Introduction
It is suggested that angiotensin II type Ia receptor blocker (ARB) reduces the infarctrion volume in experimental cerebral ischemia. The relationship between renin-angiotensin system and nitric oxide (NO) is well known. The purpose of this study is to investigate the effect of ARB on the cerebral NO production during cerebral ischemia and reperfusion in aged spontaneous hypertensive rat (SHR).
Methods
Twelve male SHR were used; control group (n=6) [350–420 g in weight; 12 months old] and candesartan group (n=6) [treated with candesartan 10 mg/kg/day for two weeks. 325–410 g in weight; 18 months old]. They were anesthetized by intraperitoneal injection of pentobarbital sodium. NO production was continuously monitored by in vivo microdialysis. Microdialysis probes were inserted into the left striatum and hippocampus and were perfused with Ringer's solution at a constant rate 2 μl/min. Laser Doppler probes were also inserted into the right striatum and hippocampus. After 2 hours equilibrium period, fractions were collected every 10 minutes. Forebrain cerebral ischemia was produced by occlusion of both common carotid arteries, and systemic hypotension (MABP < 50 mmHg) induced by hemorrhage. After 20 minutes, the loops around both common carotid arteries were released and the blood was re-infused. Levels of NO metabolites, nitrite (NO2-) and nitrate (NO3-), in the dialysate were determined using the Griess reaction.
Results
Blood Pressure; Mean BP for 40 minutes before ischemia in the candesartan group [109 ± 11 mmHg (mean ± SD)] showed significantly lower than that of the control group [158 ± 26] (p<0.05). Cerebral Blood Flow (CBF) in hippocampus and striatum; No differences in both groups were shown. Nitric oxide; The levels of NO2- in striatum of the candesartan group were significantly lower than those of the control group (p<0.05) in 20, 30, 60, 90, 100 minutes after the start of reperfusion.
The levels of NO2- in hippocampus of the candesartan group were significantly lower than those of control group (p<0.05) in 10 minutes of ischemia and 70 minutes after reperfusion. The levels of NO3- in striatum of the candesartan group were significantly higher than those of the control group (p<0.05) before ischemia and during reperfusion. (Fig. 1) The levels of NO3- in hippocampus of the candesartan group were significantly higher than those of the control group (p<0.05) after the start of reperfusion.
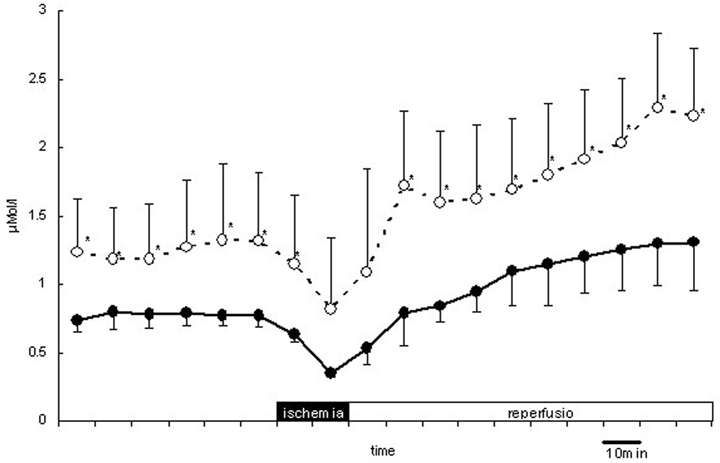
The level of NO−3 in striatum
Conclusion
These data suggest that NO production in striatum in aged SHR was enhanced by candesartan. It is concluded that candesartan recovered the NO production in aged SHR, as we have already reported that NO production in aged SHR decreased compared to the young one.
