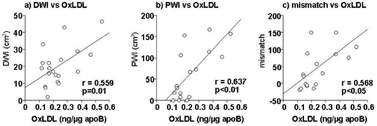
Oxidized low-density lipoprotein (OxLDL) plays a major role in atherosclerosis. In our previous study, we used specific antibody against oxidized phosphatidylcholine (FOH1a/ DLH3) by which OxLDL is recognized, and first demonstrated the significant association between raised plasma OxLDL and acute cerebral infarction, especially cortical infarction. We undertook the present study to clarify the relationship between plasma OxLDL and the ischemic volume. We used ELISA to determine plasma OxLDL levels and performed diffusion- and perfusion-weighted MRI (DWI, PWI) to measure the ischemic volume in 44 ischemic stroke patients. Based on the location of the ischemic lesion, they were divided into 3 groups: Group I (GI, n=21) had cortical lesions, Group II (GII, n=17) had lesions in the basal ganglia or brain stem, and Group III (GIII, n=6) had massive lesions that involved one entire hemisphere. In GI, but not GII and GIII, plasma OxLDL was significantly higher than in 19 age-matched controls (p<0.01) and was significantly correlated with the initial ischemic volume visualized on DWI (p=0.01), PWI (p<0.01), and the DWI-PWI mismatch (p<0.05)(Figure 1a–c). A persistent increase in plasma OxLDL was associated with enlargement of the ischemic lesion in the early phase after the insult. These findings suggest that elevated plasma OxLDL levels are associated with moderate ischemic damage in patients with cortical lesions (GI) but not those with massive hemispheric lesions (GIII) which may be irreversible. In addition, elevated plasma OxLDL may represent a predictor of enlargement of the ischemic lesion.