Abstract
Introduction and Objectives:
Pelvic lipomatosis (PL) is a rare condition characterized by diffuse pelvic overgrowth of nonmalignant but infiltrative adipose tissue in perivesical and perirectal space. 1 The incidence rate is 0.6–1.7/100,000 hospital admissions. 2 So far, only <150 cases have been reported worldwide, including only two single-center series (with 35 and 8 cases) as per the available literature. 2,3 This is the first series of six cases of PL effectively managed by robot-assisted surgery. The objective of our study is to enlighten the difficulties encountered and demonstrate the tips and tricks of techniques to effective robotic management.
Materials and Methods:
We encountered six cases of PL between 2016 and 2020 diagnosed with contrast enhanced computed tomography (CECT) kidney ureter bladder (KUB)/magnetic resonance imaging (MRI) KUB. Uroflowmetry was performed in all patients. Ethical committee clearance was obtained. Initial cystoscopy was performed in all patients and biopsy wherever necessary. All patients underwent robot-assisted wide bladder fat extirpation (at the site of reimplantation) and bilateral (B/L) ureteral reimplantation/ureteroneocystostomy (Modified Lich Gregoir extravesical refluxing type) with Double-J stenting.
Results:
The median console time was 126 (range 120–130) minutes, with a median estimated blood loss of 130 (range 100–150) mL. Postoperative complications were Clavien–Dindo grade I in three cases, and the average hospital stay was 2.7 days. At initial 3-month and annual follow-ups, all patients had normal serum creatinine and there was no evidence of disease recurrence. The challenges encountered were lack of surgical planes and difficulty in identifying the anatomic structures as the entire pelvis was filled with fat; large bladder occupying the entire pelvis, needing readjustment of ports and redocking; presence of tough, thick, adherent, and hypervascular fat planes that bleed easily on manipulation; difficulty in separating the ureter from adherent tough fat and bladder mucosa buried underneath the thick fat planes, making anastomosis difficult.
Conclusion:
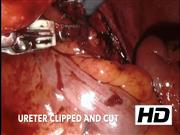
Techniques recommended for effective robotic management include identification of ureter at the level of iliac vessels, complete extirpation of bladder fat at the site of intended anastomosis, mucosal eversion stitches when the bladder mucosa is deeply buried underneath the thick fat planes, lateral/medial retraction of bladder fat screens for adequate exposure for anastomosis, minimal handling of the ureter and wide lumen for anastomosis, if the anastomosis is in tension the bladder can be dropped from anterior abdominal wall.
No competing financial interests exist.
Runtime of video: 8 mins 0 secs

Get full access to this article
View all access options for this article.
