Abstract
Introduction:
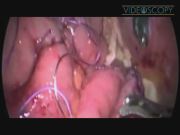
This video shows laparoscopic management of small bowel obstruction following Roux en Y gastric bypass for obesity. Small bowel obstruction has been reported following gastric bypass for several reasons, including internal herniation, anastomotic technical obstruction, incorrect reconstruction of the Roux limb, bowel rotation, and adhesions. 1,2 Early small bowel obstruction following Roux en Y gastric bypass is mechanical in the vast majority and needs an urgent intervention by open or laparoscopic techniques. Mortality following gastric bypass is depending on the type of operation and length of the limb. 3
Methods:
This was a 58-year-old patient who underwent Roux en Y gastric bypass (It was proximal type/the gastric bypass was performed using 70 cm of the bilio-pancreatic limb and 120 cm of the Roux limb.) for obesity two weeks before this operation and was presented with small bowel obstruction, which was confirmed on preoperative gastrograffin study and a CT scan, which is the best imaging modality in this clinical scenario. 4 The symptoms of nausea and vomiting started after the first week and the patient was presented at the end of the second week. An urgent laparoscopic exploration was undertaken and the finding was suggestive of mechanical obstruction at the jejuno-jejunostomy. It was high-grade partial obstruction of the bilio-pancreatic limb, which was draining through the efferent loop (alimentary loop) and the stomach was not hugely distended. However, the main problem was complete obstruction of the Roux limb. This was clearly demonstrated in the gastrograffin study (a photo was included in the beginning of the video). The options were either to revise the anastomosis or to perform two different jejuno-jejunostomies to bypass the obstruction; one between the bilio-pancreatic and the efferent limbs and the other between the afferent Roux limb and the alimentary loop. Obviously, endoscopic dilatation is not an option and it is contraindicated because this was an early anastomosis and leak, perforation and disruption of the anastomosis is expected. The decision was taken for the second option and the new anastomoses were fashioned using 40-mm Gastro Intestinal Anastomosis stapler and the openings were closed with vicryl in two layers. We think a 40-mm stapler is sufficient for the jejuno-jejunostomy. Using 60 mm is also a viable option and we have been using it for the initial 7 years, then we changed to 40 mm after we had intussussception at the jejuno-jejunostomy. A diagram has been included at the end of the video showing the pre- and postoperative anatomy. Making a new Roux en Y anastomosis would mean a major revision of the junction. This is a more risky option; it involves a long procedure time, doing the new anastomosis at area of bowel, which is edematous, inflamed, and not easy to handle with a known increased risk of leak. Our successful option of doing the two junctions at fresh and healthy segments of the small bowel was a more sensible decision. The risks of internal herniation or rotation are not expected after the two anastomoses we did, but rarely reported for the Roux en Y type of construction.
Results:
The patient had unremarkable recovery and was discharged home on the 5th postoperative day and was seen 2, 4, and 12 weeks after this operation with a satisfactory weight loss and no symptoms to report.
Conclusion:
Early acute abdomen following gastric bypass should be appropriately assessed and an urgent intervention is needed to save the patient's life and to reduce the morbidity. Early small bowel obstruction following Roux en Y gastric bypass can be successfully managed using the minimal access approach. This was safe, enhanced the recovery, and provided patient satisfaction.
There is no conflict of interest of any kind in relation to this article for either Abdulzahra Hussain or Shamsi EL-Hasani.
Runtime of video: 5 mins


Get full access to this article
View all access options for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
