Abstract
Objective:
To estimate the proportions and correlates of Australian young people who consulted with health professionals or used services via digital technologies for their mental health in 2020–2022.
Methods:
Data from 16- to 24-year-olds (N = 1620) in the 2020–2022 Australian National Survey of Mental Health and Wellbeing were analysed to estimate proportions, population counts and unadjusted odds ratios of past-year health professional consultations and use of services via digital technology for mental health within geographic regions. Logistic regression models explored socio-economic, psychosocial and clinically meaningful correlates of past-year consultation in the full sample, metro subgroup and regional, rural and remote subgroup.
Results:
In total, 24.2% of Australian young people consulted with a health professional for their mental health in the past year. Of those with a probable 12-month Diagnostic and Statistical Manual of Mental Disorders (4th ed.; DSM-IV) mental health condition, 46.3% consulted a health professional. This proportion differed by sex (male: 34.2%, female: 55.6%) and symptom severity (mild: 20.0%, moderate: 47.8%, severe: 66.0%) but did not vary by geographic region. One-in-ten (9.9%) young people used other services via digital technologies for their mental health in the past year, doubling among those with a probable 12-month mental health condition (18.8%), and increasing with severity (mild or moderate: 14.2%, severe: 33.6%). Different factors were associated with service use in different regions.
Conclusion:
Experiences of young people accessing mental health care in Australia differ by geographic region of residence, neighbourhood disadvantage, sex and disorder class. Australia’s mental health care system must facilitate diverse pathways to care that are responsive to young people’s needs and preferences.
Introduction
In 2020–2022, more than one-third of Australian young people (aged 16–24) met criteria for a 12-month mental health condition (mental or substance use disorder) (Macauley et al., in press; Volkow et al., 2021), higher than any other age group in Australia (Slade et al., 2024). Yet less than half of young people consulted with a health professional for their mental health in the same year (Harris et al., 2025). Failing to receive timely mental health care can have significant negative flow-on effects, such as health and social disparities later in life (Allen et al., 2014; Pavalko and Caputo, 2013). These may include ongoing or later recurrence of mental health symptoms (Essau et al., 2014; Thapar et al., 2022; Weavers et al., 2021); interruptions to education or employment (Butterworth and Leach, 2018; Clayborne et al., 2019; Olesen et al., 2013); lower income and living standards (Gibb et al., 2010); delinquency and social exclusion (Murray et al., 2022); lower life satisfaction (Schlack et al., 2021); or suicide (Miranda-Mendizabal et al., 2019).
On top of the many challenges young people manage during late adolescence (aged 16+), a definition that has recently been reconceptualised into early emerging adulthood (up to 24 years old) to account for delayed timing of role transitions (Sawyer et al., 2018), they must also navigate a mental health care system that has traditionally forced transition from the paediatric to adult care system at age 18 years (McGorry, 2007). The headspace model was introduced in 2006 to bridge this gap, providing primary mental health care to young people aged 12–25 years (Rickwood et al., 2019). Simultaneously, the Better Access initiative was established to increase access to primary care for Australians of all ages (Teesson et al., 2024). Modality options have since broadened to include telehealth, which may be relatively more appealing to young people (Orsolini et al., 2021) and increased during the COVID-19 pandemic (Snoswell et al., 2022). Although the proportion of Australian young people receiving mental health care has recently increased (Harris et al., 2025), barriers preventing young people from accessing care persist. These include structural barriers (long wait times, prohibitive cost), information barriers (lack of awareness of services), attitudinal barriers (stigma and shame) and distrust of the mental health care system (concerns that needs would not be met, concerns regarding confidentiality and anonymity) (Brown et al., 2016; Gulliver et al., 2010; Iskra et al., 2018).
Barriers to mental health care may be further exacerbated by the geographic region in which a young person lives. Disproportionately few general practitioners, relative to the population, work in small rural towns compared to all other geographic regions (Cortie et al., 2024), and disproportionately few mental health specialists work in rural, regional and remote areas compared to metro areas (Australian Institute of Health and Welfare, 2024). Furthermore, young people living regionally and rurally report additional barriers to accessing mental health care compared to those in metro areas. These include heightened concerns around stigma, shame and confidentiality, insufficient culturally sensitive services, inaccessible distance to services, inaccessible service hours, technological issues and lack of youth mental health specialists (Aisbett et al., 2007; Boyd et al., 2011; Capon et al., 2023; Kavanagh et al., 2023). Disparities in mental health service access have also been observed between sexes. Among young Australians with a probable mental health condition, those recorded male at birth tend to use services less than those recorded female at birth (Harris et al., 2025). This finding has been consistently reported in the literature, indicating a sex-based (and gendered) dimension to mental health service access (Radez et al., 2021; Lau et al., 2013; Tran and Silvestri-Elmore, 2021).
Uncovering the nuanced patterns of mental health service use among young people may highlight opportunities for advances in policy and practice that could bring the Australian mental health care system closer to access targets (Golden and Wendel, 2020; National Mental Health Service Planning Framework, 2024; Whiteford et al., 2023). Notably, identifying clinical need is an important part of this discussion (Hickie et al., 2025). We conceptualise ‘service use’ as a point within the client-centred process of accessing mental health care services, which spans from perceiving a need for mental health care, to the fulfilment of the need by the mental health care service, in line with Levesque et al. (2013). This definition places service use within the context of both demand-side factors (including the opportunity to perceive needs; to seek services; to reach services; to use the service; and to have the need for services met) and supply-side factors (including approachability; acceptability; availability and accommodation; affordability; and appropriateness of the service).
The present study uses the largest-ever national sample of Australian epidemiological mental health service use data collected from young people to explore patterns of service use for mental health among this group. We explore relationships between service use and sex recorded at birth, geographic region of residence and clinical indicators of service need (including probable mental health condition, distress) alongside ‘upstream’ social determinants previously identified as correlates of a probable mental health condition in this age group (Allen et al., 2014; Macauley et al., in press). Following the call by Robards et al. (2018), we also explore the use of services via digital technologies for mental health. We aim to (1) present 2020–2022 patterns of service use for mental health among young people by sex recorded at birth, geographic region of residence and mental health condition symptom severity and (2) to describe correlates of consultation with health professionals among Australian young people overall and separately for those living in metropolitan and regional, rural and remote areas.
Methods
Sample and survey design
We analysed data from the subset of all 1620 respondents aged 16–24 years who participated in the 2020–2022 Australian National Study of Mental Health and Wellbeing (NSMHWB), the national cross-sectional household survey conducted primarily face-to-face by the Australian Bureau of Statistics (ABS). The ABS randomly selected people aged 16–85 years living in private dwellings across all states and territories of Australia for participation (excluding residents of some remote [Modified Monash 6; MM6] and all very remote (MM7) areas, discrete Aboriginal and Torres Strait Islander communities and non-private dwellings). Further methodological information regarding survey design, sample selection and estimation methods (weighting) has been reported elsewhere (Australian Bureau of Statistics, 2023; Slade et al., 2024).
Measures
Supplementary Table 1 contains descriptions and details of all variables analysed in the current study. Outcomes were service use variables, measured using a service utilisation module developed by the ABS in consultation with subject matter experts. Outcome variables include self-reported consultations in the Australian Government Department of Health and Aged Care previous 12 months with health professionals (including general practitioners, psychiatrists, psychologists, other mental health or health professionals), overnight hospitalisations and use of other services via phone, Internet or another digital technology (separate to health professional consultations via phone/video) for mental health problems (e.g. Lifeline crisis support; online support groups). The World Mental Health Survey Initiative version of the Composite International Diagnostic Interview version 3.0 (WMH-CIDI 3.0) (Kessler and Üstün, 2004) was used to assess mental and substance use disorders (henceforth ‘mental health conditions’; Volkow et al., 2021). Criteria from the Diagnostic and Statistical Manual of Mental Disorders (4th ed.; DSM-IV) were used to diagnose probable 12-month mental health conditions. Respondent’s geographic region was classified by mapping their 2016 Statistical Area Level 1 (SA1) area codes to 2019 MM Model categories, which guide health resource allocation (Versace et al., 2021). Other covariates, including sex recorded at birth, were collected as part of the interview.
Positionality statement
In response to recent calls for reflexive practice in quantitative research (Jamieson et al., 2023), we position this study from the perspective of the lead author, a white cisgender woman at an Australian university. She is part of the same birth cohort as study respondents, from a metro area (Gadigal, Sydney) and has spent time in Dubbo (Wiradjuri Country), a large rural town, to understand local mental health system contexts. She is both a consumer of, and carer within, the mental health care system, with both positive and distressing experiences. These identities and experiences have informed this study.
Data analysis
Data were analysed using R version 4.4.1 (R Core Team, 2024), within the secure ABS DataLab portal. We first examined overall service use patterns, reporting estimated proportions (%), 95% confidence intervals (CIs) and estimated population counts (EPCs) for past 12-month mental health service use by sex recorded at birth, geographic region of residence and mental health symptom severity. Patterns were explored in the full sample (N = 1620) and the mental health condition subsample (n = 594). Next, we analysed correlates of any past 12-month consultation with health professionals using univariable and multivariable logistic regression models, reporting estimated proportions (%), 95% CIs, unadjusted odds ratios (uORs), adjusted odds ratios (aORs) and Wald chi2 test statistics in the full sample, metro subgroup (n = 1316) and regional, rural and remote subgroup (n = 304). The 95% CIs for prevalence estimates and ORs were generated using the jackknife replication method (Rust and Rao, 1996) to account for complex sampling. We assessed all models for adequate sample size, separation and multicollinearity.
Base multivariable regression models for all three samples included sex recorded at birth, neighbourhood disadvantage, lifetime sexual assault, distress and probable mental health condition (see Supplementary methods for more information). We engaged a planned replacement approach to measure probable mental health condition in four different ways (any mental health condition; mental health condition class [anxiety disorder, mood disorder, substance use disorder]; co-occurring mental health condition classes; symptom severity) for each sample (following prior research, Macauley et al., in press; Teesson et al., 2010) (see Supplementary Table 1). Sample size was insufficient to report on those who described their sex recorded at birth as a term other than ‘male’ or ‘female’, to report on respondents’ gender or to report on some service use patterns by geographic region of residence. Substance use disorder and symptom severity were excluded from the regional, rural and remote sample due to ABS data disclosure rules. Variance inflation factors (VIFs) were consistently below 3, all C-statistics consistently 81 or above, and residual degrees of freedom consistently 46 and above for all models.
Results
Key respondent characteristics are presented in Table 1.
Characteristics of Australian young people, including sex recorded at birth and geographic region of residence (N = 1620).
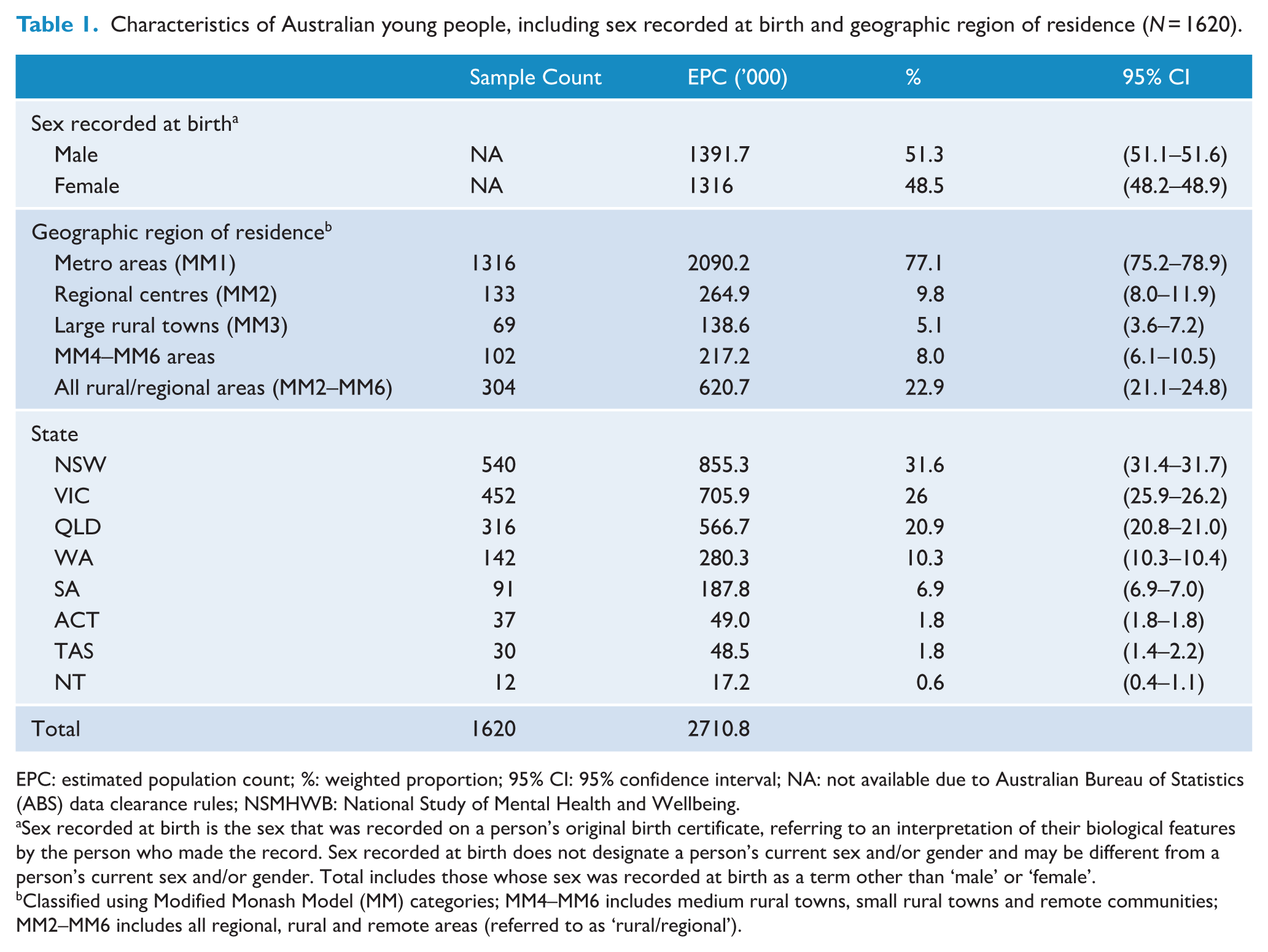
EPC: estimated population count; %: weighted proportion; 95% CI: 95% confidence interval; NA: not available due to Australian Bureau of Statistics (ABS) data clearance rules; NSMHWB: National Study of Mental Health and Wellbeing.
Sex recorded at birth is the sex that was recorded on a person’s original birth certificate, referring to an interpretation of their biological features by the person who made the record. Sex recorded at birth does not designate a person’s current sex and/or gender and may be different from a person’s current sex and/or gender. Total includes those whose sex was recorded at birth as a term other than ‘male’ or ‘female’.
Classified using Modified Monash Model (MM) categories; MM4–MM6 includes medium rural towns, small rural towns and remote communities; MM2–MM6 includes all regional, rural and remote areas (referred to as ‘rural/regional’).
Patterns of service use for mental health among young people
Table 2 displays patterns of past 12-month service use for mental health problems among young people in Australia in 2020–2022. Approximately one quarter (24.2%, 95% CI = 22.2–26.4) of young people consulted with a health professional. In total, 9.9% (95% CI = 8.5–11.5) of young people used phone or digital technologies to access other services. Those recorded female at birth used a greater variety of services examined than those recorded male at birth. No differences in proportions of service use were observed across geographic regions of residence (see Table 2).
Consultation with health professionals for mental health in the past 12 months among Australian young people by sex recorded at birth and geographic region of residence (N = 1620).
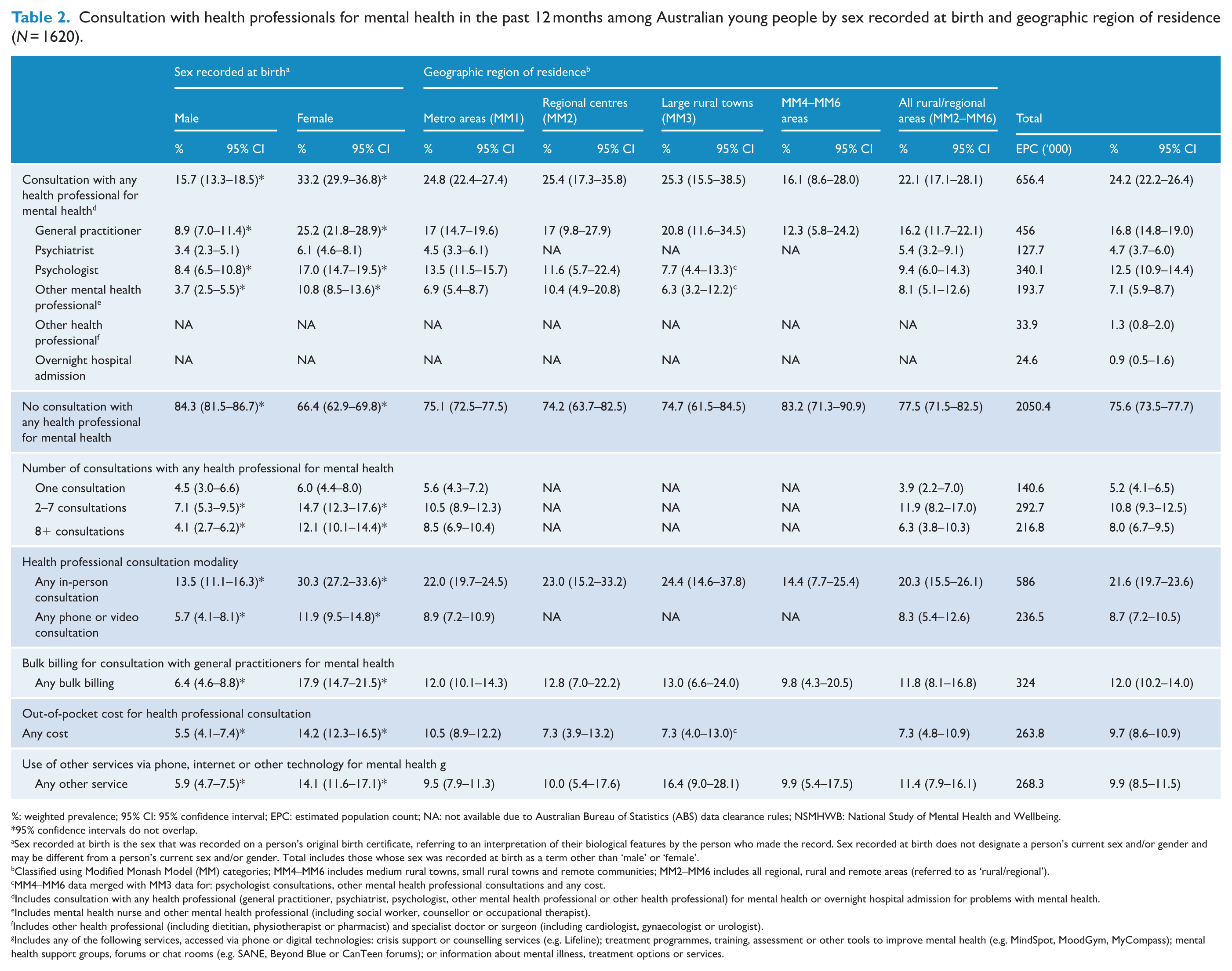
%: weighted prevalence; 95% CI: 95% confidence interval; EPC: estimated population count; NA: not available due to Australian Bureau of Statistics (ABS) data clearance rules; NSMHWB: National Study of Mental Health and Wellbeing.
95% confidence intervals do not overlap.
Sex recorded at birth is the sex that was recorded on a person’s original birth certificate, referring to an interpretation of their biological features by the person who made the record. Sex recorded at birth does not designate a person’s current sex and/or gender and may be different from a person’s current sex and/or gender. Total includes those whose sex was recorded at birth as a term other than ‘male’ or ‘female’.
Classified using Modified Monash Model (MM) categories; MM4–MM6 includes medium rural towns, small rural towns and remote communities; MM2–MM6 includes all regional, rural and remote areas (referred to as ‘rural/regional’).
MM4–MM6 data merged with MM3 data for: psychologist consultations, other mental health professional consultations and any cost.
Includes consultation with any health professional (general practitioner, psychiatrist, psychologist, other mental health professional or other health professional) for mental health or overnight hospital admission for problems with mental health.
Includes mental health nurse and other mental health professional (including social worker, counsellor or occupational therapist).
Includes other health professional (including dietitian, physiotherapist or pharmacist) and specialist doctor or surgeon (including cardiologist, gynaecologist or urologist).
Includes any of the following services, accessed via phone or digital technologies: crisis support or counselling services (e.g. Lifeline); treatment programmes, training, assessment or other tools to improve mental health (e.g. MindSpot, MoodGym, MyCompass); mental health support groups, forums or chat rooms (e.g. SANE, Beyond Blue or CanTeen forums); or information about mental illness, treatment options or services.
Patterns of service use for mental health among young people with a probable mental health condition
Tables 3 and 4 present patterns of past 12-month service use for mental health among young people with a probable mental health condition in Australia in 2020–2022. Almost half (46.3%, 95% CI = 41.9-50.8) had consulted with a health professional. Young people with a probable mental health condition most commonly consulted with general practitioners (35.4%), followed by psychologists (24.9%), other mental health professionals (13.8%) and psychiatrists (10.4%). Sample size was insufficient to report on overnight hospitalisation.
Young people with a probable mental health condition consulted in-person twice as commonly (41.0%) as they did via phone or video (19.7%). One quarter (25.4%) of young people with a probable mental health condition were bulk billed by a general practitioner at least once, and just under one in five (18.5%) personally paid out-of-pocket costs for any consultation. In total, 18.8% (95% CI = 15.7–22.4) of young people with a probable mental health condition accessed other services via phone or digital technology.
Similar to the full sample (Table 2), those recorded female at birth used a greater variety of services examined than those recorded male at birth. We observed fewer significant sex differences in the probable mental health condition group, with overlapping CIs for the proportions of those who consulted with a psychologist, had two to seven consultations with any health professional and consulted a health professional via phone/video (see Table 3). No differences in proportions of service use were observed across geographic region of residence (see Table 3).
Consultation with health professionals for mental health in the past 12 months among Australian young people meeting criteria for a 12-month mental health condition by sex recorded at birth and geographic region of residence (n = 594).
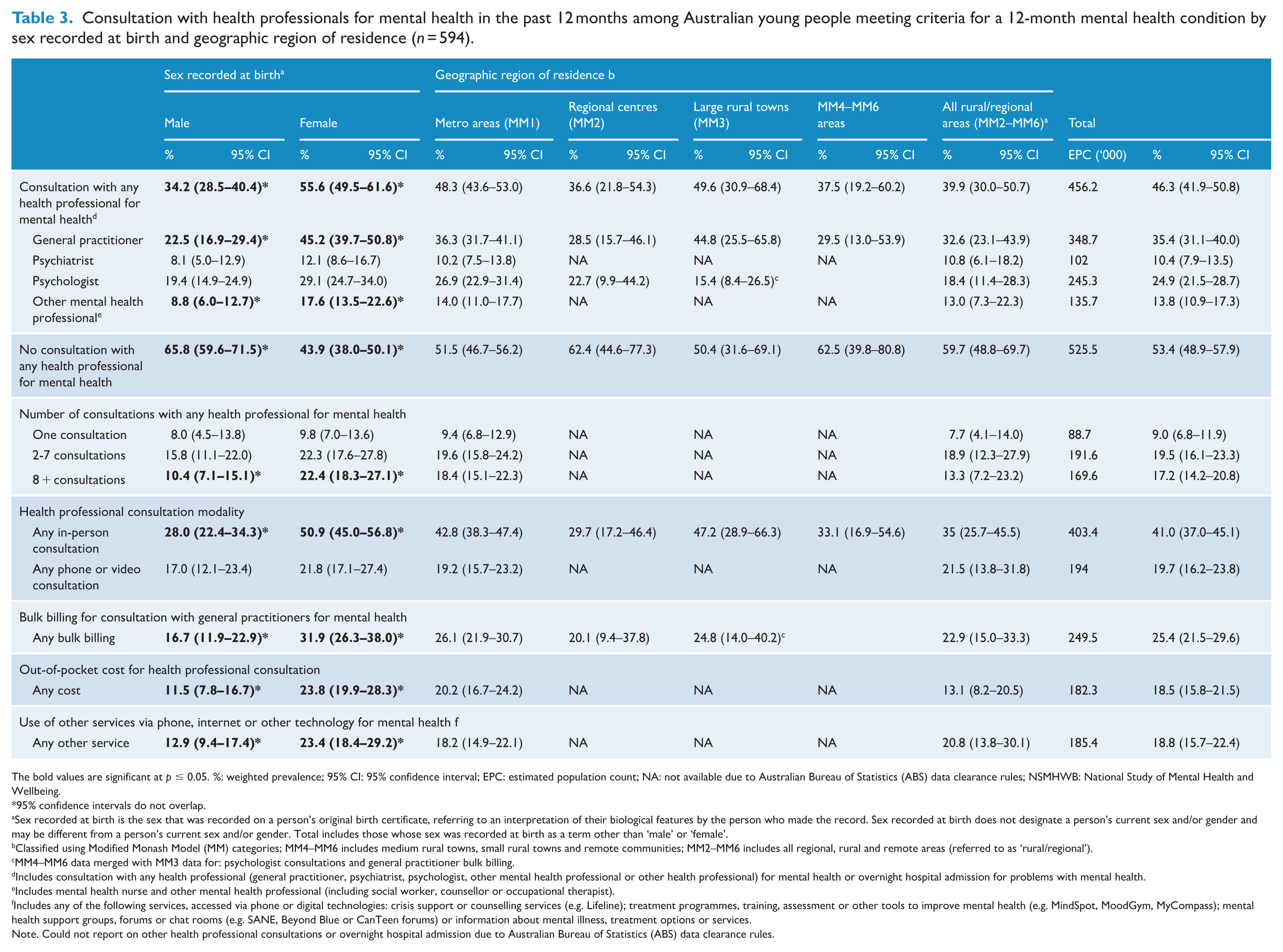
The bold values are significant at p ≤ 0.05. %: weighted prevalence; 95% CI: 95% confidence interval; EPC: estimated population count; NA: not available due to Australian Bureau of Statistics (ABS) data clearance rules; NSMHWB: National Study of Mental Health and Wellbeing.
95% confidence intervals do not overlap.
Sex recorded at birth is the sex that was recorded on a person’s original birth certificate, referring to an interpretation of their biological features by the person who made the record. Sex recorded at birth does not designate a person’s current sex and/or gender and may be different from a person’s current sex and/or gender. Total includes those whose sex was recorded at birth as a term other than ‘male’ or ‘female’.
Classified using Modified Monash Model (MM) categories; MM4–MM6 includes medium rural towns, small rural towns and remote communities; MM2–MM6 includes all regional, rural and remote areas (referred to as ‘rural/regional’).
MM4–MM6 data merged with MM3 data for: psychologist consultations and general practitioner bulk billing.
Includes consultation with any health professional (general practitioner, psychiatrist, psychologist, other mental health professional or other health professional) for mental health or overnight hospital admission for problems with mental health.
Includes mental health nurse and other mental health professional (including social worker, counsellor or occupational therapist).
Includes any of the following services, accessed via phone or digital technologies: crisis support or counselling services (e.g. Lifeline); treatment programmes, training, assessment or other tools to improve mental health (e.g. MindSpot, MoodGym, MyCompass); mental health support groups, forums or chat rooms (e.g. SANE, Beyond Blue or CanTeen forums) or information about mental illness, treatment options or services.
Note. Could not report on other health professional consultations or overnight hospital admission due to Australian Bureau of Statistics (ABS) data clearance rules.
Table 4 indicates that in 2020–2022, one-fifth (20%) of young people with mild symptoms, half (47.8%) of young people with moderate symptoms, and two thirds (66.0%) of young people with severe symptoms consulted with a health professional for their mental health. While Table 4 shows that service use was generally more common among those with more severe symptoms, there were no significant differences in the frequency of health professional consultation by symptom severity. The proportion of those who consulted with a psychologist or consulted via phone or video did not differ between those with moderate and severe symptoms (see Table 4). A greater proportion of young people experiencing severe symptoms (33.6%) compared to mild or moderate symptoms (14.2%) used phone or digital technology to access other services for their mental health.
Consultation with health professionals for mental health in the past 12 months among Australian young people meeting criteria for a 12-month mental health condition by symptom severity (n = 594).
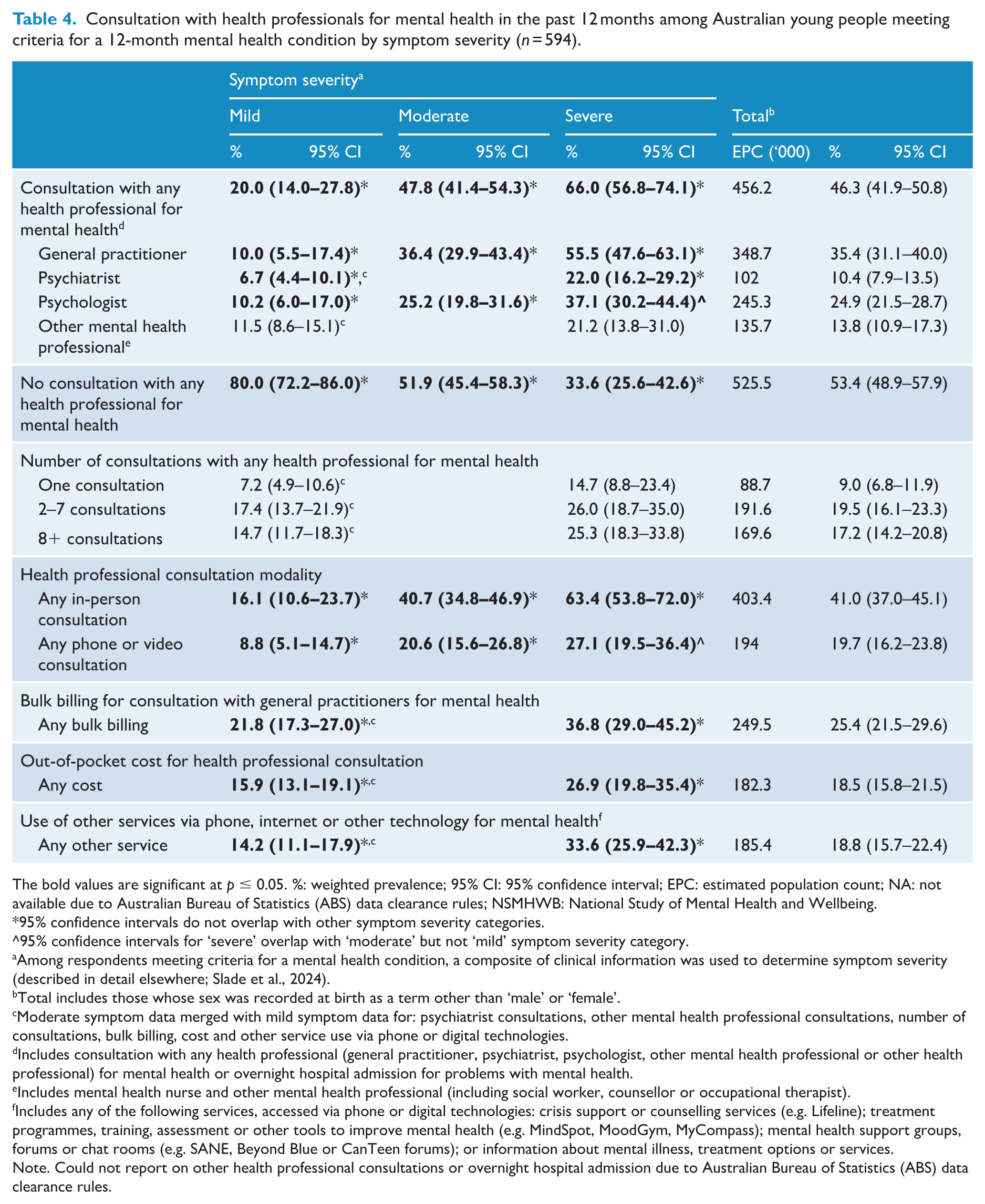
The bold values are significant at p ≤ 0.05. %: weighted prevalence; 95% CI: 95% confidence interval; EPC: estimated population count; NA: not available due to Australian Bureau of Statistics (ABS) data clearance rules; NSMHWB: National Study of Mental Health and Wellbeing.
95% confidence intervals do not overlap with other symptom severity categories.
^95% confidence intervals for ‘severe’ overlap with ‘moderate’ but not ‘mild’ symptom severity category.
Among respondents meeting criteria for a mental health condition, a composite of clinical information was used to determine symptom severity (described in detail elsewhere; Slade et al., 2024).
Total includes those whose sex was recorded at birth as a term other than ‘male’ or ‘female’.
Moderate symptom data merged with mild symptom data for: psychiatrist consultations, other mental health professional consultations, number of consultations, bulk billing, cost and other service use via phone or digital technologies.
Includes consultation with any health professional (general practitioner, psychiatrist, psychologist, other mental health professional or other health professional) for mental health or overnight hospital admission for problems with mental health.
Includes mental health nurse and other mental health professional (including social worker, counsellor or occupational therapist).
Includes any of the following services, accessed via phone or digital technologies: crisis support or counselling services (e.g. Lifeline); treatment programmes, training, assessment or other tools to improve mental health (e.g. MindSpot, MoodGym, MyCompass); mental health support groups, forums or chat rooms (e.g. SANE, Beyond Blue or CanTeen forums); or information about mental illness, treatment options or services.
Note. Could not report on other health professional consultations or overnight hospital admission due to Australian Bureau of Statistics (ABS) data clearance rules.
Correlates of any consultation with health professionals for mental health
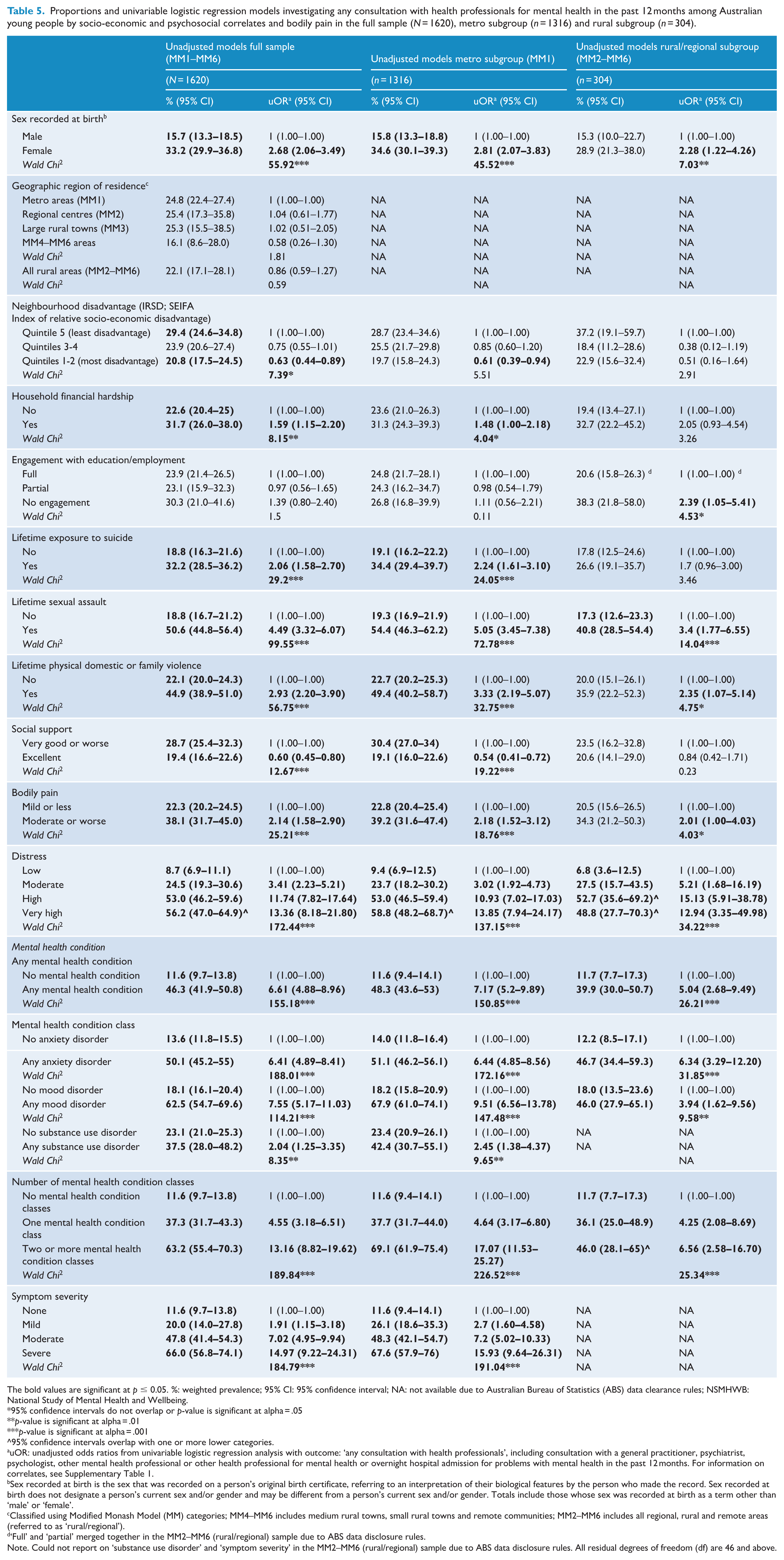
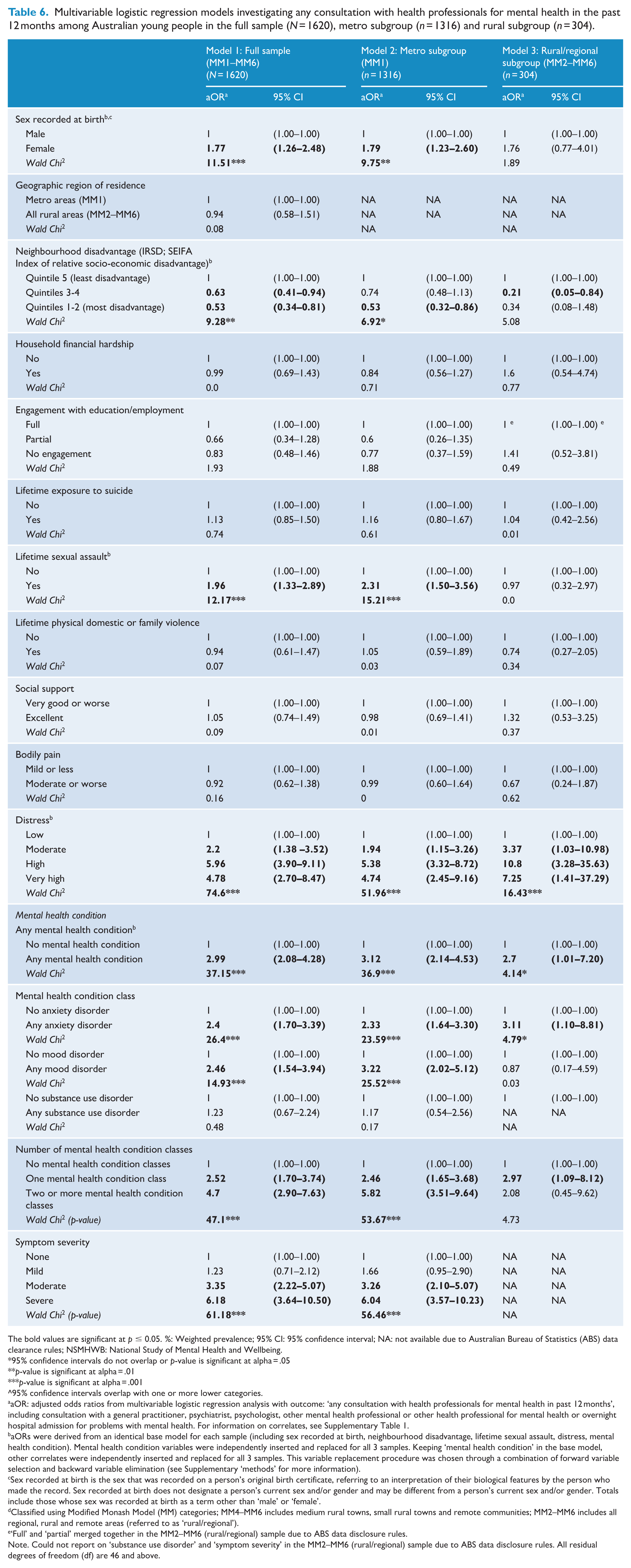
Proportions and unadjusted odds of consulting a health professional for mental health are presented for each correlate in Table 5. Table 6 displays adjusted odds ratios (aORs) for the multivariable analysis in the full sample, metro subgroup and regional, rural and remote subgroup. Several clinical correlates were uniquely correlated with higher odds of consulting with a health professional for mental health in all three samples (any mental health condition, aORs: 2.7–3.12; any anxiety disorder, aORs: 2.33–3.11; number of mental health condition classes, aORs: 2.08–5.82; past-30-day distress, aORs: 1.94–10.8). Greater neighbourhood disadvantage was uniquely correlated with lower odds of consulting for mental health in all samples (aORs: 0.21–0.63). In the metro but not regional, rural and remote subgroup, female sex recorded at birth (aORs: 1.77–1.79) and lifetime sexual assault (1.96–2.31) were uniquely correlated with higher odds of consulting for mental health problems.
Proportions and univariable logistic regression models investigating any consultation with health professionals for mental health in the past 12 months among Australian young people by socio-economic and psychosocial correlates and bodily pain in the full sample (N = 1620), metro subgroup (n = 1316) and rural subgroup (n = 304).
The bold values are significant at p ≤ 0.05. %: weighted prevalence; 95% CI: 95% confidence interval; NA: not available due to Australian Bureau of Statistics (ABS) data clearance rules; NSMHWB: National Study of Mental Health and Wellbeing.
95% confidence intervals do not overlap or p-value is significant at alpha = .05
p-value is significant at alpha = .01
p-value is significant at alpha = .001
^95% confidence intervals overlap with one or more lower categories.
uOR: unadjusted odds ratios from univariable logistic regression analysis with outcome: ‘any consultation with health professionals’, including consultation with a general practitioner, psychiatrist, psychologist, other mental health professional or other health professional for mental health or overnight hospital admission for problems with mental health in the past 12 months. For information on correlates, see Supplementary Table 1.
Sex recorded at birth is the sex that was recorded on a person’s original birth certificate, referring to an interpretation of their biological features by the person who made the record. Sex recorded at birth does not designate a person’s current sex and/or gender and may be different from a person’s current sex and/or gender. Totals include those whose sex was recorded at birth as a term other than ‘male’ or ‘female’.
Classified using Modified Monash Model (MM) categories; MM4–MM6 includes medium rural towns, small rural towns and remote communities; MM2–MM6 includes all regional, rural and remote areas (referred to as ‘rural/regional’).
‘Full’ and ‘partial’ merged together in the MM2–MM6 (rural/regional) sample due to ABS data disclosure rules.
Note. Could not report on ‘substance use disorder’ and ‘symptom severity’ in the MM2–MM6 (rural/regional) sample due to ABS data disclosure rules. All residual degrees of freedom (df) are 46 and above.
Multivariable logistic regression models investigating any consultation with health professionals for mental health in the past 12 months among Australian young people in the full sample (N = 1620), metro subgroup (n = 1316) and rural subgroup (n = 304).
The bold values are significant at p ≤ 0.05. %: Weighted prevalence; 95% CI: 95% confidence interval; NA: not available due to Australian Bureau of Statistics (ABS) data clearance rules; NSMHWB: National Study of Mental Health and Wellbeing.
95% confidence intervals do not overlap or p-value is significant at alpha = .05
p-value is significant at alpha = .01
p-value is significant at alpha = .001
^95% confidence intervals overlap with one or more lower categories.
aOR: adjusted odds ratios from multivariable logistic regression analysis with outcome: ‘any consultation with health professionals for mental health in past 12 months’, including consultation with a general practitioner, psychiatrist, psychologist, other mental health professional or other health professional for mental health or overnight hospital admission for problems with mental health. For information on correlates, see Supplementary Table 1.
aORs were derived from an identical base model for each sample (including sex recorded at birth, neighbourhood disadvantage, lifetime sexual assault, distress, mental health condition). Mental health condition variables were independently inserted and replaced for all 3 samples. Keeping ‘mental health condition’ in the base model, other correlates were independently inserted and replaced for all 3 samples. This variable replacement procedure was chosen through a combination of forward variable selection and backward variable elimination (see Supplementary ‘methods’ for more information).
Sex recorded at birth is the sex that was recorded on a person’s original birth certificate, referring to an interpretation of their biological features by the person who made the record. Sex recorded at birth does not designate a person’s current sex and/or gender and may be different from a person’s current sex and/or gender. Totals include those whose sex was recorded at birth as a term other than ‘male’ or ‘female’.
Classified using Modified Monash Model (MM) categories; MM4–MM6 includes medium rural towns, small rural towns and remote communities; MM2–MM6 includes all regional, rural and remote areas (referred to as ‘rural/regional’).
‘Full’ and ‘partial’ merged together in the MM2–MM6 (rural/regional) sample due to ABS data disclosure rules.
Note. Could not report on ‘substance use disorder’ and ‘symptom severity’ in the MM2–MM6 (rural/regional) sample due to ABS data disclosure rules. All residual degrees of freedom (df) are 46 and above.
Discussion
We analysed the largest-ever national sample of Australian epidemiological mental health service use data collected from young people to explore patterns and correlates of past-12-month service use for mental health among this group. Broadly, we found that one quarter (24.2%) of emerging adults consulted a health professional for their mental health. Among those with a probable 12-month DSM-IV mental health condition (mental or substance use disorder, Volkow et al., 2021), only half (46.3%) consulted. This is a meaningful increase from the 2007 rates of 23.9% (Harris et al., 2025). Yet, when disaggregated by symptoms, it includes one fifth (20%) of those with mild symptoms, half (48%) of those with moderate symptoms, and two thirds (66%) of those with severe symptoms. This number is still well below the access target of 67% (mild: 50%, moderate: 80% and severe: 100%) across all ages proposed in the National Mental Health Service Planning Framework (2024). Our findings likely reflect a number of factors described in Levesque et al.’s (2013) health care access framework. For example, mental health care needs appear to be rising, as evidenced by the increasing prevalence of mental health conditions in this age group (McGorry et al., 2024; Slade et al., 2024). At the same time, these findings represent an increase in health professional consultations among this age group since 2007 (Harris et al., 2025), which may indicate increased accessibility of health professional consultations.
We also found one-in-five (18.8%) young people with a probable mental health condition, and 33.6% of those with severe symptoms, used phone or digital technology to access services other than health professional consultations (e.g. Lifeline crisis support; online support groups) for their mental health conditions. Following Levesque et al.’s framework, this may indicate such supply-side factors as the approachability, acceptability, availability or affordability of online services for young people experiencing mental health conditions. It may also reflect demand-side factors, for example, mental health literacy enabling the perception of a need for care, positive perceptions of online services or comfort using digital spaces. Recent Australian research indicates that many adolescents prefer using digital (online) and health services over school and phone services for their mental health (Islam et al., 2020). Taking our findings together, we propose the Australian mental health care system could respond to the preferences and needs of young people through investment in effective, evidence-based digital services for those who prefer it, alongside continued investment in traditional service pathways. Future research could also compare the appropriateness of service pathway options.
We compared patterns of service use that differed between those with and without a probable 12-month DSM-IV mental or substance use disorder [henceforth ‘mental health condition’ (Volkow et al., 2021)], between levels of symptom severity and between those of ‘male’ and ‘female’ sex recorded at birth. Those recorded female at birth reported higher rates of consultations compared to those recorded male at birth in the full and metro samples, but not the regional, rural and remote samples. Following Levesque et al.’s framework, these findings may indicate differences in the presence or perception of mental health needs, problems reaching services or cost barriers among those recorded male at birth and those living in regional, rural and remote areas. These different patterns may also indicate problems with service approachability, acceptability, availability and affordability for birth-assigned males and those in regional, rural and remote areas.
Prior research indicates those recorded female at birth face a higher prevalence of mental health conditions compared to those recorded male at birth (Macauley et al., in press). Consequently, higher need for mental health services may explain higher rates of service use among sex-recorded females in metro areas. However, this pattern remained within the subgroup of young people meeting criteria for a mental health condition, suggesting this is not the full picture. Although it is possible that even within this group, females have a higher need for care; it is also possible that these findings represent sex-based/gendered inequity in the mental health care system. Structural, cultural or social barriers including heightened stigma towards mental health experienced by men may prevent men and those recorded male at birth from accessing services (Chatmon, 2020).
Examination of the correlates of service use indicated that probable mental health condition, distress and neighbourhood disadvantage are uniquely associated with consulting a health professional for mental health among young people after controlling for all other covariates. Both 12-month mental health condition-related factors and past-30-day distress (generally) remained significantly positively associated with consulting a health professional for mental health when included in the same model. This pattern remained after controlling for other factors in all three samples. Notably, the finding that past 30-day heightened distress was a significant correlate of consultation suggests that acute distress may act as a trigger for help-seeking, highlighting the importance of timely access to care when young people reach crisis points. After controlling for the presence of an anxiety or mood disorder, the presence of a substance use disorder was no longer uniquely associated with consultation in the full and metro samples. This suggests that meeting criteria for a substance use disorder does not further increase the odds of consulting for mental health after accounting for the presence of a mood or anxiety disorder over and above condition-related factors present in mood and/or anxiety disorders. This finding is consistent with prior research and may reflect greater barriers to seeking and accessing care among those with a substance use disorder (Chapman et al., 2015; Ritter and O’Reilly, 2025) and/or shortfalls in the mental health care system in the treatment of co-occurring mental and substance use disorders (Marel et al., 2022).
Although we did not observe significant differences in proportions of service use when comparing geographic regions in the full sample, our subgroup analyses indicated that young people’s experience of consulting a health professional for mental health is not uniform across geographic regions. For example, consistent with previous Australian research, young people living in neighbourhoods with greater socio-economic disadvantage had lower odds of consulting for their mental health compared to those in less disadvantaged areas (Dawadi et al., 2024; Visser et al., 2021). However, this was not observed in the rural/regional subsample. It is possible that neighbourhood disadvantage, rather than geographic remoteness per se, may drive inequities in service access reported in other studies comparing rural/regional and metropolitan areas due to higher socio-economic disadvantage in these areas, particularly in small rural towns (MM5 areas) (Versace et al., 2021). Alternatively, our inability to detect differences in mental health service use among young people across geographic regions may reflect the true state of affairs in this age group. Further investigation using multiple avenues of exploration is required to tease this apart.
Lifetime experience of sexual assault was associated with consultation for mental health in the full and metro samples, consistent with previous studies suggesting that experience of sexual assault is associated with mental health symptoms and resulting mental health service use (Macauley et al., in press, Price et al., 2014). However, sexual assault was not associated with consultation for mental health in the regional/rural sample. The difference in findings across geographic regions could indicate barriers to young people in rural/regional areas accessing care, including a potential lack of local service availability or heightened stigma surrounding help-seeking for sexual assault in these areas (Jones et al., 2024), or the fact that residents of some remote and very remote areas were excluded from the survey through the sampling process. Considering that 44% of female and 14% of male young people who met criteria for a mental health condition in the current sample in the past year have experienced sexual assault in their lifetime, our mental health care system must be equipped to provide sensitive and effective care across the board, regardless of where a young person lives. Other researchers have called to advance the effectiveness of mental health care specifically by not only considering sexual assault broadly but also addressing intimate partner violence (Oram et al., 2022). This topic should be investigated further.
Strengths and limitations
This study is among the few to provide estimates of 12-month mental health service use among Australian young people by geographic region. It used a large, national cross-sectional sample and rigorous, high-quality mental health measures. Variable selection was informed by prior research, a social determinants of health framework and a lived experience lens (Macauley et al., in press). Acknowledging limited data availability in regional, rural and remote health research and responding to calls by young people to embrace intersectionality, we sought a creative solution in the form of purposeful variable selection to address low sample size in the regional, rural and remote sample to achieve our research aims.
Several limitations of the service use data from the NSMHWB have been detailed in Harris et al. (2025), including the timing of data collection during the COVID-19 pandemic and the absence of disorder-specific service use information. Grouping rural/regional areas meaningfully was also challenging – for example, larger centres like Wollongong and Darwin (MM2) were grouped with smaller, remote towns like Bourke and Brewarrina (MM7), despite vastly population profiles and service access. Low cell counts in the rural/regional subgroup, and a lack of data collected in remote/very remote areas due to sampling restrictions, may have reduced power to detect significant differences and limited our ability to explore variation across region types. We also lacked sufficient data to robustly conduct sub-analysis by health professions across different geographic areas and severity of symptoms, which would have been informative in terms of guiding further funding allocation. In addition, using mental health conditions or distress as proxies for service need may overlook individuals’ ‘perceived need’ for care, which future research using this data should consider. Our findings also do not speak to the quality of care received or fulfilment of need. Finally, low cell counts for gender identity prevented analysis of transgender or gender-diverse participants, even though these groups face well-documented barriers to care (Strauss et al., 2021).
Conclusion
While rates of mental health service use among young people aged 16–24 years in Australia have increased meaningfully since 2007, data from 2020 to 2022 reveal that major barriers to care remain. Our findings highlight inequity in access to care by neighbourhood disadvantage, sex at birth and disorder class, as well as distinct patterns of service use between metropolitan and non-metropolitan areas. To address these gaps, Australia’s mental health care system must provide more diverse, accessible and culturally responsible pathways to care – tailored to the needs, contexts and preferences of young people across the country.
Supplemental Material
sj-docx-1-anp-10.1177_00048674251389790 – Supplemental material for Health services and digital technologies used for mental health among a national cross-sectional sample of young people in Australia 2020–2022: Patterns and correlates within geographic regions
Supplemental material, sj-docx-1-anp-10.1177_00048674251389790 for Health services and digital technologies used for mental health among a national cross-sectional sample of young people in Australia 2020–2022: Patterns and correlates within geographic regions by Julia Macauley, Marlee Bower, Emma Webster, Meredith Harris, Maree Teesson and Cath Chapman in Australian & New Zealand Journal of Psychiatry
Footnotes
Acknowledgements
I am grateful to Uncle ‘Riverbank’ Frank Doolan, respected Wiradjuri Elder, for his guidance and support in the early framing of this paper. I would also like to thank Debora Rickwood from headspace for her involvement in the planning of the body of work making up my PhD. I would like to acknowledge those whose lived experience informed the framing of this paper. I would like to thank those who took part in the survey and to extend this thanks to the Dubbo community for sharing their stories with me.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship and/or publication of this article: This research is supported by an Australian Government Research Training Programme (RTP) Scholarship. This work was supported by a headspace National Youth Mental Health Foundation evidence-building PhD scholarship. Maree Teesson and Cath Chapman receive NHMRC Fellowship funding.
Ethical approval
Human ethical approval was not required, as this study is an analysis of secondary data and did not involve additional data collection.
Data availability statement
The detailed microdata used in this study can be obtained by seeking approval from the Australian Bureau of Statistics.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
