Abstract
Isotretinoin (trade names Roaccutane and Oratane) or 13-cis-retinoic acid is a vitamin A derivative. Since its introduction in 1982, it has been approved for the treatment of nodular and cystic acne; a severe, scarring form of acne usually refractory to conventional therapies. Increasingly, it is being prescribed for less severe acne that is unresponsive to antibiotics. It is available in about 80 countries and has been used by over 8 million people worldwide [1]. Having an efficacy rate of more than 75% (often with complete remission) [2, 3], the drug works by reducing sebum production by sebaceous glands in the skin. Isotretinoin is teratogenic and therefore contraindicated in pregnancy, and can have other side-effects including dry skin, photosensitivity, lethargy, and abnormal liver and lipid functions [4–6].
Although a possible association between isotretinoin and depression has been known for at least 15 years, it has received scant attention in the psychiatric literature and is not well recognized by psychiatrists. In Australia, because of regulatory restrictions, isotretinoin is predominantly prescribed by dermatologists for severe cystic acne unresponsive to conventional therapy (this is the only clinical indication for the Pharmaceutical Benefits Scheme). Dermatologists are probably more aware of this potential side-effect but may not adequately screen acne patients for depressive symptoms in part because patients are unlikely to present such symptoms to them. Depression has been listed as an adverse effect on the drug label since its release. However, numerous reports linking the risk of depression and other psychiatric effects with isotretinoin has led to much recent media publicity. In 1998, the manufacturer upgraded the warnings in conjunction with The Food and Drug Administration (FDA) that isotretinoin may cause depression, psychosis and rarely suicidal ideation, suicide attempts and suicide [7].
This paper aims to provide a review of the literature published in English pertaining to the issue of depression in patients with acne who have been treated with isotretinoin, accessed through computerized databases (MEDLINE and PubMed) and other relevant data available to the authors. Overall, the available data is limited but has been categorized into case reports, review studies and systematic studies. This article further explores the psychosocial effects of acne and the methodological issues in clarifying the relationship between depression and isotretinoin. The possible predictive factors and clinical implications are also outlined.
Case reports
Acute depressive symptoms during isotretinoin treatment have been reported in patients with no past or family history of depression. Byrne and Hnatko [8] reported cases of two females and one male who developed severe depression during isotretinoin therapy and who responded with antidepressant treatment. Case descriptions of psychiatric disturbance with depressive symptoms in two patients using isotretinoin were also reported by Duke and Guenther [9]. Concerns have been raised about suicidal behaviour that has been linked to isotretinoin use involving young patients. Bravard et al. [10] described two young males, one who had attempted suicide and another who completed suicide, both of whom were associated with isotretinoin. Another case involving a young man who committed suicide after receiving 4 months of successful acne treatment was reported by Gatti and Serri [11].
A case of a 17-year-old male with acne vulgaris who developed acute depression 2 weeks after beginning isotretinoin was reported by Ng et al. [12]. Although antidepressant treatment was initially effective, the depression recurred despite skin improvement when the isotretinoin dose was increased, leading to a suicide attempt. The depressive symptoms quickly resolved when isotretinoin was discontinued. The FDA has reported 24 cases where depression resolved once isotretinoin was ceased but recurred when treatment was reintroduced [13]. Therefore, anecdotal evidence of depression being causally related to isotretinoin treatment consists of the following cases: depression developing soon after the commencement of treatment with isotretinoin; depression resolving only after drug discontinuation; and depression recurring following drug rechallenge [12–14].
Reviews
Hazen et al. [15] found depressive symptoms in six out of 110 patients treated with isotretinoin at doses between 1 and 2 mg/kg/day. Only one patient had a history of depression, and all six patients improved rapidly after stopping isotretinoin. Another study reported spontaneous depression occurring in 1% of 700 patients with cystic acne, psoriasis and other dermatological disorders participating in a clinical trial with isotretinoin [14]. The depression was unrelated to dosage (range of 0.3–1.3 mg/kg/day), duration of use or prior exposure to isotretinoin. The depressive symptoms resolved rapidly within 2–7 days after discontinuation of therapy. The authors suggested that depression is likely to be an idiosyncratic adverse effect of isotretinoin therapy. One study that evaluated the long-term safety of isotretinoin in 720 patients for up to 12 years, found persistent depression in only three patients. These patients also had dysmorphophobia and the authors concluded the depression was probably not drug related [16]. It is likely, however, that the patients who developed depressive symptoms early on in the study were excluded from the long-term arm.
From 1985 to 1998, the Adverse Drug Reactions Advisory Committee received at least 12 reports of depression related to isotretinoin in Australia [17]. Information received from the Roche Drug Safety Database (1998) stated that there had been 526 reports of depression worldwide between 1982 and 1997 of which there were six cases of suicide. About 50% of these cases had medical comorbidity, or a past or family history of depression.
The FDA has received 431 reports of depression, suicidal ideation, suicidal attempts and suicides in patients treated with isotretinoin between 1982 and 2000 in the US[18]. There were 37 suicides and 110 patients hospitalized for depression, of which a past history of psychiatric illness was reported for 22% and 44% of the patient group, respectively. Psychosocial stressors, alcohol use and other contributing factors were also identified in 57% and 52% in the respective groups. Of particular concern is that isotretinoin is ranked 4th, 5th and 10th in the FDA's database with the most reports of depression, serious depression and suicide attempts, respectively. Isotretinoin was also the only non-psychotropic medication in the top 10 ranked drugs for suicide attempts. Although such data could suggest a potential causal link, the authors stated that increased reporting since the change in product label warning and the relationship between severe acne and depression were possible reasons for the high frequency of reports.
Psychosocial effects of acne
Any attempts to tease out the association between isotretinoin and depression is complicated by the confounding psychosocial effects of acne. Severe acne, especially in adolescents and young adults, has been associated with a variety of psychological consequences. This includes depression, anxiety, low self-esteem, body image problems, self-consciousness, lack of selfconfidence and anger [19–21]. Severe acne can have a negative impact on self-image, psychological development and social interaction, leading to poor quality of life and even suicides [22]. The severity of the psychological distress appears to correlate with the patients’ rating of acne severity [21, 23].
It is therefore likely that effective acne treatment can have a positive psychological outcome. Studies have shown that clinical improvement in acne following successful treatment with isotretinoin is associated with decreased anxiety and depression [24–27]. Not surprisingly, the reductions in the level of anxiety and depression were most obvious in those with greatest skin improvement. It should be noted that these studies had small sample sizes and no control group. Due to the relationship between isotretinoin and depression some physicians may be reluctant to prescribe isotretinoin in patients with a history of depression or depressive symptoms. Therefore, a dilemma exists when depressed patients who are disfigured by their acne are deprived of an effective acne therapy that may improve their negative self-image. The risk of depression associated with isotretinoin therapy has to be balanced with the psychological gains of effective treatment.
A further important psychological issue pertains to some patients’ unrealistic and excessive expectations following acne treatment; these patients believe that the clearing of the disfiguring skin condition will resolve their personal and social inadequacies [28]. Such unfulfilled hopes may heighten their sense of failure, previously attributed to the acne and precipitate an emotional crisis or depression.
Systematic studies
In a prospective evaluation of the side-effect profile of isotretinoin using questionnaires in 124 patients treated over 4 months, the incidence of self-reported depression was 4%. No psychometric measure was used to assess depression severity. The depressive symptoms persisted throughout treatment course but did not lead to any treatment withdrawal [6].
A retrospective cohort epidemiological study of 7535 isotretinoin users from the Canadian Saskatchewan Health Database and the UK General Practice Research Database found no increase in relative risk estimates for depression, psychotic symptoms, suicide and attempted suicide [29]. However, this industry-sponsored study, which aimed to clarify the association between isotretinoin and risk of depression, had significant methodological limitations that prevented any conclusive findings [12, 30]. These included the retrospective study design; inadequate data on suicides or acne severity; uncertain validity of diagnostic information and case recognition from the use of a computerized database; and a lack of data on treatment parameters.
Ng et al. [31] conducted a prospective study to evaluate depressive symptoms and quality of life in patients with acne vulgaris treated with oral isotretinoin compared to those treated with antibiotics/topical treatments over 6 months. Depression, quality of life and acne severity measures were rated in 215 patients (mean age 20). Patients with significant medical comorbidity were excluded and only 3 patients reported a past history of depression. Mood ratings (using Beck Depression Inventory) tended to improve over the course of treatment and there were no significant differences in the level of depressive symptoms found between the isotretinoin and antibiotics/topical treatment groups. The incidence of isotretinoin patients with moderate depressive symptoms appeared less than the comparator group and was relatively unchanged over the treatment course. Although the study results did not support a link between depression and isotretinoin treatment, five patients out of 174 with no previous history of depression were withdrawn from the study due to a worsening of mood while on isotretinoin. The depressive symptoms were possibly related to isotretinoin in only two (1.1%) of these patients, but were not drug related in the other three patients who had coexisting psychosocial stressors. The authors concluded that depression is an uncommon and unpredictable idiosyncratic side-effect but due to the limitation of low numbers, a larger study was recommended to confirm its findings. Cases of depression may be too scarce to show any significant differences in small systematic studies [12].
Methodological issues
The current literature on the association between depression and isotretinoin has a number of significant weaknesses apart from the dearth of systematic studies. These include the absence of prospective randomized controlled studies, small sample sizes and the limited data on clinical parameters. However, the available information from the challenge/rechallenge data and the adverse event reporting database in the US since 1982 suggests a possible signal of causality that warrants additional studies. Several important methodological issues outlined below, not least the psychosocial effects of acne itself would need to be addressed in future systematic studies.
Many clinical variables may influence depression, including duration of acne, presence of acne scarring, past response to treatment, subjective perception of severity, various psychological attributes and a past history of depression. The lack of controlled population based studies may be explained by the difficulty and necessity to control as many of these clinical variables as possible to determine if depression is a treatment effect. This essentially means comparing a group of patients using isotretinoin with a similar control group given either a placebo or comparable treatment. A controlled randomized study design would also avoid bias in sampling and ratings of outcome measures. However, isotretinoin prescription is only limited to well-defined clinical indications such as nodulocystic acne resistant to conventional antibiotic therapy. Subjecting these patients to a randomized trial for a usual 6 months course would not be ethically appropriate as they would be deprived of isotretinoin even after they had previously failed antibiotic/topical therapy.
Another major confounding variable in clarifying the association between isotretinoin and depression is the group of patients afflicted by nodulocystic acne for which isotretinoin is used. These are mainly adolescents and young adults with severe acne who may already be predisposed to developing depression. The uncertain prevalence of depression in acne patients in the community would limit studies evaluating the relationship between drug treatment and depression. Studies would need to assess if the incidence of depression with isotretinoin is greater than the background rate of occurrence from other contributing factors [7]. Given the low frequency of such cases, a sufficiently large sample size would be required in order to find a real treatment effect. In addition, studies investigating the incidence of drugrelated depression are likely to be complicated by the issue of case identification. Acne improvement during isotretinoin treatment may lower the depression levels in patients with depressive symptoms before treatment entry [25], leading to a reduction in ‘cases’ of depression. Thus, no change in the incidence of depression may still reflect a relative increase.
The number of reported cases of isotretinoin related depression and suicides in acne patients in the US still appears considerably lower than the predicted rates of depression and suicides based on the community prevalence of depression and the estimated number of isotretinoin users [18, 32]. In a recent Australian population mental health survey, the 12-month prevalence of depression was 5.8% [33] while another populationbased study of adolescent depression found a rate of 3.5% [34]. The frequency of depression associated with isotretinoin use reported in several studies [6, 14, 18, 31] does not seem to exceed the rates of depression in the general population. This suggests that depression emerging during isotretinoin use may still be due to coincidental risk factors.
Animal studies have indicated that retinoids cross into the central nervous system and their receptors are found in the brain. They may alter neuronal pathways, such as dopamine signalling, which are known to be involved in mood and cognitive disorders [35]. Crying spells, irritability, agitation, malaise and headache can be produced by benign intracranial hypertension related to hypervitaminosis A associated with retinoids [8, 14, 36, 37]. The similarities to these neuropsychiatric symptoms have been postulated as possible mechanisms involved in isotretinoin induced depression, but have not been proven. There are no cases of depression with documented intracranial hypertension [14] nor is there evidence that isotretinoin treatment leads to hypervitaminosis A [38]. Although the relationship between systemic retinoids and depression may be plausible in neurobiological terms, the aetiological mechanisms remain unknown.
Predictive factors
Presently, it is not possible to predict the patients who may develop depression with isotretinoin therapy. Apart from a past history of depression with isotretinoin challenge and positive dechallenge, other risk factors have not been clearly identified. Byrne et al. [38] have noted that severe depression tends to occur particularly in young patients. According to case reports, there is a wide variation in the onset of depression, ranging from as brief as two weeks of treatment [12] to 10 months after stopping isotretinoin [38]. Some of the possible predictive factors were examined in the prospective study described by Ng et al. [31]. Only a weak correlation between severity of acne and depression was shown in the study. A few case studies suggest a dose dependent effect on mood [12, 14], but the study failed to find any correlation between drug dosage and depression. There is also lack of evidence that depressive symptoms prior to commencing isotretinoin are a risk factor. At baseline, 14 patients (8.0%) from the isotretinoin group had a moderate level of depressive symptoms. In this subgroup of patients with pretreatment depressive symptoms, isotretinoin had a positive effect on mood as a result of skin improvement following treatment [31].
The risk for the few patients vulnerable to developing depression with isotretinoin is likely to be multifactorial. Whether depression is related to the drug, or the psychological sequelae of severe acne, or a combination of both with other mediating psychosocial stressors has not been elucidated. The role of isotretinoin is likely to differ from one case to the next. Further studies controlling for the effects of acne and confounding risk factors are required to determine whether there is a causal relationship between isotretinoin and some cases of depression.
Clinical implications
The evidence from the data in this review suggests that depression may be rarely induced by isotretinoin in certain predisposed patients, perhaps occurring at a rate of 1% or less. The risk of depression, however, appears more likely to arise from having severe acne or a past history of depression or other psychosocial factors, than from the drug itself. Pre-existing depression does not necessarily preclude the use of isotretinoin because effective acne treatment may actually improve depressive and anxiety symptoms. In any case, depression that occurs with isotretinoin challenge or rechallenge and resolves with drug withdrawal is strongly suggestive of a causal relationship. Such drug-induced depressive illness, particularly in younger patients, can be severe and may represent a suicide risk [10–12].
A clinical approach to management of depression associated with isotretinoin use in acne is presented in Figure 1. Although we are not able to predict the occurrence of this adverse effect, physicians should assess the risk factors of depression, including relevant past history prior to prescribing isotretinoin. They should adequately inform patients and families about the possibility of depression and ask them to report depressive symptoms without delay [32]. Regular and careful patient assessment for symptoms of depression is also desirable. Screening instruments like the Beck Depression Inventory may be useful in clinical settings [31]. Depressive symptoms that develop during the treatment course will require close monitoring, especially for suicide risk. If indicated, prompt psychiatric assessment and care will be required. Significant depression may necessitate both the discontinuation of the drug and evaluation for antidepressant therapy [12]. Resolution of depression associated with isotretinoin appears to be rapid and complete with treatment. Although no doseeffect relationship has been consistently shown, it would be prudent to use a low dose in the event of drug continuation or rechallenge. Psychological factors need to be considered in those with coincidental psychosocial stressors or unrealistic expectations of resolving their personal and social problems with skin improvement [11, 28].
A clinical approach to the management of depression associated with isotretinoin use in acne.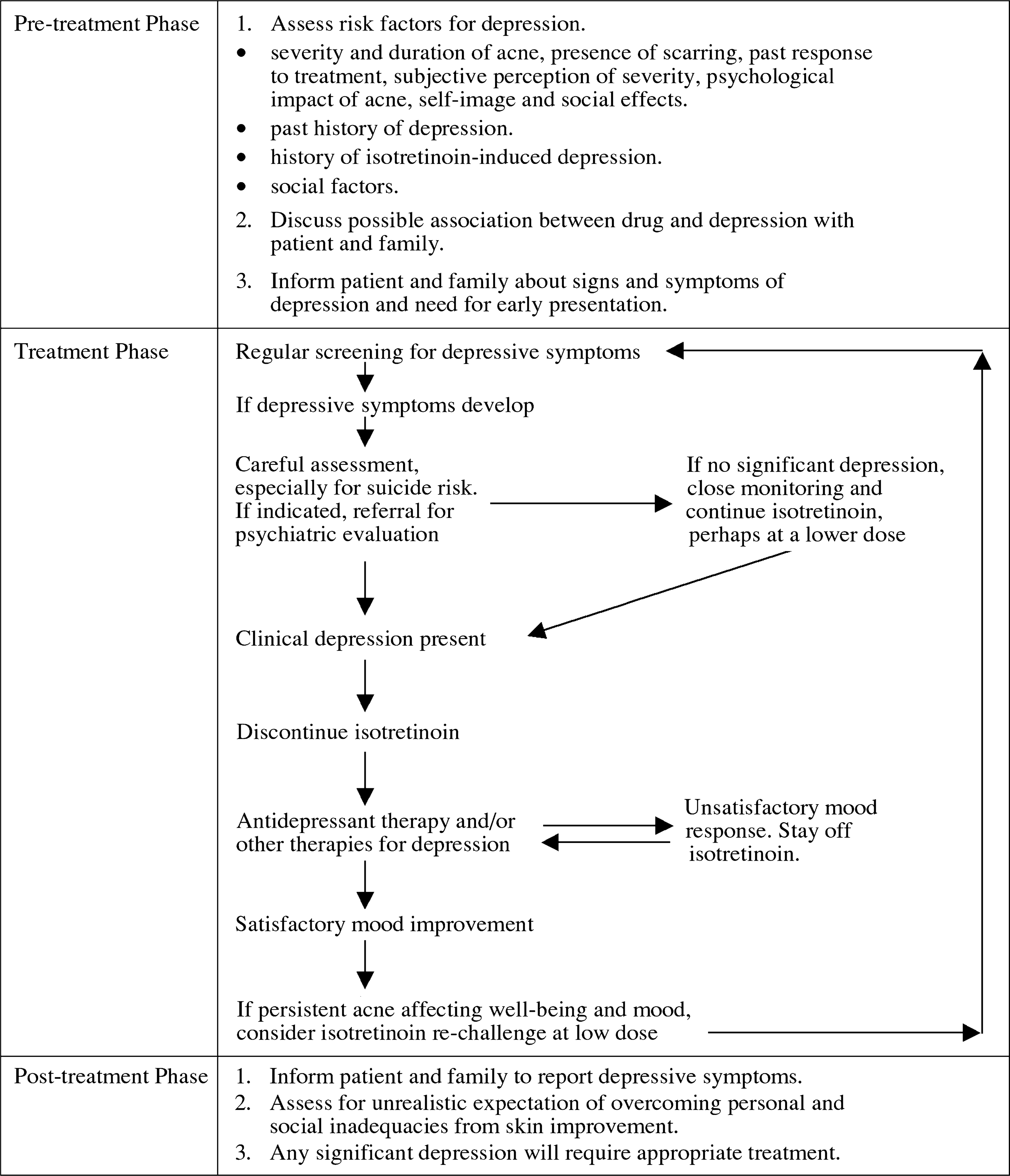
On the balance of the issues concerning the association between the drug and depression, isotretinoin is more likely to have a positive rather than negative psychological impact for the majority of patients who benefit from such a highly efficacious anti-acne treatment. Although no cause and effect mechanism has been clearly established, it is important to recognize that depression can occur as an idiosyncratic adverse effect that requires urgent and appropriate treatment because of the possible risk of severe deterioration and suicide. Psychiatrists, dermatologists and general practitioners need to be aware of such risks as the use of isotretinoin is likely to increase significantly in the future. Having a low threshold of detection and early psychiatric referral and evaluation to address both the depression and its contributing factors may prevent serious consequences.
Footnotes
Acknowledgements
Thanks to Mei Mui Tam, Virginia Tuckwell and staff of the Mood Disorders Unit, The Melbourne Clinic, for their assistance.
