Abstract
Objective:
Cognitive-behavioural therapy is recommended as the first-line treatment for children and adolescents with anxiety. Despite its efficacy, a recent United Kingdom study indicated that few children with anxiety disorders receive cognitive-behavioural therapy. The primary aim of this study was to examine the receipt of cognitive-behavioural therapy for children and adolescents with elevated anxiety symptoms in Australia. Second, this study also examined whether there was a difference in the type of treatment received based on socioeconomic status and geographical location.
Method:
Using self-reported questionnaires, parents of children aged 4–18 years and children aged 12–18 years (N = 784; elevated anxiety symptom sample n = 169) were recruited from four samples: community (n = 164), school (n = 177), clinic (n = 16) and online panel provider (n = 427). Participants reported on the child’s anxiety symptoms and the type of treatment (if any) the child received for their anxiety symptoms.
Results:
Results indicated that 19.5% of children and adolescents with elevated anxiety symptoms received evidence-based treatment (e.g. cognitive-behavioural therapy). Of those families who did seek help for anxiety in Australia, the majority (66.3%) did not receive cognitive-behavioural therapy. In addition, neither socioeconomic status (which was based on the Australian Index of Community Socio-Educational Advantage [ICSEA]) nor location (metropolitan vs regional/remote) affected whether individuals received evidence-based care or non-evidence-based care.
Conclusion:
Overall, children and adolescents in this study seeking support for their anxiety symptoms were not receiving adequate evidence-based care, regardless of socioeconomic status and location. These findings indicate there is a need to increase the receipt of cognitive-behavioural therapy for children and adolescents with anxiety symptoms. The findings should tentatively be interpreted, given data were collected during the COVID-19 pandemic.
Anxiety disorders are among the most common mental health disorders in Australian children and adolescents, affecting nearly 7% of individuals aged 4–17 years (Lawrence et al., 2015). Despite the potential lifelong impacts on a child’s well-being (Creswell et al., 2020), low rates of access to treatment for children with anxiety symptoms have been reported (Reardon et al., 2020), and the evidence assessing the type of support these individuals are receiving is limited.
Cognitive-behavioural therapy (CBT) is the most frequently evaluated and effective treatment for children and adolescents with anxiety symptoms (In-Albon and Schneider, 2006; McKinnon et al., 2018). Broad-based CBT typically involves two key components: graded exposure to the anxiety-provoking situation(s) and cognitive restructuring strategies (Creswell et al., 2020). For adults with anxiety disorders, first-line treatments include pharmacotherapy or the combination of CBT and pharmacotherapy (Andrews et al., 2018). However, for children and adolescents in Australia, CBT is the only recommended first-line treatment by the Royal Australian and New Zealand College of Psychiatrists (RANZCP) treatment guidelines for anxiety disorders (Andrews et al., 2018). In the United Kingdom, the National Institute for Health and Care Excellence (NICE, 2013) guidelines for social anxiety recommend CBT as first-line treatment for young people, and pharmacological interventions are not recommended as routine care.
In Australia, there is some evidence (Danchin et al., 2019) that suggests access to mental health treatment varies by geographic location due to fewer mental health professionals in regional Australia. However, information about the type of interventions youth with anxiety symptoms receive in remote/regional areas of Australia compared to metropolitan areas is limited. Moreover, a review of headspace centres across Australia revealed that the most common type of mental health services provided to youth aged 12–15 years was CBT (Jorm, 2015). Yet, only 28% of clients with mental health problems received ‘minimally adequate treatment’ (i.e. receiving six or more 30 minutes or longer sessions; Harris et al., 2015). Therefore, additional research with a wider sample investigating the type of interventions provided to youth with anxiety is required.
The main aim of this study was to describe the frequency and type of treatment received by children and adolescents with anxiety symptoms in Australia. This study is based on Reardon et al.’s (2020) study which was one of the first to examine the types of professional support children aged 7–11 years with anxiety disorders received in the United Kingdom. Based on parent and child interviews and questionnaires, 2.3% of children with elevated anxiety symptoms received evidence-based treatment (CBT), therefore highlighting that families seeking help for their child’s anxiety in the United Kingdom rarely receive evidence-based treatment (Reardon et al., 2020).
This study examined the receipt of evidence-based care, as per the RANZCP guidelines, within Australia for children and adolescents with anxiety symptoms. We also aimed to provide current data on the frequency and type of professional support children and adolescents receive to help manage and overcome their anxiety and whether there is a difference in the type of treatment (evidence-based vs non-evidence-based) received as based on socioeconomic status (SES) and geographical location/area.
Method
Participants
The initial sample included reports on 980 children from Australia; however, after removing participants who failed one of three attention checks dispersed throughout the survey, the final sample included reports on 784 children aged 4–18 years. Of these 784 reports, 509 were parent-/caregiver-only reports, 212 were child-only reports and 63 reports were provided by both the parent/caregiver and child (i.e. the total parent-report sample is 572 and the total child-report sample is 275). For demographic information reported by both the parent/caregiver (hereafter referred to as parents) and the child, parent report was given preference. To increase the sample diversity and size, participants were recruited from four samples: community (n = 177), school (n = 164), clinic (n = 16) and an online independent Australian and New Zealand-based paid panel provider (Cint; n = 427). Participant characteristics are described in Table 1 (see Supplemental Appendix A for participant characteristics for the four samples). Participants were allocated to the elevated anxiety symptom group if they had a Revised Child Anxiety and Depression Scale (RCADS-C/P-25) anxiety T-score greater than 65 (based on the parent and/or child report) and across the total sample, 169 (17.3%) children met the criteria for elevated anxiety symptoms.
Participant characteristics.
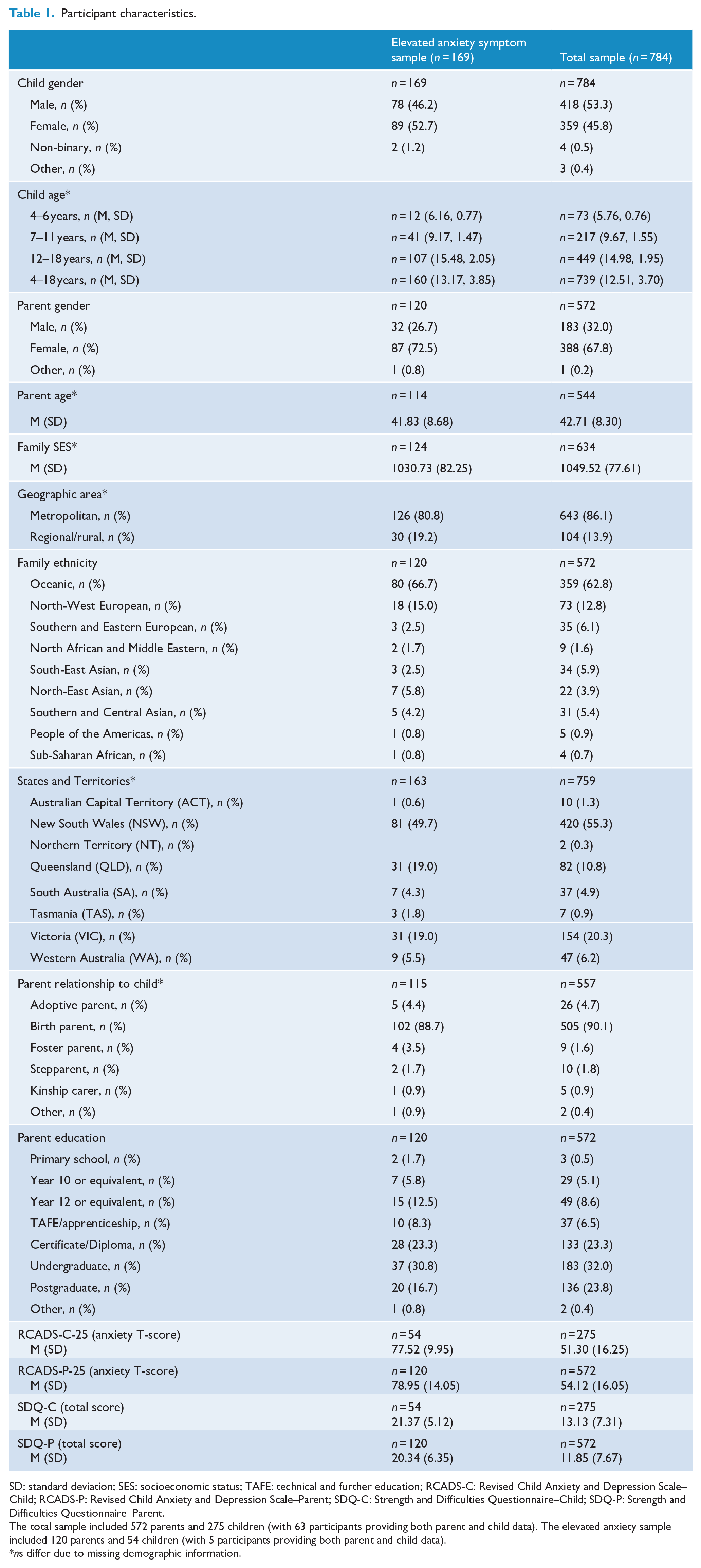
SD: standard deviation; SES: socioeconomic status; TAFE: technical and further education; RCADS-C: Revised Child Anxiety and Depression Scale–Child; RCADS-P: Revised Child Anxiety and Depression Scale–Parent; SDQ-C: Strength and Difficulties Questionnaire–Child; SDQ-P: Strength and Difficulties Questionnaire–Parent.
The total sample included 572 parents and 275 children (with 63 participants providing both parent and child data). The elevated anxiety sample included 120 parents and 54 children (with 5 participants providing both parent and child data).
ns differ due to missing demographic information.
Measures
The measures in this study were part of a wider survey which included additional measures assessing depressive and anxiety symptoms in children and adolescents. Due to the coronavirus pandemic (COVID-19), an additional measure was included to assess isolation status. This measure asked parents to report on their family’s current living situation.
Revised Child Anxiety and Depression Scale, Child and Parent short versions
Child and adolescent elevated anxiety symptoms were measured using the Revised Child Anxiety and Depression Scale–Child (RCADS-C-25) and Revised Child Anxiety and Depression Scale–Parent (RCADS-P-25; Ebesutani et al., 2012, 2017). The RCADS-C/P-25 contains 15 items assessing broad anxiety and 10 items assessing major depressive disorder and have demonstrated sufficient internal consistency in community and clinical samples with alphas ranging from 0.70 to 0.82 (Ebesutani et al., 2017; Klaufus et al., 2020). The broad anxiety scale has proven to be structurally valid and internally consistent (α = 0.82) with test–retest reliability and criterion validity also reaching acceptable levels regarding the ability to screen children with anxiety symptoms per the Diagnostic and Statistical Manual of Mental Disorders (4th ed.; DSM-IV) criteria (Klaufus et al., 2020).
Items in the RCADS-C/P-25 were scored on a 4-point Likert-type scale ranging from 0 to 3, and anxiety T-scores (which are raw scores adjusted to US age and gendered normative data) greater than 65 were categorised at the borderline clinical threshold and anxiety T-scores greater than 70 are above the clinical threshold. For this study, children scoring above 65 on either parent or child report were considered as experiencing ‘elevated’ anxiety symptoms. Based on the RCADS-C/P-25 total anxiety scale, excellent internal consistency (α = 0.91 and 0.89, respectively) was achieved in the current sample.
Strength and Difficulties Questionnaire, Child and Parent short versions
The overall mental health of the total sample was measured using the Strength and Difficulties Questionnaire–Child and Parent short versions (SDQ-C/P; Goodman, 1997). The SDQ is an emotional and behavioural screening questionnaire (Goodman et al., 2010). Items are scored on a 3-point Likert-type scale ranging from 0 to 2 and total SDQ scores range from 0 to 40 with higher scores indicating greater mental health symptoms (based on Australian age and gendered normative data; Mellor, 2005).
This measure has demonstrated acceptable internal consistency with an alpha above 0.70, moderate test–retest reliability and sufficient construct validity in both community and clinical samples (Kremer et al., 2015; Mellor, 2005). Based on the SDQ-C/P total scores, good internal consistency (α = 0.83 and 0.81, respectively) was achieved in the current sample.
Access to Evidence-Based Care Questionnaire–Child and Parent versions
Two questionnaires, one administered to children and adolescents (see Supplemental Appendix B1) and one administered to parents (see Supplemental Appendix B2), were developed for this study to assess the type of support children and adolescents received for their anxiety symptoms. The questions were based on the ‘N-CAT: National Survey of Child Anxiety and Treatment Access − Help-Seeking Views and Experiences Questionnaire’ used by Reardon et al. (2020).
Evidence-Based Care Questionnaire–Child version (aged 12–18 years)
Participants were asked to report (1) who they received support from for their anxiety/fears/worries, as well as who provided the most help, (2) the type of support they received and (3) whether they had received graded exposure therapy.
Evidence-Based Care Questionnaire–Parent version (parents with children aged 4–18 years)
Using the above modified items 1 to 3, parents were also asked about their child’s use of medication.
Procedure
The Institutional Human Research Ethics Committee approved this study and informed consent and assent were obtained from parents and children, respectively. Participants completed the survey online via LimeSurvey and only parents with children aged 4–18 years and children aged 12–18 years residing in Australia were included. Parents were required to provide data on one child only. Participants from the community, school and clinic samples had the opportunity to enter a draw to win an iPad, whereas the panel sample was provided monetary reimbursement in accordance with Cint.
Community sample
Participants were recruited via two public social media advertisements.
School sample
Participants were recruited from an independent combined primary and high school in New South Wales, Australia. The school distributed study information to 275 parents of students in the participating year groups (primary school year groups 3–6, aged 8–12 years; high school year groups 7–10, aged 13–18 years). Parents not wanting their child to participate provided opt-out consent. Students in year groups 7–10 then completed the survey during school time. Parents choosing to also participate completed the survey at a time convenient to themselves. The response rate for student participation was 60%.
Clinic sample
Families attending the Centre of Emotional Health Clinic at Macquarie University, a specialist university clinic, between July 2020 and August 2020 for an initial diagnostic interview were invited to participate. Participating parents and children then completed their respective surveys while waiting for their interview.
Panel sample
Parents were recruited via Cint, an online paid panel provider (cint.com). Participating parents who had children aged 7–18 years were given the opportunity for their child to also participate. Participants then completed the survey using the appropriate links.
Statistical analysis
Descriptive statistics
The data were analysed using Stata/IC 16.1. The type of professional and support children and adolescents received to help with their anxiety was examined across the total parent-reported sample (n = 572), total child-reported sample (n = 275) and total sample for just 7- to 11-year-olds (n = 217), and within the parent-reported elevated anxiety symptom sample (n = 120), child-reported elevated anxiety symptom sample (n = 54) and elevated anxiety symptom sample for just 7- to 11-year-olds (n = 41).
Access to treatment
Family postcodes and school location were used to determine geographic location/area (based on the Australian Statistical Geography Standard Remoteness Area data [ASGS-RA]; Australian Government Department of Health, 2019a), and school name was used to determine SES (based on the Australian Index of Community Socio-Educational Advantage [ICSEA]; national mean = 1000, standard deviation [SD] = 100; Australian Curriculum, Assessment and Reporting Authority, n.d.). A chi-square test was used to examine whether there was a relationship between treatment received (evidence-based vs not evidence-based) and area (metropolitan vs regional/remote), and an independent t-test was used to examine whether there was a relationship between treatment received (evidence-based vs not evidence-based) and SES for the elevated anxiety symptom sample and total sample. A significance level of α = 0.05 was used for all statistical tests.
Results
Descriptive analyses
Based on parent reports, the mean SDQ-P total score was 11.85 (SD = 7.67) and based on child reports, the mean SDQ-C total score was 13.13 (SD = 7.31), which suggests that the overall mental health symptoms of the current sample were slightly elevated. The study mean fell within 1 SD of the normative mean for parent reports (normative mean = 8.18, SD = 6.06) and child reports (normative mean = 8.96, SD = 5.62) (based on Australian normative data; Mellor, 2005).
Missing data
RCADS-C/P-25 total scores and SDQ-C/P total scores, respectively, were prorated for participants who had completed at least 80% of the measure items, and participants who had completed less than 80% of the respected measures were excluded from all analyses (n = 2 due to < 80% completion on the RCADS-C/P-25). As no normative data are available for participants who do not identify as either male or female, a decision was made to calculate anxiety T-scores for children who indicated ‘non-binary’ or ‘other’ gender (n = 4; n = 3, respectively) under RCADS-C/P-25 male gender norms as these norms resulted in a slightly increased likelihood, compared to female norms, of allocation to the elevated anxiety symptom group rather than exclude them from further analyses. (Note: Two of the non-binary/other gender participants were classified as reporting elevated anxiety symptoms. The decision to use male norms did not result in any of the non-binary/other gender participants being classified differently.)
Listwise deletion was used for analyses involving missing demographic information.
COVID-19 isolation status
Approximately one-fifth (19.1%) of parents reported that they were self-isolating and just under half (45.5%) of parents reported that while they were not strictly self-isolating they had reduced their usual activities due to COVID-19.
Access to evidence-based treatment
Parent-reported and child-reported help-seeking for a child’s anxiety difficulties within the elevated anxiety symptom sample and across the total parent-reported and child-reported samples are presented in Table 2. Based on parent reports, counselling was reported as the most common type of help received (based on any professional who provided help). Furthermore, psychologists were reported as the professional who provided the most help to individuals seeking help for their anxiety symptoms across parent-reported and child-reported samples.
Frequency and type of support.
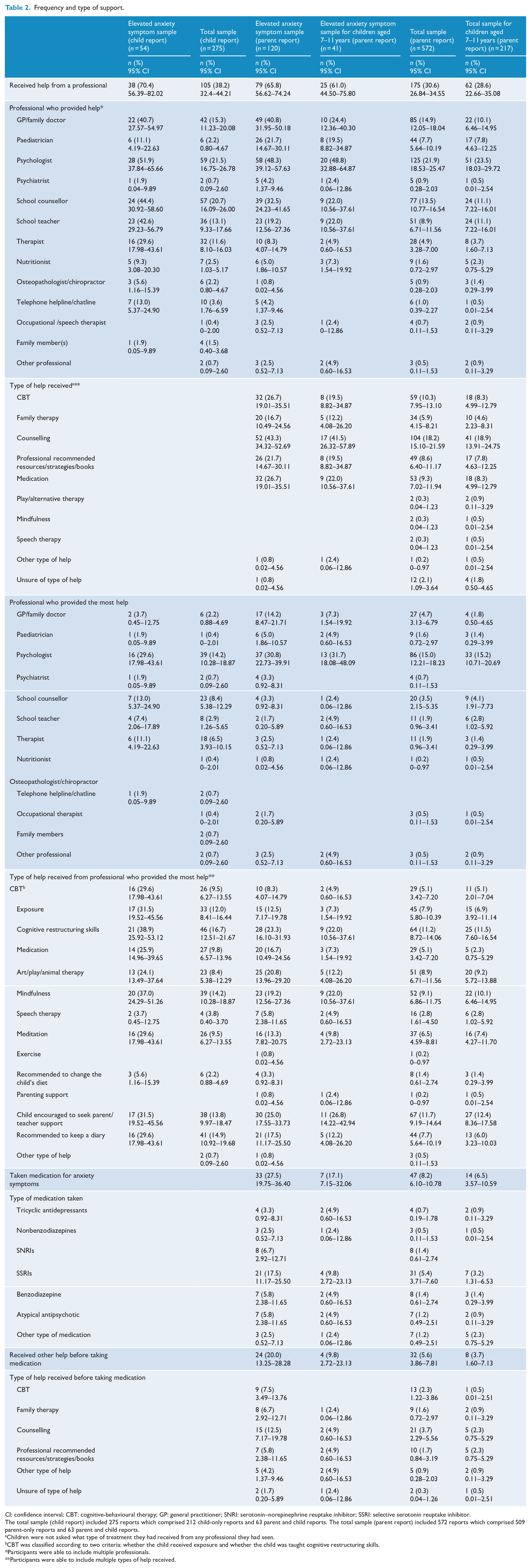
CI: confidence interval; CBT: cognitive-behavioural therapy; GP: general practitioner; SNRI: serotonin–norepinephrine reuptake inhibitor; SSRI: selective serotonin reuptake inhibitor.
The total sample (child report) included 275 reports which comprised 212 child-only reports and 63 parent and child reports. The total sample (parent report) included 572 reports which comprised 509 parent-only reports and 63 parent and child reports.
Children were not asked what type of treatment they had received from any professional they had seen.
CBT was classified according to two criteria: whether the child received exposure and whether the child was taught cognitive restructuring skills.
Participants were able to include multiple professionals.
Participants were able to include multiple types of help received.
Across the total sample, 10.3% (n = 59; 95% CI = [7.95, 13.10]) of parents reported that their child had received CBT, and across the elevated anxiety symptom sample, 26.7% (n = 32; 95% CI = [19.01, 35.51]) of parents reported that their child had received CBT (based on any professional who provided help). To allow comparison with Reardon et al. (2020), an additional estimate of receipt of CBT was determined for a subset of children aged 7–11 years. Across the total sample of children aged 7–11 years, 8.3% (n = 18; 95% CI = [4.99, 12.79]) of parents reported that their child had received CBT, and across the elevated anxiety symptom sample of children aged 7–11 years, 19.5% (n = 8; 95% CI = [8.82, 34.87]) of parents reported that their child had received CBT (based on any professional who provided help). Examining the subset of young people who had sought help for their anxiety (n = 175), 59 received CBT (33.7%). This means two-thirds (66.3%) of young people who sought help for their anxiety received treatment that was not evidence based.
Evidence-based treatment received across metropolitan vs regional/remote areas
Using the type of help received from the professional who provided the most help, a Fisher’s exact one-tailed test was used to examine the relationship between children and adolescents who received evidence-/non-evidence-based treatment and area (metropolitan vs regional/remote). The proportion of children and adolescents with elevated anxiety symptoms who received evidence-based and non-evidence-based treatment did not significantly differ by metropolitan and regional/remote areas, p = 0.49. It should be noted 13 participants were not included due to missing area data.
In addition, using a chi-square test of independence, the proportion of children and adolescents across the total sample who received evidence-based and non-evidence-based treatment did not significantly differ by metropolitan and regional/remote areas, χ2 (1, N = 747) = 0.01, p = 0.92. It should be noted that 37 participants were not included due to missing area data.
Evidence-based treatment and SES
An independent t-test was used to examine the relationship between SES and those who received evidence- and non-evidence-based treatment (according to the type of help received from the professional who provided the most help). Based on the elevated anxiety symptom sample, SES was not significantly different for children and adolescents with elevated anxiety symptoms who received evidence-based treatment (M = 1049.85, SD = 72.49) compared to participants who received non-evidence-based treatments (M = 1027.06, SD = 83.81), t(122) = 1.14, p = 0.26 (see Table 3). To account for missing SES scores from 6 participants who received evidence-based treatment and 39 who received non-evidence-based treatment, participants were given a mean SES score of 1000 (based on ICSEA mean score), and due to the violation of normality, the Mann–Whitney’s test was used. This did not change the interpretation of the result, U(Nevidence-based treatment = 26, Nnon-evidence-based treatment = 143) = 51,589.08, z = −1.59, p = 0.11, (evidence-based treatment, Mdn = 1021; non-evidence-based treatment, Mdn = 1000).
Receiving evidence-based treatment according to socioeconomic factors.
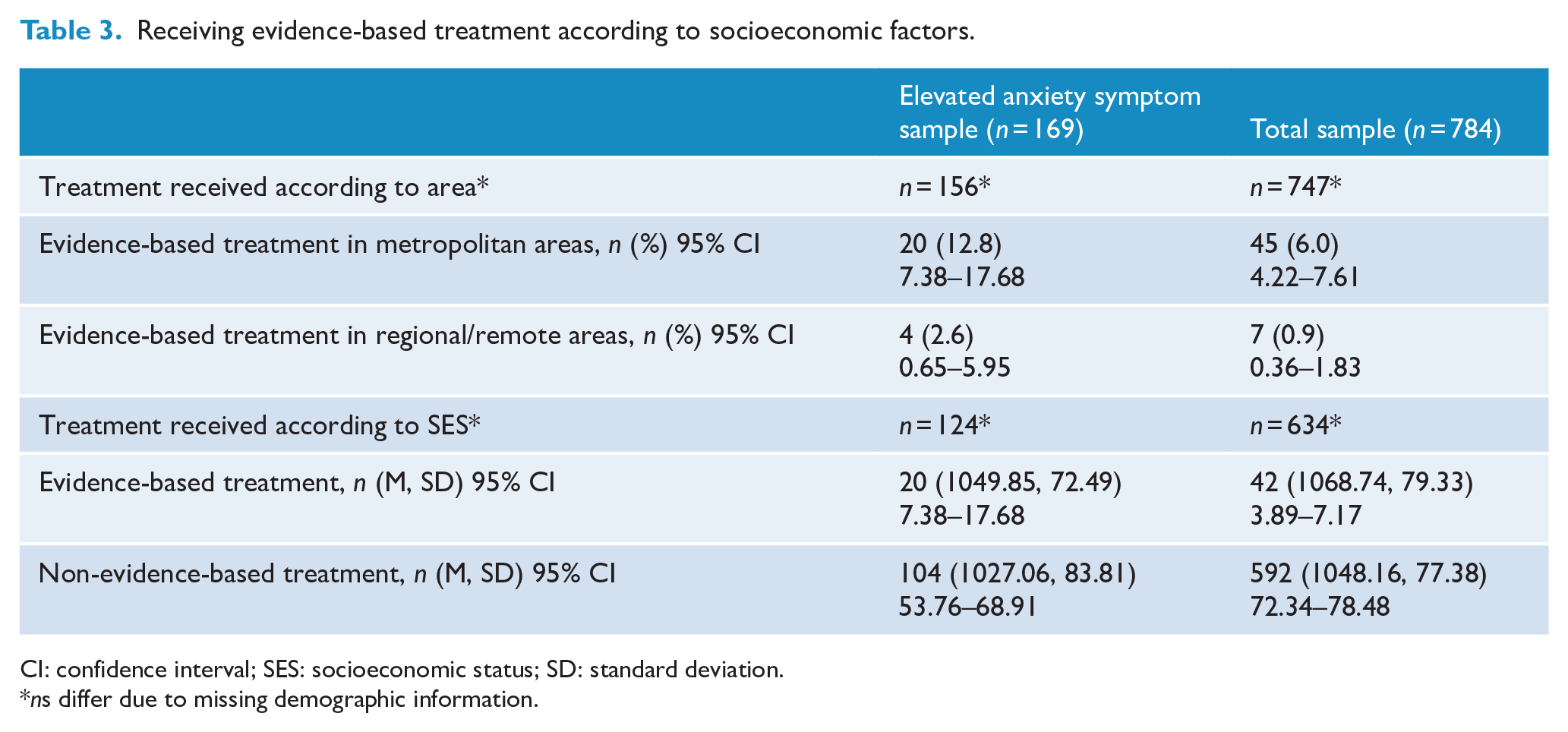
CI: confidence interval; SES: socioeconomic status; SD: standard deviation.
ns differ due to missing demographic information.
Across the total sample, SES was not significantly different for participants who received evidence-based treatment (Mdn = 1021) compared to participants who received non-evidence-based treatment (Mdn = 1026), U(Nevidence-based treatment = 42, Nnon-evidence-based treatments = 592) = 1,303,091.29, z = −0.97, p = 0.33 (see Table 3). To account for missing SES scores from 12 participants who received evidence-based treatment and 138 who received non-evidence-based treatment, participants were given a mean SES score of 1000 (based on the ICSEA mean score), and this did not change the interpretation of the result, U(Nevidence-based treatment = 54, Nnon-evidence-based treatment = 730) = 2,547,212.22, z = −0.87, p = 0.39, (evidence-based treatment, Mdn = 1021; non-evidence-based treatment, Mdn = 1021).
Discussion
CBT is the only recommended first-line treatment for children and adolescents with anxiety disorders in Australia (Andrews et al., 2018); however, the receipt of evidence-based care for these individuals is limited, and hence was the primary aim of this study. The findings illustrate that the youth with elevated anxiety symptoms are not currently receiving adequate evidence-based care. Consequently, there is a need to increase the usage of CBT for youth with anxiety symptoms in Australia.
Comparing our findings to that of Reardon et al. (2020), a higher percentage of children aged 7–11 years with elevated anxiety symptoms received CBT in Australia than the United Kingdom (19.5% vs 2.3%, respectively). When examining the entire sample of children and adolescents with elevated anxiety symptoms, 26.7% received CBT. In addition, and in contrast to previous Australian findings (Lawrence et al., 2015), parents and children most frequently reported receiving help from a psychologist and were also more likely to select a psychologist as the professional who provided the most help regarding reducing the child’s anxiety symptoms. This difference between our findings and Reardon et al. (2020) could be due to the difference in the type of professional administering the help. Young people in the United Kingdom most reported receiving help for their anxiety symptoms from school personnel (National Health Service [NHS], 2018; Reardon et al., 2020); however, the effectiveness of CBT administered in school settings tend to be variable and inconsistent (O’Callaghan and Cunningham, 2015; Starrenburg et al., 2017). Widespread training of CBT may be required across professional fields, particularly for school mental health professionals. Furthermore, it is important to note the methodological differences between our study and Reardon et al. (2020), specifically that data on 7- to 11-year-olds in our study were based on self-report by parents only, whereas Reardon et al. (2020) recruited via screening in schools.
Evidence-based treatment is lacking in Australia as the majority of children and adolescents (66.3%) who received treatment for their anxiety did not receive CBT (based on the type of help received from any professional). Furthermore, and consistent with previous findings (Whiteside et al., 2016), the receipt of exposure and cognitive restructuring strategies was low across both the parent- and child-reported samples. Exposure to the anxiety-provoking situation is a central component of CBT (Creswell et al., 2020), yet research shows that therapists and clinicians own negative beliefs towards exposure reduced utilisation (Ginsburg et al., 2019; Whiteside et al., 2016). Consequently, when considering how to increase the usage of evidence-based treatment, it may be valuable to address these misconceptions surrounding exposure.
In line with previous research (Danchin et al., 2019), selective serotonin reuptake inhibitors (SSRIs) were reported by parents of children with elevated anxiety symptoms and across the total sample as being the most common type of medication taken. Furthermore, based on parent reports, 7.5% of participants in the elevated anxiety symptom sample and 2.3% across the total sample reported utilising CBT before medication. Therefore, suggesting a need to address the efficacy of how CBT as a first-line treatment is being administered by practitioners.
In contrast to previous literature (Danchin et al., 2019), our findings tentatively illustrate that area (metropolitan vs regional/remote) and SES play a limited role in whether a child receives evidence-based care. Children with elevated anxiety from lower SES areas and regional/remote areas were just as likely to receive CBT as those from higher SES areas and those in metropolitan areas. One possible interpretation for our findings could be due to the changes in the Better Access Telehealth initiative which have allowed patients living in rural Australia to claim Medicare rebates for video conferences for mental health care (Australian Government Department of Health, 2019b). Nevertheless, services in rural Australia often still have poorer Internet access and connectivity than urban areas (Park, 2017). In addition, the included regional/remote area sample may not have been representative of the wider regional and rural population that receive treatment. Furthermore, given that the SES of families tends to vary within each school, categorising SES according to ICSEA may have restricted this variation, and as such, the findings should be tentatively interpreted.
Limitations and future directions
This study relied on retrospective reports rather than clinical records and, depending on knowledge (and memory), the findings may be underestimated. Furthermore, parent reports alone were used to collect information for children aged 4–11 years. As a result, future research utilising both larger parent-report and child-report samples, as well as larger samples from each group (e.g. community, school and clinic), could enable exploration and comparisons between parent reports and child reports regarding the receipt of mental health care young people receive. We also identified youth with current elevated symptoms and therefore may not have captured children who have recovered from anxiety. Furthermore, as the sample was predominantly non-clinical, with an underrepresentation of participants from non-Oceanic and lower socioeconomic backgrounds, the findings may not sufficiently reflect the type of support children with clinical anxiety disorders received and the generalisability of findings may be limited with regard to these groups. Also, although the study provided data representing families from all states and territories across Australia, the greatest representation was from New South Wales and Victoria and given the recruitment strategies used in this sample, they were not nationally representative. Consequently, and given that few studies have examined the type of treatment children with anxiety symptoms receive, with even fewer studies comparing mental health care usage across countries, it is important to establish a way to examine the receipt of mental health care across countries. Hence, future research could adapt the questionnaire utilised in this study to help explore the receipt of evidence-based care for youth mental health across different samples and populations.
Due to COVID-19, anxiety and depression symptoms in children and adolescents may have increased (Fegert et al., 2020) and this could have increased the percentage of children who were classified as having elevated anxiety symptoms and those who reported having received help. These findings need to be replicated during a period that is not reflective of a national (and international) crisis.
Conclusion
This study was one of the first to examine the receipt of evidence-based care for youth with anxiety symptoms in Australia and illustrates that most youth with anxiety symptoms do not receive evidence-based treatment. This study also tentatively suggested that receiving evidence-based care may not be influenced by SES or geographic location; however, future studies utilising larger and more representative samples are required. Overall, there is a need to increase access to CBT including increasing widespread training, support and supervision to all professionals who may provide services to children with anxiety symptoms. This means improving CBT training for psychologists, social workers, school counsellors and teachers, general practitioners, psychiatrists and paediatricians as these are professionals from whom young Australians with anxiety seek help.
Supplemental Material
sj-docx-1-anp-10.1177_00048674211068780 – Supplemental material for Receipt of evidence-based care for children and adolescents with anxiety in Australia
Supplemental material, sj-docx-1-anp-10.1177_00048674211068780 for Receipt of evidence-based care for children and adolescents with anxiety in Australia by Esther Gandhi, Maddison OGradey-Lee, Alana Jones and Jennifer L Hudson in Australian & New Zealand Journal of Psychiatry
Footnotes
Author Note
Alana Jones is now affiliated to Macquarie University Centre for Reading, Macquarie University, Sydney, NSW, Australia.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
