Abstract
A broad range of psychological treatments is utilized for child and adolescent mental health problems [1]. Psychoanalytic psychotherapy (PP) is suggested as a suitable therapy for adolescents with serious psychiatric and emotional disturbance who have not been able to achieve the developmental tasks of adolescence [2, 3]. Although there is some evidence for the effectiveness of PP with adults [4], there is little empirical research into PP compared to research in cognitive and behaviour-based psychotherapies [5–8].
One reason is that core features of PP are that the patient develops insight about their own intrapsychic conflict and attachment experiences, which influence the formation of their behaviour and defences against anxiety. These relationships are re-experienced by the patient in therapy, referred to as transference and are therefore not easily reduced to quantifiable data [9]. PP thus appears incongruent with randomized controlled trial (RCT) research methodology for evaluating treatment efficacy, which is regarded as the gold standard or highest level of scientific evidence [10–13].
Contrary to the conditions required for an RCT, PP is typically of variable duration, non-manualized and does not target a single disorder or specific symptom [14–16]. Patients receiving PP usually have multiple and complex problems [17]. The therapy is relationship based, focuses on development of insight into the meanings of a symptom rather than the symptom itself, thus the goals of the treatment can be difficult to measure [14, 11]. It has also been suggested that psychoanalytic psychotherapists have actively avoided using scientific methods to demonstrate evidence of treatment effectiveness [5, 11].
There is even less research available on PP for adolescents [15, 18, 19]. Research into adolescent psychiatric problems generally has lagged behind research with adults, possibly reflecting the perpetuation of false assumptions that early psychiatric problems are maturational and will be outgrown, and that treatments that work for adults can be readily applied to children and adolescents [5]. Adolescents who are referred to mental health services usually have high levels of dysfunction, comorbidity and associated family stress [20, 21], which increase the likelihood of poor treatment compliance and dropout, creating further practical obstacles to research [22].
There is growing recognition that the method of participant selection and treatment administration within an RCT does not reflect usual clinical practice and that study results may not readily translate to settings outside the trial [13]. The problem of the external validity of RCTs is addressed by complementary ‘effectiveness studies’. These studies use a naturalistic design and evaluate a treatment's effectiveness under real practice conditions [23]. Effectiveness studies can yield useful and credible empirical validation of a treatment [12, 17] and the methodology is more readily applied to PP than RCT methodology.
Some effectiveness studies have been conducted into PP for adolescents. Trowell et al. reported on 72 children and young adolescents with moderate–severe depression who received 9 months of individual PP [24]. After treatment 75% of participants were no longer clinically depressed, and 6 months on, none was clinically depressed. A comparative group who received family therapy had similar results after treatment but slightly less success 6 months later, with 81% no longer clinically depressed.
Empirical studies of cognitive behaviour therapy, interpersonal therapy, pharmacotherapy and their combination demonstrate therapeutic effectiveness for depressive, obsessive–compulsive and anxiety disorders in adolescents [25] but approximately 30% of patients do not respond to treatment and high rates of relapse are reported [6–8, 26]. Therefore, research into the effectiveness of alternative treatments for adolescent mental illness such as psychoanalytic therapy is necessary [11, 16, 27].
This paper reports on changes to the mental health and general functioning of adolescents with complex, severe mental illness who received individual PP for up to 12 months in addition to usual management. The adolescents had a range of diagnoses and comorbid symptoms severe enough to warrant referral for assessment for inpatient treatment through public Child and Mental Health Services (CAMHS). Most were currently receiving or had received inpatient treatment.
Using a naturalistic study design, we aimed to determine whether PP was associated with changes to symptoms and functioning beyond changes associated with CAMHS treatment as usual (TAU) for adolescents with serious mental illness. It was expected that PP would be associated with a reduction in depressive, social and attention problems and an increase in overall functioning beyond improvements associated with TAU after 12 months. Given the recognized association between family functioning and adolescent mental illness [15], the study also examined family functioning over time and its association with PP.
Method
Study design
In this longitudinal, naturalistic study participants were the natural clinical population of adolescents consecutively referred to CAMHS for inpatient services assessment. The adolescents did not have to fulfil specific diagnostic criteria thus there was strong external validity [11]. Open-ended PP was offered when a therapist was available at the time of initial assessment as an additional treatment to CAMHS TAU. Those who did not receive PP formed a comparison group. All participants completed an initial assessment and were then reassessed at 12 month follow up. The naturalistic design reflects real clinical practice, in which patients were referred to PP when it was available rather than randomly allocated. The effectiveness of PP was compared, using the same outcome measures, with CAMHS TAU in a clinical setting where variables could not be controlled or manipulated [28].
Participants and procedure
Ethics approval was obtained from the university and health services. Participants were aged 12–18 years and well enough to provide consent and be interviewed; parents/carers were also asked to provide participatory consent. When possible, the assessment of patients who were too unwell was postponed until they were well enough to participate. Participants were required to have sufficient English to complete the assessment measures and participate in therapy. These minimal exclusion criteria ensured the inclusion of typical diagnostically complex cases referred to CAMHS.
A total of 80 young people with serious mental illness consecutively presenting to the CAMHS inpatient service were enrolled in the study. Because this was a naturalistic clinical study, therapists were not always available. Therefore random allocation was not possible but PP was offered to 40 young people (25 female) each time a therapist became available. The other 40 youth (18 female) were allocated to the assessment-only group. All of the young people continued to receive TAU.
Of the 40 adolescents offered PP, 23 (15 female) engaged in the therapy. The reasons for not accepting PP were because they thought the therapy was unnecessary (n = 5); their circumstances prevented therapy (e.g. the family was unsupportive, participation in therapy was not possible because the adolescent was engaged in multiple other treatments; n = 10); the therapist became unavailable (n = 2). The 17 adolescents who did not agree to therapy were invited to continue with the assessment-only TAU comparison group. Seven agreed and were re-allocated to the comparison group.
At 12 month follow up, 55 (32 female, mean age = 15.11 years) of the original 80 young people enrolled in the study agreed to be reassessed (68.75% retention). They consisted of 22 PP participants and 33 in the TAU comparison group.
Forty-six of the 55 participants were currently receiving or had received inpatient treatment. One participant from the PP group and 24 from the assessment-only group did not participate at 12 months. The main causes of attrition were that the family declined to participate (80%) or were not contactable (20%).
Psychotherapy treatment
Treatment consisted of once- or twice-weekly individual 50 min sessions. Patients were offered indefinite therapy but could terminate treatment at will. Eighteen patients remained in therapy at 12 months. The length of treatment among patients who completed therapy ranged from 4 to 9 months (mean = 6.8 months).
The therapists were 13 trainees or graduates of Monash University's Master of Child Psychoanalytic Psychotherapy postgraduate course. The course emphasizes an inclusive object relations approach to psychotherapy, incorporating the three schools of the British Psycho-Analytic Society [29, 30]. The therapists used an interpretative model utilizing transference and counter-transference processes, except at times when the young person was psychotic and a supportive model was used. All therapists had weekly supervision from supervisors trained in the same course. The common training received by therapists and supervisors increased the likelihood that the nature of the psychotherapy provided was similar and consistent.
Measures
Assessments were performed prior to commencement of therapy and 12 months later. Adolescents completed the Youth Self Report (YSR) and parents completed the companion Child Behaviour Checklist (CBCL) [31]. Normative data for children (0–18 years) are available for these reliable and valid psychometric measures [31]. The CBCL and YSR include 123 competence and behavioural problem items rated on a 3 point scale for how well each item describes the child. These items are split into two broadband factors of externalizing and internalizing behaviours containing eight constructs/syndromes. Withdrawn–Depressed subscale was examined on the YSR and Social and Attention subscales on the CBCL.
Parents and adolescents each completed the 12-item General Functioning Scale of the Family Assessment Device (FAD) [32, 33]. These items rate seven dimensions of family functioning on a 4 point scale. The FAD is a widely researched instrument with good internal consistency and test–retest reliability and validity, and measures global family functioning. Higher FAD scores indicate greater family dysfunction.
CAMHS case clinicians completed the Global Assessment of Functioning (GAF), a 100 point hypothetical continuum of mental health through to severe mental illness, and the Global Assessment of Relational Functioning (GARF), an equivalent continuum for overall family functioning. For both these clinician-rated assessments, low scores indicate greater difficulties in overall functioning [34, 35]. Research project clinicians also completed a GAF and GARF based on participants’ accumulated information and independent of the clinicians’ rating. Case clinicians made a DSM-IV diagnosis as part of the standard CAMHS assessment procedure. Diagnostic information at initial assessment is reported for descriptive purposes.
Data analysis
The initial results for adolescents who engaged in therapy were compared with results for adolescents who did not engage, using analysis of variance (ANOVA) and χ2 test. Equivalent analyses were conducted for adolescents who did and did not complete a 12 month assessment. Twelve month results were analysed using analysis of covariance (ANCOVA). Group (PP, assessment only) was the between-subjects factor, 12 month results the dependent variable and corresponding initial results the covariate. ANCOVA was used to account for pretreatment differences because it is generally the most powerful of the alternatives [36]. Differences between the PP and assessment groups at 12 months were further examined using the Johnson–Neyman (J-N) technique [37] to take account of a possible relationship between initial severity of symptoms and outcome.
Results
Engagement in therapy
Engagement was not associated with sex, age, or results of individual or family measures at initial assessment.
Retention at 12 months
There was no significant association between participation at 12 months and sex, age, results of measures at initial assessment, single- or two-parent family status or country of birth. The following analyses exclude adolescents who did not participate at 12 months.
Demographics
Table 1 shows the demographic profiles of the two groups. There was no significant difference in mean age (F(1,53) = 2.05, p > 0.05). There was not a significantly higher proportion of female subjects in the PP group (χ2(1) = 1.51, p > 0.05).
Subject characteristics
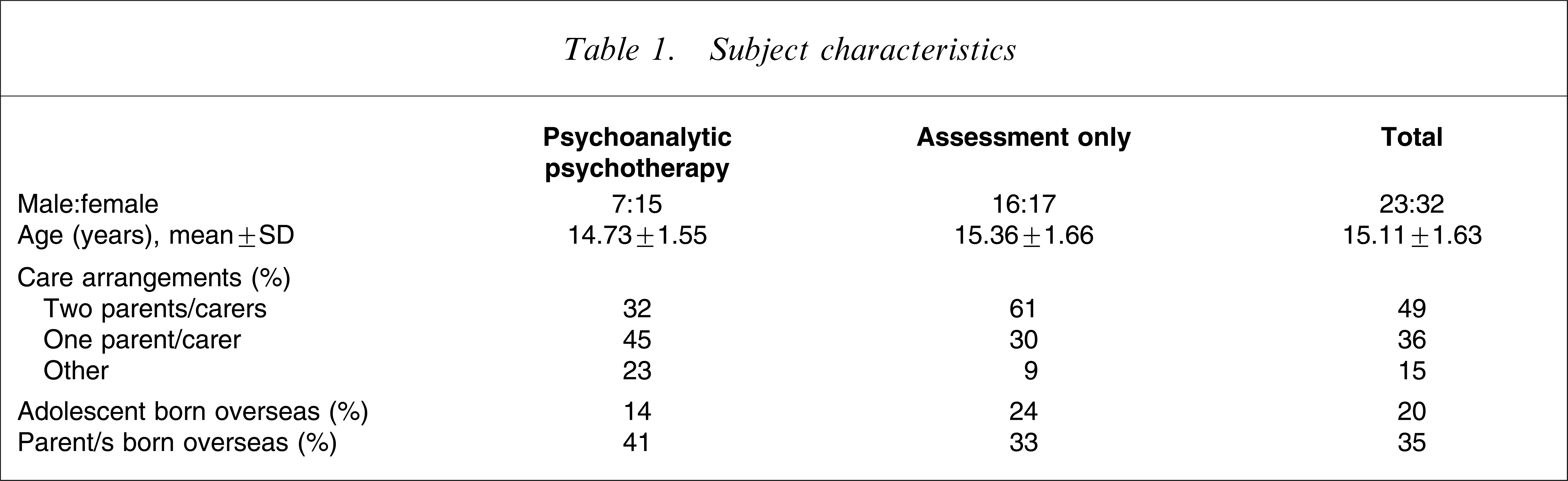
A greater proportion of the PP group lived with a single parent (Table 1). Care arrangements overall differed from national data, which show that 80.5% of children living with family live in a two-parent/carer home [38]. The percentage of overseas-born participants (Table 1) was higher than national census data, which show that 24% of the population were born overseas and 26% of Australian-born people have a parent born overseas [39]. Nine of the 11 adolescents born outside Australia were born in non-English-speaking nations.
Table 2 shows the principal DSM-IV Axis I diagnoses at initial assessment. Most adolescents (64%) had multiple Axis I diagnoses, with parent–child relational problems the most common second diagnosis (n = 13). More psychotherapy participants had multiple Axis I diagnoses than assessment-only participants (91% vs 45%). On DSM-IV Axis IV, all PP participants and 76% of assessment-only participants were diagnosed with ‘problems with primary support group’.
DSM-IV Axis I Principal Diagnosis (n = 55)
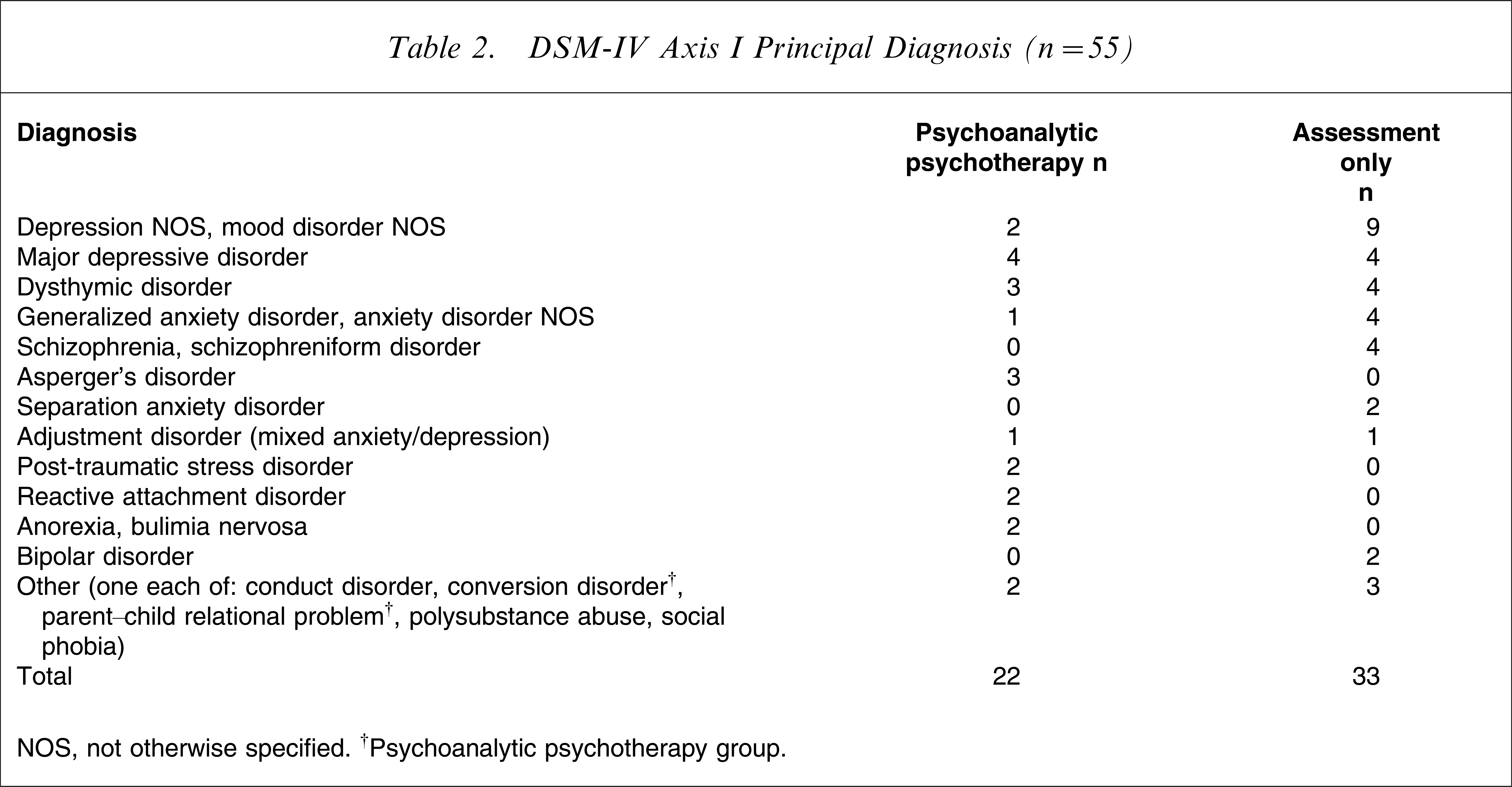
NOS, not otherwise specified. †Psychoanalytic psychotherapy group.
Results of measures at initial assessment
Most adolescents (55%) obtained a GAF score of ≤50, indicating serious symptoms and/or seriously impaired functioning; 43% reported borderline–clinical or clinical levels of Withdrawn–Depressed symptoms, 36% had clinical-level attention problems and 37% clinical-level social problems. Forty-nine per cent obtained a GARF score of ≤60, indicating that their family unit was ‘clearly dysfunctional with, at best, occasional times of satisfying and competent functioning’ [34]. Seventy-one per cent of adolescents and 41% of parents reported clinical-level family dysfunction on the FAD.
12 month assessment results
Sex and age were investigated as possible covariates. A series of ANOVAs with 12 month results as the dependent variable, sex as the between-subjects factor and initial results as the covariate found no effect of sex. There was no association between age and group (F(1,53) = 2.05, p > 0.05) and correlational analyses showed that age was not associated with 12 month results. Sex and age were not included as covariates.
Table 3 presents a summary of results of measures versus group. There were significant between-group differences in initial GAF scores (F(1,53) = 10.14, p < 0.01) and initial adolescent-reported FAD scores (F(1,52) = 8.35, p < 0.01), reflecting greater psychopathology in the PP group on these measures.
Measures versus group (mean±SD)
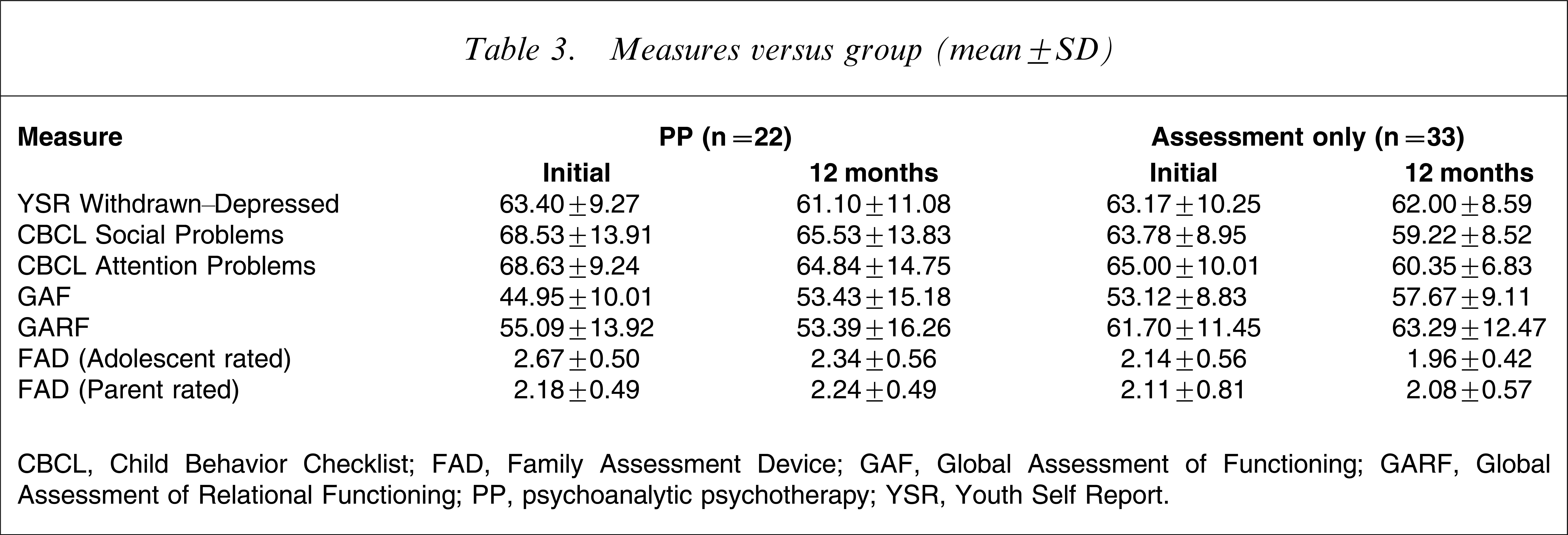
CBCL, Child Behavior Checklist; FAD, Family Assessment Device; GAF, Global Assessment of Functioning; GARF, Global Assessment of Relational Functioning; PP, psychoanalytic psychotherapy; YSR, Youth Self Report.
YSR Withdrawn–Depressed problems
A significant main effect of treatment group was found for 12 month Withdrawn–Depressed problems, covarying for initial scores (F(1,40) = 7.49, p = 0.01). The interaction term (group×covariate) was also significant (F(1,40) = 7.30, p = 0.01). The interaction presented a problem for interpreting the ANCOVA results because it indicated that an assumption of the test was violated. The assumption is homogeneity of regression slopes within the treatment groups [37]; that is, that treatment group is unrelated to the covariate in predicting the outcome variable. The interaction indicated that the magnitude of the treatment effect varied for different levels of the covariate [40, 41]. The violation can cause ANCOVA results to be misinterpreted [41].
An alternative to ANCOVA is the J-N technique [37], which does not assume homogeneity of slopes. The technique can establish the value of the covariate beyond which groups differ significantly with regard to the dependent variable. Using J-N analysis, a significant difference between the groups was identified when the initial level of problems was >74.60. For adolescents in this range, which is above the clinical cut-off of 70, psychotherapy was significantly more effective than TAU in reducing symptoms. The value corresponded to the 88th percentile in the total sample, indicating that approximately 12% of adolescents would be expected to benefit from psychotherapy above TAU in reducing Withdrawn–Depressed symptoms.
CBCL attention problems
The main effect of group was not significant (F(1 35) = 4.00, p = 0.05), but the interaction between group and the covariate (initial Attention score) was significant (F(1,35) = 4.55, p = 0.04), indicating that J-N analysis was again suitable. J-N analysis identified that psychotherapy was superior to TAU when initial Attention Problems score was >71.88 (clinical cut-off = 70). The value corresponded to the 73rd percentile; indicating that 27% of patients would be expected to benefit from psychotherapy above TAU.
CBCL social problems
The main effect of group was not significant (F(1,31) = 2.21, p = 0.15) but there was a near-significant interaction between group and the covariate (F(1,31) = 2.89, p = 0.09). J-N analysis showed that the psychotherapy group differed significantly from the assessment-only group when initial problems were >67.72, just above the borderline–clinical range cut-off of 65. The value corresponded to the 65th percentile, indicating that approximately 35% of patients would be expected to benefit from psychotherapy beyond TAU in reducing social problems.
GAF scores
Researcher-rated GAF and GARF scores were highly correlated with scores provided independently by case clinicians at initial assessment (GAF: r = 0.72, p < 0.01.; GARF: r = 0.64, p = 0.01) and at 12 months (GAF: r = 0.70, p < 0.01; GARF: r = 0.58, p = 0.01), supporting the validity of researcher ratings.
Researcher-rated GAF scores increased significantly at 12 months across all participants (F(1,51) = 15.20, p = 0.00). Covarying for initial scores, the main effect of treatment group was not significant (F(1,48) = 1.09, p > 0.05) nor was there an interaction between group and initial scores (F(1,48) = 1.28, p = 0.26).
Family functioning
An ANCOVA with 12 month GARF scores as the dependent variable did not identify a significant main effect of group (F(1,48) = 1.66, p > 0.05) or a significant interaction (F(1,48) = 1.38, p = 0.25). There was no overall change to GARF scores over time (F(1,51) = 0.36, p = 0.55).
Analyses of 12 month adolescent- and parent-rated FAD results similarly failed to identify an effect of group, covarying for initial values (F(1,40) = 0.023, p > 0.05; F(1,24) = 1.05, p > 0.05, respectively). There was no overall change to parent-reported family functioning, but adolescents reported a significant decrease in dysfunction (F(1,42) = 14.10, p = 0.001).
Discussion
After 12 months, PP was associated with a greater reduction in depressive, social and attention problems than TAU for adolescents whose problems were initially more severe. Specifically, adolescents whose initial depressive or attention problems were in the clinical range (representing 12% and 27% of the group, respectively) or whose social problems were in or above the borderline clinical range (35% of the group) appeared to benefit. In contrast, there was no significant effect of psychotherapy on global functioning or family functioning.
At initial assessment, adolescents typically displayed high levels of complex symptomatology, diagnostic diversity and impaired functioning, consistent with the profile of CAMHS inpatients [42]. The high rates of comorbid Axis I diagnoses, problems with primary support group and educational/occupational difficulties reflected that these adolescents typically faced multiple and complex difficulties. Family dysfunction was typical and consistent with other studies [42–45].
A key finding identified through J-N analysis [37] was that the effectiveness of the therapy over TAU depended on adolescents’ initial level of symptomatology, or a ‘floor effect’ [46], with the effect of therapy being most salient for those adolescents with more severe problems. This finding empirically supports a conclusion that PP might add value to the treatment of the most severely ill adolescents by further improving those who have not responded as well to usual management. Usual CAMHS case management includes medication, cognitive behavioural therapy, psychoeducation and parental guidance, family therapy, social skills group programmes and school or workplace consultation and liaison.
The adolescents’ overall functioning as indicated by GAF scores was not significantly improved by psychotherapy, although there was a trend toward greater improvement in the therapy group. General functioning is a broad construct and other studies have similarly reported that PP did not improve the overall functioning of young people more than other types of treatment over a 12 month period [24, 47]. It is possible that a significant shift in overall functioning may take longer than 12 months.
Family functioning did not significantly improve according to parent or researcher report. Perhaps the result is not surprising. PP was provided to the adolescent only and family therapy is not always provided by CAMHS, although parent education and guidance is provided briefly to families of inpatients. The ongoing difficulties experienced by families of adolescents with mental illness have been reported elsewhere [43], and results emphasize the family unit as a necessary focus for clinical attention. Nonetheless, the results further support the effectiveness of psychoanalytic treatment for the adolescent, because improvements often occurred in the context of ongoing family dysfunction.
Limitations
Participant dropout occurred at two points: 17 of 40 adolescents assigned to psychotherapy did not engage; and 25 of 80 adolescents did not complete a 12 month assessment, only one of whom had received therapy. The higher rate of attrition in the assessment-only group might reflect that this group did not receive a tangible benefit from involvement and therefore was less motivated to participate.
Adolescents who did or did not participate in the 12 month assessment were comparable on demographic and initial results, suggesting that the attrition did not create a bias in the remaining sample. It is acknowledged that the higher rate of attrition in the assessment group might have artificially improved the group's 12 month results, if adolescents functioning well at 12 months were more likely to participate than adolescents doing poorly. A less likely alternative is that adolescents doing well were less likely to participate at 12 months, with the implication that the assessment-only group was biased towards adolescents doing poorly; thus presenting a greater challenge to the interpretation and validity of the study's results.
The participants who did not engage in the therapy are also a potential source of bias. Most of the adolescents who did not accept PP perceived the therapy as unnecessary, or personal circumstances prevented attendance. The dropout cases may have influenced the outcome results for both the therapy and assessment groups. An inability to engage in therapy possibly indicated a more general difficulty to treat, suggesting that these were more difficult cases with poorer prognoses generally [48]. If so, their removal from the psychotherapy group might have artificially increased the group's scores. Further, the seven adolescents who were re-assigned to the assessment-only group may have lowered that group's 12 month scores.
Contrary to these possibilities, adolescents who did and did not engage in therapy were comparable on almost all aspects of initial assessment, suggesting that the dropout group were not markedly different from those accepting therapy. The seven adolescents who did not engage in PP but who completed a 12 month assessment were compared to the remaining assessment-only participants. No significant differences were found at 12 months, suggesting the seven cases did not significantly bias the assessment-only group's results.
The enrolment process and a lack of random allocation to PP may have biased results if patients with particular characteristics such as receptivity to treatment, were enrolled and if these characteristics caused them to improve regardless of treatment. This criticism of the internal validity of this and other effectiveness studies is valid. It is not possible to definitively infer that differences between a treatment and non-treatment group are caused by the treatment, only that differences are associated with the treatment [13]. There are advantages, however, to a naturalistic design.
While a randomized controlled trial has greater internal validity; a naturalistic design is likely to have better external validity [12, 17]. The two methods combined might best provide empirical validation of psychotherapy [12].
The high rate of Axis I comorbidity and family dysfunction in the psychotherapy group confirms that complex and difficult cases were engaged in treatment. The study results showed that therapy was most beneficial when initial symptoms were severe, confirming the suggestion of Fonagy that PP may particularly suit difficult and complex adolescent cases [9].
Conclusions
This naturalistic study found that individual PP combined with TAU was associated with a greater reduction in symptoms than TAU alone for adolescents who initially experienced clinical levels of depressive, social and attention symptoms. Results support the literature indicating that PP is a justifiable and effective additional treatment option for seriously mentally ill adolescents [24, 47, 48]. In contrast, PP did not provide an added therapeutic effect on family functioning, which remained problematic over time. The development of more effective interventions to improve the well-being of patients’ parents and families requires greater clinical and research attention.
A strength of PP is that it can be applied in the treatment of a range of psychiatric disturbances and can be used to treat patients with complex or multiple diagnoses. These patients may be less responsive to short-term symptom-specific interventions [17]. The period of time required for treatment to have an effect was relatively short (12 months), which contrasts with conceptions of PP as necessarily lengthy. The current study is ongoing, with further long-term follow-up assessments pending. It will be important to establish whether gains made in the first 12 months are maintained or develop over time.
Footnotes
Acknowledgements
The authors thank Dr Stanley Gold for his contribution to the initial proposal, obtaining funding and as the chairperson of the advisory committee; participating Victorian CAMHS, Stepping Stones Inpatient Unit clinicians (Southern Health); and Ms Nicola Williams for her contribution to data collection and clinical interviews. This research was funded by The Pratt Foundation and The Dara Foundation.
