Abstract
Introduction:
Radiofrequency ablation (RFA) is a nonsurgical treatment for benign thyroid nodules, traditionally performed through a transisthmus approach to avoid injury to the recurrent laryngeal nerve (RLN). We present a case with unique technical considerations to thyroid RFA. The patient is a 77-year-old man with history of right supraglottic laryngeal squamous cell carcinoma status postradiation therapy and total laryngectomy 20 years ago, followed by cervical spinal osteomyelitis requiring anterior cervical discectomy and fusion, who presented with enlarging left thyroid nodules causing stomal deviation and difficulty inserting his lary tube. He phonates through tracheoesophageal voice prosthesis, complicated by perifistular granulation tissue thought secondary to thyroid compression. Serial ultrasound and CT imaging demonstrated multiple enlarging left-sided mixed solid and cystic nodules, the largest 5.7 × 3.4 × 4.9 cm, extending into the superior mediastinum with mass effect on the left internal jugular vein and deviation and narrowing of the trachea and pharynx. Initial FNA biopsy (2018) demonstrated a small focus of atypical cells, but follow-up core biopsy (2018) and repeat FNA (2022) confirmed benign thyroid tissue.
Materials and Methods:
The patient underwent RFA of his left thyroid nodules. The standard transisthmic approach was made challenging because of stoma location. In addition, the patient required intraprocedural manual access to the stoma to phonate and cough. To address these challenges, the stoma was prepped in the field with betadine, and the patient's right hand sterilely gloved. The superior cystic portion of the nodule was aspirated, and the ablation was performed using a STARmed© ablation probe with 7 mm active tip. An oblique superior-lateral to inferior-medial approach was employed, using the moving shot technique, slightly overlapping ablation zones. Multiple fanning passes were performed posteriorly to anteriorly, moving cephalad to caudad for complete ablation of the nodule, taking care to avoid the posterior capsule and the tracheal border. The small-footprint linear array transducer improved observation medially and inferiorly, near the stoma.
Results:
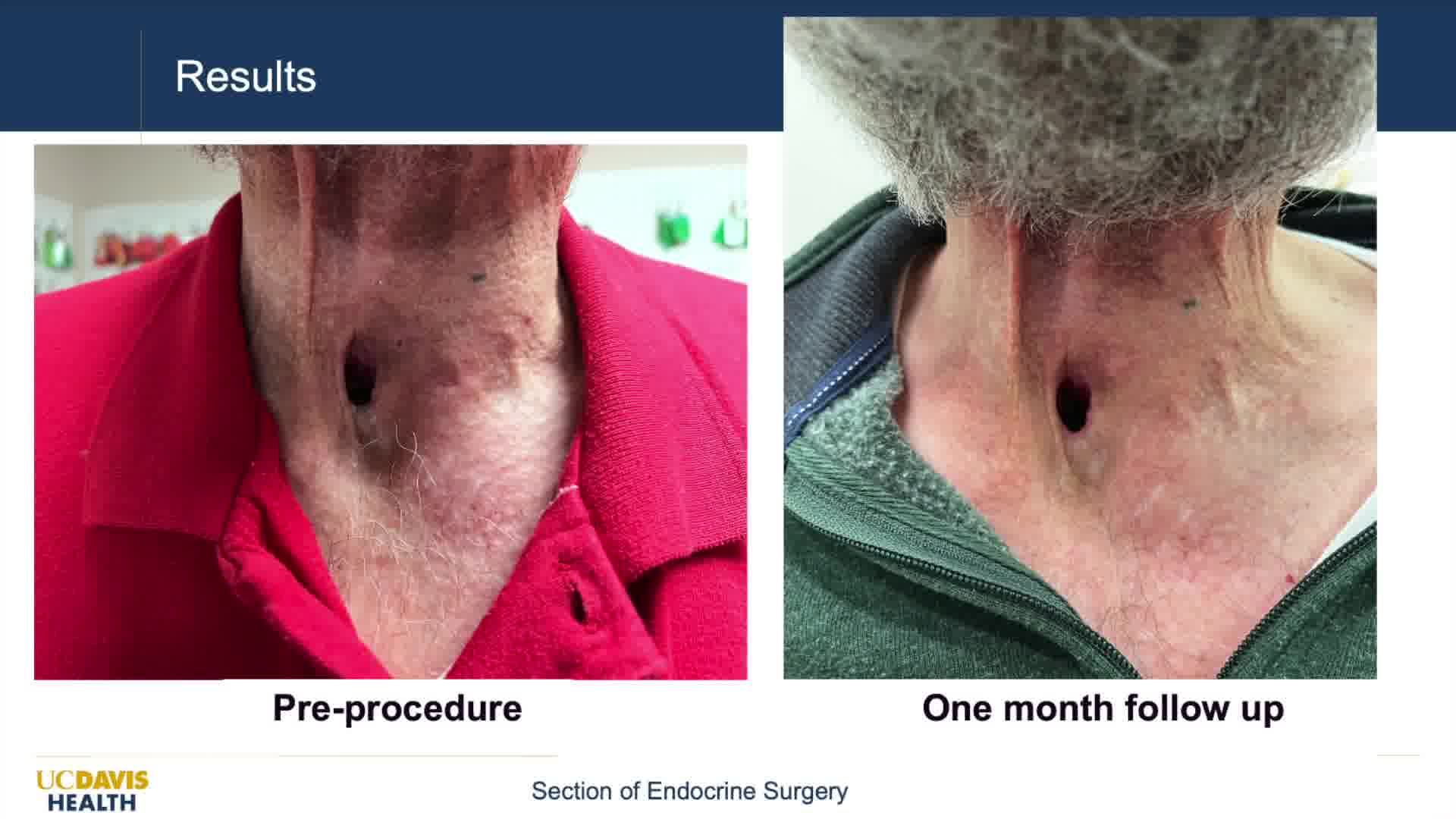
The patient reported mild swelling a few nights postprocedure, which fully resolved. He had no bruising, pain, or voice changes, was eating and drinking normally, without changes in swallowing. At 1-month follow-up, he stated the nodule felt and looked smaller. He had more ease placing his lary tube and less irritation wearing it. On ultrasonography, volume reduction of the nodule was 29%. His thyroid stimulating hormone was normal.
Discussion:
There are unique technical considerations to performing RFA in a patient after total laryngectomy. In patients with prior radiation, observation may be more difficult because of poor neck extension and lack of clear tissue planes. This should be carefully assessed in potential ablation candidates. The patient requires intraprocedural access to the stoma, making a transisthmus approach less feasible, but this approach is also less pertinent, as RLN injury is not a concern. Therefore, an oblique or longitudinal approach can be considered, although the proceduralist must still be mindful to avoid the posterior capsule and tracheal or esophageal injury. Finally, in areas where the stoma causes skin indentation, the small-footprint phased array transducer may provide better procedural observation.
No competing financial interests exist
.
Authors have received and archived patient consent for video recording/publication in advance of video recording of procedure.
Runtime of video: 8 mins 12 secs
Presented as podium talk at the North American Society for Interventional Thyroidology Annual Meeting, March 11, 2023, in New Orleans, LA.

Get full access to this article
View all access options for this article.
