Introduction
We have reported that peroxisome proliferator-activated receptor (PPAR gamma) agonist, pioglitazone, protects against cerebral injury by anti-oxidant mechanisms. 1 The neuroprotective effect of pioglitazone induces SOD-1, suggesting that PPAR gamma activation is involved as a mechanism of the protection against cerebral injury. It is suggested that nitric oxide synthase is closely related to PPAR especially in inflammatory change. The purpose of this study is to investigate the effect of pioglitazone on the nitric oxide production in brain during ischemia and reperfusion.
Methods
Seventeen male Wistar rats were used. We gave pioglitazone 20 mg/kg/day in 10 rats for 4 days (pioglitazone group), and 7 rats were used as contol group. Microdialysis probes were inserted into the left striatum and hippocampus. The probes were perfused with Ringer's solution at a constant rate of 2 μl/min. After 2 hours equilibrium period, the fractions were collected every 10 minutes. Laser Doppler probes were also inserted into right striatum and hippocampus. Cerebral ischemia was produced by bilateral occlusion of common carotid arteries and induced hyotension (mean blood pressure was less than 50 mmHg) by exsanguination of the blood for 20 minutes. After 20 minutes ischemia, bilateral common carotid arteries were reopened and blood was reinfused. The levels of nitrite (NO2-) and nitrate (NO3-) in the dialysate samples were measured by the Griess reaction.
Results
Blood Pressure There were no significant differences between the two groups. Cerebral Blood Flow (CBF)
Striatum No significant differences were observed between the two groups. Hippocampus: CBF in pioglitazone group (215.7 ± 62.5%, mean ± SD) showed significantly higher than that of control group (149.9 ± 39.1%) in 10 minutes after reperfusion. Nitric oxide
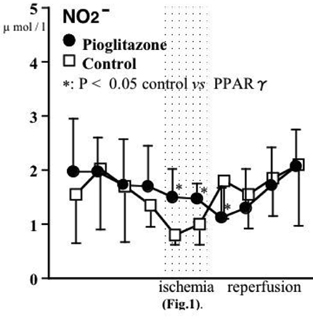
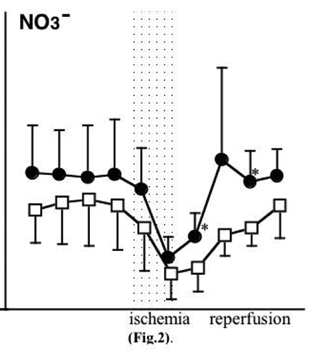
Striatum The level of NO2- in pioglitazone group (1.5. ± 0.5, 1.5 ± 0.3 μmol/l) showed significantly higher than that of control group (0.8 ± 0.2, 1.0 ± 0.4) during ischemia. The level of NO2- in pioglitazone group (1.1 ± 0.6) showed significantly lower than that of control group (1.8 ± 0.7) 10 minutes after the start of reperfusion (Fig. 1). The level of NO3- in pioglitazone group (1.2 ± 0.4, 2.2 ± 0.5) showed significantly higher than that of control group (0.7 ± 0.4, 1.4 ± 0.3) at 10 and 30 minutes after reperfusion (Fig. 2). The level of total NO (NO2- + NO3-) in pioglitazone group (3.5 ± 1.2, 2.4 ± 0.4) was significantly higher than that of control group (2.2 ± 0.8, 1.6 ± 0.6) during ischemia. Hippocampus: There were no significant differences between the two groups.
Conclusion
These data suggest that pioglitazone activate nitric oxide synthase in the striatum during cerebral ischemia.
