Abstract
Hysteria has been an important and well-accepted disease for 3900 years, with an extraordinary and irregular conceptual evolution that ended in its disappearance from the majority of scientific writings [1]. In 1980 hysteria was replaced by distinct illnesses in the DSM and ICD, namely somatization, dissociative, and conversion. The DSM-IV-TR classifies conversion disorder within somatoform disorders, along with somatization disorder [2]. In the ICD-10 conversion disorder is categorized as a dissociative disorder (keeping its ‘hysteria’ designation), and somatization disorder goes with somatoform disorders [3]. Many investigators, however, noted the great overlap between dissociative and somatoform disorders, as defined in DSM and ICD [4–8]. Several investigations showed that dissociative disorders may present with somatic symptoms [7, 9–17] and conversion symptoms [7, 10, 11, 18]. Conversely, many patients with somatization disorder also have dissociative symptoms [17, 19], especially if they have been abused [17, 20]. Additionally, many patients with conversion disorder report dissociative symptoms [8, 21–23], namely patients with pseudoneurological conversion conditions [24–29]. There is a great overlap between these disorders, and many studies have defended the inclusion of the conversion disorder in the group of dissociative disorders [6, 30, 31], like Pierre Janet's perspective [32]; while others have supported the differentiation between conversion and somatization [33].
Dissociation, somatic and psychological, seems to be the underlying mechanism of these three pathologies. The mechanism of psychoform dissociation involves the loss of the integration of consciousness, memory, identity, and perception of the environment [2]. Somatoform dissociation is viewed as the lack of integration of somatic experiences, functions and responses [34–38]. The most extensively employed self-report measures of dissociation, the Dissociative Experiences Scale (DES) [39] and Somatoform Dissociation Questionnaire (SDQ-20) [36], were developed to measure psychoform and somatoform dissociation, respectively.
As far as we know, no other study has investigated the three hysterical nosological presentations, nor compared them with other psychopathological disorders in terms of somatoform and psychoform dissociation. This study was undertaken to assess the common and different features of somatization, dissociative and conversion disorders, studying the phenomena of psychoform dissociation, somatoform dissociation, and general psychopathology, and to compare them with other psychiatric conditions.
Methods
We present the cross-sectional and self-report data collected.
Subjects
We selected 151 patients from among 1162 consecutive cases registered between 2005 and 2006 from three mental health centres; they met DSM-IV criteria for conversion disorder (n=26), dissociative disorders (n=39), somatization disorder (n=40) and other psychiatric disorders (n=46). Twenty-seven were inpatients and 124 were outpatients. We ruled out patients with psychotic disorders, substance abuse disorders, bipolar disorder, personality disorders, and those under 18 years old. Expert clinicians with several years of training (mean practice=19.7 years) performed a longitudinal evaluation using all data available (LEAD methodology) [40]. Because of logistical factors, only the diagnoses of 62 of these patients were confirmed with a Portuguese version of the Dissociative Disorders Interview Schedule (DDIS) [41]. Due to discharge, two patients did not fill out the SDQ-20. None of the other psychiatric patients met criteria for any of the aforementioned disorders. All patients gave written informed consent, and anonymity was preserved, according to the Code of Medical Ethics of the World Medical Association Declaration of Helsinki.
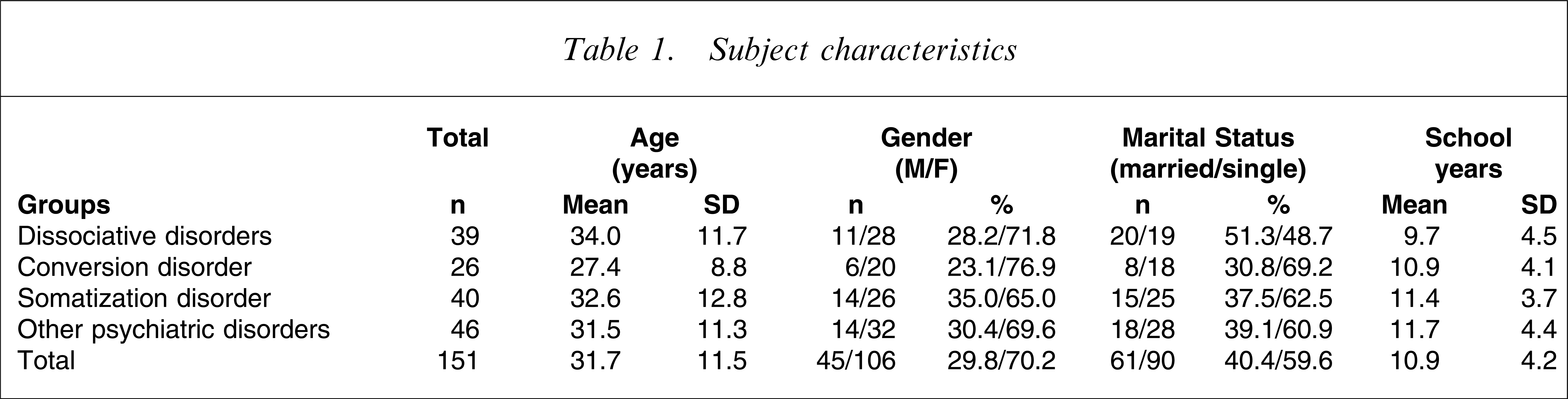
The demographic characteristics of the samples are listed in Table 1. There were no significant differences in age among the four groups (F=1.81, df=3, p>0.05), nor between genders (χ2=1.14, df=3, p>0.05), marital status (χ2=3.10, df=3, p>0.05), school years (F=1.82, df=3, p>0.05), or number of inpatients versus number of outpatients (χ2=7.07, df=3, p>0.05). Table 2 lists the subsample diagnosis frequencies.
Subject characteristics
Group pathologies and their main disorder frequencies (n=151).
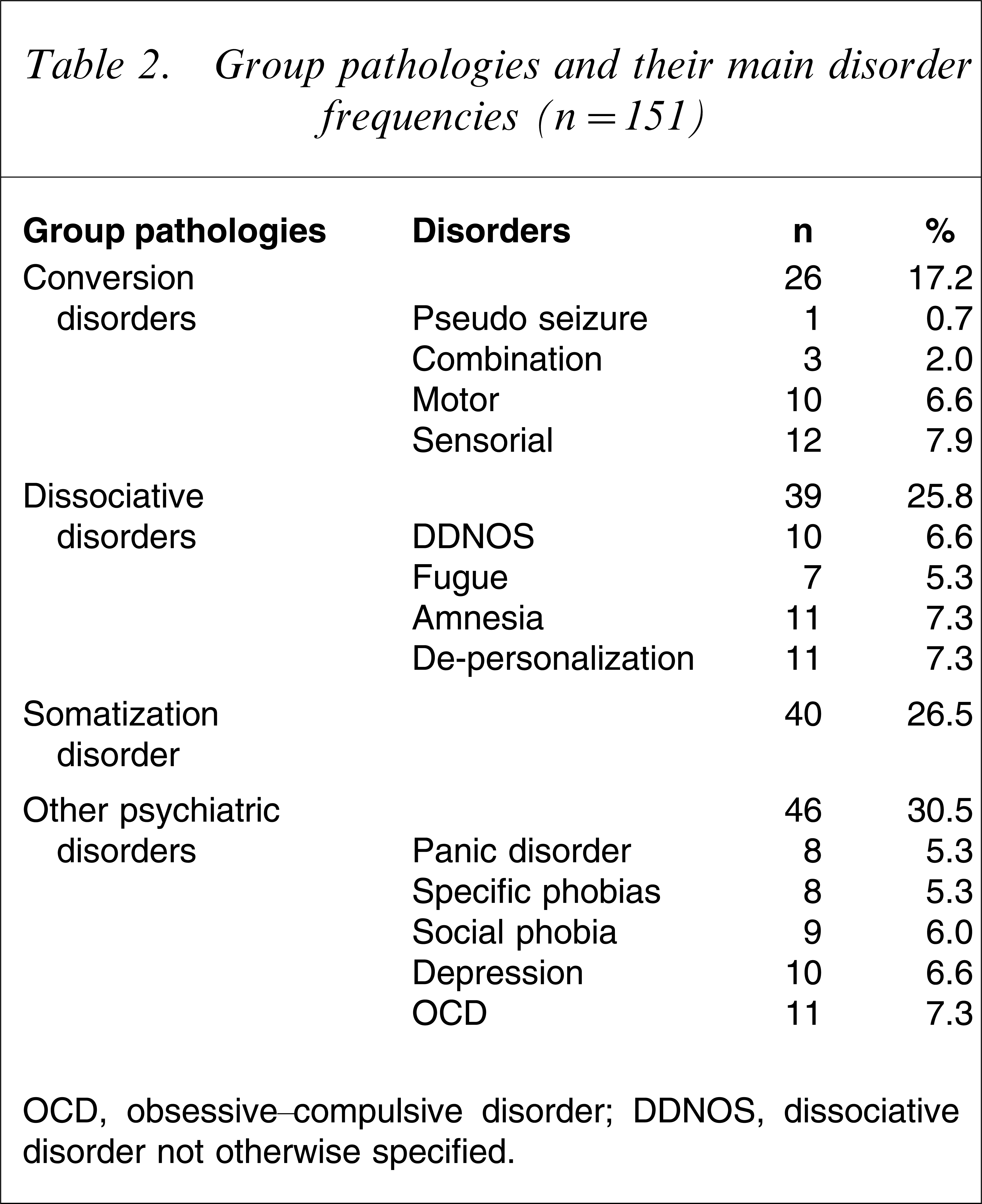
OCD, obsessive–compulsive disorder; DDNOS, dissociative disorder not otherwise specified.
Instruments
Dissociative Experiences Scale: Portuguese version
The DES is a self-administered 28-item questionnaire that measures the frequency of dissociative experiences [39], with subjects answering by circling the percentage of time they experience dissociation (0–100 in increments of 10%). The Portuguese version has good reliability (Cronbach's α=0.94) [42].
Somatoform Dissociation Questionnaire
The SDQ-20 is a 20-item self-administered tool to evaluate the intensity of somatoform dissociation [36]. Reliability of the Portuguese form was 0.88 (Cronbach's α) [43].
Brief Symptom Inventory
The Brief Symptom Inventory (BSI) is a 53-item self-report clinical rating scale that measures psychological distress (global severity index: GSI) and nine dimensions: somatization, interpersonal sensitivity, anxiety, phobic anxiety, obsessive–compulsive symptoms, depression, hostility, paranoid ideation, and psychoticism [44]. We used the Portuguese threshold of ≥1.7 [45] for each subscale as an indication of symptom severity. These symptom subscales do not correspond to psychiatric diagnosis. Cronbach's alpha for the subscales ranged from 0.62 (phobic anxiety) to 0.80 (somatization).
Dissociative Disorders Interview Schedule
The DDIS is a 131-item semi-structured interview that identifies all dissociative disorders, somatization disorder, and conversion disorder according to DSM-IV diagnoses, and in agreement with a Portuguese adaptation (sensitivity=84%, specificity=100%, and overall κ=0.83) [41, 46].
Statistical analysis
Data were analysed using SPSS 11.0.3, for Mac OS X (SPSS, Chicago, IL, USA). Subjects with the four diagnoses were compared with each other according to the frequency (mean DES scores) and severity (cut-off score ≥30) of dissociative experiences; mean SDQ-20 scores, and severity; distress and psychopathological symptoms from the BSI. None of these measures was normally distributed, therefore Kruskal–Wallis tests were used, followed by post-hoc Mann–Whitney tests on each pair of groups and adjusted p with Bonferroni method (p divided by the six paired comparisons made; in this way a significant level was set at p<0.008).
Results
Results are described through the DES, SDQ and BSI measures used in this study.
Psychoform dissociation: DES
The DES ratings of all 151 patients ranged from 1.92 to 72.69, with a mean±SD of 26.82; there were no significant differences (U=23.42, p=0.935) between the mean DES scores of women (26.32±14.03) and men (27.97±17.55) or between single (26.23±15.34) and married patients (27.69±14.90) (U=2555.50, p=0.579). Inpatients (mean±SD=30.06±15.40) and outpatients (mean±SD= 26.10±15.06) did not differ significantly (U=1425.00, p=0.249). There was no significant correlation between age and the scale scores (ρ=0.138, p=0.094) or between number of school years and scale scores (ρ=0.102, p=0.214). Thirty-eight per cent of the patients scored ≥30. There were no significant differences between higher and lower scores in terms of demographic characteristics.
Mean±SD DES scores were higher for the conversion patients, followed by dissociative disorders, somatization, and the comparison group. These scores differed significantly overall (H=68.86, df=3, p<0.001, Kruskal–Wallis one-way analysis of variance by ranks). Pairwise post-hoc U-tests showed that dissociative and conversion patients did not differ, nor did somatizing patients from the comparison group. The other group comparisons, however, were significantly different. These results are shown in Table 3.
DES, SDQ, GSI scores and psychopathological symptoms (n=151)
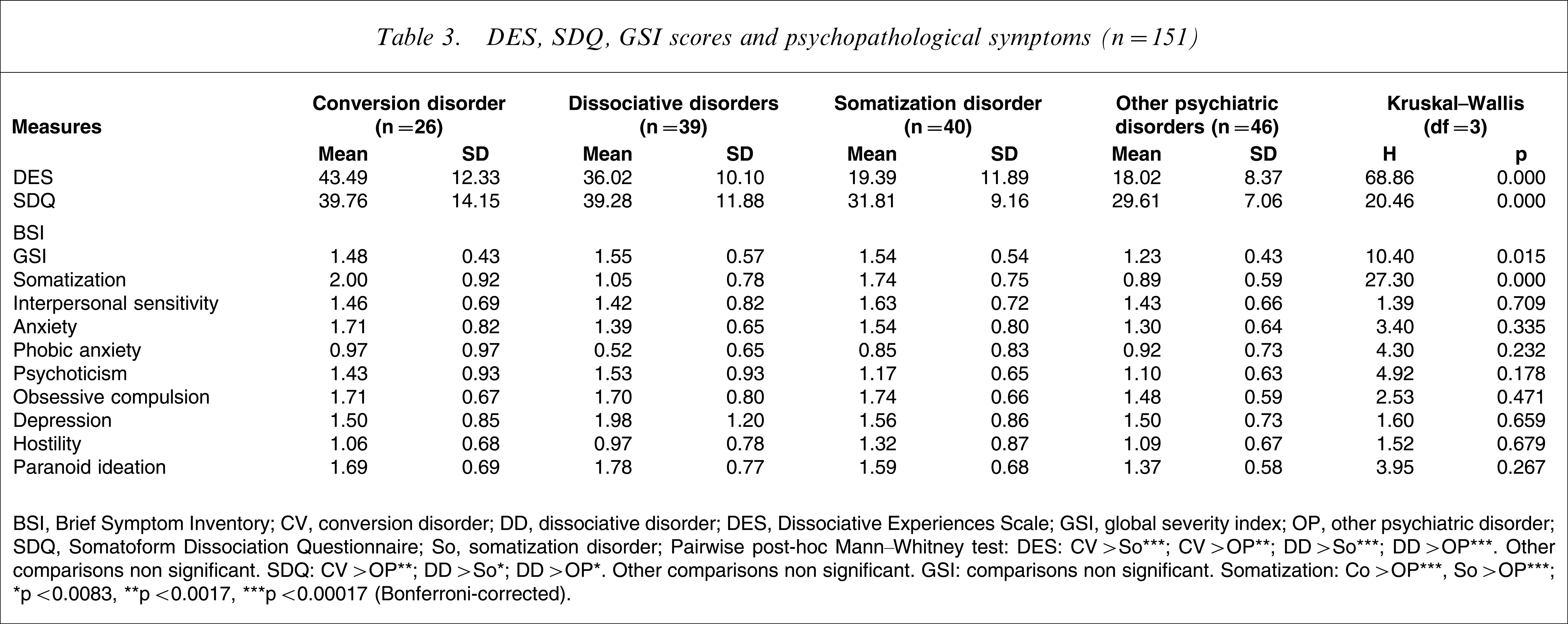
BSI, Brief Symptom Inventory; CV, conversion disorder; DD, dissociative disorder; DES, Dissociative Experiences Scale; GSI, global severity index; OP, other psychiatric disorder; SDQ, Somatoform Dissociation Questionnaire; So, somatization disorder.
Pairwise post-hoc Mann–Whitney test: DES: CV>So∗∗∗; CV>OP∗∗; DD>So∗∗∗; DD>OP∗∗∗. Other comparisons non significant. SDQ: CV>OP∗∗; DD>So∗; DD>OP∗. Other comparisons non significant. GSI: comparisons non significant. Somatization: Co>OP∗∗∗, So>OP∗∗∗.
∗p<0.0083, ∗∗p<0.0017, ∗∗∗p<0.00017 (Bonferroni-corrected).
The proportions of patients from the diagnostic categories with scores above cut-off on the DES are presented in Table 4. Conversion and dissociative patients had significantly more severe dissociative experiences than patients with somatization or other psychiatric disorders (H=58.73, df=3, p<0.001).
Scores above the cut-offs on DES and SDQ-20 (n=151).
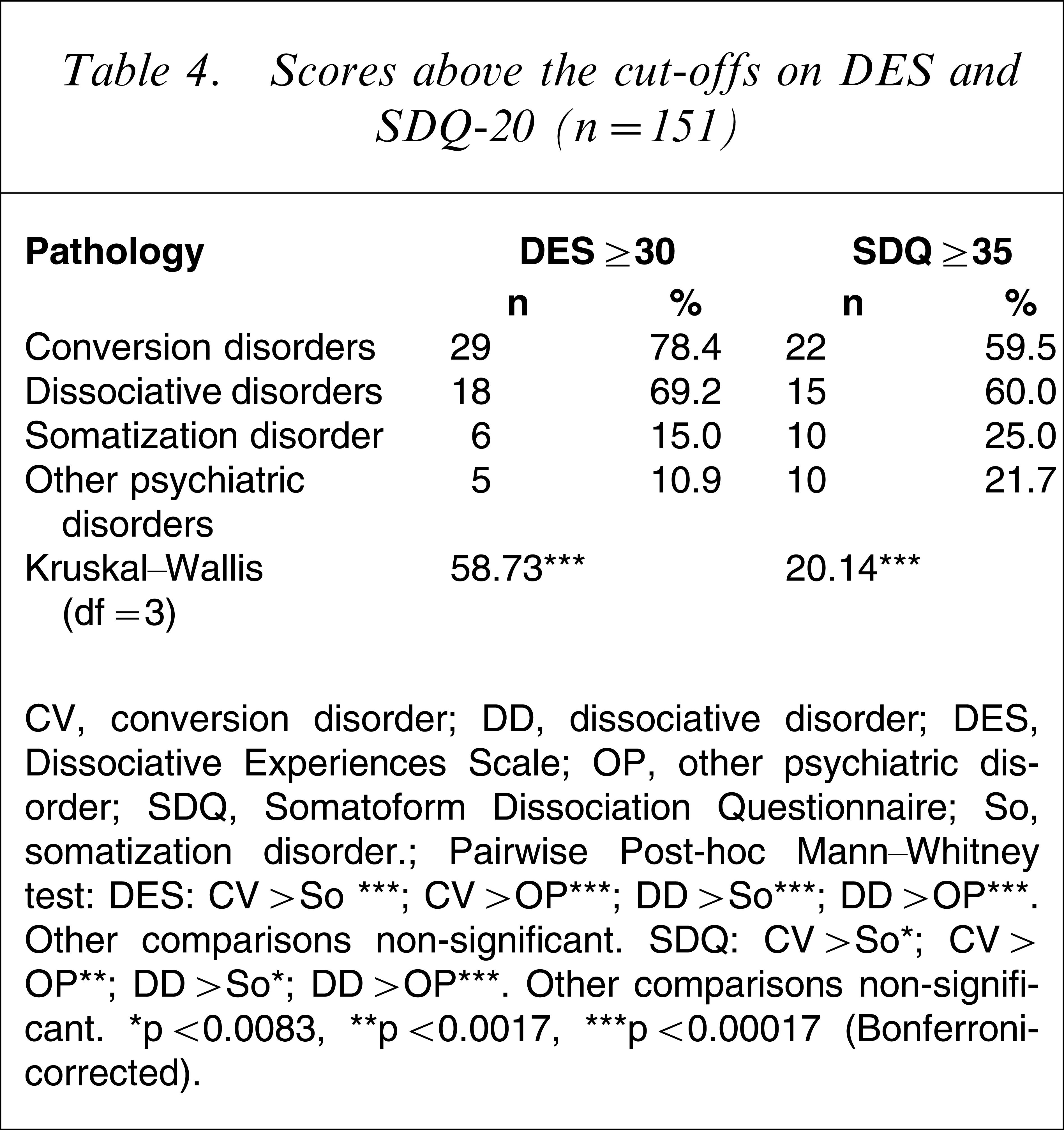
CV, conversion disorder; DD, dissociative disorder; DES, Dissociative Experiences Scale; OP, other psychiatric disorder; SDQ, Somatoform Dissociation Questionnaire; So, somatization disorder.
Pairwise Post-hoc Mann–Whitney test: DES: CV>So ∗∗∗; CV>OP∗∗∗; DD>So∗∗∗; DD>OP∗∗∗. Other comparisons non-significant. SDQ: CV>So∗; CV>OP∗∗; DD>So∗; DD>OP∗∗∗. Other comparisons non-significant.
∗p<0.0083, ∗∗p<0.0017, ∗∗∗p<0.00017 (Bonferroni-corrected).
Somatoform dissociation: SDQ
The SDQ ranged from 20.00 to 76.00 and had a mean±SD of 32.00±11.29 for all patients. Women scored 34.32±11.73 and men, 33.56±10.30, and their differences were not significant (U=2145.00, p=0.394); single patients scored 33.01±9.58 and married patients scored 35.67±13.34, and their difference was also non-significant (U=2453.00, p=0.465). Inpatients had significantly higher (U=1215.00, p=0.038) somatoform dissociation scores (mean±SD=39.15±14.21) than outpatients (mean±SD= 32.96±10.26). There was no significant correlation between scale scores and age (ρ=0.121, p=0.142). Less-educated subjects, however, had higher scores (ρ=−0.231, p=0.005). A score of ≥35 was attained by 38% of the patients.
Conversion patients also had higher mean±SD SDQ scores, followed by dissociative patients, then somatizing patients, and then other psychiatric patients. These scores differed significantly (H=20.46, df=3, p<0.001). The post-hoc Mann–Whitney tests indicated significant group differences between dissociative and somatizing patients, dissociative patients and controls, and between conversion patients and controls. Once again, dissociative and conversion patients did not differ from each other, nor did somatizing patients from controls. Conversion patients did not differ from somatizing patients (Table 3).
More conversion patients scored >35, followed by dissociative, then somatization and other psychiatric patients; these differences were significant (H=20.14, df=3, p<0.001; Table 4).
Psychopathology
The BSI data are presented in Table 3. The mean GSI scores were below the 1.7 threshold for the four groups. Conversion patients scored >1.7 in anxiety and obsessive–compulsive symptoms. Dissociative patients had higher levels in obsessive, depression and paranoid symptoms. Somatizing patients scored higher in somatization and obsessive symptoms. As a group, patients with other psychiatric disorders did not score high in any subscales. There were no significant differences between any paired groups in mean±SD GSI scores. We found significant differences only in somatization symptoms, with conversion patients and somatization patients having higher levels than patients with other psychiatric diagnoses.
Discussion
The aim of the present study was to analyse the relationship between conversion disorder, dissociative disorders and somatization disorder across the spectrums of psychoform dissociation, somatoform dissociation, and general psychopathology.
As far as we know, there is only one investigation that has compared conversion and somatization disorder with regard to psychoform dissociative symptoms, and that study reported no significant differences [21]; the present results do not support that study: the patients with conversion had higher scores.
We found no studies that compared dissociative and somatization disorder, considering psychoform dissociation. The present findings indicate that dissociative patients scored higher than the somatization subjects.
We also found that patients with conversion, and dissociative disorder patients differed significantly from somatization patients regarding somatoform dissociative symptoms; no other study measured this aspect.
The main finding was a closer association between conversion and dissociative disorders, than between conversion and somatization disorder. This result is supported by: (i) greater psychoform and somatoform dissociation in conversion and dissociation; (ii) a lack of differences between conversion and dissociative disorders using measures of psychoform dissociation, somatoform dissociation and general psychopathology; and (iii) differences between conversion and somatization disorder in psychoform but not somatoform dissociation. Additionally, there is a common element to the three groups of pathology, and this is the obsessive symptoms.
These are timely findings, considering the discussion regarding somatoform disorder classification. There are both practical [47, 48] and theoretical issues [49]. Some argue that conversion is misplaced in DSM-IV [6–8, 37] and should be reunited with dissociative disorders [6, 7, 22, 50–52] or that it definitely has a dissociative component [21, 23, 53]. We also propose that conversion is re-conceptualized as a particular type of dissociative disorder, with a somatization aspect. We suggest that psychoform and somatoform dissociation are specific mechanisms of dissociative and conversion disorders.
There were some limitations to the present study. Given the small sample size, it is possible that some statistically significant differences occurred by chance, thus the conclusions are limited to general trends, and larger replication studies are required.
Also, the demographics were disproportionate in relation to the population; despite the fact that we had no significant differences in the proportions of demographic characteristics across the four groups, this selection bias may limit the generalization of the study. We do know, however, that women are more likely to search for medical or psychological help [54], and are usually overrepresented in these studies. Moreover, men and women had no significant differences in mean DES or SDQ scores or in the proportion of higher scores. We are aware that younger subjects tend to report higher levels of psychological dissociation [34, 55–59] and somatoform dissociation [16, 60]. The same tendency occurs in less-educated subjects for somatoform dissociation [16, 60]. These possible selection biases were controlled: there was no correlation between age or number of school years and scores of the DES or SDQ, except for the proportion of patients with an elevated SDQ score, who were less educated. Thus, it is important to control the level of education in further studies. Some studies show a relationship between being single and psychological dissociation [57–59], and somatoform dissociation [57]. Again, there were no significant differences in mean DES or SDQ scores or in the proportion of higher scores between single and married subjects.
A potential bias may have occurred due to the self-report measures. It is possible that symptom exaggeration and contamination with social desirability took place, because we used the structured interview for only 62 subjects (41%). In addition, we recognize that individuals with psychiatric conditions may have a comorbid dissociative disorder that goes undiagnosed unless a structured interview takes place [61]. Moreover, we used wide psychiatric categories instead of specific diagnosis, which could introduce unmeasured confusion. And it has been demonstrated that conversion disorder could be a heterogeneous diagnostic category [62]. Additionally, the evaluators were not blind to the diagnosis. Therefore, a growing area for replication would be to use structured interviews combined with self-report measures, do more research on specific diseases, and involve blinded interviewers, unaware of the investigation hypothesis.
Despite these limitations, there were also strengths in the present study. The participants were inpatients and outpatients: knowing that inpatients are more likely to have psychiatric comorbidity, outpatients could have introduced fewer biases. We used, as well, a consecutive sampling procedure, which made the sample closer to a community sample. Finally, this study was the first to explore the three types of hysteria through psychological and somatoform dissociation.
