cortex, and skin were not significantly different from the baseline during the experimental period (Figures 4
–6). The blood flow was significantly higher at 12 h and lower at 18 h after the injury in the multiple versus the single injection group.
Regional blood flow (RBF) to the ileum at various time points after the induction of sepsis determined by single versus multiple injections of fluorescent microspheres. The data are presented as % of baseline values. Baseline is represented by the dotted line. Differences between groups were detected by t-test. Regional blood flow (RBF) to the renal cortex at various time points after the induction of sepsis determined by single versus multiple injections of fluorescent microspheres. The data are presented as % of baseline values. Baseline is represented by the dotted line. Differences between groups were detected by t-test. Regional blood flow (RBF) to the skin at various time points after the induction of sepsis determined by single versus multiple injections of fluorescent microspheres. The data are presented as % of baseline values. Baseline is represented by the dotted line. Differences between groups were detected by t-test.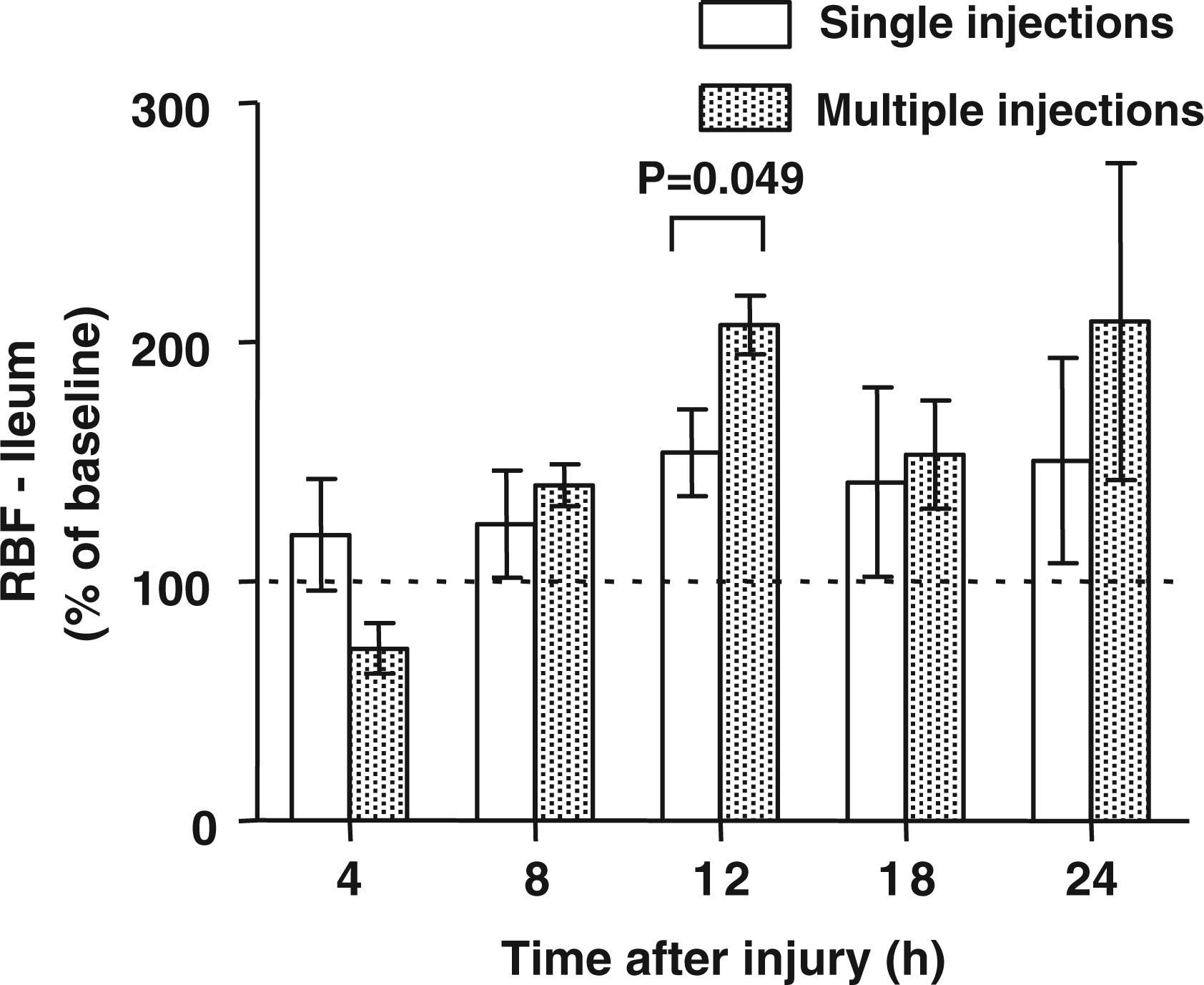
Discussion
The present study demonstrates that multiple injections of microspheres as compared to single injections delivered similar results of regional organ blood measurements in our established ovine sepsis model.
As mentioned previously in detail, concerns about the fluorescent microsphere technique for the determination of regional blood flow include the size and quantity of microspheres. If the spheres are too large in size or quantity, they may obstruct the vascular bed and impair microcirculatory blood flow. 5,12 This may become a significant source of error, particularly when multiple injections of microspheres are applied. Furthermore, there is concern about the spectral overlap when applying multiple injections of colored microspheres. This may also affect the tissue sample analysis and lead to significant measuring errors with an increasing number of injected spheres. 13
In our established ovine model of sepsis, we utilized the fluorescent microsphere technique to assess the pathophysiological alterations during sepsis and to test the effects of new treatment strategies on regional blood flow to different organs. 9,14,15 We considered the multiple injection technique to be the method of choice because it allows testing organ blood flow at various time points in the same animals. However, the effects of multiple versus single injections of microspheres on regional blood flow in our model have not yet been compared. The possible negative effects of multiple microsphere injections have not been sufficiently studied.
Although the multiple microsphere injection technique has been utilized in several different models before, we believe that the use of microspheres in a sepsis model requires especial attention. Sepsis itself is typically associated with significant impairment of microcirculatory blood flow. The regulation of vascular tone and microcirculatory flow is influenced by the amount of nitric oxide (NO) production. 16 NO is an endogenous vasodilator that is generated from L-arginine by a family of enzymes called NO synthases. Excessive production of NO is believed to be critically involved in the pathophysiology of sepsis-related hemodynamic derangements and multiple organ failure. 16 –18 The amount of NO production within the vascular system during sepsis may vary at different anatomical sites, causing different degrees of vasodilation. This may result in underperfusion of metabolically active tissue and overperfusion of metabolically inactive tissues, ultimately contributing to tissue hypoxia and end organ damage. 19 However, the distribution of regional blood flow cannot be reliably predicted owing to the complex pathophysiological variances of systemic inflammatory disease. 18 Therefore, the measurement of regional blood flows by the injection of fluorescent microspheres appears to be a useful tool for the determination of the effects of various treatment strategies during experimental sepsis.
In addition, previous investigations have demonstrated that excessive NO may not only influence vascular tone, but may also exert cytotoxic effects by reacting with superoxide radicals from activated neutrophils, thereby yielding reactive oxygen and nitrogen species such as peroxynitrite (ONOO−). ONOO− may induce cell damage by oxidizing and nitrating/nitrosating proteins and lipids 20,21 and may induce excessive activation of the nuclear repair enzyme poly(ADP ribose) polymerase (PARP), 22,23 which may cause ATP depletion and cell damage. 23,24 Together, these sepsis-associated alterations promote maldistribution of blood flow, endothelial damage, microvascular hyperpermeability, and ultimately multiple organ failure. It has previously been demonstrated that experimental acute lung injury and bacterial inoculation in sheep is reliably associated with increased NO production, ONOO− formation, PARP activation, as well as microvascular dysfunction and hyperpermeability, resulting in severe multiple organ dysfunction. 8,16 –18,25,26 The effects of different innovative treatment strategies on regional blood flow have previously been tested in the same animal model. These previous experimental studies have shown that either administration of NO synthase inhibitors or an ONOO− decomposition catalyst partially reverses the microcirculatory derangements during sepsis as assessed by the fluorescent microsphere technique. 16,27
From histological examinations in previous studies with the same model, we know that pneumonia-induced sepsis in sheep leads to significant effects on the tissue of the lung and extrapulmonary organs. Thus, it may be assumed that preceding tissue destruction during sepsis interferes with the accumulated microspheres and influences the post-mortem tissue analysis. The injected microspheres at earlier time points may partially vanish at the later time points when significant tissue damage has occurred. Another possibility is that the microspheres injected later during the course of sepsis become increasingly ‘stuck’ in the microvasculature because previously injected spheres obstruct the drainage. In this regard, it is worth mentioning that the blood flow results indicated higher flows in the multiple injection group in the trachea (18 h) and ileum (12 h). The mechanism causing these differences should be tested in future studies to compare regional blood flow by using different methods such as ultrasonic flow meters.
Uncertainty about the reliability of the results following multiple microsphere injections may have led to the preferential use of single injections in many research laboratories. This inevitably results in the need for a larger number of animals when multiple time points are studied. Therefore, the results of the present study can help reduce the quantity of animals required in future experiments. In the current experiment, only three out of 30 comparisons between groups showed a statistically significant difference. Importantly, the blood flow was higher on two of the three occasions, indicating that the multiple microsphere injections did not reduce the regional flow.
In conclusion, the current study demonstrates that multiple versus single injections of fluorescent microspheres in sheep with acute lung injury and pneumonia-induced sepsis does not cause detectable differences in key hemodynamic variables between groups, suggesting the multiple injection technique has negligible drawbacks. Importantly, the majority of regional blood flow measurements were not significantly different between groups. This finding may help reduce the quantity of animals used in future experiments with this model.
Footnotes
Funding
This study was supported by grants from the American Heart Association 0565028Y, Shriners Burns Institute 8450, 8954, and 8630.
