Introduction
Despite many years of research the pathogenesis of vasospasm after subarachnoid haemorrhage (SAH) still remains elusive and no specific treatment exists to alleviate the condition. Previous studies have shown that endothelin type B (ETB) and 5-hydroxytryptamine type 1B (5-HT1B) receptors are upregulated following experimental SAH. However, the intracellular pathways responsible for this receptor upregulation remains unclear. The purpose of the present study was to investigate the involvement of protein kinase C (PKC) in an experimental induced SAH model. We also wanted to test whether PKC inhibition could alter the degree of SAH induced ET and 5-HT1 receptor upregulation in addition to prevent the cerebral blood flow reduction.
Methods
SAH was induced by injecting 250 μl blood into the prechiasmatic cistern. In conjunction and after the induced SAH the PKC inhibitor RO-31-7549 was injected intracisternally. Two days after the SAH basilar arteries (BA) and middle cerebral arteries (MCA) were harvested and contractile responses to endothelin-1 (ET-1; ETA and ETB receptor agonist) and 5-carboxamidotryptamine (5-CT; 5-HT1 receptor agonist) were investigated by sensitive myographs. ETA, ETB and 5-HT1B receptor mRNA levels were analyzed by real-time PCR. In addition the regional CBF in sham, SAH and SAH treated with PKC inhibitor was evaluated by an autoradiographic technique.
Results
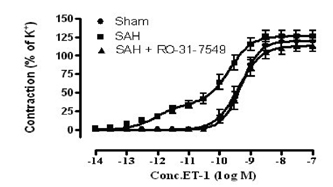
The PKC inhibitor RO-31-7549 decreased the maximum contraction elicited by application of ET-1 in BA and MCA as compared to SAH. A sigmoidal curve was obtained with an Emax of 113±8%, and a pEC50 of 9.42±0.16 (Fig. 1). Interestingly there was no significant difference in the contractile response between sham and RO-31-7549 treated rats. Treatment with RO-31-7549 also decreased the maximum contraction elicited by application of 5-CT considerably as compared to SAH. In parallel the PKC inhibition downregulated ETB and 5-HT1B receptor mRNA levels. No differences were observed in the ETA receptor mRNA levels. The reduction in global and regional CBF observed after SAH was significantly prevented with treatment with RO-31-7549 (SAH: 56.5±4.0 and RO: 116.6.±7.3 ml/min/100 g). Statistical analyses were performed using the nonparametric Wilcoxon rank test, differences were considered significant at p≤0.05. Data are expressed as mean ± s.e.m.
Conclusion
Our study suggests that PKC plays an important role in the pathogenesis of cerebral vasospasm. Inhibition of PKC prevented the reduction in the perfusion of global and regional CBF. It also attenuated the vasoconstriction mediated by ETB and 5-HT1B receptors and decreased the receptor mRNA levels in rat cerebral arteries after SAH. These results indicate that PKC may be an important intracellular mediator for receptor upregulation and via its inhibition we can prevent the cerebral vasospasm associated with SAH.
