Abstract
Service in war zones is known to be associated with elevated levels of morbidity in the veterans of those deployments [1,2]. In Vietnam veterans, posttraumatic stress disorder (PTSD) has been a particular focus of attention because it can be directly attributed to combat exposure [3,4]. While morbidity effects of war service have been identified in many studies, there has been little systematic work to identify the associated health-care costs.
One approach to estimating the full cost of healthcare consumption is to use self-report data and examine reported health-care consumption in relation to various health and psychosocial factors [5]. An earlier analysis of self-reported health-care consumption focused on PTSD as a particular issue among veterans. Posttraumatic stress disorder was found to be a major predictor of total self-reported health-care consumption, along with depression and other mental health problems. Other psychosocial factors that were found to be associated with healthcare consumption included perceived social support and stressful experiences during the veterans' Vietnam deployment [6].
The self-reported health-care consumption measure used a short reference period (2 weeks). This was chosen to minimise recall bias and maximise recalled detail of the health services used [5]. However, there was some concern that the short reporting period may have given a distorted picture of longer-term service use. For this reason, data were sought on health-care consumption over a longer period. An approach was suggested by a limited amount of previous studies of survey samples [7,8] which drew on records of the Department of Veterans' Affairs (DVA) and/or the Health Insurance Commission (HIC) to examine actual medical service utilisation. A readily available indicator of actual service utilisation is the cost of services used and paid for through Medicare and DVA benefits.
The DVA and HIC agreed to provide assistance in extracting data on benefits paid for subjects in the epidemiological study of Vietnam veterans reported previously [6]. The HIC data was limited to only medical services used by the veterans. While the DVA data represented all services provided by DVA to entitled veterans, they did not account for all services used by these veteran subjects, as some were only partially entitled or not entitled to DVA-funded services for all their healthcare. Therefore, by combining DVA and HIC data it was possible to cover all medical services for which payments had been made. Non-medical health-care services were not available.
It was hypothesised that medical-care cost would increase with age and with more physical and mental health problems, including PTSD in particular. It was also hypothesised that certain aspects of service in Vietnam would predict increased medical-care cost with health status and age controlled.
Method
The subjects examined in this study were 641 Vietnam veterans interviewed from a random sample of 1000 veterans. Of the 1000 subjects sampled, 213 could not be found, 50 were known to have died, 61 refused interview, and 35 were unable to be interviewed in the time available [9]. The Australian Natural University Ethics in Human Experimentation Committee approved the extended study.
Measures
The data used in the analyses for the veteran subjects came from health and psychological state questionnaires and the veterans' army personnel files and psychological records. The DVA and HIC extracted administrative data on the subjects according to an agreed protocol that protected subjects' privacy during data linkage and produced a de-identified, linked data set as the final product of the matching and extraction algorithm.
Initially, 4 years of records were extracted and only 40 of the 641 subjects interviewed had no records retrieved of benefits payment. The most likely explanation for these subjects is that most were non-users of medical consultation services during this period. Alternatively, some may not have been correctly identified in the HIC and DVA client indexes.
Dependent variable
The DVA and HIC data were merged. Benefits paid by DVA for other than medical services were then removed. The medical-care utilisation records for each subject were selected from 6 months before to 6 months after the assessment interview. Medical-care costs were summed to produce a value for the total medical-care cost in the 12-month period surrounding the interview for each subject.
Predictor variables
The selected predictor variables were examined in seven blocks of related measures listed in Table 1. The variables were selected to minimise collinearity while still representing all of the predictor factors of interest as far as possible. However, there inevitably remained some correlation between some pairs of measures, even though each represented important separate, but related, constructs. Examples are PTSD, ‘often thinking about Vietnam’, anxiety and depression. For this reason, groups of variables were also examined as blocks of factors.
List of variables examined as predictors of medical-care utilisation cost
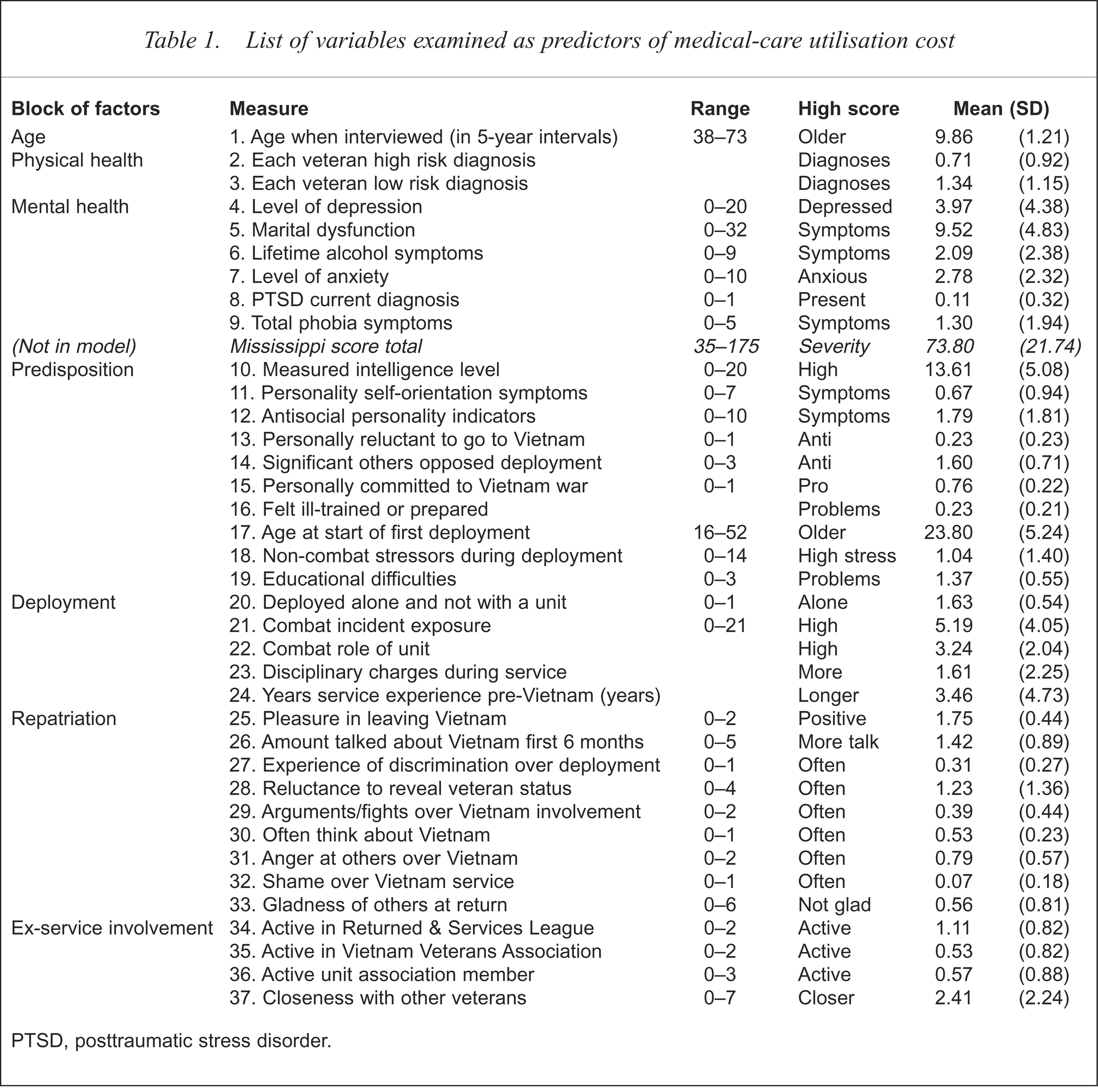
PTSD, posttraumatic stress disorder.
Age (measured in 5-year steps) at time of interview was included as a predictor factor within the model, because age is a known predictor of health-service use [10–12].
Physical health was indicated by the number of diagnoses reported in the survey, excluding mental health conditions. Diagnoses were divided between two variables: conditions that occur more frequently in veterans and those that do not [13].
Mental health (six variables) was measured by a detailed structured interview for PTSD [14] that had been adapted for use with Australian veterans (AUSCID-V) [9]. We also used the National Institute of Health Diagnostic Interview Schedule [15] and self-completion questionnaires including the Mississippi PTSD scale [16], the 28-item General Health Questionnaire [17], the Army Self Description Inventory (SDI) [18], the Center for Epidemiologic Studies Depression Scale (CES-D) [19], the Spielberger Trait Anxiety Inventory (STAI) [20] and the Spanier Dyadic Adjustment Scale [21].
Predisposition (10 variables) or pre-existing risk indicator variables were selected to measure: (i) personality attributes and attitudes prior and during the veterans' deployment which could make them vulnerable to stress related disorder or physical injury; and (ii) interpersonal or social circumstances that could add to the stress of deployment or reduce their coping resources.
Demographic and historical health and psychosocial data were obtained from Army health and personnel records. Self-completed questionnaires provided retrospective information on military service experiences and postservice adjustment issues.
Deployment (five variables) encompassed the sorts of exposure to health risks the soldier had leading up to and during deployment and how they reacted to those experiences. Combat exposure was measured with a 21-item questionnaire developed by Wilson and Krauss [22], administered during the AUSCID interview.
Repatriation (nine variables) related to the quality of the veterans' homecoming and repatriation after their deployment. It included variables relating to the veterans' attitudes and adjustment during repatriation. These factors were measured by subjects' self-report of: (i) how well they were supported and received; (ii) the opportunities that they had to readjust; and (iii) whether they saw their deployment as having been a positive contributor to their personal status and achievements.
Ex-service involvement (four variables) included membership of ex-service associations and involvement with other veterans. This is often suggested as being a major contributor to veterans' health-care consumption through additional use of DVA services.
Analyses
A univariate linear regression approach was taken first in examining the relationship between the individual predictor variables and medical-care cost. The unstandardised coefficients generated by these regression analyses could then be interpreted as dollars of medical-care costs per year associated with a unit increase in the predictor factor concerned. This was measured first individually for each factor and then with selected blocks of other factors held constant.
As the analysis focused on the relationship of PTSD and medical-care cost, those blocks of variables which had common causal pathways with PTSD (the Vietnam experience and veteran status), were not added to models until after the relationship between PTSD and medical-care cost had been explored. Age and physical conditions, which were hypothesised to have a largely independent association with health-care cost, were fitted first to the multivariate models so that the relationship between PTSD and medical-care cost could be identified with age and physical health controlled.
When examining variables individually and with blocks of other predictor factors controlled, four models were used.
All 37 variables were first examined individually (Model 1). This enabled the relationship between medical-care cost and PTSD to be identified with all other variables free to covary.
The relationship of each variable to medical-care cost was also examined after controlling for age and physical health (Model 2).
The variables in the last four blocks representing risk factors in the areas of predisposition, deployment and repatriation social support were then fitted to the model with age, physical health and mental health controlled (Model 3). This enabled any relationship between health-care consumption and the predisposition, deployment and repatriation variables to be examined with the physical and mental health variables controlled.
All 37 variables selected to provide a balance between comprehensive concept representation and minimum collinearity were then fitted to the regression model (Model 4). This enabled measurement of the variance of the model with all blocks of variables fitted.
In relation to the aim of this study, the model of major interest in these analyses is Model 2 with PTSD fitted, and age and physical health controlled. In this way, costs associated with PTSD free of correlated physical illness could be examined.
The R2 statistic was used to measure the variance of each block and is reported here with all fitted to the model.
Results
The mean medical-care cost of the whole sample (n = 641) for the 12-month period was $226. No medical-care costs were incurred by 128 (20%) of the subjects and the 30 (4.7%) highest-cost subjects accounted for $54 434 (38%) of the $144 764 total medical-care costs for all the subjects. For the 73 subjects with a current diagnosis of PTSD, the mean medical-care cost was $356. Of these subjects, 10 (13.7%) incurred no medical-care costs.
The Model 1 column of Table 2 shows the relationship of each predictor variable and medical cost with other factors left to covary. Age was found to be a strong predictor of medical-care cost. Each five-year increase in age was associated with increased medical-care cost of $47 per annum (p < 0.001). This effect was even greater once other variables were controlled (Model 4), with each five-year age group increasing medical benefits payments by $137 per year (p < 0.001). In the area of physical health, each physical diagnosis was associated with an increase in health-care cost: $112 per year for diagnoses that are more common in veterans (p < 0.001) and $81 per year for diagnoses not more common in veterans (p < 0.001). This relationship persisted when other variables were controlled.
Results of regression models examining 37 variables individually and fitted together as predictors of medical-care cost in Vietnam veterans
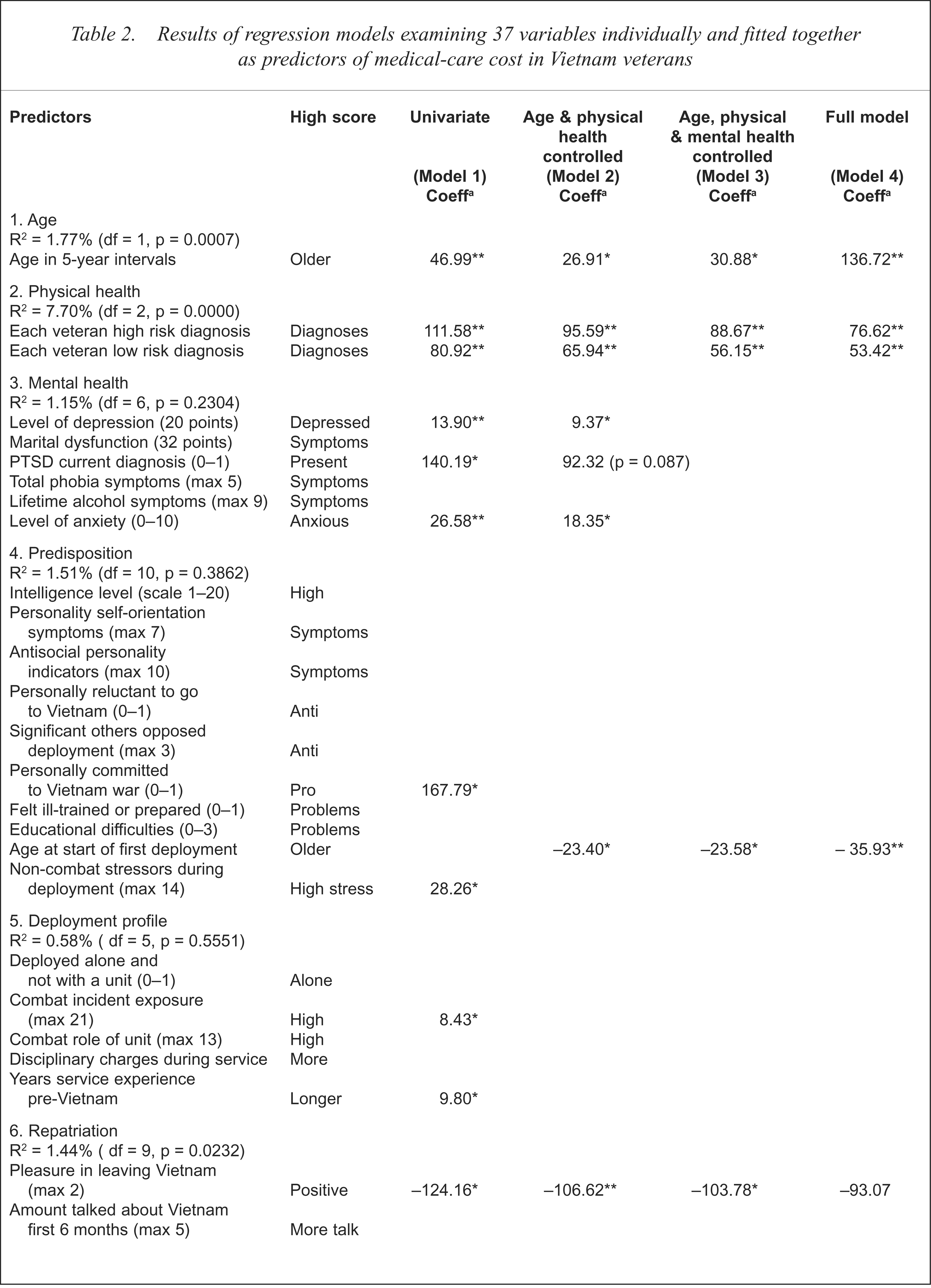
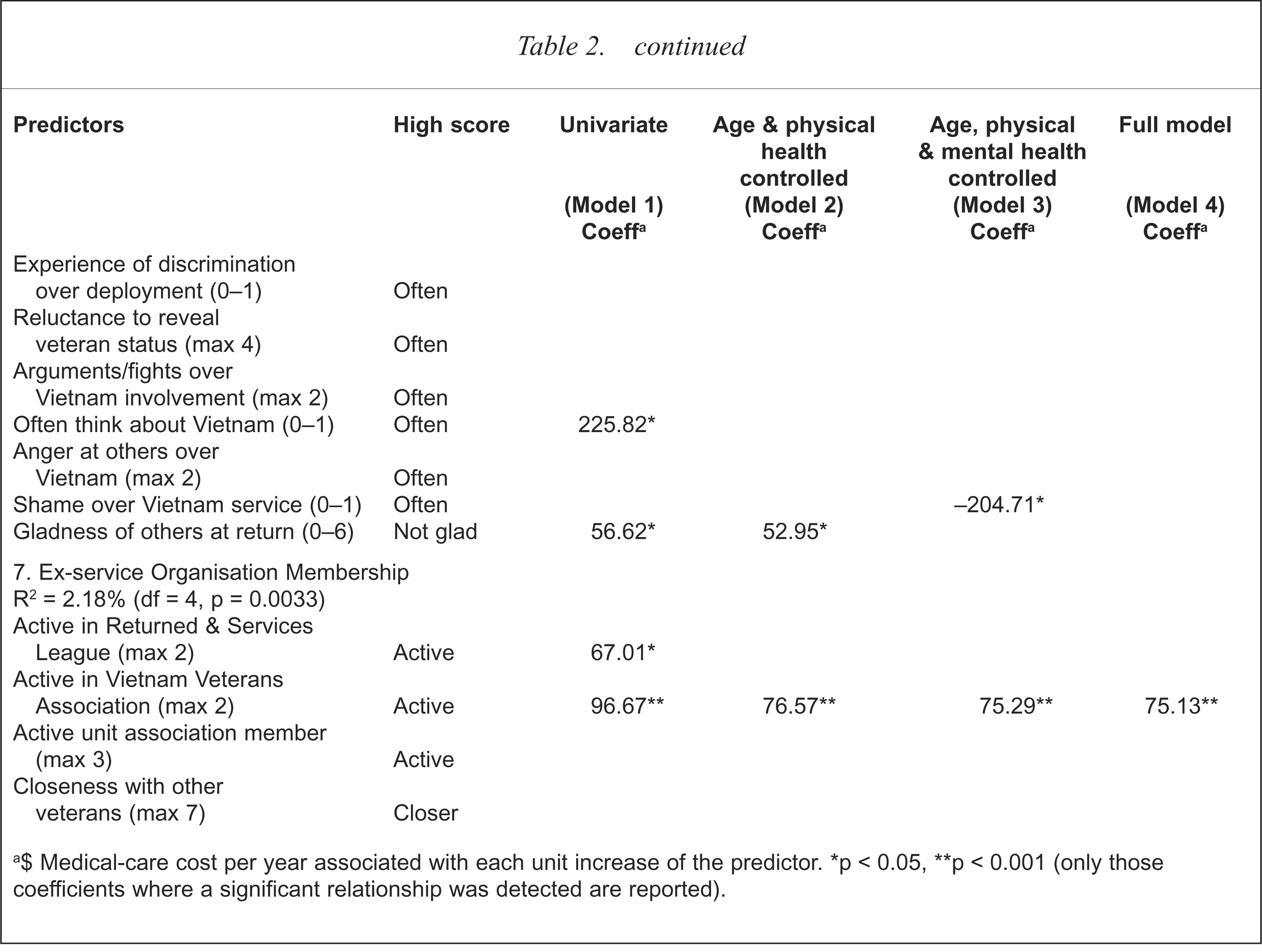
Of the mental health variables, a diagnosis of PTSD was found to have a major association with medical-care cost ($140 per year, p < 0.05). Although it did not achieve significance once age and physical health were controlled (Model 2, $92.32 per year, p = 0.087), the coefficient was reduced as in the self-report study where a significant relationship did persist with age and physical health controlled [6]. The failure to retain statistical significance with the sparser medical-care cost data in this study was probably due to the conservative nature of the diagnostic criteria used as the measure of PTSD in this model. (A one-tailed statistical standard could be applied in this context as it is not really conceivable that a positive diagnosis could reduce medical costs. This would see the relationship judged statistically significant). This relationship was also tested by substituting the Mississippi PTSD symptom score as the PTSD measure and a significant relationship with actual medical-care cost was observed. Each point of the (35–175) Mississippi scale predicted an increase in medical-care cost of $1.90 per year (p < 0.05) after controlling for age and physical health measures.
Loss of significance of PTSD as a predictor of medical-care cost once other mental health problems were controlled (Model 3) may be associated with the high degree of covariance between these diagnoses. This would be consistent with the findings of Grayson et al. [23] indicating the same sort of relationship between combat and depression, anxiety and other mental health disorders, as that observed for PTSD. The Mississippi score was, in fact, moderately correlated with CES-D (0.606, p < 0.001) and STAI anxiety (0.732, p < 0.001).
Other major mental health problems that we found to be strongly related to medical-care cost were depression and anxiety symptoms. Each point in the 0–20 scale derived from the CES-D score was associated with an increased medical-care cost of $14 per annum (p < 0.001). Each point on the 0–10 scale derived from the STAI anxiety score was associated with an increased medical-care cost of $27 per year (p < 0.001). An important finding was the lack of association between a history of alcohol abuse and medical-care costs. This was also consistent with the finding for self-reported total health-care consumption cost [6].
Other factors
Of the predisposition factors, the only predeployment characteristic found to be associated with increased medical-care cost was the veteran's propensity to be a supporter of the war effort ($168 per annum more medical care, p < 0.05). However, this relationship lost statistical significance when age and physical health were controlled. Veterans who were older at the start of their first tour were found to consume less medical care once current age, physical and mental health and other factors in the model were controlled. This is a strong relationship, with each year of age at the start of the first tour being associated with $36 per year less medical-care cost after all other variables of interest were controlled (p < 0.001).
From the block of variables covering deployment profile, the combat index was found to predict higher cost of medical care ($8.43 per year for each point on the 21-item scale, p < 0.05). Time in the Army prior to Vietnam also predicted higher use of medical care ($9.80 per year, p < 0.05). However, these relationships were not so strong after current age and physical health were controlled.
Of the repatriation variables, a positive attitude to coming home reduced use of medical care by $124 per annum for each point on the 0–2 index (p < 0.05). After controlling for other factors (Model 4), this relationship remained significant with each point being associated with a $93 per year reduction in medical-care cost (p < 0.05). Thinking often about Vietnam was associated with an additional medical-care cost of $225 per year (p < 0.001). The veteran's feeling ashamed of his Vietnam service became associated with a significantly lower cost of medical care (lower by $205 per year, p < 0.05) after age, physical and mental health were controlled (Model 3).
As in the analysis of the self-report data, perceived lack of gladness of other people towards their return was also a predictor of increased health-care consumption cost. However, in contrast to this association with total health-care consumption, identified previously [6], the relationship of this variable with medical-care cost disappeared once age, physical and mental health were controlled.
Among the factors covering ex-service organisation membership, the strongest association was found to be with membership of the Vietnam Veterans Association (VVAA). Even after all other variables were controlled, membership of the VVAA was found to be associated with additional medical-care cost of $75 per year for each point on the 0–2 scale (p < 0.001).
Variance analysis of blocks of factors
With all blocks fitted to the model, the major contributor to the R2 for the model was the physical health indicator block, basically consisting of the number of diagnoses for physical illness reported (R2 change = 7.7%, df = 2, p < 0.001). Age added a further 1.8% (df = 1, p < 0.001), the repatriation block 1.4% (df = 9, p < 0.05) and ex-service organisation membership 2.2% (df = 4, p < 0.05).
Discussion
There were two major areas of outcome for this study. First, predictors of medical-care utilisation costs over a period of a year were determined using ‘hard data’ rather than self-report of health-care consumption. Second, the match extraction of the subjects' medical-care cost data replicated the success of other recent studies in demonstrating reliable retrieval of these data [7,8].
The relationship between PTSD and medical-care cost is the important finding of this study. These findings on PTSD are useful because they are linked to a clinically diagnosable level of PTSD using clearly defined symptom probes [14]. The relationship between diagnosed PTSD and medical-care cost was statistically weaker after physical health measures were controlled. However, when the (more sensitive and less conservative) Mississippi measure of PTSD symptomatology was used [16], the strong relationship between medical-care cost and PTSD symptomatology remained, even after controlling for the effects of age and physical health.
Therefore, the effect observed in Model 2 was consistent with a utilisation pattern where a proportion of the medical-care cost associated with PTSD may have been related to additional physical diagnoses in those patients with PTSD [6]. This is compatible with theories of somatisation [24–26] or alternative causal pathways. Under this circumstance, controlling for the effects of physical health, and similarly age, could be regarded as a very conservative approach. If PTSD was causally implicated in poor physical health or had a natural progression with age, this analytic strategy would overcontrol for these variables and remove a real effect of PTSD.
The relationship between mental health factors including PTSD and medical-care cost also overlapped with the predisposition, deployment and repatriation blocks of factors. This is not surprising, as many of these are known moderators or behavioural consequences of PTSD symptom patterns. For example, fights over the topic of Vietnam and perceived discrimination over Vietnam status may be related to hyperarousal symptoms in PTSD patients; often thinking about Vietnam could be a manifestation of intrusion symptoms in PTSD patients.
Whatever the causal pathway that generates the relationship between PTSD and medical-care cost observed in Model 1, the attribution required by DSM-IV diagnostic criterion A for PTSD [4] links it (and its associated effects) to these veterans' deployment. On that basis alone, it warrants serious attention.
Other predictors
As expected, it was found that current age and physical health (diagnosed illnesses) were strong predictors of medical-care cost. As single variables, a number of mental health problems were also predictors of medical-care cost.
Veterans who were younger at deployment tended to be higher consumers of medical care, as were those with higher levels of combat exposure and longer time in the Army prior to deployment. The relationship with age at deployment was strengthened in the full regression model, suggesting a real propensity for those who were young at deployment to use more medical care even after other health and social factors are controlled.
Repatriation factors associated with higher medical-care cost were self-perceived negative homecoming experience and membership of ex-service organisations. However, these relationships disappeared after age and physical health effects were controlled, suggesting that, as with PTSD, repatriation factors may also have been largely related to medical-care costs via presenting physical symptoms.
A feeling of shame over Vietnam service was associated with reduced medical-care cost once other health and psychosocial factors were controlled. This association is consistent with veterans avoiding visits to their medical practitioner because of a reluctance to reveal their veteran status.
The lack of relationship between alcohol abuse and health-care consumption that was observed with the self-report consumption data [6] was also found with this medical-care cost data that covered a 12-month period. A study of a New Zealand population sample found similar results [27]. This remains a surprising finding, as previous research with clinical samples found that alcohol was associated with significant health-care costs [28]. Other recent studies on this topic [29,30] relate to costs associated with treatment of alcohol abuse or costs of treating alcohol-related trauma. Our findings do not dispute that large costs are incurred treating people for alcohol abuse or alcohol-related problems. However, such effects may not be evident in a population sample.
The variance explained by the mental health block was lower when other factors were controlled in the full model. This effect is again consistent, with much of the medical-care utilisation associated with mental health factors being also associated with increased physical diagnoses and behavioural factors. Overall, the size of the variance explained by this model is consistent with that obtained in larger studies of utilisation costs [31,32].
The match-extraction of the records on benefits paid to this sample of subjects who had been randomly selected from the community was apparently very successful. Records were found for the majority of cases. The location of records is consistent with levels found in earlier studies of this type [7,8].
Implications
Posttraumatic stress disorder was found to be associated with substantial medical costs, 60% higher than average. A large proportion of those costs may not be obvious, as they appear to relate to treatment for physical health problems. When we add to healthcare costs of PTSD the economic and personal costs that must be associated with such pathology, the potential rewards for effective prevention and treatment programs for PTSD are better understood.
Further studies that are prompted by the findings in this study include further investigations of the relationship between PTSD, anxiety and depression; the causal relationship between physical health problems and PTSD; and the interrelationship between PTSD, lifestyle and medical-care utilisation. The validity of self-report for estimating both cost of health care consumed and the predictor factors requires further examination and this will be taken up in detail in a separate report.
Acknowledgements
A Commonwealth Department of Health and Family Services Casemix Education and Study Grant supported the study. The earlier data collection was supported by grants from the National Health and Medical Research Council, Public Health Research and Development Committee, the Australian Vietnam War Veterans Trust, the Department of Veterans' Affairs, the Westmead Research Institute and the Australian War Memorial. Assistance from Department of Defence (Army), Canberra with facilities and support for data extraction and analysis is particularly appreciated. The findings and views expressed in this report are those of the authors and are not to be taken as the official opinion of the Department of Defence or the Department of Veterans' Affairs.
