Abstract
Introduction:
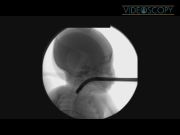
Congenital tracheoesophageal fistula without esophageal atresia (H-type TEF) is an unusual entity that typically presents in the first months of life with clinical signs of aspiration. Surgical repair is usually facilitated by placement of a catheter or wire through the fistula during rigid bronchoscopy. 1,2 This cannulation allows the surgeon to identify the fistula during dissection of the neck. 3 We describe a case of H-type TEF in which, the fistula could not be identified on rigid bronchoscopy, but was only visible on esophagoscopy. Cannulation of the fistula was therefore achieved using video esophagoscopy. The video depicts the placement of the guidewire under a video esophagoscope using an ultraslim (pediatric) side-viewing duodenoscope. Fluoroscopic images confirming fistula cannulation are also shown. The video runtime is 1:44.
Materials and Methods:
The patient is a male born prematurely at 34 weeks, birth weight 2.0 kg. Respiratory distress was noted on the first day of life and a contrast study revealed the H-type TEF. Rigid bronchoscopy failed to identify the fistula. The fistula was noted on rigid esophagoscopy, but could not be cannulated given the acute angle of the fistulous opening on the esophageal side. A repeat procedure was undertaken with video esophagoscopy. The forward-view endoscope, Olympus N180 (Olympus Medical), was used for initial examination and determination of the fistula position within the esophagus. Once the exact measurement was obtained, an Olympus PGF160 (Olympus Medical) was introduced transorally and advanced to the predetermined depth within the esophagus. The H-type fistula opening was identified and cannulated using a slim (5F) tapered ERCP cannula (Mini-Tome; Wilson-Cook). A 0.018-inch soft GI guidewire (Pathfinder wire) (Boston Scientific) was then placed through the ERCP cannula. The wire placement was done under video and fluoroscopic control. The tip of the guidewire crumpled on the bronchial side of the fistula and was felt to be too flexible and soft, so it was exchanged for a 0.021-inch guidewire (Wilson-Cook). The surgical repair was then performed with the guidewire in place.
Results and Conclusions:
Primary repair of an H-type TEF is usually aided by placing a cannula or guidewire through the fistula under bronchoscopy. In this case, failure to place a wire was due to high takeoff of the fistula within the hypopharynx and difficulty visualizing the opening from the tracheal side. Transesophageal evaluation and guidewire placement using a side-viewing duodenoscope was undertaken and was successful. Placement was relatively smooth and atraumatic when compared with rigid bronchoscopy. This index case validates the use of this technique. Expanded experience with this technique would be needed to clarify questions regarding safety and reproducibility. In complex cases with difficult fistula cannulation during bronchoscopy, this technique offers another option for TEF guidewire placement before repair.
No competing financial interests exist
.
Runtime of video: 1 min and 44 secs


Get full access to this article
View all access options for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
