Abstract
Keywords
Mounting data suggest an association between trauma, particularly childhood trauma, and adult somatization [1–3]. These data mainly come from three sources. First, traumatized individuals have been found to show more somatization and endorse more medically unexplained symptoms than non-traumatized subjects [4]. This seems to be particularly true for those with a history of childhood trauma [5–7] and those who meet diagnostic criteria for post-traumatic stress disorder (PTSD) [8], [9]. Second, in medical patients from primary care settings, trauma, PTSD and somatization were closely linked [10], [11]. Similarly, patients with a variety of unexplained symptoms including chronic pain have frequently experienced childhood maltreatment [12–14]. The same holds true for patients suffering from syndromes with ill-defined pathological mechanisms such as irritable bowel syndrome or fibromyalgia [15–17]. Third, childhood trauma has often been observed in mental disorders characterized by somatization, that is, the somatoform disorders. Specifically, child abuse and neglect have been associated with both hypochondriasis and conversion disorders including pseudoseizures [18–22]. While the association between early adverse life experiences and later somatization has been well established, the underlying mechanisms are poorly understood [23]. Recently it has been suggested that emotional arousal and insecure attachment, which can both arise from childhood maltreatment, may have a mediating function in the causal chain from childhood trauma to adult somatization [23], [24].
Independent of these important pathways, there is surprisingly little knowledge about childhood maltreatment in patients with the most extreme form of somatization, that is, somatization disorders. For example, Morrison reported a significantly higher frequency of molestation (defined as unwanted sexual contact with or without intercourse) among 60 women with somatization disorder as compared to 31 women with affective disorders, but he did not investigate other forms of childhood maltreatment [25]. In a consecutive series of female outpatients screened for at least two medically unexplained symptoms Pribor et al. found significantly more histories of childhood sexual, physical and emotional abuse in those 51 women with Briquet's syndrome (which is very similar to DSM-IV somatization disorder) than in those without this syndrome [26]. Most recently, Brown et al. compared 22 patients with somatization disorder to 19 neurological patients with dystonia [27]. They reported a significantly higher exposure score for emotional abuse and greater severity of physical abuse in the somatization patients than in the neurological patients, but the two samples did not differ with respect to early separation, neglect or sexual abuse. In addition to some inconsistencies, particularly regarding the relevance of sexual abuse, these previous studies hold some methodological limitations. Two of the cited investigations did not apply a structured interview to capture childhood trauma, did not include other types of trauma than abuse (i.e. neglect) and focused exclusively on women [25], [26]. The most recent study [27] included patients with an organic disease as a comparison group; therefore it remains undecided if the reported findings are specific for patients with somatization disorder or if they can be found in other mental disorders such as depression, which has been associated with traumatic early-life experiences, too [28–30].
Taking these considerations into account, the aim of the present paper was to clarify previous inconsistencies and to overcome methodological shortcomings of prior studies. To adequately assess all types of childhood maltreatment we applied both a structured interview and a self-report measure widely used in trauma research [31]. Furthermore, we did not exclude men because both general population and clinical studies suggest that a relevant proportion of subjects with somatization disorders are male [32–34]. Finally, our comparison sample consisted of patients with major depressive disorder (MDD) matched for age and gender.
Method
Procedure and participants
The selection criteria consisted of DSM-IV diagnosis of somatization disorder, age between 18 and 65 years, exclusion of any organic or psychotic disorder as well as intellectual disabilities that impair understanding of the study and engagement in the interview and self-report questionnaire. Both inpatients and outpatients referred to Ernst-Moritz-Arndt-University Department of Psychiatry and Psychotherapy were screened with respect to the selection criteria. Within the study period a total of 35 patients with somatization disorder were eligible, but four individuals refused to participate, and three dropped out for logistical reasons. Thus, 28 patients with DSM-IV somatization disorder as confirmed by the respective section of the Structured Clinical Interview for DSM-IV, Axis I (SCID-I) [35] were included in the study group. The comparison group consisted of 28 patients with MDD as diagnosed by the brief German version of the Anxiety Disorders Interview Schedule [36], [37]. None of the MDD patients met criteria for current or lifetime somatization disorder as assessed by the SCID-I [35]. They were matched to the patients of the study group on age, gender, and – if possible – on socioeconomic status. All participants gave written informed consent.
Instruments
The Structured Trauma Interview (STI) is an expert interview addressing traumatic childhood experiences including parental dysfunction, early separation from parents (before the age of 12 years), witnessing interparental violence as well as sexual and physical abuse before the age of 16 years. The term ‘parents’ also includes step- and adoptive parents. ‘Parental dysfunction’ represents the operationalization of emotional neglect referring to the unavailability of either mother or father due to recurrent illness, nervousness, depression, and use of psychotropic substances. It has the advantage to refer to observable behaviour of caregivers rather than to purely perceived unavailability or lack of affection. ‘Early separation from parents’ indicates an interruption in the continuous relationship between the child and his caregiver for more than 6 months. ‘Witnessing interparental violence’ is defined as observation of physical or sexual violence between the parents. ‘Physical abuse’ according to the STI refers to severe parental aggression including being kicked or hit with a fist or an object, being tied up, or being thrown down the stairs. ‘Sexual abuse’ is defined as any pressure to engage in or any forced sexual contact ranging from fondling to penetration. Although the STI has been used in several studies [18], [38], [39], no data on its reliability and validity have been published.
The Childhood Trauma Questionnaire (CTQ) was used for the self-report of child maltreatment [40]. It is brief, reliable and valid screening device for histories of childhood trauma including emotional, sexual and physical abuse as well as emotional and physical neglect. Twenty-eight items about childhood events are endorsed on a 5-point Likert scale with higher scores indicating more severe forms of traumatic experiences. In independent studies the CTQ was reported to have good reliability and validity. Additionally, the five-factor model (i.e. the five subscales reflecting the different types of childhood trauma) was empirically confirmed [40–43].
Statistical analysis
The data analyses were computed using SPSS, version 12.0 (SPSS, Chicago, IL, USA). Patients of the study and control group were compared by analyses of variance for continuous variables and χ2 test for categorical variables; if case frequency was <5, Fisher's exact test was applied. Due to the small sample size we also calculated effect sizes (Cohen's d) when possible. The relationship between somatization disorder (dependent variable) and the various types of childhood maltreatment as assessed by the STI (independent variables) was assessed by means of binary logistic regression according to the backward elimination method. For significant predictors, we report regression coefficients (β), odds ratios (ORs) and 95% confidence intervals (CIs). Significance level was set at p < 0.05.
Results
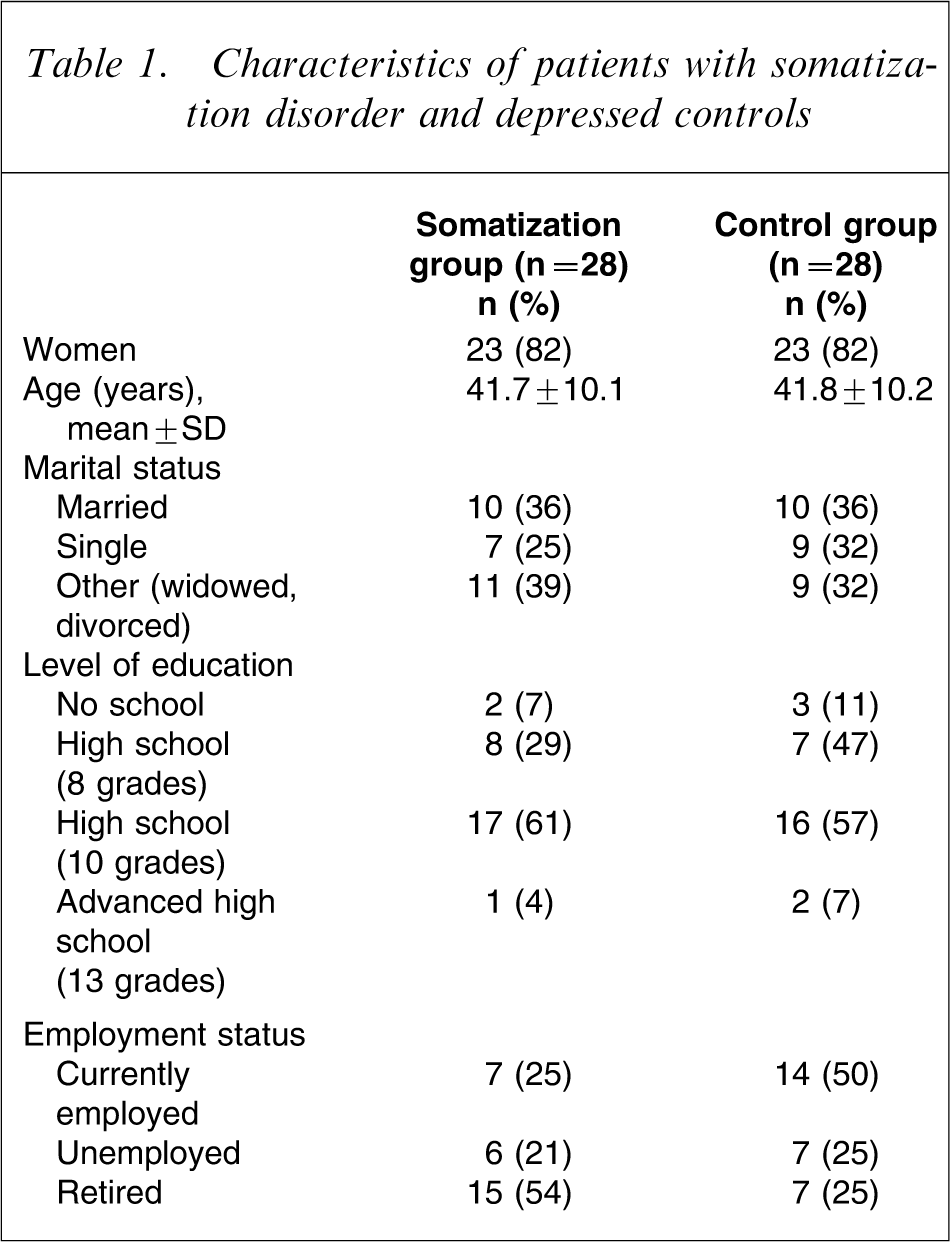
The sociodemographic characteristics of both the patients with somatization and affective disorders are presented in Table 1. As can be seen, there were no differences with respect to sex or age. Furthermore, both groups were almost matched for their socioeconomic status as indicated by the marital status (χ2=0.45, p = 0.799), the educational background (χ2=0.63, p = 0.889), and the employment status (χ2=5.32, p = 0.070).
Characteristics of patients with somatization disorder and depressed controls
According to the STI there were no differences between the study and the control group with respect to parental dysfunction, early separation from parent, and witnessing interparental violence. But physical abuse, particularly abuse by mothers, and sexual abuse were significantly more frequent in patients with somatization disorders than in those with MDD. Further descriptive characteristics of the traumatic childhood experiences indicating their severity and duration are given in full detail in Table 2.
Comparison of expert-rated traumatic childhood experiences (STI) between patients with somatization disorder and depressed controls
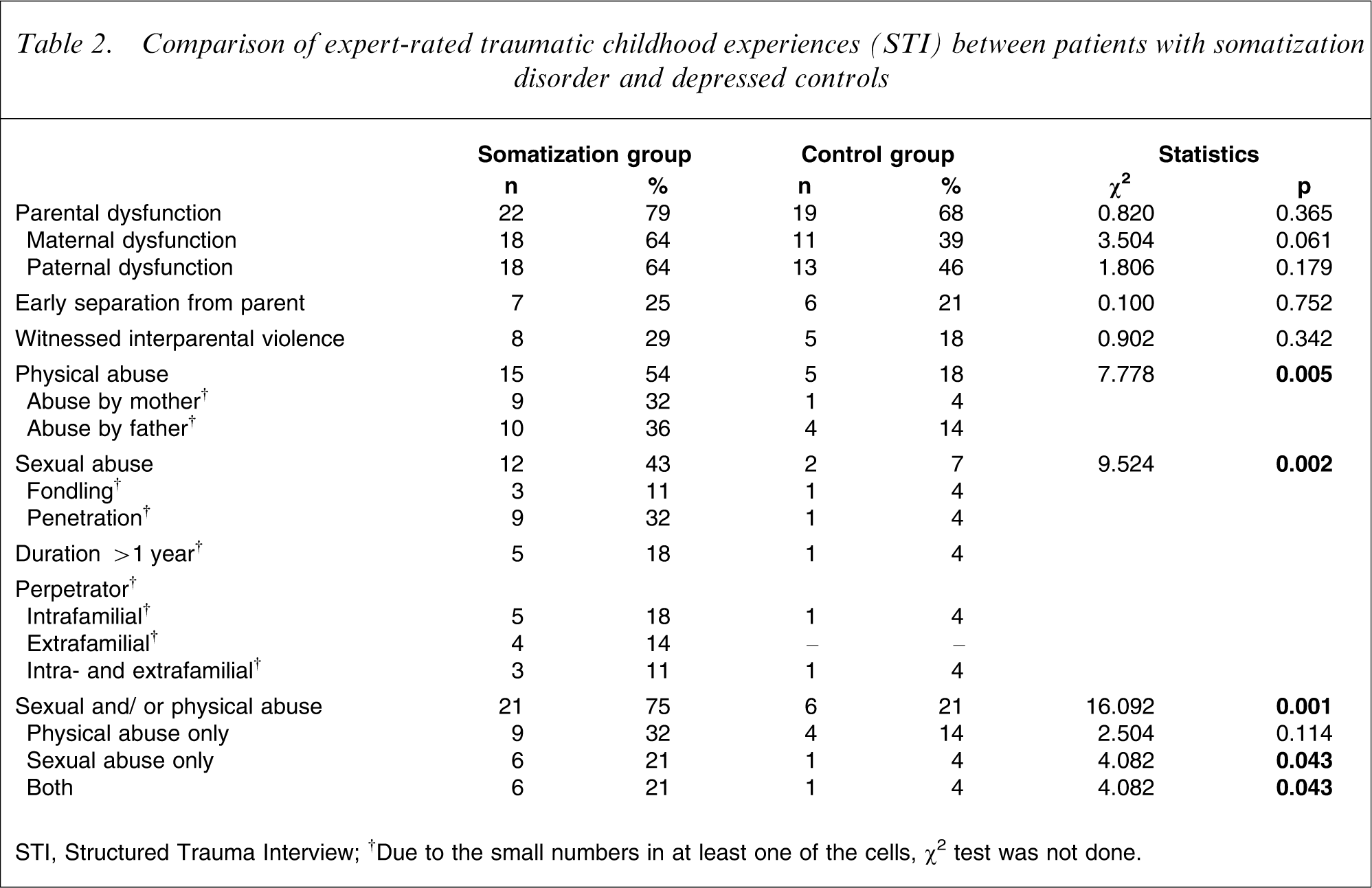
STI, Structured Trauma Interview.
†Due to the small numbers in at least one of the cells, χ2 test was not done.
A similar pattern was captured by the self-report questionnaire, as shown in Table 3. Patients with somatization disorders scored significantly higher in the CTQ total score and in the subscales sexual and physical abuse as well as physical neglect as compared to the MDD patients.
Comparison of self-reported childhood maltreatment (CTQ) between patients with somatization disorder and depressed controls
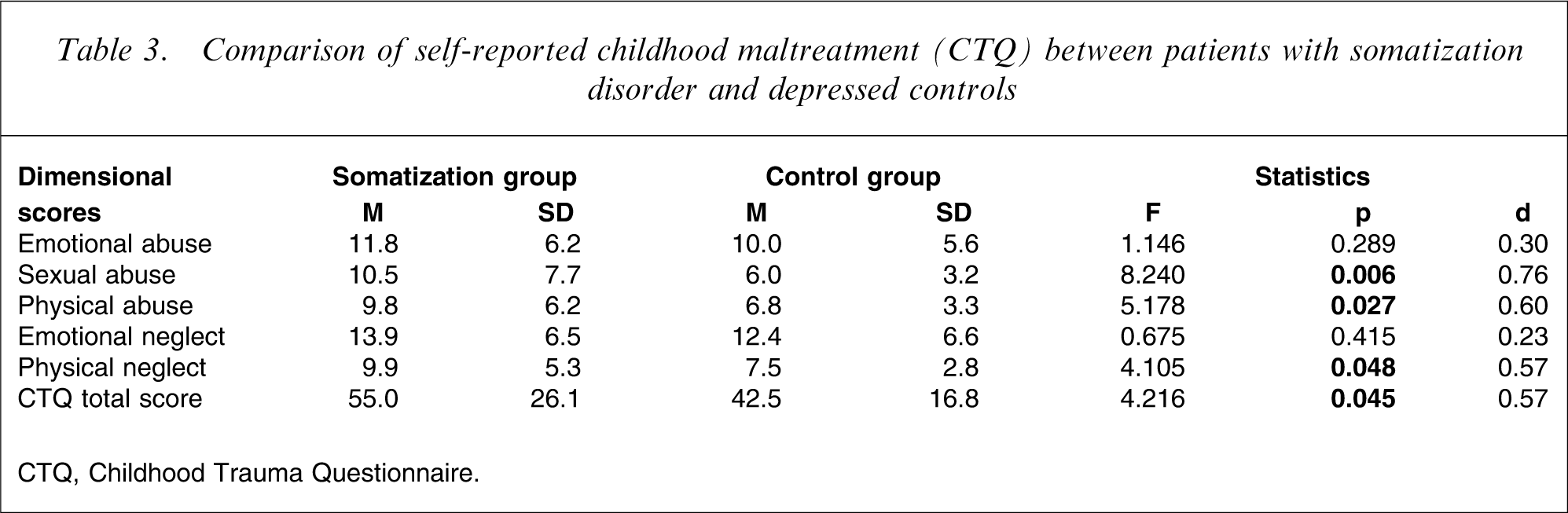
CTQ, Childhood Trauma Questionnaire.
In a stepwise backward logistic regression with somatization disorder as the dependent variable and STI childhood traumatic experiences as independent variables, parental dysfunction, early separation from parent, and witnessing interparental violence were not retained in the equation. The only significant predictors were both physical abuse (β = 1.63, OR = 5.11, 95%CI = 1.37–19.0) and sexual abuse (β = 2.24, OR = 9.39, 95%CI = 1.73–50.96). Likewise, when entering the CTQ subscales as independent variables, only sexual abuse emerged as significant predictor (β = 0.15, OR = 1.16, 95%CI = 1.01–1.35).
Discussion
To the best of our knowledge this is the first study assessing all types of childhood maltreatment (i.e. abuse and neglect) in patients with somatization disorders as compared to patients with MDD matched for age and gender. Categorical data derived from the interview and dimensional scores obtained by the self-report measure indicated a strong association between somatization disorder and childhood sexual abuse in both univariate and multivariate analyses. The odds of having been sexually abused was ninefold higher in somatization patients relative to MDD subjects (OR = 9.39, 95%CI = 1.73–50.96). Additionally, the interview findings indicated that physical abuse may be an important factor, but this was not confirmed by the results of the questionnaire. Both interview and self-assessment did not find differences between somatizing and depressed participants with respect to other types of maltreatment including parental dysfunction, emotional neglect, early separation from caregivers or emotional abuse. Physical neglect as assessed by the CTQ might also be related to somatization disorder (effect size d = 0.57). We were not able to confirm this finding by the expert rating, but it must be kept in mind that the trauma interview does not adequately address physical neglect such as deprivation of food, clothing, shelter or medical care. Therefore, the putative association between physical neglect and somatization disorder warrants replication.
The present results are consistent with prior research indicating a close link between sexual abuse and somatization disorder [25], [26]. In contrast, the most recent study addressing this issue failed to find such a relationship [27]. But, rather than reporting the total number of participants with sexual abuse, the median of the greatest severity and total exposure scores were presented, which makes it difficult to compare these findings with the present data.
Although childhood physical abuse was related to somatization disorder in prior research [26], [27], the present results are inconclusive. Although the expert rating suggested that physical abuse may be important, the self-rating produced a significant result only in univariate analysis, not in multivariate analysis. The same studies found emotional abuse to be associated with somatization disorder [26], [27]. In contrast, we were not able to replicate this association, but emotional abuse was assessed only by the self-report measure in the present study. Further studies are needed to clarify the relationship of somatization disorder to physical and emotional abuse. In line with the investigation by Brown et al. [27], the present findings do not indicate that emotional or physical neglect, parental dysfunction, early separation from parent or witnessing interparental violence are related to somatization disorder.
Several methodological limitations of the present study merit discussion. Due to the relatively small size of the study population (n = 28 in each sample) statistical power may be compromised; but a post-hoc analysis showed that the power of the regression models was 90% with an α of 5%. Nevertheless, the precision of the risk estimates was low as reflected by large confidence intervals. Thus, the present findings should be regarded as preliminary and need to be replicated with larger numbers of patients suffering from somatization disorder. Furthermore, because we included patients referred to a university department (i.e. a tertiary care setting), it remains unknown if the present results can also be applied to other samples of somatizing individuals, for example in the general population or in primary care settings. Another methodological limitation is the disregard of axis II disorders. For example, the percentage of comorbid personality disorders (PDs) ranged between 50% and 70% among subjects with somatization disorders [44], [45]. Conversely, there is a tight link between PDs, somatoform disorders and somatization [46]. This is particularly true for borderline personality disorder [47], [48], which has also been associated with childhood trauma [49–51]. Therefore it might well be that the reported relationship between childhood sexual abuse and somatization disorder is mediated by an underlying borderline condition.
Despite these caveats possibly limiting the generalizability of the present findings, we suggest that childhood maltreatment, particularly sexual abuse, may be a relevant factor in somatization disorder. Prior studies indicated that abused children are likely to develop an insecure attachment [52], [53], including the expectation that others will not meet one's emotional needs, and this expectation, in turn, may prompt two reactions that interact in the development of somatization. First, because caregivers have been experienced as unreliable, the child will focus the attention on the self and the body, possibly resulting in a body-focused attentional bias, which is a key factor in somatization [24]. Second, experiencing important others as unresponsive to emotional distress can increase the emphasis on and reporting of somatic concerns as a way to seek their help [23], thus ‘communicating psychological distress in the form of somatic symptoms’ [54]. These considerations indicate that our understanding of the multifactorial aetiopathogenesis of somatization [24], [54] might be broadened by integrating a developmental perspective focusing on childhood adversities [55], [56]. Finally, treatment of patients with somatization disorders is difficult and does not have a lasting and clinically meaningful influence on the physical complaints [57]. Integrating trauma-therapeutic techniques and interventions might improve the psychosocial treatment outcomes of these patients. Future research is warranted to shed light on these issues.
