Abstract
Abstract
Introduction:
A thyroglossal duct cyst (TDC) is the most common form of congenital anomaly in the neck. There is no consensus regarding the method of choice for preoperative imaging and assessment of a TDC.1–6 However, in a majority of patients, ultrasound (US) was the only preoperative imaging method used.7,8 US is the ideal preoperative investigation for a clinically suspected TDC as it is an inexpensive tool. Although the role of CT scan has been well documented, CT is often utilized only as a complementary technique for confirmation of diagnosis or for assessing complications.1,9,10 The aim of this video was to highlight the value of preoperative CT scan of TDC for surgical planning.
Case:
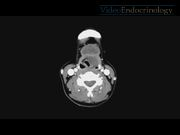
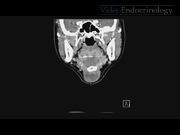
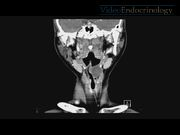
A 46-year-old Chinese female patient with no significant medical history presented in the clinic with a 2-week history of a neck lump. The patient did not have symptoms suggestive of dysphagia, dyspnea, or hoarseness. On physical examination, a 3 × 4 cm nontender cystic lesion was palpated in the midline at the level of the hyoid bone. Thyroid function test was normal. Contrast-enhanced CT scan revealed a 35 × 23 × 22 mm well-circumscribed, well-marginated multilocular cystic lesion in the midline of the anterior neck at the level of the hyoid bone extending down to the infrahyoid region. CT scan also revealed another well-defined 27 × 18 × 25 mm cystic lesion in the pre-epiglottic space that extends into the left paraglottic space, obliterating the supraglottic larynx and the left piriform sinus. Both cystic lesions communicate with each other through the thyrohyoid membrane. Due to the preoperative CT scan findings, the extent of surgical excision can be planned in advance. This will favor the reduction of the chance of recurrence related to incomplete excision. Also, intraoperative dissection must be performed carefully to avoid entering surrounding structures. Furthermore, the intralaryngeal extension could possibly represent a challenge for intraoperative airway management as the laryngeal anatomy is often distorted. A better informed consent can also be taken as the patient can be warned of the increased risk of entering the larynx and pharynx during the surgery and the increased risk of damage to the laryngeal nerves. Our patient subsequently underwent an uncomplicated Sistrunk operation and histopathology confirmed the diagnosis of the TDC. The patient had an uneventful postoperative period and was discharged on postoperative day 3.
Conclusion:
TDC with intralaryngeal extension is rare. To the best of our knowledge, there have been 15 case reports in the literature so far of a TDC with intralaryngeal extension in adults.11–16 Importantly, a patient with symptoms suggestive of a TDC may not necessarily have intralaryngeal extension, as was the case in our patient. As US is the ideal investigation for a clinically suspected TDC, the diagnosis may be made only during surgery. CT scan is an excellent modality for providing information about the TDC location, size, and relation to surrounding structures, which has the potential to help with surgical planning. 17
No competing financial interests exist.
Runtime of video: 7 mins 37 secs
Get full access to this article
View all access options for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
