Abstract
Background:
Persistent hyperparathyroidism after surgical management occurs in ~3%–6% of cases and failure to cure is usually because of an unidentified ectopic or supernumerary gland.Intravagal parathyroid adenoma are rare and can lead to unsuccessful surgical treatment.
Methods:
We present the surgical management of an intravagal parathyroid adenoma in a 49-year-old woman with persistent primary hyperparathyroidism after multiple ineffective attempts of parathyroidectomy.
Results:
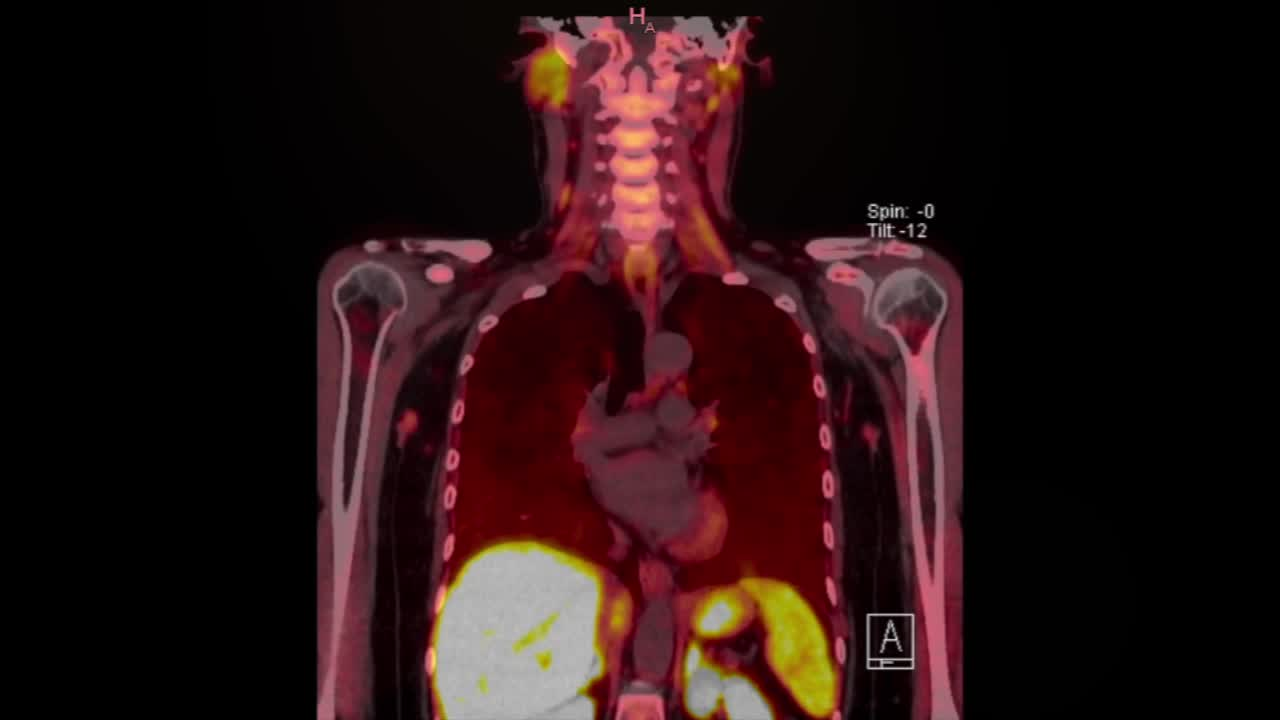
The patient was found to have primary hyperparathyroidism at the age of 22 years. Between 1994 and 2004, she underwent two cervical explorations with resection of the thyrothymic ligaments however with persistent hyperparathyroidism; a mediastinoscopy followed by a thoracoscopic thymectomy was performed without identification of pathologic parathyroid tissue. As complications of the persistent hyperparathyroidism, she developed severe hypercalcemia, recurrent nephrolithiasis, chronic pancreatitis, osteoporosis, gastric ulcer, depression, and musculoskeletal pains. After 15 years of the last surgery, radiologic studies (cervical ultrasound, 99m-Tc-Sestamibi scan and 18F-fluorocholine PET/CT) were repeated and were concordant for a suspected right paratracheal adenoma that was resected. The fresh frozen section turned positive for a lymph node. Intraoperative study of the F-choline PET CT imaging showed an additional zone of high uptake 2 cm cranially to the left carotid bifurcation. A left submandibular laterocervical exploration was carried out and an intravagal autofluorescent parathyroid adenoma was evidenced. We performed a microsurgical dissection of the vagal nerve to resect the adenoma that was embedded into the nerve fibers.1,2 The Parathormone value at the first postoperative day came back to normal and the patient went home with a left recurrent nerve palsy. The histopathologic analysis confirmed a hyperplastic parathyroid gland.
Conclusion:
The high accuracy of 18F fluorocholine in detecting parathyroid adenoma together with the use of intraoperative autofluorescence provides the opportunity to improve the surgical management of patients with persistent hyperparathyroidism because of ectopic localization.
No competing financial interests exist
.
Authors have received and archived patient consent for video recording and publication in advance of video recording of the procedure.
Runtime of video: 5 mins 54 secs
Poster presentation at the 9th Biennial Congress of the European Society of Endocrine Surgeons (ESES), Athens (Greece), May 28, 2022.
Video presentation at the Swiss Congress of Surgery, Bern (Switzerland), February 6, 2022.

Get full access to this article
View all access options for this article.
