Abstract
‘Do you have any idea how much schizophrenics smoke? Tons. It's unbelievable.’ http://thestoneoftear.blogspot.com/2007/07/denialism-blog-shows-some-bad-science.htmls
The most recent review of studies reporting on smoking and schizophrenia among both outpatients and inpatients showed that the pooled prevalence of smoking in people with schizophrenia in published studies across 20 nations was 62%, with a range of 14–88% [1]. A smoking prevalence of >80% was found in 6/42 (14.3%) of the studies, with the numbers of smoking patients in these six studies totalling 484/4686 (10.3%) of all smokers in the studies. We have observed, however, in the introductory and discussion sections of research literature and in press reports and websites that smoking prevalence in people with schizophrenia is often reported as being much higher, frequently ‘around’, ‘up to’ or ‘about’ 90%, a level markedly higher than the average 62% when the 42 studies were pooled. A recent widely publicized report on smoking by people with mental illness in Australia [2] recycled the same statement (‘People with schizophrenia in particular have extremely high rates of smoking, with most studies finding a prevalence rate of about 90%’) [3].
Citation bias is the selective citation of published results to support the findings, arguments or interests of authors and those funding their work [4]. Journal prestige and impact factors [5] are common contributors to citation bias [6], and there are associations between authors’ nationality and ethnicity and the country of the journals in which they publish [7–9].
We were curious to determine whether citation bias exists in research literature on the reporting of the prevalence of smoking in people with schizophrenia. We were also curious to determine whether websites tend to report higher rates of smoking by people with schizophrenia than lower, more realistic rates.
We examined evidence relevant to the consideration of two hypotheses: (i) that studies on the prevalence of smoking in people with schizophrenia that found high rates of smoking would be cited more often than studies showing lower rates of smoking; and (ii) that statements about smoking rates among people with schizophrenia on the Internet would report extremely high rates instead of more realistic, less dramatic rates.
Methods
Hypothesis 1
On 26 September 2008, total and average per year citation counts for all 42 studies included by de Leon and Diaz [1] in their 2005 meta-analysis of global studies showing the prevalence of smoking in samples of people with schizophrenia were obtained from the Web of Science. Negative binomial regression was used to estimate the association between the number of citations and the reported prevalence of smoking in people with schizophrenia. The log of the number of years since publication was included in the model as offset. We also examined whether the country where the study was carried out (USA vs elsewhere), and whether the prestige of the journal in which studies were published (measured by average journal impact factor obtained from Journal Citation Reports for 2002–2006) was associated with the number of citations per year.
Hypothesis 2
‘What percent of schizophrenics smoke?’ was entered into the Google search engine, and the contents of the first two screens (i.e. 20 links) returned were examined. Eighty-eight per cent of web traffic has been observed to go to the first five results returned from online searches [10].
Results
Hypothesis 1
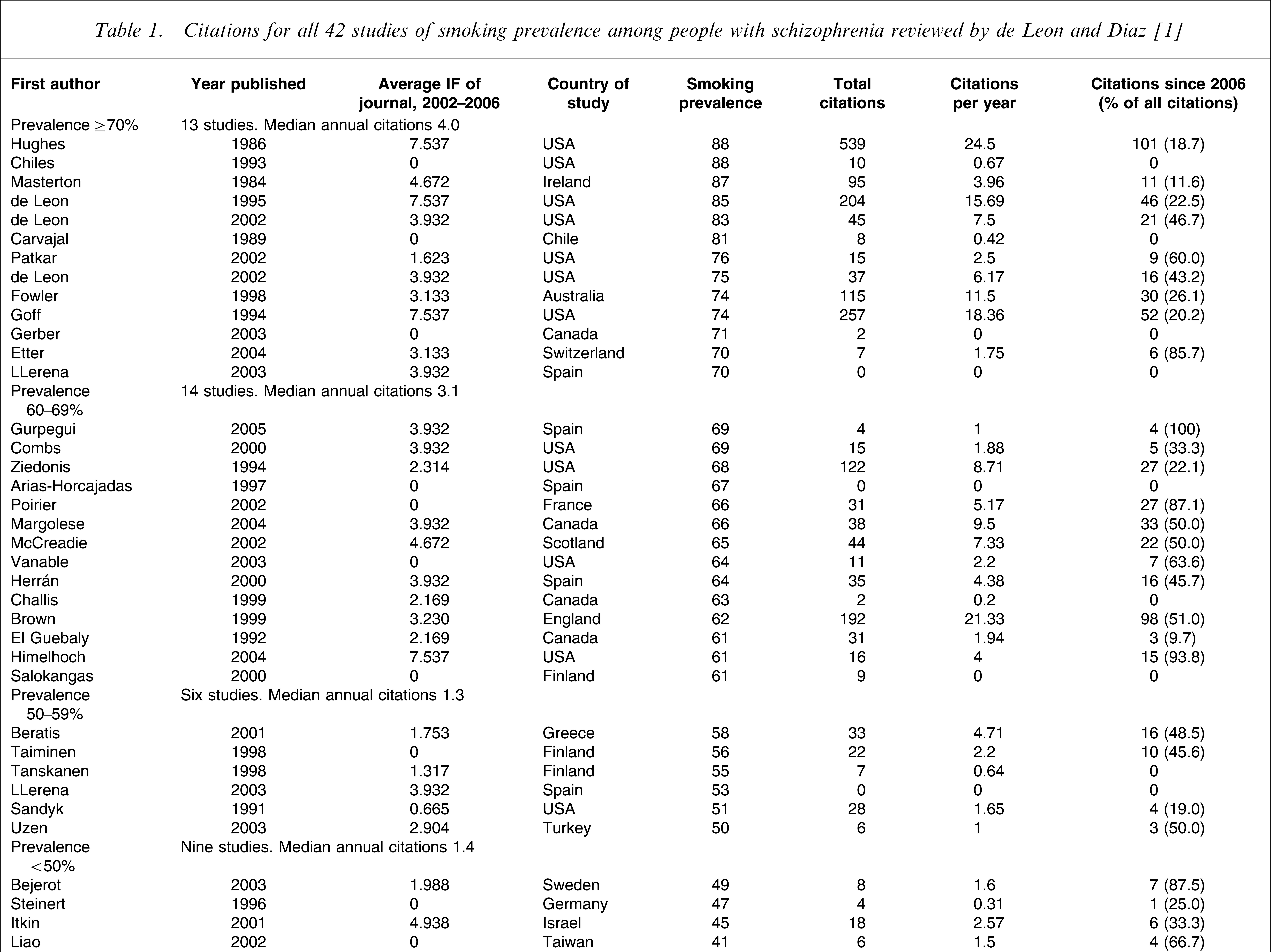
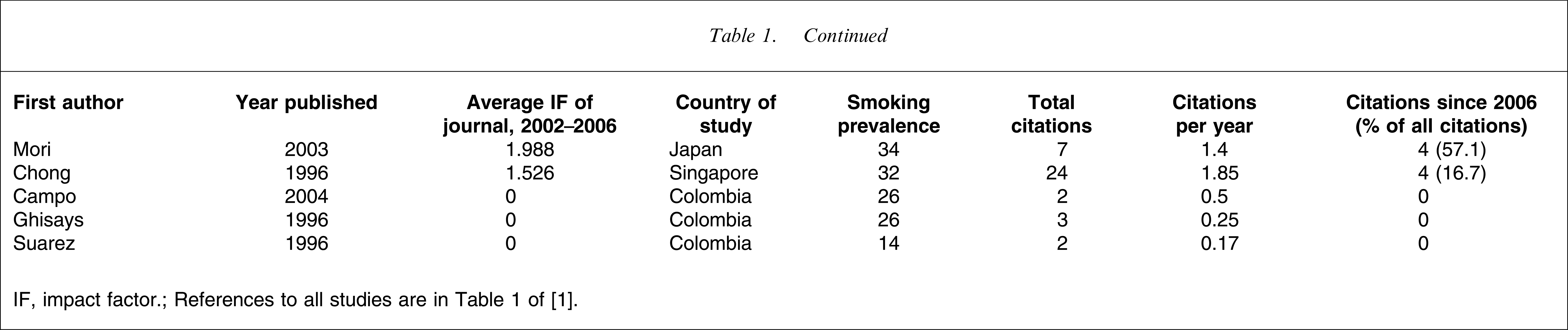
Table 1 shows citations for all 42 studies of smoking prevalence among people with schizophrenia reviewed by de Leon and Diaz [1].
Citations for all 42 studies of smoking prevalence among people with schizophrenia reviewed by de Leon and Diaz [1]
A 10% increase in the reported prevalence of smoking was associated with a 61% (95% confidence interval (CI)=30–98%) increase in the rate at which a paper was cited. The country of study did not have an effect on the citation rate (p=0.90), after adjusting for journal impact factor. Journal impact factor was significantly related to citation rate (p=0.001), with the rate at which a paper was cited increasing by 32% (95%CI=12–56%) for an increase in impact factor of 1. After adjustment for impact factor, a 10% increase in the reported prevalence of smoking was associated with a 28% increase (95%CI=1–62%) in the rate at which a paper is cited. The prevalence of smoking was also moderately associated with impact factor (Spearman rank correlation=0.44, p=0.004).
Hypothesis 2
Table 2 shows relevant excerpts from the first 20 sites returned from the search string ‘what percent of schizophrenics smoke?’ entered into Google. Nine sites referred to a smoking prevalence of at least 80%, with a further six including a prevalence of at least 80% within their range. Only two accurately referred to prevalence being around 60%.
Statements on smoking prevalence among people with schizophrenia contained in the first screen returned for Google search string ‘What percent of schizophrenics smoke?’

Discussion
Papers reporting a high prevalence of smoking among people with schizophrenia are cited more often than studies showing a lower prevalence, providing confirmatory evidence of citation bias favouring higher prevalence studies.
The citation bias existed independently of country of study. This result was reduced when impact factor was taken into account, although it remained statistically significant. Papers reporting higher smoking prevalence rates tended to be published in journals with higher impact factors. This may indicate a publication bias, whereby authors of such studies anticipate high interest in startling reports, which might be reciprocated in editors seeing such papers as potentially newsworthy. There is an association between the news value of research and its subsequent downloading and citation rates [11].
The present study takes evidence about citation bias a step further by showing how this bias toward scientific citation of higher rates of smoking is also reflected in publicly accessible information about smoking by people with schizophrenia. With Google returns dominated by links showing statements of ultra-high smoking prevalence, the public as well as health professionals could be forgiven for believing that the prevalence of smoking in people with schizophrenia is ‘about 90%’.
Where does this figure come from? We can only presume that it originates from a small but highly influential early paper by Hughes et al., which showed the prevalence of smoking in a sample of people with schizophrenia to be 88% [12]. This finding derived from a sample of only 24 people with schizophrenia living in one US city and attending a hospital outpatient service in 1981–1982. Researchers have since cited the paper often (n=539), with peak citations occurring in 2005: 23 years after the data were collected, despite its age and small sample size. Among the 21 citations to the Hughes et al paper made in 2008 (27 years after data collection) was a statement in Physiological Reviews that ‘it has been shown that people with schizophrenia smoke cigarettes at a very high rate,
In many nations, smoking prevalence in the general population has fallen markedly in recent decades. In Australia for example, the proportion of adults who smoke at least weekly has halved from 36% in 1980 [14] to 17.9% in 2007 [15]. If, today, researchers or journalists were to routinely refer to smoking prevalence today as being 36%, such grossly incorrect statements would be strongly criticized as ill-informed. An apparent propensity for researchers and commentators to erroneously ‘talk up’ smoking rates in people with schizophrenia is therefore noteworthy and the ‘around 90% smoke’ may qualify as a ‘factoid’: ‘a spurious (unverified, incorrect, or invented) ‘fact’ intended to create or prolong public exposure or to manipulate public opinion’ (http://en.wikipedia.org/wiki/Factoid).
Some authors have also inflated the figures. For example, a 2004 review stated: ‘patients with schizophrenia smoke at nearly three times the rate of the general population, with most studies finding prevalence rates of about 90%’ [16], and cited three supportive references that all reported smoking prevalence of below 90% [12, 17, 18].
Since 2005 researchers have had the opportunity to cite the de Leon and Diaz meta-analysis with its mean 62% smoking prevalence. It has so far attracted a creditable 70 citations: still considerably less than the Hughes et al. 1986 study, which continues to be the highest cited paper (with 101 citations since 2006). From 2006 to the present, the 42 studies in the de Leon and Diaz meta-analysis have been cited 589 times.
The de Leon and Diaz meta-analysis drew heavily on clinical populations. There are few general population estimates of smoking prevalence among those with schizophrenia, but a US study of data from 1991–1992 found current smoking rates for respondents with no mental illness, lifetime non-affective psychosis, and past-month non-affective psychosis of 22.5%, 49.4%, and 45.3%, respectively. Those with a history of mental illness also had substantial quit rates [19]. A recent 11 year follow up of a Canadian sample of outpatients with schizophrenia found that smoking prevalence had fallen from 63.2% in 1995 to 43.3% in 2006, a rate of decline highly favourable compared with cessation rates in the wider Canadian community [20]. Notions that people with schizophrenia almost all smoke and that their smoking is intractable are therefore contestable.
Nonetheless, people with schizophrenia are seldom advised to quit smoking [21, 22] and are sometimes advised not to do so [23, 24], despite evidence that they are interested in cessation [25]. Governments do not run campaigns and seldom allocate resources to help them quit. Too often, doctors and nurses think that it is reasonable for mentally ill patients to smoke, because somehow the same concerns about the health and welfare costs of smoking are implied to not apply [26]. Too often, people in psychiatric hospitals are given cigarettes to keep them calm, or as staff bonding gestures [27].
It is possible that an important reinforcer of the higher than average rates of smoking among those with schizophrenia in most countries is the ubiquity of the 90% factoid. If such a large percentage of those with schizophrenia are assumed to smoke, then many would reason that it must be somehow intrinsic to their disease. If their smoking is explained by their disease, then health professionals may believe that there is little they can do about it, and that there is no point in trying. Sociocultural and contextual factors relevant to an understanding of smoking among people with schizophrenia can remain unexamined. We believe that erroneous assumptions about the near inevitability of smoking in people with schizophrenia may reinforce institutional and clinical neglect of this stigmatized group of people and stultify innovation in targeted smoking cessation. Although it is possible that the repetition of the ‘around 90%’ factoid may be motivated by a well-meaning concern to magnify the severity of the issue to attract support or funding, uncritical recitation of statements about misleadingly high smoking rates in schizophrenia patients should be challenged.
Footnotes
Acknowledgements
This study was funded by a 2006 research grant from the Cancer Council New South Wales.
